Classical cong.h disease 5th power point presentation (3)
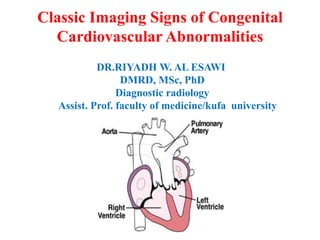
- 1. Classic Imaging Signs of Congenital Cardiovascular Abnormalities DR.RIYADH W. AL ESAWI DMRD, MSc, PhD Diagnostic radiology Assist. Prof. faculty of medicine/kufa university
- 2. The field of cardiovascular imaging is rapidly expanding, and it is important that radiologists &physicians be familiar with the classic signs of congenital cardiovascular abnormalities in both pediatric and adult patients. An understanding of the origin and pathophysiologic significance of each of these signs is essential in daily radiologic practice.
- 3. 1-TPGA In transposition of the great arteries (TPGA), the pulmonary artery is situated to the right of its normal location and is obscured by the aorta on frontal chest radiographs. This malposition, in association with stress induced thymic atrophy and hyperinflated lungs, results in the apparent narrowing of the superior mediastinum on radiographs, the most consistent sign of transposition of the great arteries. The cardiovascular silhouette varies from normal in the first few days after birth to enlarged and globular, with the classic appearance described as an egg on a string.
- 4. 1-Egg on string Chest radiograph obtained in a neonate shows narrowing of the superior mediastinum, enlargement of the cardiac silhouette with abnormal convexity of the right atrial border, and increased vascular flow—typical features of transposition of the great arteries.
- 5. 2-SNOW MAN TAPVR; total anomalous pulmonary venous return occurs when the pulmonary veins fail to drain into the left atrium and instead form an aberrant connection with some other cardiovascular structure. In type I ... (55% of cases), the anomalous pulmonary veins terminate at the supracardiac level. On chest radiographs, this cardiovascular anomaly resembles a snowman.
- 6. SNOW MAN
- 7. TAPVR 11&111 Type II TAPVR (30% of cases) involves a pulmonary venous connection at the cardiac level. The pulmonary veins join either the coronary sinus or the right atrium. Type III TAPVR (13% of cases) involves a connection at the infracardiac or infradiaphragmatic level. The pulmonary veins join behind the left atrium to form a common vertical descending vein, which courses anterior to the esophagus and passes through the diaphragm at the esophageal hiatus. This vertical vein usually joins the portal venous system but occasionally connects directly to the ductus venosus, the hepatic veins, or the inferior vena cava. Type III TAPVR is virtually always accompanied by some degree of obstructed venous return.
- 8. 3-Scimitar sign The scimitar sign is produced by an anomalous pulmonary vein that drains any or all of the lobes of the right lung. The so-called scimitar vein curves outward along the right cardiac border, usually from the middle of the lung to the cardiophrenic angle, and usually empties into the inferior vena cava but also may drain into the portal vein, hepatic vein, or right atrium. Although the diameter of the scimitar vein depends on whether it drains the entire right lung or only a portion of it, the diameter generally increases as the vein descends
- 10. 4-Gooseneck deformity • The gooseneck-shaped deformity in endocardial cushion defect is caused by a deficiency of both the conus and sinus portions of the Interventricular septum, with narrowing of the left ventricular outflow tract. The concavity of the interventricular septum below the mitral valve, along with the elongation and narrowing of the left ventricular outflow tract, produces a characteristic shape that has been compared to a sitting goose with an elongated neck on the anteroposterior projection in left ventricular angiography.
- 11. 4-Gooseneck deformity Endocardial cushion defects, which account for 4% of all cases of congenital heart disease,
- 12. 5-Boot shape Tetralogy of Fallot accounts for 10%–11% of cases of congenital heart disease. On chest radiographs in those affected by this syndrome, the heart has the shape of a wooden shoe or boot (in French, coeur en sabot). This deformity is due to uplifting of the cardiac apex because of right ventricular hypertrophy and concavity of the main pulmonary artery. The shadow of the pulmonary arterial trunk is almost invariably absent, and blood flow to the lungs is usually reduced.
- 13. 5-BOOT SHAPE Ventricular septal defect (1), infundibular pulmonary stenosis (2), overriding aorta (3), and right ventricular hypertrophy (4). The oxygen-rich blood in the left side of the heart (5) mixes with oxygen-poor blood in the right side of the heart (6) before it proceeds to the aorta (7).
- 14. 6-Ebestine anomaly Ebstein anomaly is characterized by the downward displacement of the septal leaflets and posterior leaflets of the tricuspid valve into the inflow portion of the right ventricle. This displacement results in the formation of a common right ventriculoatrial chamber and causes tricuspid regurgitation. The most consistent imaging feature is right atrial enlargement; the right atrium may be huge and fill the entire right hemithorax. The left atrium is normal in size, but the left cardiac contour has a shelved appearance because of the dilated right ventricular outflow tract. The aorta is small, and the pulmonary trunk, which normally appears as a discrete convex bulge, is absent. This combination of features produces a cardiac silhouette that has been described as box shaped
- 15. 6- Box shape Ebstein anomaly, first described by German physician Wilhelm Ebstein in 1866, accounts for 0.5%– 0.7% of cases of congenital heart disease
- 16. 7- coarctation of the aorta Two classic radiologic signs associated with aortic coarctation are the figure-of-three sign and the reverse figure-of-three sign. The aortic segment affected by coarctation has a shape that resembles the number 3 on frontal chest radiographs. The reverse figure-of-three sign, a mirror image of the number 3, is observed on the left anterior oblique view during barium esophagography. This sign is seen in 50%–66% of adults with aortic coarctation
- 17. 7-figure 3 sign
- 18. Coarctation Coarctation of the aorta accounts for 5%–10% of congenital cardiac lesions and is usually sporadic. However, it occurs with increased frequency among patients with Turner syndrome, 20%–36% of whom are affected. Clinical manifestations vary from congestive heart failure in infancy to hypertension with differential pressures between the upper and lower extremities in adulthood.
- 19. I AA According to the Celoria-Patton classification of IAA , type A is defined as interruption distal to the left subclavian artery (42% of cases); in type B, the interruption is between the left common carotid artery and subclavian artery (53%), finally, in type C, the interrupted segment is between the innominate artery and left common carotid artery (4%).
- 20. Interupted Coarctation of the aorta 30 y ,F ,HYPERTENSIVE
Editor's Notes
- The aorta (1) arises from the right ventricle (2), and the pulmonary artery (3) arises from the left ventricle (4). Communication between the systemic and the pulmonary circulation—an interatrial septal defect (5), an interventricular septal defect (6), or both—sustains life by allowing oxygenated blood from the left atrium (7) to mix with deoxygenated blood from the right atrium (8) before it flows via the right ventricle to the aorta and via the left ventricle to the pulmonary artery.