Wound Healing
- 1. Prof. U. Murali. Wound Healing
- 2. Learning Objectives •Introduction •Phases of wound healing •Types of wound healing •Factors of wound healing •Complications
- 3. • Wound healing is a complex and dynamic biological process. • It is related to tissue reconstitution which is the process by which the body replenishes cells that are being lost. • All wounds heal following a specific sequence of phases which may overlap. • The process of wound healing depends on the type of tissue which has been damaged and the nature of tissue disruption. Introduction
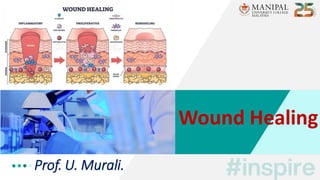
- 4. 4 • Classically, wound healing has been arbitrarily described in 3 overlapping but distinct stages / phases and include: • Inflammatory phase [ Lag / Substrate / Exudative phase ] • Proliferative phase [ Collagen / Fibroblastic phase ] • Remodeling phase [ Maturation phase ] Phases of Wound Healing
- 5. 5 • It begins immediately after wounding & and lasts 2–3 days. • Hemostasis, is often described as the immediate phase occurring before inflammation. • Hemostasis is achieved by vasoconstriction with formation of platelet plug [PT adhere, activate and aggregate] & activation of clotting pathway, resulting in formation of fibrin matrix. • The fibrin clot helps to stabilize the platelet plug and form a scaffold for migration of inflammatory cells [PMLs] into the wound. I. Phase – H & I
- 6. • In the early inflammatory phase (days 1–2), platelet activation causes an influx of inflammatory cells led by PMLs, particularly neutrophils. • Neutrophils – the first infiltrating cells to enter the wound site. • They are important for minimizing bacterial contamination of the wound, by phagocytosis. • Platelets and the local injured tissue release vasoactive amines such as histamine & serotonin, which increase vascular permeability, thereby aiding infiltration of further inflammatory cells. I. Inflammatory Phase - Early
- 7. • During the late inflammatory phase (days 2–3) monocytes appear in the wound and differentiate into macrophages. • Macrophages play a vital role in wound healing. • They function as phagocytic cells and release proteolytic enzymes to help debride the wound. • They are also the primary producer of cytokines and growth factors promoting fibroblast proliferation & angiogenesis. • Historically, this phase has been described by rubor (redness), tumor (swelling), calor (heat) and dolor (pain) – RTCD. I. Inflammatory Phase - Late
- 8. 8 • The proliferative phase starts around day 3 and lasts for 2–4 weeks. • It is during this phase that the wound continuity is re-established. • It consist mainly of fibroblast activity with the production of collagen & ground substance (glycosaminoglycans and proteoglycans). • Also, the growth of new blood vessels as capillary loops (angio-neogenesis) & the re-epithelialization of the wound surface. II. Proliferative Phase
- 9. 9 • The wound tissue formed in the early part of this phase is called granulation tissue (contains fibroblasts, macrophages & endothelial cells). • It has a pink and granular appearance. • Some fibroblasts differentiate into myofibroblasts, which are contractile cells. • These play an important role in contraction to bring the edges of the wound together. II. Proliferative Phase
- 10. • In the latter part of this phase, there is an increase in the tensile strength of the wound due to increased collagen, which is at first deposited in a random fashion and consists of type III collagen. • Initial angiogenesis occurs following release of factors from keratinocytes & macrophages. • Later re-epithelialization of the wound surface occurs by migration of basal layer of the retained epidermis which proliferates, differentiates and stratifies to form wound closure. II. Proliferative Phase
- 11. 11 • The remodeling phase begins 2–3 weeks after injury and lasts for a year (or) more. This phase is characterized by maturation of collagen. • Type III collagen, which is prevalent during proliferation, is replaced by stronger type I collagen until the normal skin ratio of 4:1 type I to type III collagen is re-established. III. Remodeling Phase
- 12. • The collagen becomes more cross-linked and uniformly aligned. • This maturation of collagen leads to increased tensile strength in the wound/scar, which is maximal 12 weeks post injury and represents approximately 80% of the uninjured skin strength. • The final matured scar is acellular and avascular. III. Remodeling Phase
- 16. 16 • Wound healing is accomplished in one of the following 3 ways – • Healing by primary intention [wounds with opposed edges] • Healing by secondary intention [wounds with separated edges] • Healing by tertiary intention [tertiary wound healing] Types of Wound Healing
- 17. • It occurs in a clean incised wound (or) surgical wound with good apposition of the edges. • The incision causes only focal disruption of epithelial BM continuity & death of a relatively few epithelial connective tissue cells. • As a result, there is more epithelial regeneration than fibrosis. • Wound heals rapidly with complete closure and leaving best scar. Scar will be linear, smooth, and supple. Primary Intention
- 18. 18 • This occurs in open wounds, particularly when there has been significant loss of tissue, or wounds with irregular margins. • Regeneration of parenchymal cells cannot completely reconstitute the original architecture. • It heals slowly with fibrosis. It leads into a wide scar, often hypertrophied and contracted. It may lead into disability. Secondary Intention
- 19. • Delayed primary healing occurs when the wound edges are not opposed immediately, which may be necessary in contaminated or untidy wounds. • After debridement of non-viable tissue and when the wound is clean, the wound edges may be surgically approximated. This is also called healing by tertiary intention. • Primary contaminated or mixed tissue wounds heal by tertiary intention. Tertiary Intention
- 22. 22
- 24. • Various factors can adversely affect wound healing and include – •Local Factors •Systemic / General Factors Factors - Wound Healing
- 55. Complications – W H • Excessive Scar Formation: Hypertrophic scar, Keloid. • Deficient Scar Formation: Result in wound dehiscence [or] rupture of the wound due to inadequate formation of granulation tissue. • Exuberant Granulation (Proud Flesh): Excessive GT that protrudes above the skin level. • Deficient contraction – Skin grafts Excessive contraction – In Burns • Others: Pigmentary changes, Incisional hernia, Dystrophic calcification, Neoplastic changes.
- 56. 56 • Phases of wound healing. • The changes in each phases - pathophysiology. • Types of wound healing. • Factors affecting wound healing – Local & Systemic factors. • Complications of wound healing. To Summarize
- 57. References
- 58. • Explain the first phase of wound healing. • List 4 differences between 1 & 2 union of wound healing. • Enumerate 5 local factors affecting wound healing. • Mention the complications of wound healing. • Write about tertiary intention. • Illustrate with flow-chart the phases of wound healing. • Describe the nutritional deficiencies affecting wound healing. • Write the stages of wound healing. Question Time
- 59. Factors impairing wound healing include all the following, except – ◼ a) Excessive tension. ◼ b) Lack of hemostasis. ◼ c) Inversion of wound edges. ◼ d) Drains. ◼
- 60. The tensile strength of the wound starts and increases after – ◼ a) Immediate suture of the wound. ◼ b) 3 – 4 days. ◼ c) 7 – 10 days. ◼ d) 6 months. ◼
- 61. Which one of the following cells plays an important role in bringing the edges of the wound together? – ◼ a) Myofibroblasts. ◼ b) Macrophages. ◼ c) Polymorphonuclear leukocytes. ◼ d) Fibroblasts. ◼
- 62. Factors that may adversely affect the healing of wounds include all the following, except – ◼ a) Exposure to radiation. ◼ b) Advanced neoplasia. ◼ c) Exposure to UV light. ◼ d) Obstructive jaundice. ◼
- 63. When is the maximum collagen content of wound tissue? – ◼ a) 2 – 5 days. ◼ b) 6 – 10 days. ◼ c) 11 – 16 days. ◼ d) 17 – 21 days. ◼
- 64. 64
