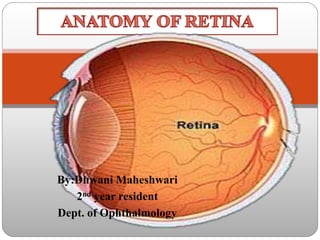
Anatomy of retina
- 1. By:Dhwani Maheshwari 2nd year resident Dept. of Ophthalmology
- 2. Retina • Retina, is the innermost tunic of the eyeball • Thin,delicate,transparent membrane • Highly developed tissue of the eye • Appears purplish red
- 3. EMBRYOLOGY OF RETINA Retina is developed from the two walls of the optic cup, namely: (a) nervous retina from the inner wall, and (b) pigment epithelium from the outer wall (a) Nervous retina The inner wall of the optic cup is a single-layered epithelium. It divides into several layers of cells which differentiates further.
- 4. (b): Outer pigment epithelial layer. Cells of the outer wall of the optic cup become pigmented. Its posterior part forms the pigmented epithelium of retina and the anterior part continues forward in ciliary body and iris..
- 7. GROSS ANATOMY Three distinct regions of retina: 1.optic disc 2.macula lutea 3.peripheral retina retina extends from optic disc to ora serrata Surface area:266 mm²
- 8. Optic disc Palepink in colour; well defined circulararea Diameter: 1.5mm All the retina layers terminate here,exceptthe nerve fibre which pass through the lamina cribrosa to run into the optic nerve. In contrast to the rest of the retina,the optic disc appears pale due to lamina cribrosa, medullated nerve fibres behind it & absence of vascular choroid.
- 9. MACULA Themacula lutea iscomparatively darkarea 5.5 mm in diameter , situated at the posterior pole of the eyeball, temporal to optic disc Alsocalled asyellow spot or areacentralis Primary function :- photoptic vision Oxygenated carotenoids, in particular lutein & zeaxanthin,accumulate within the central macula & cause yellow colour. They have antioxidants properties & also function to filter the blue wavelengths of light ,possibly preventing photic damage.
- 10. Foveacentralis is central depression in macula;measuring 1.50 mm in diameter & 1.55 mm thickness It ismost sensitive part of retina It is entirely made up of cones. fovea Foveola
- 11. Foveola Diameter:- 0.35mm Central floor offovea Umbo isthe tiny depression in centre of foveola macula FOVEA FOVEOLA UMBO
- 12. APPLIED; • Lack of blood vessels and neural tissue in foveola allows light to pass unobstructed into the photoreceptor outer segment • Chronic retinal oedema may result in the deposition of hard exudates around the fovea in the layer of Henle with a macular star configuration
- 13. UMBO : it corresponds to visible foveolar reflex,seen in most normal eyes. Loss of the FR may be an early sign of damage. Greatest concentration of cones is found in the umbo, 150- 200µm diameter known as central bouquet of cones. FOVEALAVASCULAR ZONE; It is located inside fovea but outside foveola,its location can be determined accurately only by fluorescin angiography.
- 14. PARAFOVEA- refers to a belt that measures 0.5mm in width & surrounds the foveal margin. PERIFOVEA-refers to 1.5mm belt surrounding perifoveal region. Histologically ,it has several layers of ganglion cells & 6 layers of bipolar cells.
- 15. Peripheral retina Theperipheral retina canbe divided intofour regions 1. Nearperiphery 2. mid periphery 3. Farperiphery 4. Extremeperiphery
- 16. PR is divide into four parts 1. Near periphery • (1.5mm around the macula ) 2.Mid-periphery • (3mm around the near periphery ) • 3.Far periphery; Extends 9-10 mm from optic disc on the temporal side and • 16 mm on the nasal side in the horizontal meridian 9-10mm macula 5.5m m 16mm 1.5mm 3mm
- 17. EXTREME PERIPHERY-refers to the area of ora serrata & pars plana ORA SERRATA- Description Length Width of ora serrata 2.1mm temporally 0.7-0.8mm nasallly Location from limbus 6mm nasally 7mm temporally From equator 6-8mm From optic disc 25 mm nasally
- 18. APPLIED: Ora serrata is a watershed zone between ant. & post. Vascular systems hence peripheral retinal degenerations are most common
- 19. 1. Retinal pigment epithelium 2. Layerof rods andcones 3. External limiting membrane 4. Outer nuclear layer 5. Outer molecular (plexiform)layer 6. Inner nuclear layer 7. Inner molecular (plexiform)layer 8. Ganglion cell layer 9. Nerve fibre layer 10. Internal limiting membrane Microscopic structure of theretina (from without inward)
- 20. RETINAL PIGMIENT EPITHELIUM It isthe outermost layer ofretina Made up of single layer ofhexagonal cells Thecells contain pigments It isfirmly adherent to the underlying bruch’s layer & loosely attached layer to layer of rod and cone cells Sub-retinal space:- potential spacebetween RPE & retina
- 21. • 4- 6 million RPE cells per eye. • Extends from the optic disc to the ora serrata, Bruch’s membrane RPE Photorecep tor layers
- 22. RPE are Cuboidal cells with three Cell Surfaces characteristics 1.Apical surface –inner surface 2.Paracellular surface/intercellular surfaces 3.Basal surface –outer surface Apical surface • Has microvillous processes- Increases Surface area • Interdigitate with outer segments of photoreceptor cells • Contains melanin granules –more in macular region RPE- ULTRA STRUCTURE
- 23. APPLIED; • No specialized junctional complex between RPE and photoreceptors- they are loosely adhered • Creates potential space( subretinal space- prone for RD)& the fluid between these two layers is called subretinal fluid
- 24. Basal surface; • Attached to its basal lamina, of Bruch's membrane. • Nutrients from choriocapillaries diffusess to RPE through basal lamina • It has convoluted infolds to increase the surface area for absorption & secretion of material. Paracellular surface; • Contains tight junction( Zonula Occluden & adheran, gap junctions) • Junctional complex form blood-retinal barrier • Maintains retinal homeostasis and prevents from toxic damages
- 25. FUNCTIONS OF RPE: • Visual pigment regeneration • Phagocytosis of shed photoreceptor outer-segment discs • Transport of necessary nutrients and ions to photoreceptor cells and Removal of waste products from photoreceptors • Absorption of scattered and out-of-focus light via pigmentation • Adhesion of the retina • Synthesis and remodeling of the interphotoreceptor matrix, • Formation of the blood-retina barrier, • Elaboration of humoral and growth factors.
- 26. APPLIED: • Failure of the RPE to process cellular debris associated with outer segment turnover cause deposition of Drusen in ARMD • Disruption of blood retinal barriers causes retinal edema eg. Macular edema
- 27. Layerof Rods& Conecells Rods& conestransform light energy intonerve impulses.
- 28. RODS CONES maximum density in 20°(3mm) from the fovea.(160,000 rods/mm2) minimum density- fovea Rodscontain photosensitive substancerhodopsin Night vision- scotoptic 3 types of iodopsin trichromatic pigments: 1. S wavelength cones- 440nm blue light) 2.M wavelenght cone- 540nm green 3. L wavelenght cone- 577nm red - density is maximum at fovea (199 000 cones/mm2) minimum density- periphery conescontain photosensitive substance iodopsin - photopticvision rhodopsin is sensitive to blue-green light- 493nm
- 29. APPLIED: • Mutation of rhodopsin in retinitis pigmentosa causes maximum pigmentation 3mm around the fovea • With advanced age there is progressive loss of photoreceptors (rods are affected more than cone)- poor night vision in elderly
- 30. Structure of photoreceptor Rods and cones are composed of several parts- six main parts 1. The outer segment, containing the visual pigment molecules for the conversion of light into a neural signal; 2. A connecting stalk, the cilium(cytoplasmic isthmus) 3. The inner segment, containing the metabolic apparatus; 4. The outer fiber; 5. The cell body- forms outer nucleated layers 6.The inner fiber, which ends in a synaptic terminal outer plexiform layer
- 32. STRUCTURE OF ROD CELL: 1. 40-60 µm long. 2. Outer segment is cylindrical- contains visual pigments 3. Pigments are located in flattened double lamellae in the form of discs. 4. Discs various between 600 to 1000/rod cell. There are no special attachments bet. discs or bet. discs and plasma membrane. 5. Discs contain 90% of the visual pigment remaining is scattered on plasma membrane. 6. Inner segment of the rod is thicker than the outer. It has two regions. a. Outer eosinophilic ellipsoid which contains more mitocondria. b. Myoid which contains glycogen as well as usual organelles
- 33. Outerrodfibre arisesfrom innerendof rod & passesthrough external limiting memebrane further swellsinto densely stainednucleus Thenucleusterminates further into innerrod fibre Theinner rod fibre endsasabulb calledrod spherule APPLIED; • Rod need great sensitivity to detect the small amount of light available • Rod are numerous and contains about a million rhodopsin molecule in each sac/disc
- 34. 1. Conical in shape 2. 40 TO 80 µm long 3. Cone at periphery is short(40) but in central fovea it is tall(80) and resembles rod 4.Outer segment contains photo pigments called iodopsin. 5. The cone outer segment have more discs (1000-1200 per cone) than do rod outer segments 6. Lamellar disc are attached to the membrane CONES- MORPHOLOGY
- 35. 1.Inner segment becomes directly continuous with the nucleus & lies in the outer nuclear layer 2. Ellipsoid contains a large number of mitochondria. 3. Cone inner fibre ends in cone pedicle/foot which lies in the outer plexiform layer
- 36. • Not a true membrane • Composed of the junctions(zonulae adherentes) between Muller cells and photoreceptors Fenestrated membrane Extents from the ora serrata to the edge of optic disc. MULLER CELL ONL ELM RPE EXTERNAL LIMITING MEMBRANE
- 37. OUTER NUCLEAR LAYER Made up of the nuclei of rods & cones Conenuclei:- 6-7 um Rodnuclei :-5.5um Thesenuclei lie in asingle layer nextto external limiting membrane Rodnuclei form the bulk of this layer except at cone dominated fovealregion
- 38. Variation in Thickness • Nasalto disc:- 45um ( 8-9 layers) • Temporal to disc :- 22um (4rows) • Fovealregion :- 50um (10rows) • Restof retina except ora serrata – 27 um(1 row of cones & 4 rows of rods)
- 39. OUTER PLEXIFORM LAYER Thislayer ismadeof synapsesbetween the rod spherules & conepedicles with the dendrites of bipolar cells. Also known as Henle’s layer
- 40. INNER NUCLEAR LAYER This layer disappears at fovea & in rest of the retina consists of the following: Bipolar cells Horizontalcells Amacrinecells Somaof Mullers cells Capillaries ofCentral retinal vessels
- 41. BIPOLAR CELLS Under light microscopy nine types are seen: a. Rod bipolar cells(RB) b. Invaginating midget bipolar(7) – c. Flat midget bipolar d. Invaginating diffuse bipolar e. Flat diffuse bipolar f. On-centre blue cone bipolar g. Off-centre blue cone bipolar h. Giant bistratified bipolarGBB) i. Giant diffuse invaginating bipolar
- 42. ROD BIPOLAR CELLS: they have large soma & profuse dendrites which arborize only with the rod sperules. MIDGET BIPOLAR CELLS: They make contact with cone pedicle.
- 43. HORIZONTAL NEURONS They are flat cells having numerous horizontal associative & neuronal interconnections between photoreceptors & bipolar cells in the outer plexiform layer
- 44. AMACRINE CELLS These have a pyriform body & a single process which passes inwards in the inner plexiform layer & forms connections with the axons of the bipolar cells & the dendrites & soma of ganglion cells. Thus they perform an integrative function.
- 45. MULLER CELLS The nucleus & cell bodies of the muller’s cells are located within the inner nuclear layer. Fibres from their outer end extend upto external limiting membrane & those from inner end extend upto inner internal limiting membrane. Function:provides structural support Aids in metabolism of sensory retina
- 47. INNER PLEXIFORM LAYER Consistsof synapsebetween bipolar cell& dendrites of ganglioncell Absent at fovea
- 48. GANGLION CELL LAYER Consistof cellbody& nucleiof ganglioncell( 2nd orderneurons) Absentat fovea At the edge of foveola (macula) it is multi layer(6-8 layered) and on temporal side of disc it has two layers. Ganglion cells transmits signal from the bipolar cell to the lateral geniculate body Varioustypes of ganglioncell:- 1) W, X ,Y ganglion cell 2) P(P1&P2)& M GANGLIONCELL 3) Off centre & on centre cell 4) Monosynaptic & polysynaptic cell
- 49. NERVE FIBER LAYER The nerve fibre layer contains the axons of the ganglion cells Optic nerve consists of approximately 1.2- 1.5 million axons of retinal ganglion cells Their course runs parallel to the retinal surface The fibers proceed to the optic disc at a right angle, and exit the eye through the lamina cribrosa as the optic nerve. The fibers generally are unmyelinated within the retina
- 50. ARRANGEMENT OF NERVE FIBRES IN THE RETINA 1. Fibres from the nasal half of the retina come directly to the optic disc as superior and inferior radiating fibres (srf and irf). 2. Fibres from the macular region pass straight in the temporal part of the disc as papillomacular bundle (pmb). 3. Fibres from the temporal retina arch as superior and inferior arcuate fibres (saf and iaf).
- 51. The papillomacular bundle represents the thinnest portion of the nerve fibre layer around the optic disc
- 52. ARRANGEMENT OF NERVE FIBRES OF THE OPTIC NERVE HEAD: • Fibres form the peripheral part of the retina lie deep in the retina but occupy the most peripheral part of the optic disc. • While the fibres originating closer to the optic nerve head lie superficially in the retina and occupy a more central (deep) portion of the disc.
- 53. THICKNESS OF NERVE FIBRE LAYER AT THE DISC: Thickness of the nerve fibre layer around the different quadrants of the optic disc margin progressively increases in the following order: 1.Most lateral quadrant (thinnest) 2.Upper temporal and lower temporal quadrant 3.Most medial quadrant 4.Upper nasal and lower nasal quadrant (thickest)
- 54. CLINICAL SIGNIFICANCE OF DISTRIBUTION AND THICKNESS OF NERVE FIBRES AT THE OPTIC DISC MARGIN: 1. Papilloedema appears first of all in the thickest quadrant (upper nasal and lower nasal) and last of all in the thinnest quadrant (most lateral). 2. Arcuate nerve fibres are most sensitive to glaucomatous damage, accounting for an early temporal arcuate visual scotoma in glaucoma 3. Macular fibres occupying the lateral quadrant are most resistant to glaucomatous damage and explain the retention of the central vision till end.
- 55. Internal limiting membrane • Itformsinterfacebetweenretina&vitreous • Consistsof followingelements:- • 1) collagenfibrils • 2) proteoglycans of vitreous • 3) basementmembrane • 4) plasmamembrane of mullercells • 5) other glialcells
- 56. Blood supply of retina • Outer 4 layers :- choriocapillaries • Inner 6 layer:- central retinalartery • Fovea:- choriocapillaries • Macular region:- superior & inferiortemporal branches of central retinalartery