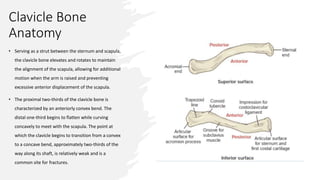
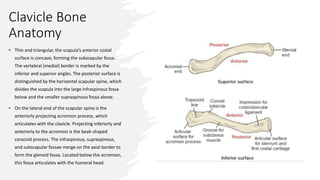
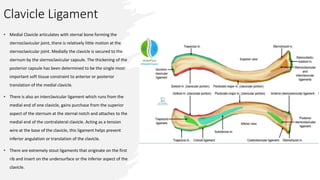
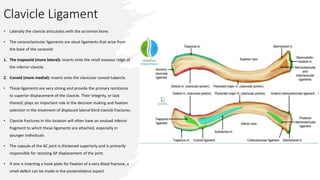
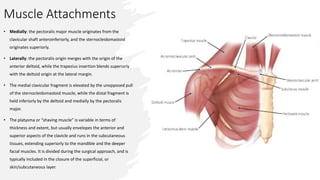
The document provides a detailed overview of clavicle anatomy, including its structure, ossification, and the associated joints and ligaments. It outlines the functional importance of the clavicle in arm movement and the stability of the sternoclavicular and acromioclavicular joints. Additionally, the document discusses the neurovascular anatomy related to the clavicle and the implications for surgical approaches.




![References:
1. Orthofixar | Orthopedic Surgery Learning
2.Millers Review of Orthopaedics -7th Edition Book.
3.Rockwood and Green's Fractures in Adults 8th Edition book.
4.Hyland S, Charlick M, Varacallo M. Anatomy, Shoulder and Upper
Limb, Clavicle. [Updated 2021 Jul 26]. In: StatPearls [Internet].
Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from:
NBK525990.](https://image.slidesharecdn.com/clavicleanatomy-230413111641-a9857839/85/clavicle-Anatomy-pptx-16-320.jpg)