MD61 Group2 - Chronic Venous Insufficiency (Presentation).pdf
- 2. Chronic Venous Insufficiency Keywords: Varicositas, Varicose vein, Venous Insufficiency, Venous Reflux Disease, Chronic venous disease (CVD), Valvular Incompetence, Subj: Hospital Surgery II Prof. MOK THEAVY, DES Group 2
- 3. Member Hon Makara (1) Definition (2) Epidemiology (4) Physiology Anatomy Hel Siyean (5) Pathophysiology (6) Clinical Feature (8) Diagnosis Ro Sophara (9) Differential Diagnosis (10) Management Measrithsomaly Sreypich (11) Complication (12) Prognosis Map Ratanakvattey (3) Classification Yi Bunyong (7) Etiology
- 4. Content 1). Definition 2). Epidemiology 3). Classification 4). Physiology Anatomy 5). Pathophysiology 6). Clinical Feature 7). Etiology 8). Diagnosis 9). Differential Diagnosis 10). Management 11). Complication 12). Prognosis
- 5. Overviews What is a Venous Disorder? Acute venous diseases Chronic venous diseases 1) Leg vein thrombosis 2) Vein inflammation (phlebitis) 1) Spider veins 2) Varicose veins 3) Vein weakness: Venous insufficiency 4) Leg ulcer (ulcus cruris venosum)
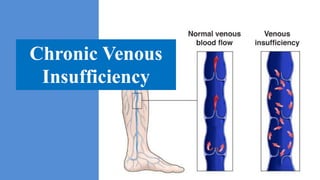
- 6. I. Definition • Chronic venous insufficiency (CVI) refers to functional changes that may occur in the lower extremity due to persistent elevation of venous pressures. • This most commonly results from venous reflux due to faulty valve function developing as a long-term sequela of deep vein thrombosis (DVT) and recanalisation and may also develop due to primary valvular incompetence without previous episode(s) of DVT. • The term 'CVI' is usually reserved for more advanced disease involving oedema, skin changes, or frank ulcers. • Varicose Vein: Varicose veins are subcutaneous, Permanently dilated veins 3 mm or more in diameter when measured in a standing position; however, they may not be visible. • Varicosity (Plural varicosities): An enlarged vessel or nerve, particularly a blood vessel.
- 7. II. Epidemiology Chronic venous insufficiency: • CVI affects about 7% of the population. • Prevalence of venous leg ulcers, the most extreme form of • CVI, has been estimated to range from 1% to 2%. • Following treatment, up to 7 in 10 wounds recur. • The total cost of treating venous leg ulcers in the US alone was $3 billion in 2006.
- 8. Varicose veins: • Generally, prevalence rates are higher in industrialised countries and in more developed regions. • Prevalence of visible varicose veins in the Western population aged over 15 years is 10% to 15% in men and 20% to 25% in women. • Prevalence rates in the US are 15% (range from 7% to 40%) in men and 27.7% (25% to 32%) in women. • Visible varicose veins are more prevalent in Hispanic people (26.3%) and less prevalent in Asian people (18.7%). Mortality Prevalence
- 9. III. Physiology Anatomy • Capillaries and Venules, collect the used, oxygen-depleted blood from the muscles and organs. • Venous Return: Heart and Breathing, The venous valves, calf muscle pump, Vein tension and vein dilation. • Venous Flow: Saphenous veins (Greater, Smaller), Popliteal vein. • Venous Type: Deep veins, Superficial veins, Perforating veins. • Gravitational effects • Blood flow travel against gravity: valves, muscle pumps. • Venous valve function: Opening, Equilibrium, Closing, Closed. • Contraction • Relaxation (muscle pump) allows blood to refill to the deep venous system.
- 10. Venous Pressure • Normal Venous Pressure (Refill Time > 20 seconds) (1) Resting Standing Pressure: 80 – 90 mmHg (2) Drop in Exercise: 20 – 30 mmHg • Abnormal Venous Pressure (Refill Time < 20 seconds) (1) Resting Standing Pressure: Higher than normal (2) Drop in Exercise: Blunt (decrease 50%) • Abnormal Venous Pressure , Venous Obstruction (1) Resting Standing Pressure: Higher than normal (2) Not-Drop in Exercise
- 11. IV. Clinical Feature Common: 1) Corona phlebectatica (malleolar flare or ankle flare) 2) Ankle swelling 3) Hyperpigmentation 4) Lipodermatosclerosis 5) Atrophie blanche 6) Leg ulcers Uncommon: 1) Leg fatigue, aching, and/or discomfort 2) Heavy legs 3) Leg cramps 4) Telangiectasias 5) Reticular veins 6) Dilated tortuous veins 7) Dry and scaly skin Atrophie blanche: • L'atrophie blanche est la traduction clinique d'une ischémie cutanée par occlusion localisée des petits vaisseaux du derme superficiel.
- 12. Telangiectasias • Telangiectasias are small, widened blood vessels on the skin. • They are usually harmless, but may be associated with several diseases. Reticular veins • Reticular veins are the visible veins below your skin that appear blue-purple in colour, • They don't bulge out as varicose veins do. Telangiectasias
- 13. Corona phlebectatica: • Corona phlebectatica is a cutaneous sign of chronic venous insufficiency, characterized by abnormally dilated veins around the ankle. • It is characterised by the presence of abnormally visible cutaneous blood vessels at the ankle with: 1) Venous cups 2) Blue and red telangiectasis 3) Capillary stasis spots
- 14. V. Etiology • Primary varicose veins are thought to be due to genetic or developmental defects in the vein wall that cause 1) Diminished Elasticity 2) Valvular Incompetence. • Secondary varicose veins arise from destruction or dysfunction of valves caused by: 1) Trauma 2) Deep Venous Thrombosis 3) Arteriovenous Fistula 4) Nontraumatic Proximal Venous Obstruction (Pregnancy, Pelvic Tumor)
- 15. • Severe CVI usually results from: 1) Chronic Valvular Reflux 2) Venous Obstruction 3) Frequently from a combination of both.
- 17. Arteriovenous Fistula (1) Arteriovenous (AV) fistula is an irregular connection between an artery and a vein. (2) Blood flow avoids tiny blood vessels (capillaries) and moves directly from an artery into a vein. (3) Arteriovenous (AV) fistula is an irregular connection between an artery and a vein. (4) Due to: Injuries that pierce the skin, Congenital arteriovenous fistulas, Genetic conditions, Dialysis-related surgery.
- 18. Trauma
- 19. Pregnancy
- 20. Pelvic Tumor
- 21. VI. Physiopathology • Chronic Venous Insufficiency, Retrograde blood flow. • Venous Return ( calf and foot muscle pumps, patent veins, and competent valves). • Venous insufficiency or Chronic Venous Insufficiency (CVI). • Venous Reflux
- 22. Venous Reflux (1) • Venous Reflux or Retrograde flow of blood serves to increase hydrostatic pressures. • Valve Incompetence lead to rapid refill and accumulation of fluid. • This excessive local pressure can produce dilatation of the superficial veins. • Hydrostatic pressures: Vessel wall is thin, direct injury or Superficial phlebitis.
- 23. Venous Reflux (2) • Abnormal capillaries: accumulation of fluid, macromolecules, and extravasated red blood cells into the interstitial space (oedema). • The typical constellation of findings that ensue include: 1) Oedema 2) Lipodermatosclerosis 3) Ulceration 4) Hyperpigmentation • Microangiopathy: Macrocirculation > Venous microangiopathy.
- 24. Microangiopathy • There have been several postulated mechanisms for the development of Venous Microangiopathy, including: 1) Fibrin Cuff Hypothesis 2) White Blood Cell Trapping
- 25. • Fibrin Cuff Hypothesis , venous hypertension with resultant extravasation of plasma proteins and fibrinogen into the soft tissue, resulting in a fibrin cuff around the capillaries and Tissue Hypoxia. (1) Venous hypertension (2) Fibrinogen leaks from the capillaries (3) Fibrinogen coagulates and hardens to form a fibrin cuff (4) Cuff surrounds the capillaries (5) Cuff establishes a barrier that prevents oxygen and nutrients (6) Skin cannot reach of oxygen and nutritional (7) Tissue hypoxia
- 26. • White cell trapping that white cells are trapped in capillaries due to venous hypertension, with secondary escape of proteins into the interstitial space and resultant Diminished Tissue Oxygenation. (1) Increase Venous Blood Pressure (2) Leukocyte surrounding tissue and attack to vessel wall. (4) When, leukocytes are activated and releasing of pro-inflammatory and cytokine. (5) Then, present as ulceration. (6) Chronic Inflammatory State / Chronic Venous Insufficiency
- 27. • After Ulceration / Cell Injury / Subcutaneous • Lipodermatosclerosis characteristically results from capillary proliferation, fat necrosis, and fibrosis of the skin and subcutaneous tissues. (1) Hypertension leads to an increase of leukocytes in the veins, which migrate to surrounding tissue. (2) Leukocytes are activated, releasing proinflammatory cells and cytokines, inducing a chronic inflammatory state. (3) Increased collagen production leads to the fibrosis of subcutaneous fat. Lipodermatosclerosis
- 28. Hyperpigmentation • Hyperpigmentation (usually a reddish-brown discoloration) of the ankle and lower leg is also known as brawny oedema. • It results from extravasation of blood and deposition of haemosiderin in the tissues due to long-standing ambulatory venous hypertension. (1) Hemosiderin (Protein Compound) (2) Red Blood Cell contain Hemoglobin (3) Hemoglobin carry Oxygen & Iron (4) RBC breakdown, releasing of Iron from hemoglobin. (5) Accumulated fluid lead to Iron Trap upper skin tissue.
- 29. Physiopathology (2): Varicose Veins • The venous system acts as both a reservoir and a conduit in the return of blood to the heart and lungs for oxygenation and re-circulation. • End capillary venous pressure is low (20 mmHg). Veins are thin-walled and lack the muscular walls of arteries. • Therefore, veins require assistance in blood return. This is provided by valves and muscle pumps - as one walks, the muscle pumps contract and push blood against gravity, and as the muscle pump relaxes, the fall of the blood is stopped by the valve system. • When one of these factors is not functioning properly, venous hypertension and insufficiency can ensue, possibly leading to varicose veins. • A normal vein wall has three smooth muscle layers that all help to maintain its tone. • Varicose veins demonstrate marked proliferation of collagen matrix as well as decreased elastin, leading to distortion and disruption of muscle fibre layers.
- 30. IV. Classification Revised CEAP criteria: • C = Clinical class • E = Etiology • A = Anatomy • P = Pathophysiology
- 31. Clinical (C) • C0: No visible sign of venous disease • C1: Telangiectases or reticular veins • C2: Varicose veins • C3: Edema • C4: Changes in skin and subcutaneous tissue C4a: Pigmentation or eczema C4b: Lipodermatosclerosis or atrophie blanche • C5: Healed ulcer • C6: Active ulcer
- 32. Etiologic (E) • Ec: Congenital (eg, Klippel-Trenaunay syndrome) • Ep: Primary • Es: Secondary (eg, postthrombotic syndrome, trauma) • En: No venous cause identified
- 33. Anatomic (A) • As: Superficial • Ad: Deep • Ap: Perforator • An: No venous location identified
- 34. Pathophysiologic (P) • Pr Reflux • Po Obstruction, thrombosis • Pr,o Reflux and obstruction • Pn No venous pathophysiology identified
- 35. Venous Disorder Stages • Stage 0: No signs that can be seen or felt (like achy or tired) • Stage 1: Visible blood vessels, including spider veins. • Stage 2: Varicose veins at least 3 millimeters wide. • Stage 3: Edema (swelling) but no skin changes. • Stage 4: Changes to your skin’s color and/or texture. • Stage 5: Healed ulcer. • Stage 6: Acute (active) ulcer.
- 38. VII. Diagnosis 1). Clinical Feature 2). Physical Examination 3). Noninvasive Testing a) Venous Duplex Imaging b) Air Plethysmography c) Computed Tomographic or Magnetic Resonance Venography d) Other Techniques 4). Invasive Testing a) Contrast Venography b) Intravascular Ultrasound c) Ambulatory Venous Pressure
- 39. Clinical Feature (1) Symptomatic (2) Major (3) Congenital
- 40. Symptomatic 1) Heavy legs, leg fatigue, aching, and/or discomfort. 2) Burning and itching of the skin and leg cramps.
- 41. Major • CVI present with: 1) Dilated veins, varicose vein, tenderness 2) Edema 3) Leg pain 4) Cutaneous changes in the leg.
- 42. Congenital • Congenital disorders are those that are present at birth but may be recognized later in life. • These include the well-recognized syndromes of: (1) Klippel-Trénaunay Syndrome (varicosities and venous malformations, capillary malformation, and limb hypertrophy) and (2) Parkes-Weber (venous and lymphatic malformations, capillary malformations, and arteriovenous fistulas).
- 43. Klippel-Trénaunay Syndrome • A newborn boy was noted to have a diffuse erythematous rash at birth. • He had been born at 40 weeks of gestation to a 19-year- old gravida 2, para 2 mother who had had adequate prenatal care. • The pregnancy had been complicated by chlamydia infection with documented cure after treatment, anemia, and an episode of self-limited hives. • He had been born by spontaneous vaginal delivery and had Apgar scores of 8 at 1 minute and 9 at 5 minutes. • Physical examination findings were remarkable for a diffuse erythematous macular rash with blanching on his trunk and extremities. https://www.consultant360.com/article/consultant360/kl ippel-trenaunay-syndrome Diffuse Erythematous Macular Rash
- 44. Klippel-Trénaunay syndrome Lymphorrhea Capillary-venolymphatic Malformation (CVLM) Link: https://www.compva.com/patientexamples/klippel-trenaunay-syndrome-lymphorrhea
- 45. Link: https://www.nejm.org/doi/full/10.1056/NEJMicm1312948 Parkes-Weber Syndrome • Fingertip ulcers • Arteriovenous malformation of the left arm • Hypertrophy, with a giant arteriovenous malformation (Fingers, forearm, elbow, and upper arm) • Enlarged and tortuous arteries and veins Parkes Weber syndrome consists of: venous and capillary malformations
- 46. Physical examination • Sign • Tourniquet Test (1) Brodie-Trendelenburg Test (2) Perthes Test (3) Delbet-Mocquot test (4)
- 47. Sign 1) Early signs of CVI: Telangiectasias, Reticular Veins, Corona Phlebectatica 2) Palpation for bulges consistent with varicose veins. 3) Ankle swelling (usually unilateral but may be bilateral) due to oedema is also common. 4) Severe CVI: Atrophie blanche, Lipodermatosclerosis, and Hyperpigmentation. 5) Venous ulcers are located in the gaiter area.
- 48. • CVD represents a spectrum of conditions ranging from simple telangiectases or reticular veins to more advanced stages, such as skin fibrosis and venous ulceration. Leg venous ulceration
- 49. Brodie-Trendelenburg Test • Patient's leg is elevated to drain venous blood. • Elastic Tourniquet (saphenofemoral junction mid thigh and the patient then stands) • Rapid filling (<30 seconds) of the saphenous system from the deep system indicates perforator valve incompetence. • When tourniquet is released, additional filling of the saphenous system occurs if the saphenofemoral valve is also incompetent.
- 50. (1) Negative Varicose Vein • Patient standing with tourniquet, Varicose is not appearing • If elastic tourniquet is release and varicose vein is not appearing • Called: Negative Varicose Vein (2) Positive Varicose Vein • Patient standing with tourniquet, Varicose is not appearing • If elastic tourniquet is release and varicose vein is appearing • Due to Perforating Vein Incompetence • Called: Positive Superficial Varicose Vein (3) Double Positive Varicose Vein • Patient standing with tourniquet • Elastic tourniquet is not release but varicose vein is appearing • Called: Positive Deep Varicose Vein
- 51. Brodie-Trendelenburg Test Watch1: https://www.youtube.com/watch?v=b5l3PcoZ65A Watch2: https://www.youtube.com/watch?v=UAtO1Zt-ydg
- 52. Perthes Test • Purpose assess patency of the deep femoral vein. • German surgeon Georg Perthes. (1) The limb is elevated and an elastic bandage is applied firmly from the toes to the upper 1/3 of the thigh to obliterate the superficial veins only. (2) With the bandage applied the patient is asked to walk for 5 minutes. (3) If deep system is competent, the blood will go through and back to the heart. (4) If the deep system is incompetent, the patient will feel pain in the leg.
- 53. Delbet-Mocquot test • French physicians Pierre Delbet and Pierre Mocquot.
- 54. Noninvasive Testing A variety of techniques may be employed to investigate patients with CVI: 1) Duplex Ultrasound 2) Ascending phlebography 3) Computed tomography (CT) and Magnetic Resonance Venography 4) Intravascular ultrasound (IVUS) 5) Air plethysmography
- 55. Duplex Ultrasound • Speed of blood flow, and structure of the leg veins. • Localize sites of obstruction and valvular reflux (deep and superficial venous systems). • Goal: Venous Reflux, Retrograde or reversed flow, valve closure time >0.5 seconds.
- 60. Invasive Testing Ambulatory Venous Pressure • Gold standard assessment. • Insert needle to dorsal foot vein with transducer. • Detect: Refill time and Leg Pressure
- 64. VIII. Differential Diagnosis 1) Diabetic foot ulcer 2) Arterial ulcer 3) Squamous cell carcinoma (Marjolin) 4) Pyoderma gangrenosum 5) Kaposi's sarcoma 6) Lymphoedema 7) Congestive heart failure 8) Renal disease 9) Hepatic disease • Excluded: 1) Acute Venous Problem 2) Deep Vein Thrombosis • Included: 1) Heart failure 2) Nephrosis, 3) Liver 4) Endocrine disorders Oedema
- 65. IX. Management (*) Early Management: 1) Wound and Skin Care 2) Pharmacologic Therapy 3) Compressive Leg Garments (*) Prevention: • Exercise Therapy • Conservative Management (*) Interventional Management: a) Superficial venous reflux (Saphenectomy, Endovenous laser therapy, Foam sclerotherapy) b) Endovenous Ablative Therapy c) Endovenous Deep System Therapy d) Surgical Management e) Surgery for Truncal Vein f) Perforator Vein Surgery g) Valve Reconstruction
- 66. Wound and Skin Care • Moisturiser: moisturising cream to combat skin dryness and flaking in eczematous skin changes and mild stasis dermatitis is generally thought to be beneficial.
- 67. Compressive Leg Garments • Graded Compression Stockings: CVI-related oedema, stasis dermatitis, and small venous leg ulcers is use of graded compression knee-high stockings.
- 68. Pharmacologic Therapy 1) Eczematous skin changes and mild stasis dermatitis 2) Venous leg ulcers 3) Leg pain • Pentoxifylline or Diosmin: Pentoxifylline is used to treat claudication, 400 mg orally three times daily.
- 69. Pentoxifylline • Classes: Hemorheologic Agents • Dosage Forms: 400mg • Intermittent Claudication: Effects may be seen within 2-4 weeks; recommended to continue treatment for at least 8 weeks. • Contraindications: Recent retinal or cerebral hemorrhage. Diosmin is most often used for hemorrhoids and leg sores caused by poor blood flow. • Side effects: stomach pain, diarrhea, dizziness, headache, skin redness and hives, muscle pain, blood problems, and altered heart rate.
- 70. Interventional 1. Superficial venous reflux Saphenectomy, Endovenous laser therapy Foam sclerotherapy 2. Angiomata and varicosities 3. Perforating vein incompetence 4. Iliac vein obstruction 5. Deep venous reflux a) Endovenous Ablative Therapy b) Endovenous Deep System Therapy c) Surgical Management d) Surgery for Truncal Vein e) Perforator Vein Surgery f) Valve Reconstruction
- 71. (1) Saphenectomy (vein ligation and stripping) • Painless technique is the sapheon closure device which uses glue to seal the vein. • It is used to remove a damaged vein and prevent complications of vein damage. • If several valves in a vein and the vein itself are heavily damaged, the vein (or the diseased part of the vein) is removed (stripped).
- 72. (2) Radiofrequency Ablation Generator & Catheter • The heating element burns the vein from the inside and the vein shuts down.
- 73. (3) Foam Sclerotherapy • This is a relatively Painless out patient procedure. • This causes the walls of the vein to stick together. • Over time the collapsed vein turns into scar tissue. • Sclerotherapy is a non- invasive procedure taking only about 30 minutes to perform. • Affected: Bruising, Raised red areas, Small skin sores.
- 74. (4) Endovenous Deep System Therapy
- 75. (5) Surgery for Truncal Vein
- 76. (6) Perforator Vein Surgery
- 78. Prevention Primary prevention: • No specific measures have been shown to prevent CVI. • Activity • Long-term treatment with low molecular weight heparin, rather than oral anticoagulation after DVT, may reduce or prevent development of post-thrombotic CVI. Secondary prevention: • Avoided: Prolonged standing, especially in one place. • Advised to lose weight if obesity.
- 79. Emerging treatments: • Balneotherapy • Spray-applied cell therapy • Other pharmacological therapies • Exercise Balneotherapy is the set of methods and practices which, based on scientific evidence, use medically and legally recognized mineral-medicinal waters, muds, and natural gases from natural springs for therapeutic purposes inside the facilities of thermal spa centres.
- 80. X. Complication 1) Haemosiderin 2) Venous ulceration 3) Haemorrhage 4) Infection 5) Severe CVI: • Atrophie blanche, Lipodermatosclerosis, • and Hyperpigmentation. Complication Related: 1) Spermatic cord (varicocele), Esophageal varices 2) Anorectum (hemorrhoids), 3) Varicosities of the legs, Trunk varices
- 82. XI. Prognosis (1) If CVI is left untreated it is usually progressive and leads to the post-phlebitic syndrome and venous ulcers. (2) Poor Prognosis: CVI + Diabetes and peripheral arterial occlusive disease. (3) Lifelong graded compression: Patients with severe CVI (CEAP C4-6) or previous ulcers generally require lifelong graded compression stockings of at least 30 to 40 mmHg. (4) Recurrence of venous leg ulcers: Failure with stocking. (5) Mortality rate was very low, 0.0056%.
- 83. XII. Reference 1) Robert T. Eberhardt, MD; Joseph D. Raffetto, MD 2) https://bestpractice.bmj.com/topics/en-gb/507/prognosis 3) https://www.medi.de/en/diagnosis-treatment/venous-disorders/anatomy-veins/ 4) https://lajollaveincare.com/vein-conditions/venous-reflux-is-a-progressive-condition-worsens- over-time/ 5) https://my.clevelandclinic.org/health/diseases/16872-chronic-venous-insufficiency-cvi 6) http://www.sophierenton.co.uk/treatments-for-varicose-veins/ 7) https://www.ahajournals.org/doi/10.1161/CIRCULATIONAHA.113.006898
- 85. THANKS