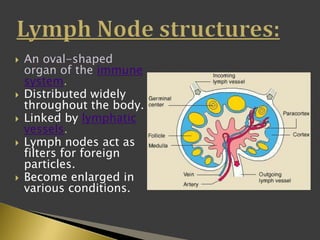
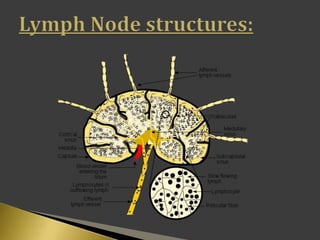
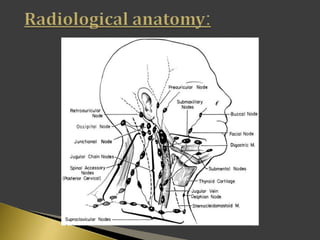
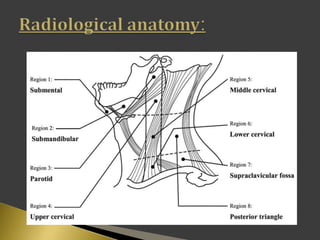
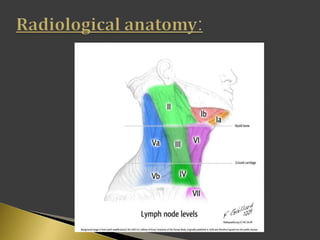
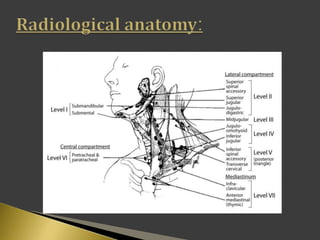
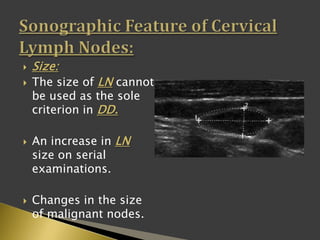
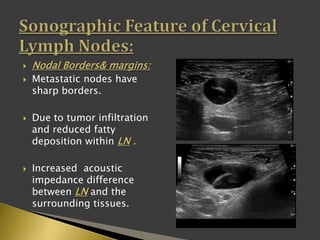
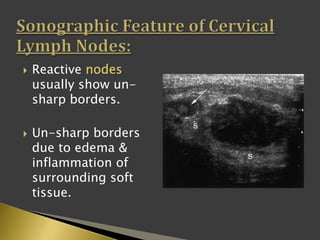
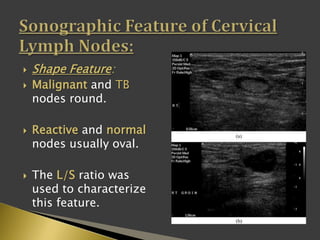
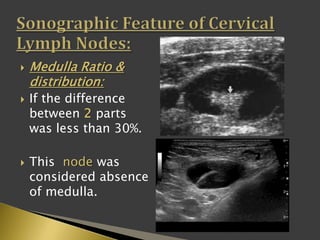
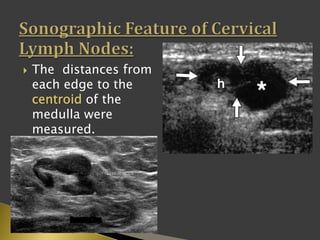
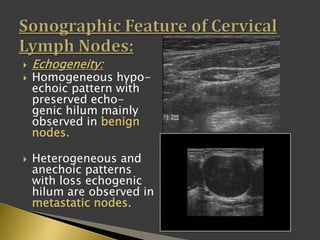
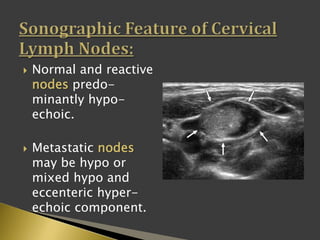
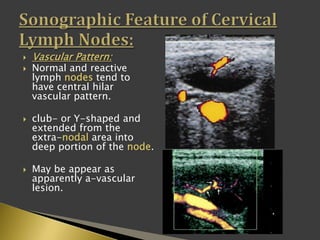
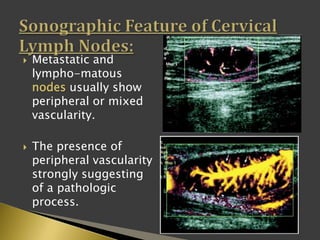
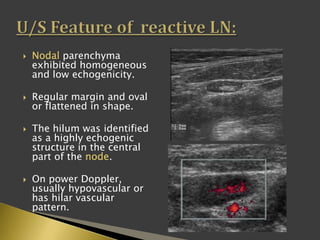
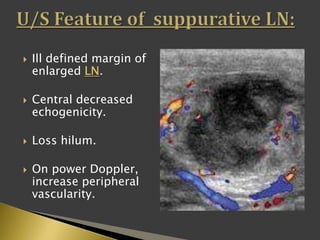
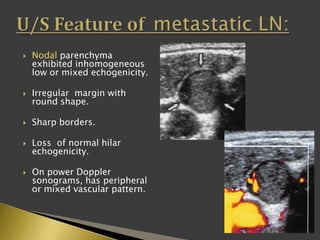
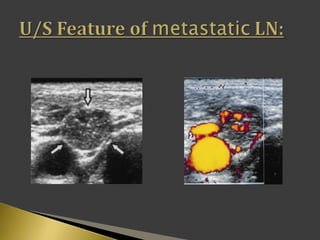
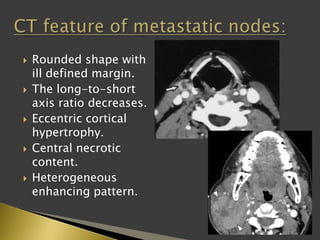
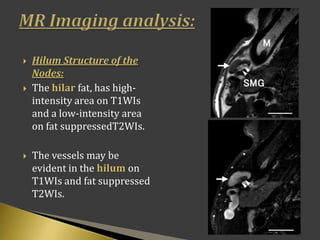
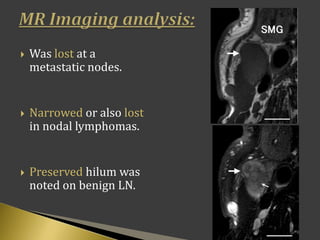
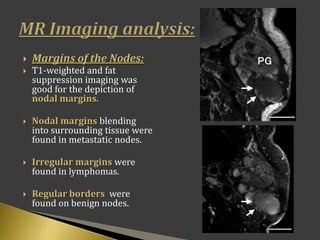
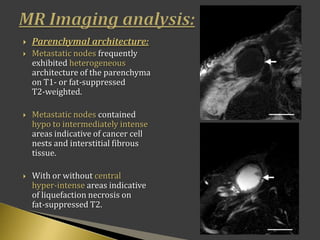
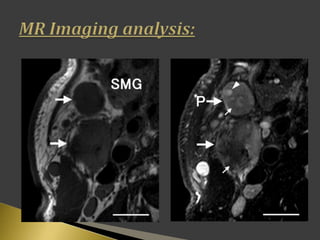
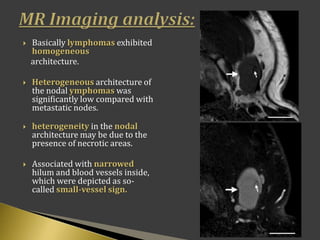
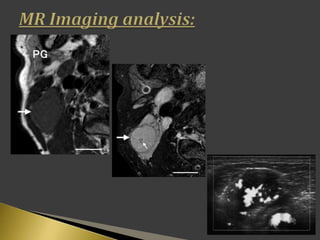
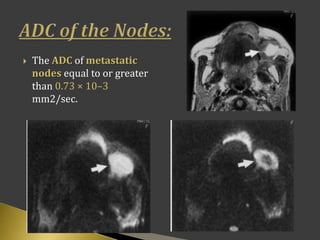
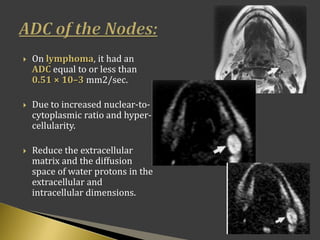
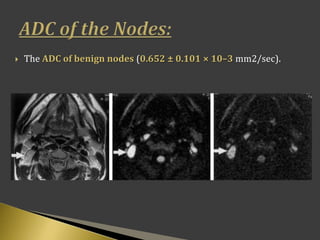
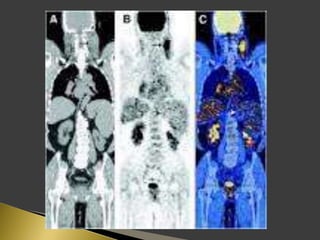
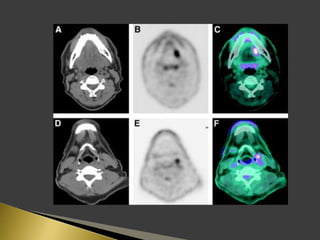
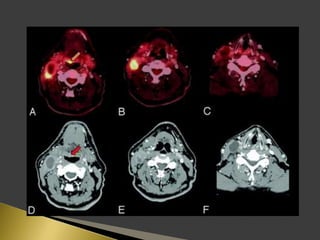
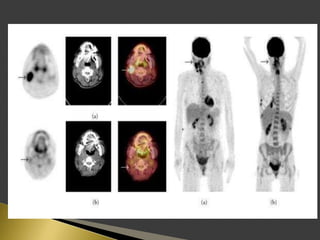
This document discusses diagnostic imaging techniques for evaluating lymph nodes in patients with head and neck cancer. It describes the use of ultrasound, CT, MRI, diffusion-weighted MRI, and PET imaging to analyze lymph node characteristics like size, shape, margins, echogenicity, necrosis and vascularity which can help differentiate between metastatic, inflammatory and normal lymph nodes. Quantitative measurements like ADC from diffusion MRI and SUV from PET can also provide diagnostic information and predict cancer spread and treatment response.