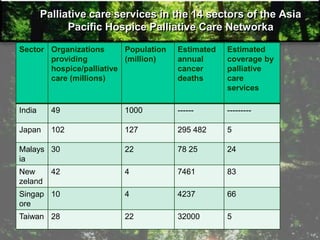
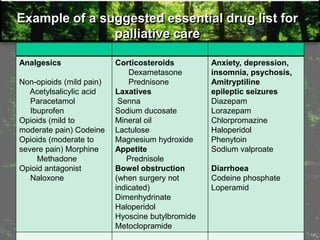
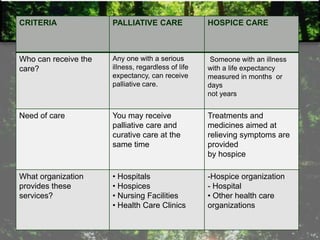
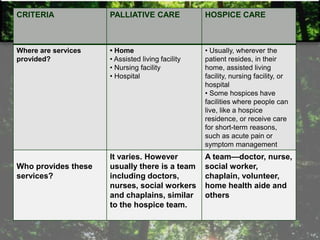
The document provides information on palliative care, including:
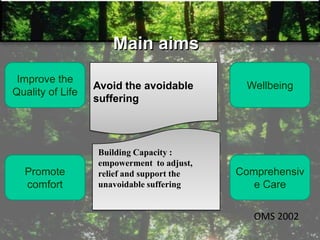
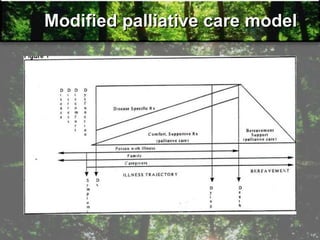
- Palliative care aims to improve quality of life and relieve suffering for patients with life-limiting illnesses and their families.
- It focuses on pain management and other symptom relief without hastening or postponing death.
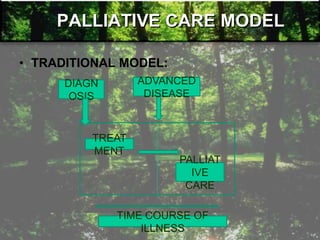
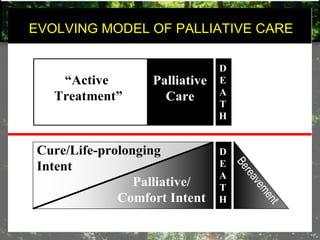
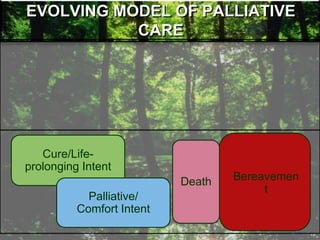
- Palliative care is appropriate at any stage of illness and can be provided alongside curative treatment.












![• Informal caregivers are not members of
an organization. They [usually] do not
have formal training, and are not
accountable to norms of conduct or
practice. They may be family members
or friends‖ (CPCA, 2001).
5/23/2014 Free PowerPoint Template from www.brainybetty.com 13](https://image.slidesharecdn.com/palliativecare-140522235402-phpapp01/85/Palliative-care-13-320.jpg)