NEPHROTIC SYNDROME.pdf
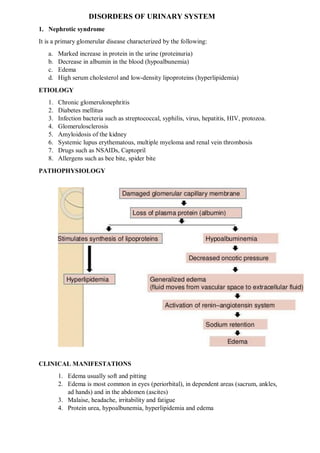
- 1. DISORDERS OF URINARY SYSTEM 1. Nephrotic syndrome It is a primary glomerular disease characterized by the following: a. Marked increase in protein in the urine (proteinuria) b. Decrease in albumin in the blood (hypoalbunemia) c. Edema d. High serum cholesterol and low-density lipoproteins (hyperlipidemia) ETIOLOGY 1. Chronic glomerulonephritis 2. Diabetes mellitus 3. Infection bacteria such as streptococcal, syphilis, virus, hepatitis, HIV, protozoa. 4. Glomerulosclerosis 5. Amyloidosis of the kidney 6. Systemic lupus erythematous, multiple myeloma and renal vein thrombosis 7. Drugs such as NSAIDs, Captopril 8. Allergens such as bee bite, spider bite PATHOPHYSIOLOGY CLINICAL MANIFESTATIONS 1. Edema usually soft and pitting 2. Edema is most common in eyes (periorbital), in dependent areas (sacrum, ankles, ad hands) and in the abdomen (ascites) 3. Malaise, headache, irritability and fatigue 4. Protein urea, hypoalbunemia, hyperlipidemia and edema
- 2. 5. Hypertension 6. Pleural effusion 7. Severe exertional dyspnea 8. Weight gain DIAGNOSTIC EVALUATION 1. History collection and physical examination 2. Urinalysis reveals proteinurea. Oval fat bodies (tubular epithelial cells with cholesterol esters) are also found in the urine in patients with nephrotic syndrome 3. 24 hr urine protein excretion is greater than 3.5g/1.73m3 /24 hr. 4. Abnormalities of blood chemistries include serum albumin less than 3g/dL, decreased total protein, elevated serum cholesterol, glucose, azotemia. 5. Ultrasonography of kidneys 6. Chest X-ray MANAGEMENT 1. Bed rest tolerated, avoidance of nephrotoxic drugs, low fat, fluid restriction in hyponatremic patients; normal protein intake unless urinary protein loss 0exceeds10g/24hr 2. Improved urinary protein excretion and serum lipid changes have been observed with a low fat soy protein diet providing 0.7 g of protein/kg/day. 3. However, because of increased risk of malnutrition, many nephrologists recommend normal protein intake 4. Strict sodium restriction to help manage peripheral edema 5. Close monitoring of patients for development of peripheral venous thrombosis and renal vein thrombosis because of hypercoagulable state secondary to loss of antithrombin III and other proteins involved in the clotting mechanism 6. Diuretic agents may be prescribed for the patient with severe edema 7. Use of angiotensin converting enzyme 8. Inhibitors to reduce proteinuria is generally indicated even in normotensive patients. Combination of an ACE inhibitor and angiotensin receptor blocker leads to decreased proteinuria and a beneficial effect on preserving renal function. 9. Statins are effective in controlling hyperlipidemia. There is evidence that lowering lipids slows the progression of renal disease. 10. The mainstay of therapy is treatment of the underlying disorder a. Minimal change disease generally responds to prednisone 1mg/kg. relapses can occur when steroids are discontinued. In these individuals, cyclophosphamide and chlorambucil may be useful b. Focal segmental glomerulosclerosis: Steroid therapy is also recommended. c. Membranous glomerulonephritis: Prednisone 2mg/kg day may be useful I including remission. Cytotoxic agents, cyclosporine can be added if there is poor response to prednisone. d. Membranoproliferative glomerulonephritis: most patients are treated with steroid therapy and antiplatelet drugs. COMPLICATIONS 1. Blood clots: The ability of the glomeruli to filter blood properly can lead to blood patients that help prevent clotting. This increases risk of developing a blood clot in veins.
- 3. 2. High blood cholesterol and elevated blood triglycerides: When the level of the protein albumin in blood falls, liver makes more albumin. At the same time, liver releases more cholesterol and triglycerides. 3. Poor nutrition: Loss of too much blood protein can result in malnutrition. This can lead to weight loss, but it may be masked by swelling. 4. High blood pressure: Damage to glomeruli and the resulting buildup of wastes in bloodstream can raise blood pressure. 5. Acute kidney failure: If kidneys lose their ability to filter blood due to damage to the glomeruli, waste products may build up quickly in blood. 6. Chronic kidney failure: Nephrotic syndrome may cause kidneys to gradually lose their function overtime. 7. Infections: People with nephrotic syndrome have an increased risk of infections. NURSING MANAGEMENT 1. Monitor intake and output, note signs of low plasma volume and impaired circulation with prerenal acute renal failure. 2. Instruct patient receiving steroids or cyclosporine regarding medication, signs and symptoms that must be reported to physician. 3. Measure blood pressure while the patients is in a supine position and also while he is standing, be alert for a drop in blood pressure that exceeds 20 mm Hg. 4. Instruct patient in selecting a high-protein diet while restricting cholesterol and fat intake. 5. The patient who is receiving corticosteroids or cyclosporine requires instructions about the medications and signs and symptoms that should be reported to the physician. 6. Provide good skin care because the patient with nephrotic syndrome usually has edema, if needed provide antiembolism stockings. To avoid thrombophlebitis, encourage activity and exercises.