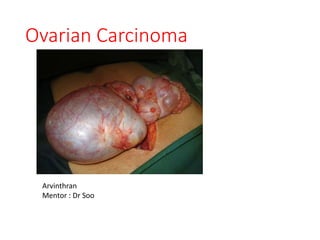
Ovarian carcinoma
- 1. Ovarian Carcinoma Arvinthran Mentor : Dr Soo
- 2. Malaysian National Cancer Registry Report 2007-2011 Epidemiology
- 7. Aetiology Believed to be due to irritation of ovarian surface epithelium by damage during ovulation Thus, risk increased if multiple ovulations and decreased if ovulation suppressed: - Nulliparity - Early Menarche and late menopause - COCP - Pregnancy
- 10. Ovarian Ca: Types • Epithelial 65% • Serous Cystadenocarcinoma • Mucinous Cystadenocarcinoma • Clear Cell Carcinoma • Endometrioid Carcinoma • Transitional cell tumours - Malignant Brenner tumour - Transitional cell carcinoma • Epithelial-stromal - Adenosarcoma - Carcinosarcoma • Sex Cord/Stromal (10%) • Granulosa Cell Tumour • Sertoli-Leydig Cell Tumour
- 11. Ovarian Ca: Types • Germ Cell (15%) • Dysgerminoma • Immature Malignant Teratoma • Endodermal Sinus Tumour • Choriocarcinoma • Metastatic Tumour • Endometrium • Cervix • Fallopian tube • Krukenberg tumours- breast, stomach, colong lymphoma, melanoma carcinoid
- 12. Serous adenocarcinoma • Most common type of epithelial ovarian cancer • May contain psammoma bodies • Often associated with CA125 elevation
- 13. Mucinous adenocarcinoma • Rarely be associated with pseudomyxoma peritonei • CA 125 levels may not be markedly elevated • CA19.9 may be elevated • Relatively chemoresistant • Differential diagnosis of a mucinous ovarian tumour includes metastatic disease from an appendiceal primary
- 14. Endometriod carcinoma • Associated with endometriosis or and independent uterine cancer of similar histology • May occur with early stage disease in younger patients, although advanced disease is possible
- 15. Clear cell carcinoma • Most chemoresistant type • Often contains “hobnail” cells with cleared out cytoplasm due to glycogen
- 16. Granulosa Cell tumour • Include granulosa cell tumour, themocas and fibroma • Cells of granulosa cell tumours produce estrogenic or less commonly, androgenic steroids (eg Oestradiol) • May secrete other factors such as inhibin and Mullerian inhibitory substance, useful as a tumour markers during follow up • Peak incidence in young girls and post menopausal women • Present will PMB, menstrual problems or precocious puberty • May be associated with concurrent endometrial cancer
- 17. Sertoli-Leydig cell tumour • Mostly produce androgens • Present with hirsuitism, amenorrheoea and virilization ( male pattern baldness, clitoromegaly, deepening of voice, hairiness, oily skin) • Normally benign tumours- treated surgically
- 18. Dysgerminoma • Median age 18 • Raised AFP Endodermal Sinus Tumour ( Yolk Sac) • Secrete LDH • Spread earlier through lymphatic • Female equivalent of a seminoma • Common in XY karyotypically abnormal gonads ( Turner’s’ syndrome)
- 19. Chroriocarcinoma • Rare • Usually younger than 20 years old • Raused hCG levels ( choriocarcinoma) or hCG and AFP (embryonal carcinoma)
- 20. Symptoms: • Abdominal discomfort • Urinary frequency/ pressure effects upon bladder & rectum • Abdominal fullness • GIT symptoms – abdominal discomfort/pain, change in bowel habit • Abnormal bleeding (rarely) • Menstrual irregularities (associated with sex cord-stromal tumours) • Postmenopausal bleeding
- 21. Physical signs: •Abdominal mass •Ascites •Cachexia •Pleural effusion •Bowel obstruction
- 22. Investigations Haematological Full blood count, biochemical profile and serum tumour markers Imaging • Pelvic and abdominal ultrasound • Chest x-ray • Other imaging modalities may be appropriate such as intravenous urogram, CT/MRI of the abdomen & pelvis
- 23. Serum Tumour Markers • CA125 - 80 percent epithelial ovarian tumour - Also increased in endometrial , pancreatic and breast cancer and benign conditions such as endometriosis , inflammatory bowel disease and hepatitis - Valuable as an early marker for disease recurrence, treatment response and early treatment failure • CA19.9 • CEA : May be elevated in stage III disease • AFP and Beta HCG - Measure if less than 40 years old to help rule out germ cell tumour
- 24. TVS • Important in evaluation of patients with a pelvic mass • Classic sonographic finding of malignancy is a complex cyst, defined as containing both solid and cystic components, sometimes with septations and internal echogenecity
- 26. CT/MRI abdomen/pelvis • Helpful preoperatively if advanced disease • Useful in assessment of retroperitoneal lymph node involvement
- 27. Staging
- 28. Staging
- 29. Staging
- 30. Staging
- 31. Staging
- 32. Staging
- 33. Staging
- 34. Treatment •The aim of Primary surgery is to : • confirm diagnosis • stage the disease • remove all cancer or optimally cytoreduce or debulk the cancer •Full staging laparotomy - Laparotomy - Hysterectomy - Bilateral salpingo-oophorectomy - Omentectomy - Lymph node sampling ( pelvic and para aortic) - Omentectomy - Pelvic washing /asciting sampling
- 35. Debulking Surgery •The current recommendation is to aim for minimum residual disease, leaving deposits with a maximum individual diameter of 1 cm
- 36. Choice of surgeon • Ovarian cancer or cases with high level of suspicion should be managed by a trained gynaecological oncologist (i.e. RMI >200)
- 37. Classification of Chemotherapy Agents Department of Obstetrics & Gynaecology, RCSI •Alkylating Agents: • impair cell function by forming covalent bonds with amino, carboxyl, sulfhydral and phosphate groups. • This alkylation occurs in DNA, RNA, and proteins. • Alkylating agents are classified according to their chemical structures and mechanisms of covalent bonds. 1. Nitrogen Mustards: cyclophosphamide,chlorambucil 2. Nitrosureas: highly lipid soluble, mainly used in brain tumours 3. Platinum complexes: carboplatin, cisplatin
- 38. Classification of Chemotherapy Agents Department of Obstetrics & Gynaecology, RCSI • Antimetabolites: are structural analogues of naturally occurring compounds. •They exert toxicity either by competing with normal metabolites or substituting for a metabolite that is normally incorporated into DNA or RNA. •They are divided as follows: 1. Folate Analogues: methotrexate 2. Purine/Pyrimidine/ Adenosine analogues: Mercaptopurine
- 39. Classification of Chemotherapy Agents •Natural Products: a variety of compounds with anti- tumour activity have been isolated from natural substances such as plants, fungi, bacteria. 1. Taxanes: Paclitaxel/Docetaxel are semi-synthetic derivatives from yew plants. They cause microtubular assembly and stability which blocks the cell in mitosis. 2. Anti-tumour antibiotics: doxorubicin 3. Epipodophyllotoxins: etoposide
- 40. Side Effects •Taxanes (Paclitaxel): bone marrow suppression, cardiotoxicity, peripheral neuropathy, rash, hair loss, mucositis, myalgia •Carboplatin: bone marrow suppression, nausea and vomiting, peripheral neuropathy, ototoxicity •Cisplatin: renal damage, nausea, vomiting, peripheral neuropathy, bone marrow depression, ototoxicity
- 41. Side Effects • Chemotherapy can have life-threatening complications. • A number of baseline investigations are performed before deciding on the most appropriate treatment regime. • Baseline investigations include: • Renal Function - 24 hour creatinine clearance • Liver Function Tests • Audiometry • Cardiac Function – echo • The treatment regime involves anti-emetics and steroids to reduce the side effects of vomiting and hypersensitivity reactions
- 42. Stage IA, IB or grade 1/2 • Do not require adjuvant chemotherapy • However they must have undergone appropriate surgical staging
- 43. Stage IC or stage IA/IB grade 3 • Adjuvant chemotherapy warranted • Paclitaxel and carboplatin is the combination regimen of choice • Those allergic to paclitaxel, combination of carboplatin and docetaxel is a suitable alternative • Recurrence rate of ovarian cancer in patient completing 6 cycles was 24% lower than those receiving 3 cycles. However the difference was not statistically significant • Six cycles associated with more toxicity (neurotoxicity , anaemia and granulocytopenia)
- 44. Stage II,III and IV ( completely or optimally debulked • Intraoperative histology to confirm ovarian ca • Surgery followed by chemo preferred • Those who are not surgical candidates, neoadjuvant Chemo should be considered • If advanced disease discovered, maximal surgical effort to debulk all tumour deposits Necessary • Those who undergo complete or optimal debulking surgery(no nodule >1cm) IP chemo with cisplatin and paclitaxel recommended.
- 45. Stage II,III and IV ( sub-optimally debulked) • Surgery followed by chemo preferred • Those who are not surgical candidates, neoadjuvant Chemo should be considered • Paclitaxel and carboplatin for 6 to 8 cycles
- 46. Platinum-sensitive recurrent disease Those who are treatment free for more than 6 months after achieving complete response post first line tx • Combination therapy with carboplatin+liposomal doxorubicin, carboplatin+paclitaxel , carboplatin +gemtricitabine
- 47. Platinum-resistant recurrent disease Those who are treatment free for less than 6 months • Palliative chemotherapy – doxorubicin liposomal, topotecan, gemcitabine, paclitaxel, bevacizumab, pemetrexed and etoposide • Palliative surgery - Colostomy - Lysis of adhesions - Management of small bowel obstruction • No universal standard • Selection based on patient factors (performance status, bone marrow reserve, quality of life)
- 48. Tumours with BRCA1/BRCA2 mutations Poly adenosine diphosphonate (ADP) ribose polymerase (PARP) act by interfering repair in cancer cells with aberrant BRCA genes Olaparib – has been approved by European Medicines Agency for women with relapsed ovarian cancer with mutations in one of the two BRCA genes who have responded to platinum based chemotherapy
- 49. Role of radiotherapy • Radiotherapy is used infrequently in the treatment of ovarian carcinoma • There is no evidence to support the use of adjuvant radiotherapy in epithelial ovarian cancer Adjuvant Whole Abdominal Radiation Therapy (WART) - Used in stage III ovarian cancer - >2cm residual - Complication of WART • Acute – diarrhea, nausea/vomiting, leukopenia, thrombocytopenia • Chronic- transient lft elevation, chronic diarrhea, basal pneumonitis, serious bowel obstruction • Can also be used for bone and brain mets
- 50. Follow-up • The ideal and most effective follow-up of asymptomatic women who have completed primary debulking surgery and chemotherapy and have no clinical evidence of disease is unclear • Current practice •Follow-up every three months in the first two years and to reduce that to six monthly interval until five years have elapsed
- 51. Palliative Care • Is a comprehensive approach towards the optimization of quality of life in patients with a life-limiting illness. Pain Management: In gynaecological malignancies patients can develop severe neuropathic pain secondary to lumbosacral plexus invasion or visceral or perineal pain. 1. Treatment of nausea, vomiting, constipation. 2. Correction of anemia 3.. Psychological issues
- 52. References 1.Malaysian National Cancer Registry Report 2007-2011 2.Björkholm Elisabet, Pettersson Folke, Einhorn Nina, Krebs I, Nilsson Bjorn, Tjernberg B. Long-term follow- up and prognostic factors in ovarian carcinoma; the radiumhemmet series 1958 to 1973. Acta Radiologica Oncol. 1982;21:413–9. [PubMed] 3.Högberg Thomas, Carstensen John, Simonsen Ernst. Treatment results and prognostic factors in a population-based study of epithelial ovarian cancer. Gynecol Onco. 1993;48:38–49. [PubMed] Society of Gynecologic Oncology 4.Sorbe Bengt, Frankendal Bo, Veress Bela. Importance of histologic grading in the prognosis of epithelial ovarian carcinoma. Obstet Gynecol. 1982;59:576–82. [PubMed] ACOG practice bulletin 5.Nice CG122 Ovarian cancer: recognition and initial management 6.BMJ best practice- ovarian cancer 7.Oxford handbook of obstetrics and gynaecology 3rd edition 8.NCCN Guidelines for Patients Ovarian Cancer version 1 2017 9. WHO classification of ovarian neoplasms. PathologyOutlines.com website. http://www.pathologyoutlines.com/topic/ovarytumorwhoclassif.html. Accessed January 26th, 2019.
