Amniotomy by dr alka mukherjee dr apurva mukherjee nagpur m.s. india
- 1. DR ALKA MUKHERJEE DR APURVA MUKHERJEE NAGPUR M.S. INDIA Amniotomy
- 2. DR ALKA MUKHERJEE MBBS DGO FICOG FICMCH PGDCR PGDMLS MA(PSY) Director & Consultant At Mukherjee Multispecialty Hospital MMC ACCREDITATED SPEAKER MMC OBSERVER MMC MAO – 01017 / 2016 Present Position Director of Mukherjee Multispecialty Hospital Hon.Secretary INTERNATIONAL COUNCIL FOR HUMAN RIGHTS Hon.Secretary NARCHI NAGPUR CHAPTER (2018-2020) Hon.Secretary AMWN (2018-2021) Hon.Secretary ISOPARB (2019-2021) Life member, IMA, NOGS, NARCHI, AMWN & Menopause Society, India, Indian medico-legal & ethics association(IMLEA), ISOPRB, HUMAN RIGHTS Founder Member of South Rapid Action Group, Nagpur. On Board of Super Specialty, GMC, IGGMC, AIIMS Nagpur, NKPSIMS, ESIS and Treasury, Nagpur for “ WOMEN SEXUAL HARASSMENT COMMITTEE.” mukherjeehospital@yahoo.com www.mukherjeehospital.com https://www.facebook.com/ Mukherjee Multispeciality https://www.instagram.com/ Achievement Winner of NOGS GOLD MEDAL – 2017-18 Winner of BEST COUPLE AWARD in Social Work - 2014 APPRECIATION Award IMA - MS Past Position Organizing joint secretary ENDO-GYN 2019 Vice President IMA Nagpur (2017-2018) Vice President of NOGS(2016-2017) Organizing joint secretary ENDO-GYN Organizing secretary AMWICON – 2019
- 3. Introduction • Amniotomy - artificial rupture of membranes (AROM) "breaking the water," - the intentional rupture of the amniotic sac by an obstetrical provider. • Common procedure during labor management. • The reasons – Multifold and include – Influencing the speed of labor, Allowing for more direct monitoring of fetal status, and Qualitative assessment of the amniotic fluid.
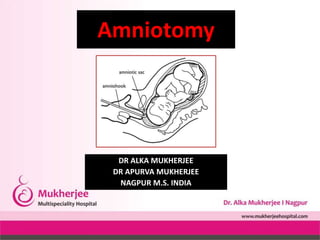
- 4. Anatomy and Physiology • The amniotic cavity is an enclosed space within the uterus in which the fetus develops and is protected during the antepartum period. • The amniotic cavity is comprised of a dual layer membrane, which includes an inner layer known as the amnion and an outer layer known as the chorion. • This potential space forms early in pregnancy and is filled with serous fluid during the first few weeks of pregnancy. • With further development of the fetus, specifically the fetal urinary system, the fluid in this potential space increases as the developing fetus excretes urine. Fetal urine comprises most of the amniotic fluid. • Typically, this barrier remains intact throughout the duration of gestation, and the amniotic membranes will spontaneously rupture, releasing the amniotic fluid either immediately preceding spontaneous labor or sometimes after the onset of spontaneous labor.
- 5. Indications • The two principal reasons for artificial rupture of membranes are (1) to induce or augment the labor process or (2) to assist in placement of internal fetal monitoring to provide the direct assessment of fetal status. Monitoring of fetal heart rate uterine activity is required during labor. (3) The amniotic membrane presents a physical impediment to this form of monitoring, and to place a fetal scalp electrode or intrauterine pressure catheter the membranes must necessarily be broken before placement.
- 6. Contraindications Few and obvious. In the case of malpresentation, Vasa previa, Suspected velamentous insertion of the umbilical cord or in case of the unengaged fetal head or unstable lie. If the fetal presentation is unknown or not fully engaged as the risk for cord prolapse is increased. If the pregnant woman is not in active labor or if the patient refuses the intervention.
- 7. Equipment • Amniotomy hook or amniotomy finger cot • Sterile gloves and lubricant. • Personal protective equipment (gloves, gown, drapes, mask, eye protection) • Absorbent pads and towels • Electronic fetal monitor (Cardiotocography CTG) • Tocolytics
- 8. Who can do it? • Obstetrician • Midwife • Delivery sister
- 9. Preparation The two most commonly used devices are (1) An approximately 10-inch rod with a hook on the end of the rod or (2) a finger cot with a hook on the end of the cot. First assess cervical dilation by p/v exam. Assess the fetal presenting part, ensure that the presenting part - the fetal head and Assess if that the fetal head is well engaged in the pelvis or not After confirmation of both fetal presentation and engagement, the dr can proceed with artificial rupture of membranes
- 10. Technique • If using the rod-hook device – • The end of the rod that remains outside of the vagina is typically held with the non-dominant hand. • The hook end of the rod is then protected between two fingers when entering the vagina. • When the practitioner can palpate the amniotic membrane and the presenting part, the non-dominant hand is used to advance the hook to the amniotic membrane. • The membrane is then snagged with the hook, and gentle traction is applied in a superior direction to tear the amniotic membrane. • Successful rupture of membranes most commonly is determined by the immediate return of amniotic fluid from the vagina.
- 11. STERILE ARM HOOK
- 12. • This fluid - usually clear and odorless , in certain cases - meconium or may be blood-tinged. • It is important to note the color of the fluid at the time of rupture. • Typically, following artificial rupture of membranes, the practitioner should not immediately remove their hand from the vagina because it is at this point that the highest risk of potential cord prolapse can occur and will be noted as the amniotic fluid continues to drain. • After the immediate flow of amniotic fluid ceases, and there is no palpable cord in the vagina, the vaginal hand then can be removed.
- 14. Complications • Complications relatively few. • Rupture of membranes does eliminate the primary barrier between the fetus and the polymicrobial environment of the vagina. • If performed too early in the labor process - increased risk of intrapartum chorioamnionitis. • The most common complication - prolapse of the umbilical cord. Specially when the head is not engaged in the maternal pelvis. • In the case of an unengaged fetal head, umbilical cord prolapse – compression of umbilical cord - fetal bradycardia and emergency cesarean section. • Easily avoidable - iatrogenic cause of emergency delivery.
- 15. Clinical Significance o Artificial rupture of membranes either can assist in inducing labor or augmenting spontaneous labor. o It relieves the amniotic sac pressure of amniotic fluid - induces uterine contraction activity, increases the strength of contractions, and may augment labor by allowing direct pressure from the fetal scalp on the uterine cervix which may assist in dilating the cervix. o While these are commonly held beliefs of many practitioners, the data to support amniotomy for these reasons is uncertain. o When there is a delay in labor, the meta-analysis suggests there is a modest reduction in the rate of cesarean section when the rupture of membranes in conjunction with the use of oxytocin is used as an early intervention.
- 17. Enhancing Healthcare Team Outcomes • Prior to the procedure, the nurse monitors the vital signs of the patient and reporting any untoward changes to Dr. • The nurse plays a vital role during the procedure in monitoring the mother as well as the fetus, she also notes the color of the draining amniotic fluid and documents the findings in the medical chart. • After the procedure - a. Assess the maternal temperature every two hours and watches out for any signs of infection. b. Monitor the fetal heart rate via continuous electronic fetal monitoring and c. Communicate the findings to the Dr d. The nurse needs to frequently change underpads.
- 18. • Nursing, Allied Health, and Interprofessional Team Monitoring • Hemodynamic status of the pregnant woman • Vital signs • Any signs of infection • Any signs of cord prolapse • Fetal heart rate • Color of the amniotic fluid (liquor)