Liver trauma
- 1. Liver Trauma Dr Dhaval Mangukiya
- 2. Liver ● Most frequently injured abdominal organ ○ Blunt - most common ○ Penetrating - second most common ● Most - Conservative management ● Intervention ○ Angiography/embolisation ○ Surgery (14% of all liver trauma)
- 3. Mechanism
- 4. Trauma Evaluation ● ATLS ● FAST ● DPL ● X ray ● CT scan Associated injuries in 80 percent cases
- 6. Diagnosis CECT abdomen - Liver Angiography Conventional Angiography
- 7. Hepatic Injury Grading - AAST Grade 1
- 8. Grade 2
- 9. Grade 2
- 10. Grade 2
- 11. Grade 3
- 12. Grade 4
- 13. Grade 5
- 14. Non operative management ● Observation ● Repeated evaluation ● Haemostatic agents
- 15. Hepatic embolisation ● 93 % success rate ● Improved success of nonoperatively managed patients with grade III or IV injuries exhibiting contrast extravasation visualized on admission CT scan ● Xu H, Jie L, Kejian S, et al. Selective Angiographic Embolization of Blunt Hepatic Trauma Reduces Failure Rate of Nonoperative Therapy and Incidence of Post-Traumatic Complications. Med Sci Monit 2017; 23:5522.
- 16. 1. Melloul E, Denys A, Demartines N. Management of severe blunt hepatic injury in the era of computed tomography and transarterial embolization: A systematic review and critical appraisal of the literature. J Trauma Acute Care Surg 2015; 79:468. In one systematic review of severe liver injuries (grade III/IV), overall, 1 to 5 percent of patients treated nonoperatively required embolization for recurrent bleeding more than 24 hours after admission, while 12 to 28 percent of those requiring laparotomy for hemodynamic instability required secondary embolization to control recurrent postoperative bleeding
- 17. Risk of observation ● Missed intra-abdominal injury particularly hollow viscus injury ● Transfusion-related illness (TACO, TRALI, TRIM) ● Risks associated with embolization techniques ○ hepatic necrosis (15%) ○ abscess formation (7.5%) ○ bile leaks 1. Green CS, Bulger EM, Kwan SW. Outcomes and complications of angioembolization for hepatic trauma: A systematic review of the literature. J Trauma Acute Care Surg 2016; 80:529.
- 18. Failed non operative management ● 7 % in severe injuries ● Patients with grade IV or V injuries are more likely to fail nonoperative management ● In one study, logistic regression found that blood transfusion ≥3 units was an independent risk factor for surgical intervention ● Huang YC, Wu SC, Fu CY, et al. Tomographic findings are not always predictive of failed nonoperative management in blunt hepatic injury. Am J Surg 2012; 203:448. ● Most protocols allow for continued observation with up to 4 units of blood transfusion related to the hepatic injury
- 19. Mortality Many of these higher-grade injuries can be successfully managed nonoperatively with overall low mortality rates ranging from 0 to 8 percent. Higher mortality rates are seen for those patients with high-grade injuries who require surgical management either immediately or as a result of failed nonoperative management (30 to 68 percent)
- 20. Complications ● 5, 22, 52 percent in grade 3, 4, 5 ● Kozar RA, Moore FA, Cothren CC, et al. Risk factors for hepatic morbidity following nonoperative management: multicenter study. Arch Surg 2006; 141:451. (series of 669 patients) ● Bile leak (0.5-21 percent) ○ Biliary ascitis ○ Persistent haemoperitoneum ○ Abscess formation ● Hepatic necrosis ○ Resectional debridement in conjunction with interventional drainage procedures, or hepatic lobectomy ● Laparoscopic Lavage ● Pigtail ● Exploration
- 22. Surgical techniques ● Appx in 14% require surgery ● Goal ○ Control bleeding with preserving liver paranchyma ○ Resection for severe injuries only
- 24. Surgical technique ● Superficial liver lacerations may respond to conservative techniques such as compression, topical hemostatic agents, electrosurgical techniques, or packing. ● Deep lacerations, large open tract lacerations, and larger parenchymal avulsions will typically require direct ligation or clipping of bleeding vessels augmented with suture plication and packing ● Severe injuries require more aggressive means for controlling bleeding, including hepatic artery ligation and resectional debridement, followed by suture approximation of the raw edges of the liver or therapeutic liver packing, with or without topical hemostatic agents
- 25. Surgery technique ● Incision and exposure
- 26. Techniques of haemostasis ● Manual compression ● Porta clamping (pringle) ● Perihepatic packing ● Mesh wrapping ● Tropic haemostatic agents ● Electrocautery ● Parenchymal Vessel ligation ● Direct Liver suturing
- 27. Severe Injury ● Hepatic artery ligation ● Liver Resection ○ Resectional Debridement ○ Anatomical Resection (mortality rate 60 percent)
- 28. ● Abdminal closure ● Drainage ● Postoperative imaging
Editor's Notes
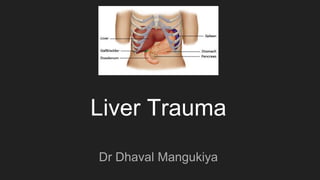
- The liver margin, which can usually be palpated 2 to 3 cm below the right rib margin, rises and falls with the diaphragm during respiration. The dome of the liver rises as high as the level of T4 (nipple) with expiration. Thus, injuries to the chest wall are often associated with significant injury to the liver. Similarly, the inferior margin of the liver descends to as low as T12 with deep inspiration, and injuries, particularly penetrating injuries, have the potential to injure the liver lower in the abdomen than might be expected. The posterior portion of the right lobe (figure 2) is the most common site of hepatic injury in blunt trauma
- The time course for developing anemia following post-traumatic hemorrhage is variable and related to the rapidity of exogenous fluid administration and endogenous fluid shifts. Thus, the absence of anemia at the time of initial patient presentation does not rule out significant liver trauma-related bleeding. Many studies have investigated the predictive value of liver function studies in diagnosing liver injury, but no consensus regarding their utility has been reached
- Grade I – Subcapsular hematoma <10 percent surface area. Parenchymal laceration <1 cm in depth The AAST grading system is useful for predicting the likelihood of success with nonoperative management, which is higher for low-grade injuries (grade I, II, III) compared with high-grade injuries (grade IV, V). Patients with grade VI injuries are universally hemodynamically unstable, mandating surgical intervention.
- Subcapsular hematoma 10 to 50 percent surface area
- intraparenchymal hematoma <10 cm in diameter
- Laceration: 1 to 3 cm parenchymal depth and ≤10 cm in length
- Subcapsular hematoma >50 percent of surface area; ruptured subcapsular or parenchymal hematoma. Intraparenchymal hematoma >10 cm. Laceration >3 cm in depth (image 5). Any injury in the presence of a liver vascular injury or active bleeding contained within liver parenchyma.
- Parenchymal disruption involving 25 to 75 percent of a hepatic lobe (image 6 and image 7 and figure 2). Active bleeding extending beyond the liver parenchyma into the peritoneum.
- Parenchymal disruption of >75 percent of a hepatic lobe (figure 2). Juxtahepatic venous injury to include retrohepatic vena cava and central major hepatic veins
- Depending upon the nature of the injury and technical factors, embolization coils, microspheres, absorbable gelatin sponge, or endogenous clot can be used to interrupt blood flow in the main hepatic artery or branch vessels. Ischemic complications related to angioembolization are not uncommon and may lead to a need for surgical debridement or liver resection
- missed intra-abdominal injury, particularly hollow viscus injury, transfusion-related illness, and risks associated with embolization techniques, which include hepatic necrosis, abscess formation, and bile leaks Blood transfusion is associated with many complications that can include intravascular volume overload (transfusion-associated circulatory overload [TACO]), transfusion-related acute lung injury (TRALI), hypothermia, coagulopathy, and immunologic and allergic reactions, as well as immunomodulation (transfusion-related immune modulation [TRIM]) The most frequently reported complications following hepatic embolization include hepatic necrosis (15 percent), abscess formation (7.5 percent), and bile leaks [42]. The risk of contrast-induced nephropathy may be greater when embolization is performed following contrast CT scan, particularly in patients who may already be volume depleted. Contrast-induced nephropathy and its prevention are discussed in detail elsewhere.
- Patients with grade IV or V injuries are more likely to fail nonoperative management. In one study, logistic regression found that blood transfusion ≥3 units (odds ratio 10.8, 95% CI 1.6-72.2) was an independent risk factor for surgical intervention [53]. Most protocols allow for continued observation with up to 4 units of blood transfusion related to the hepatic injury.
- Many of these higher-grade injuries can be successfully managed nonoperatively with overall low mortality rates ranging from 0 to 8 percent. Higher mortality rates are seen for those patients with high-grade injuries who require surgical management either immediately or as a result of failed nonoperative management (30 to 68 percent)
- The timing of repeat laparotomy for removal of the abdominal packs is controversial [8,16-19]. Rates of rebleeding are higher when packs are removed less than 24 hours after the initial laparotomy; however, the incidence of perihepatic sepsis is higher when a longer period of time has elapsed. Pack removal between 24 to 48 hours following the initial laparotomy is a reasonable compromise, and if no bleeding recurs when the packs are removed, definitive closure of the abdominal wall may be possible. Hepatic bleeding that resumes necessitates repacking the liver, and reexploration is performed after another 24 to 48 hours.
