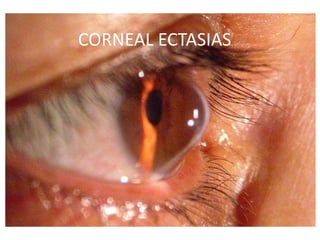
Corneal ectasias
- 2. CORNEAL ECTASIAS • It is a group of diseases affecting the corneal shape due to CORNEAL THINNING. – Anterior Keratoconus – Keratoglobus – Pellucid Marginal Degeneration – Posterior Keratoconus • Key Features: – Usually Bilateral, often asymmetrical – Isolated to cornea – Non inflammatory
- 3. KERATOCONUS • Progressive corneal steepening, typically inferior to the centre of the cornea. • Non inflammatory, usually bilateral. • Incidence: Between 50 and 230 per 100 0001. • Unilateral involvement is 2–4%2. • Onset starts at the age of puberty. 1. Krachmer JH, Feder RS, Belin MW. Keratoconus and related noninflammatory corneal thinning disorders. Surv Ophthalmol. 1984;28:293–322. 2. Holland DR, Maeda N, Hannush SB, et al. Unilateral keratoconus. Incidence and quantitative topographic analysis. Ophthalmology.1997;104:1409–1413.
- 4. ASSOCIATED DISEASES Systemic Atopic Diseases (35%)1. Down’s Syndrome (5.5-15%)2. Ehler-Danlos and osteogenesis imperfecta. Mitral valve prolapse. Marfan Syndrome. Ocular Vernal Conjunctivitis. Retinitis Pigmentosa. Leber’s congenital amaurosis Retinopathy of prematurity. Fuchs’ Dystrophy. 1. Rahi A, Davies P, Ruben M, et al. Keratoconus and coexisting atopic disease. Br J Ophthalmol. 1977;61:761–764. 2. Cullen JF, Butler HG. Mongolism (Down’s syndrome) and keratoconus. Br J Ophthalmol. 1963;47:321–330.
- 5. ETIOLOGY BIOCHEMICAL: • Up-regulation of degradative enzymes (acid esterase and acid phosphatase, cathepsins B and G, and some matrix metalloproteinases) and the down-regulation of proteinase inhibitors. • There is a four fold increase in the receptors of INTERLEUKIN 1 causing apoptosis of stromal keratocytes. • Microtrauma Release of IL-1 from epithelial epithelium.
- 6. HEREDITY • Autosomal dominant with incomplete penetrance. • Frequency of inheritance is 6%. • Keratoconus prevalence in first-degree relatives to be 3.34%, about 68 times that found in the general population. PATHOLOGY • Keratoconus can involve every layer and tissue of cornea. • Superficial cell enlargement and prominence of elongated cells in the corneal epithelium.
- 7. Early degeneration of basal epithelial cells. Disruption of epithelial basement membrane. Epithelium grows posteriorly into the Bowman’s Layer, with collagen growing anteriorly into the epithelium. Z shaped interruptions at the level of the basement membrane. Fragmentation of the Bowman’s layer. (Early change)
- 8. Fleischer ring found at the base of the cone is a hallmark of keratoconus. Breaks in Bowman’s layer fill with scar tissue. Fine scars consolidate leading to formation of reticular branched opacities at this level. Collagen lamellae are released from their interlamellar attachments or from their attachments to Bowman’s layer and become free to slide Thinning without collagenolysis.
- 9. Alteration of the normal orthogonal arrangement of the collagen fibrils leads to stromal tissue instability. Most common location for the apex of the cone, in the central or inferior cornea, isrelated to this. Endothelial cell pleomorphism and polymegathism
- 10. DIAGNOSIS • Onset of the disease is at puberty. • Usually appears in the 2nd or 3rd decade. SYMPTOMS: • Progressive visual blurring & disortion due to irregular astigmatism. • Frequent change of glasses. • Pain, photophobia. • Eye rubbing.
- 11. Scissoring of red reflex on retinoscopy One of the earliest signs SIGNS:
- 12. Munson Sign Buldging of the lower eye lid in downward gaze.
- 13. Papillae, trantas dots, limbal nodule, pigmentation, ropy discharge.
- 15. Corneal ectasia: Apex is inferior to the horizontal line to the pupillary axis. Corneal thinning of about 1/2-1/5 is observed at the apex. 2 types of cones: Round/ Nipple shaped Oval shaped
- 16. Fleischer Ring Iron depositions in the corneal epithelium. The ring configuration is due to irregular distribution of tears at the base of the cone and resultant deposition.
- 17. Vogt’s Striae Fine vertical lines formed due to compression of descemet’s membrane. Parallel to the axis of the cone
- 20. • Breaks in Descemet Membrane • Stromal edema
- 21. Charleux Sign Dark reflex in the area of the cone on observation of the cornea with pupil dilated using a direct ophthalmoscope set on plano.
- 22. DIFFERENTIAL DIAGNOSIS • Pellucid marginal degeneration. • Keratoglobus. • Post traumatic corneal ectasia. • Protrusion of cornea subsequent of corneal thinning from ulceration. • Corneal ectasia following keratorefractive surgery.
- 23. CLASSIFICATION
- 25. INVESTIGATIONS • KERATOMETRY: Mires are commonly steep, highly astigmatic, often egg shaped. Inability to superimpose the central keratometric rings is due to irregular astigmatism. (hallmark) LIMITATIONS: Provides information only of the central 3mm of cornea. Not useful in irregular astigmatism.
- 26. • VIDEOKERATOMETRY Based on Placoid disc principle. Early disease: Isolated area of smaller ring spacing and distortion. Advanced disease: Decrease in overall ring spacing and becomes increasingly irregular LIMITATIONS: Does not give accurate information about the posterior curvature and corneal thickness. Cannot detect early keratoconus.
- 27. Astigmatism progression: Symmetric Bow tie pattern Asymmetric appearance Inferotemporally displaced steep sided cone
- 28. • ORBSCAN Uses the principle of scanning slit combined with a Placoid system. Provides reliable information about the anterior and posterior elevation and best fit sphere and a corneal pachymetry map. LIMITATIONS The posterior curvature map might not be 100% accurate. Requires patient fixation for accurate data. Data pertaining to the central cornea is not accurate.
- 30. • PENTACAM USES a rotating Scheimpflug camera. Provides reliable data of anterior and posterior corneal elevation and accurate measurement of corneal thickness. The images taken by a pentacam maintain the central point of each meridian hence the software can re register these central points and eliminate the eye movement. Data is 10 times more accurate than the that obtained from Orbscan.
- 33. • PACHYMETRY Ultrasonic and optical based devices can be used. Measurement of corneal thickness is useful for diagnosis, documenting progression, and planning treatment. • OCULAR RESPONSE ANALYSER Helps in making a diagnosis and classifying by assessing corneal hysteresis and resistance.
- 35. TREATMENT • NON SURGICAL – Spectacles: Only in early cases. • Once irregular astigmatism develops this type of visual correction cannot be used. – Contact lens: Soft toric lenses, standard bicurved hard lenses, custom back toric lenses, piggyback systems, hybrid lens, scleral and mini scleral lens.
- 36. RIGID GAS PERMEABLE LENS • First choice in correcting irregular astigmatism. • Fitting strategies: Apical clearance: There is no touch in the apical area. Advantage: 1. Reduced risk of scarring 2. Whorled keratopathy 3. Corenal erosion Limitation: Hampers tear exchange, edge can come in visual axis. Rarely used now days.
- 37. Apical touch : Aims at providing primary lens support at the apex of the cornea. The central optic zone of the lens touches the central cornea. ADVANTAGE: Better quality of vision LIMITATION: Corneal scarring and intolerance over long term use. Three point touch: Most popular technique The lens bearing is shared between apex and mid peripheral cornea. Minimizes apical scarring, better comfort and longer wearing time.
- 38. PIGGYBACK LENS SYSTEM • Consists of the fitting a rigid gas permeable on top of a soft contact lens. • The soft lens is used to improve wearing comfort and provide a more regular area for the gas permeable contact lens to sit. • The gas permeable contact lens is used for providing adequate visual acuity.
- 40. HYBRID CONTACT LENS • Contain a rigid gas permeable center with a soft skirt. • They are fitted with no or minimal apical touch in the central cornea. ADVANTAGE: Can be fit on cones of any severity. LIMITATION: Can cause hypoxia related changes like vascularisation and central corneal clouding.
- 42. ROSE K LENSES • Multicurve lenses with small optical zone which fits snugly over the cone. • Rose K contact lens provides greater comfort, better quality of vision and requires lesser chair time. • Rose K2 IC is a larger diameter, intralimbal lens that can be used for oval cones.
- 43. SCLERAL LENSES • They rest on the sclera without touching the cornea or the limbus leaving a clear area between the contact lens and the cornea. • They are of two types: – Prosthetic Replacement Of the ocular Surface Ecosystem (PROSE) – Boston Ocular Surface Prosthesis (BOSP)
- 44. ADVANTAGE Good centration, stability and improved Visual acuity. Extermely useful in patients with advanced ectasias who are intolerant to contact lenses or when immediate surgery is not possible LIMITATION High cost, reduced tear exchange and difficult insertion and removal.
- 45. • SURGICAL MANAGEMENT – INTRACORNEAL RING SEGMENT INSERTS – CORNEAL CROSS LINKAGE – LENTICULAR REFRACTIVE SURGERY – CORNEAL TRANSPLANT
- 46. INTRACORNEAL RING SEGMENT INSERTS • Ferrara rings: Fixed inner diameter of 5.00 mm with a triangular anterior contour. • Intacs: Inner diameter of 6.8 mm and a flat anterior contour. Hexagonal in cross section. Intacs SK: Inner diameter of 6.00 mm and elliptical cross section. The ring segments should be inserted upto 2/3rd depth of the cornea. Minimum corneal thickness should be 450 µ. They do not prevent the progression of the disease.
- 47. The technique involves the implantation of one of two polymethy metha acrylate segments in the stroma to flatten the central cornea. Intralamellar pockets are created with the help of a vaccum lamellar dissector or femtosecond laser.
- 48. CORNEAL COLLAGEN CROSSLINKING • The most recent addition to surgical management. • It may slow or halt the progression with photo- oxidative treatment to increase the rigidity of the corneal stroma. • 60-70% patients show some stabilization following this treatment. • The therapeutic effects are limited upto 300 µ of the anterior stroma. • This technique should not be performed for corneas less than 400µ in thickness. • It carries a slight risk of development of keratitis.
- 49. STEPS: Under topical anaesthesia 6-7 mm of central corneal epithelium is removed. Riboflavin 0.1% solution is applied topically (10-30 mins) and cornea is irradiated with UVA light of 370 nm for 30 mins. Production of reactive oxygen species helps create covalent bonds between collagen fibrils.
- 52. CORNEAL TRANSPLANTATION Penetrating Keratoplasty: Success rate in 90-95%. Visual recovery takes several weeks to months. Full stabilisation might even take a year. Hydrops that does not clear by 3-4 months is best treated by Penetrating keratoplasty.
- 53. DEEP ANTERIOR LAMELLAR KERATOPLASTY • It is the procedure of choice as there is good endothelial count even after hydrops. • Advantages over Penetrating keratoplasty: Reduced risk of Rejection Reduced risk of Endopthalmitis Greater wound stability Reduced need for topical steroids Faster healing
- 54. LAYER BY LAYER MANUAL DISSECTION Partial trephination of variable depth ranging from 50-70% of corneal thickness, stroma is removed with the help of a crescent. Layer by layer removal of the stroma to reach as close to the Descemet’s membrane. LIMITATION: Poor visual outcome due to residual stroma and interface haze.
- 55. AIR ASSISTED DALK Archila first described this technique involving air injection to achieve dissection as close to DM as possible. The Big bubble technique was described by Anwar and Teichmann and is the most widely used technique. Steps: Air injection into the stroma through a groove created by trephining 60-80% of the stromal thickness. Air infiltrates the potential space between deep stroma and DM and creates a Dome shaped detachment of DM. Once the plane of separation is created the stroma can be easily excised.
- 56. FEMTO LASER ASSISTED DALK It can be used to create corneal incisions with customised graft edges and lamellar planes for both donor and recipient corneas. ADVANTAGE: Accuracy of forming the bubble at desired corneal depth Positive refractive outcome LIMITATIONS: Cost and availability
- 57. KERATOGLOBUS • Bilateral ectatic disorder which is non progressive or minimally progressive. • Generalised thinning with marked peripheral thinning. • Types: – Congeital: Ehler’s-Danlos type IV and brittle cornea syndrome. – Acquired: Initially keratoconus keratoglobus.
- 59. Clinical Features Blurring of vision. Corneal perforation spontaneous or following minimal trauma. Rarely might present as photohobia, glare, pain, conjunctival injection following acute hydrops. Limbus- limbus corneal thinning Blue sclera due to thinning
- 60. Differential Diagnosis Keratoconus Pellucid Marginal Degeneration Megalocornea Congenital glaucoma
- 61. Investigations Diagnosis is essentially clinical. Ultrasonic Pachymetry shows reducude corneal thinckness. Corneal Topography shows generalised thinning and irregular astigmatism is difficult to perform in advaced cases .
- 62. Management Conservative: Observation is the rule in early cases. Patient is advised to use polycarbonate glasses. Visual rehab is done using refractive correction for high myopia. Scleral lens, rigid gas permeable lens, reverse geometry hydrogel lens, large diameter inverse geometry rigid gas permeable lenses can be used.
- 63. Surgical Management It is difficult to manage these patients by surgery: Large sized grafts are required increasing the risk of rejection. Peripheral sutures often cut through. Proximity of the graft to the limbus increases risk of rejection. Higher chances of perforation.
- 64. PELLUCID MARGINAL DEGENERATION • Bilateral corneal ectatic disorder. • Band of thinning 1-2mm in diameter extending from 4 to 8 o’clock. • Area of thinning is separated from the limbus by 1-2mm of normal cornea. • Onset: 2nd- 5th decade of life. Beer Belly appearance
- 65. • Blurring of vision due to against the rule astigmatism. • Frequent chances of glasses. • Ocular examination reveals thinning of inferior cornea with 1-2 mm separation from the limbus. • Ectasia is just superior to the thinning. • Protruding cornea is of normal thickness. • Occasional concentric Descemet folds seen inferiorly.
- 66. Investigations • Corneal topography: Inferior peripheral steepening extending into the mid periphery. Crab- claw appearance. Against the rule: Superiorly. With the rule: Inferiorly.
- 67. Management • Spectacles in early cases. • PROSE, BOSP and hybrid contact lens can be used. • Large diameter Penetrating keratoplasty. • Combined Lamellar with penetrating keratoplasty. • Crescentric lamellar keratoplasty. • Crescentric or wedge excision if ectasia in small sector.
- 68. POSTERIOR KERATOCONUS • It is a congenital corneal anomaly in which the posterior corneal surface protrudes into the stroma. • Sporadic, unilateral, non progressive. • Variant of corneal mesenchymal dysgenesis. • Scarring is seen anterior to the descemet bulge. • Pathologic Examination: Scarring at Bowman’s membrane and thinning of descmet membrane with excrescences.
Editor's Notes
- Scarring of Bowman’s layer and the anterior stroma are common and correlate histopathologically with collagen fragmentation, fibrillation, and fibroblastic activity.
- Arrow head pattern
- Lysyl hydroxylase activity normal in brittle cornea synd