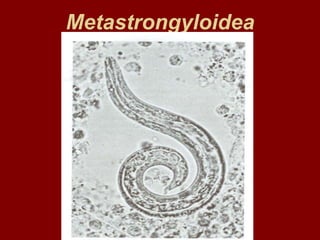
Lecture 9 metastrongyloidae
- 2. Characteristics • Most worms in this superfamily inhabit the lungs or the blood vessels adjacent to the lungs. • The typical life cycle is indirect, and the intermediate host is usually a mollusk.
- 3. Oslerus osleri (TRACHEAL WORM) Definitive Host Spectrum • Canids Geographic Distribution • Worldwide, but low prevalence Morphology • Adults - males 5 mm, females 9-15 mm • Eggs - larvated, 80 x 50 microns, hatch before passing in feces • Larvae - 232-266 microns, with S-shaped tail
- 4. Life Cycle (Stages) • L 1 are passed in feces or saliva • These L 1 are immediately infective • Major modes of transmission are by the bitch licking her pups, fecal contamination, licking of mouth, and feeding by regurgitation (wild canids) • Once acquired larvae migrate to the trachea via the lymphatic and venous portal systems • Prepatent period - 6-7 mos.
- 5. Site of Infection • Trachea and bronchi Pathogenesis/Clinical Signs • Adult worms live in or under the tracheal or bronchial mucosa and cause grayish-pink fibrous nodules to develop which cause a cough. • These granulomas are usually less than 1 cm in diameter • Clinical signs - cough, dyspnea, anorexia, emaciation • Usually a chronic disease of young dogs, but can be fatal
- 6. Diagnosis • Bronchoscopy - nodules at the bifurcation of the trachea (predilection site) • Typical larvae in feces, tracheal swabs or sputum - in feces they are neither plentiful nor very active • Thoracic radiography Treatment • No satisfactory treatment - can try levamisole, albendazole, fenbendazole or avermectins (cautionary in dogs) Other control Measures • Remove pups by caesarian section and raise them in isolation but not practical;
- 7. Filaroides hirthi (LUNGWORM) Definitive Host Spectrum – Canids Geographic Distribution – Eastern US, Texas Morphology – Adults - males 2-3 mm, females 6.6-13 mm – Larvae - 240-290 microns long Life Cycle (Stages) – Similar to F. osleri – Prepatent period - 5 weeks
- 8. Site of Infection: Lung parenchyma Pathogenesis/Clinical Signs • Focal granulomatous reaction • Usually no clinical disease • Fatalities have occurred in severely stressed or immune deficient dogs Diagnosis • Finding larvae in feces - zinc sulfate flotation is better than Baermann technique • Usually diagnosed post mortem Treatment • Albendazole • fenbendazole
- 9. Aelurostrongylus abstrusus (CAT LUNGWORM) Definitive Host Spectrum • Felids Intermediate Host • Snails • Rodents, frogs, lizards and birds may serve as paratenic hosts Geographic Distribution • Worldwide; in the US, southern states Morphology • Adults - rarely seen intact because they are deeply imbedded in tissue; males up to 7 mm, females up to 10 mm • Larvae - about 360 microns, tail has a double bend and a dorsal spine
- 10. Life Cycle (Stages) • Eggs are laid by females, L 1 hatch and are carried up the bronchial tree and are swallowed and passed in feces • Larvae penetrate IH and undergo 2 molts • Cats acquire the infection either by eating snails or by eating the paratenic host which has eaten an infected snail • Larvae migrate from the stomach to the lungs through the peritoneal and thoracic cavities • Prepatent period - 4 to 6 weeks Site of Infection • Terminal bronchioles and lung parenchyma
- 11. Pathogenesis/Clinical Signs • Usually nonpathogenic • Lesions are subpleural grayish nodules which are firm, raised, and 1-10 mm in diameter • The parasite causes smooth muscle hypertrophy of the bronchioles, alveolar ducts and tunica media of the small arteries as well as hyperplasia. • Clinical signs - usually none; in heavy infections cough, dyspnea, emaciation, nasal discharge and sneezing Diagnosis • Typical L 1 in feces • Radiographic evidence includes bronchial, alveolar disease and pulmonary artery hypertrophy (PAH) Treatment • Fenbendazole Other Control Measures • Impractical, try to stop ingestion of intermediate or transport hosts
- 12. Protostrongylus rufescens (RED LUNGWORM) Definitive Host Spectrum: Sheep, goats, Intermediate Host : Snails (several genera) Geographic Distribution – North America, Europe, Africa, Australia Morphology – Adults - slender, reddish, males 16-28 mm, females 25-35 mm – Larvae - 250 to 340 microns; tip of tail has wavy outline, but no spine Life Cycle (Stages) – Larvae (L 1 ) are passed in feces – L 1 penetrate snails – 2 molts in snail – DH ingests snails while grazing – Migration to the lungs via mesenteric lymph glands and circulation – Transplacental transmission occurs – Prepatent period - 30 to 37 days
- 13. Site of Infection – Small bronchioles Pathogenesis/Clinical Signs – Worms produce local inflammation of small bronchioles – Exudate fills alveoli distal to the parasites – The affected alveolar and bronchiolar epithelium is desquamated, blood vessels are occluded and infiltration with round cells occurs resulting in a small focus of lobular pneumonia – 2 o bacterial infections possible – Usually no definite clinical signs
- 14. Diagnosis • Finding larvae in feces Treatment • Levamisole, fenbendazole, ivermectin, doramectin Other Control Measures • Keep lambs off pastures previously used by infected animals • Salt blocks or range cubes containing anthelmintics • Molluscicides
- 15. Muellerius capillaris (HAIR LUNGWORM) Definitive Host Spectrum Sheep, goats, Intermediate Host Snails ( Helix , Succinea ) Geographic Distribution Worldwide, not of major importance in the US Morphology Adults - delicate, threadlike; males 12-14 mm, females 19-23 mm Larvae - 230-300 microns, tip of tail wavy and with a dorsal spine Life Cycle L 1 are passed in feces L 1 penetrate IH or are ingested 2 molts in IH DH ingests snail or slug while grazing Migration to lungs via lymphatics Prepatent period - about 6 weeks
- 16. First larva of Muellerius capillaries; whole larva (A); anterior end (B); posterior end (C); wavy tip of the tail with a dorsal spine
- 17. Site of Infection – Alveoli and lung parenchyma, terminal bronchioles – Pathogenesis/Clinical Signs – Worms produce grayish nodules up to 2 cm in diameter, consisting of degenerating leucocytes and pulmonary tissue – Nodules may calcify – Occasionally, adenoma-like proliferation of bronchial epithelium is seen – 2 o bacterial infection of the nodules may occur; nodules may coalesce to form septic lesions – Usually no clinical signs, but in heavily infected goats coughing and dyspnea may occur – Diagnosis – Finding L 1 in feces – Treatment – Try repeated doses of fenbendazole, or avermectin class – Other Control Measures – Same as for Protostrongylus ; also spreading lime to kill snails
- 18. Characteristic nodular lesions associated with Muellerius infection of sheep lung