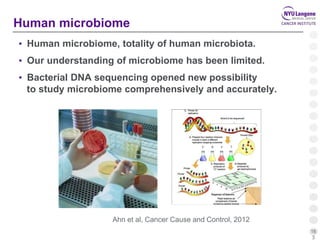
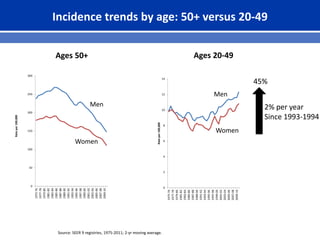
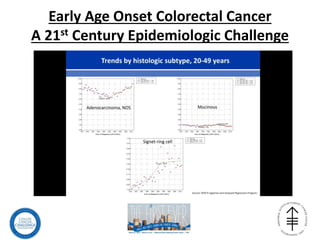
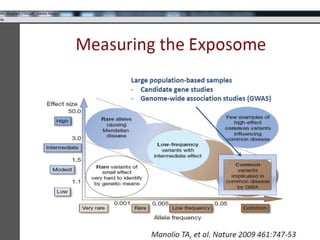
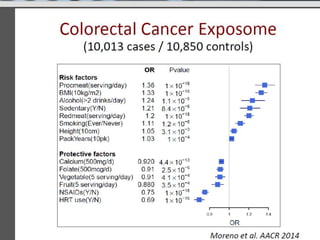
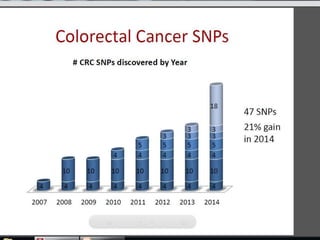
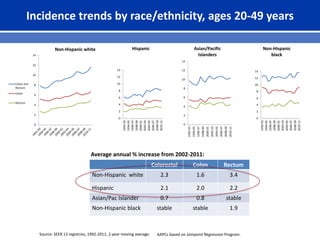
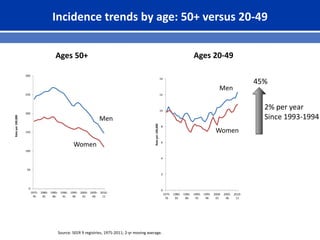
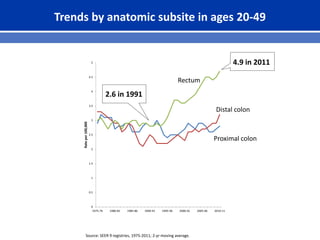
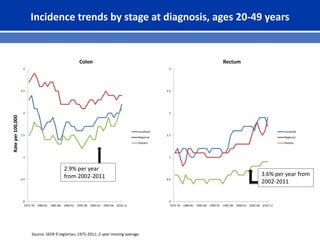
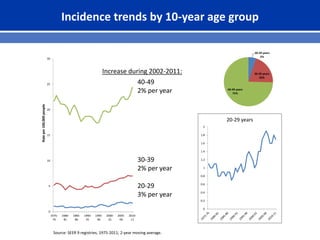
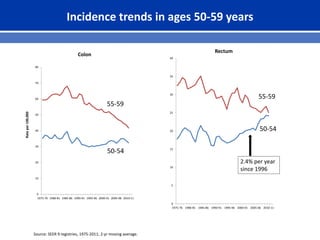
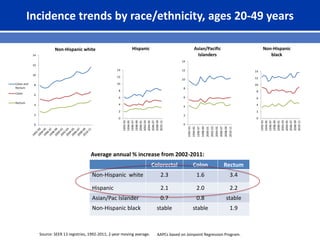
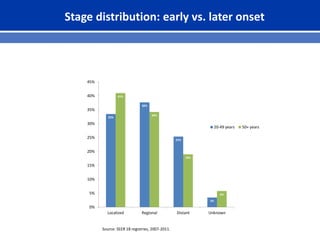
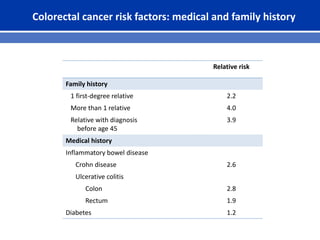
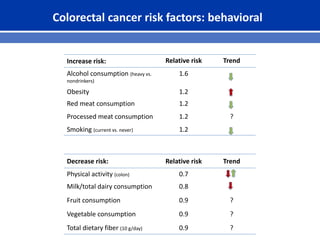
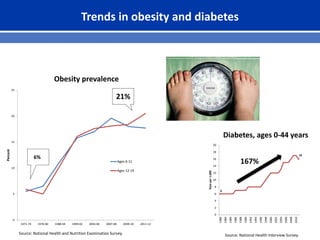
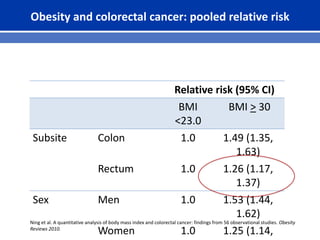
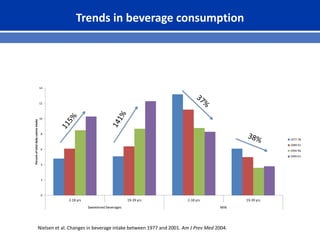
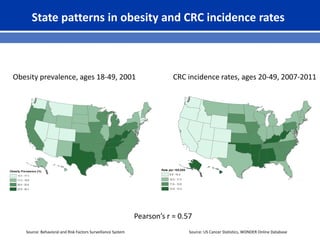
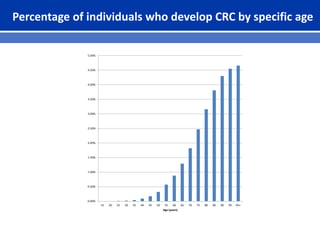
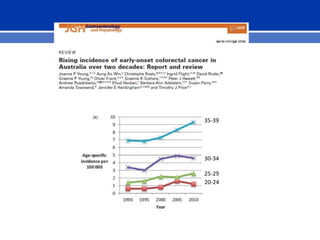
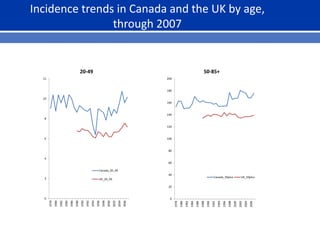
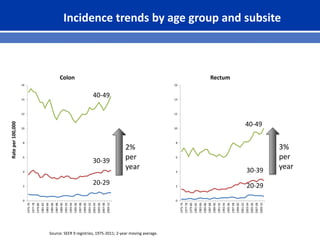
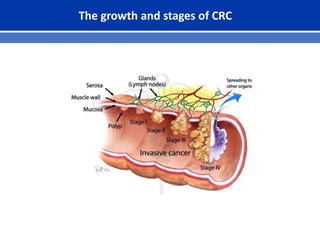
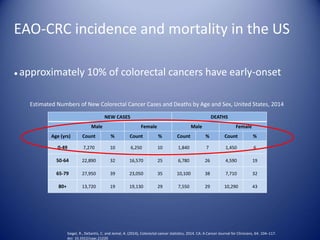
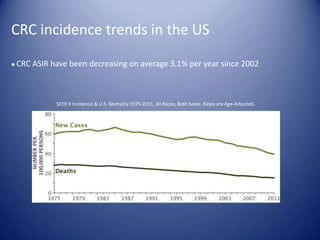
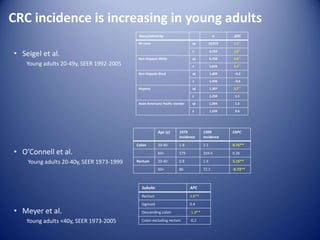
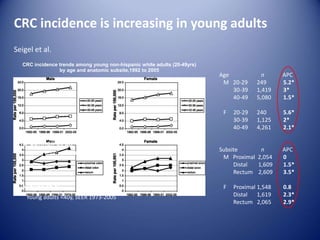
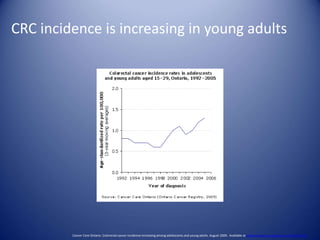
This document summarizes recent trends in colorectal cancer incidence among young adults in the United States. It finds that rates of colorectal cancer among those under 50 have been rising about 2-3% annually since the early 1990s. This is concerning as colorectal cancer typically affects older adults. Risk factors like obesity, lack of physical activity, and unhealthy diets may be contributing to earlier onset of the disease. More research is still needed to understand the full causes of the increasing trends in young adults. The document recommends awareness of family history to guide early screening when appropriate.































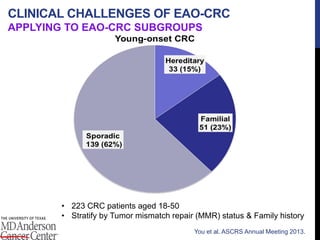


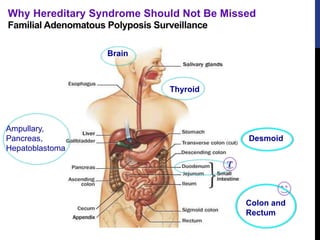
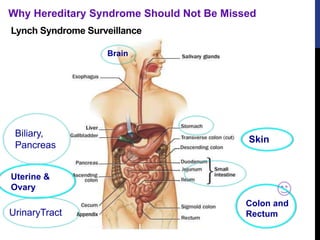



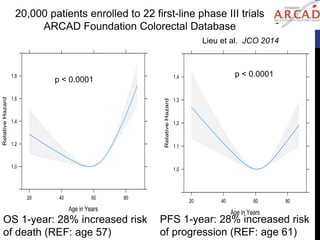

































































![References
Ferlay J, Soerjomataram I, Ervik M, et al. GLOBOCAN 2012 v1.0, Cancer Incidence and Mortality Worldwide: IARC Cancer Base No. 11 [Internet]. Lyon, France: International Agency for Research on Cancer; 2013. Available
from: http://globocan.iarc.fr, accessed November 15, 2014.
American Cancer Society. Colorectal Cancer Facts and Figures 2014-2016. Atlanta: American Cancer Society; 2014.
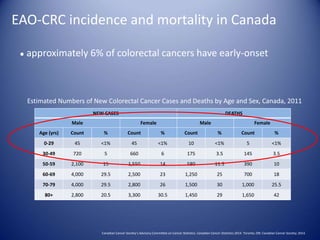
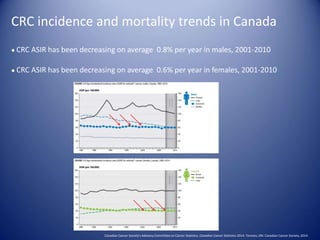
Canadian Cancer Society's Advisory Committee on Cancer Statistics (2014). Canadian Cancer Statistics 2014. Toronto, ON: Canadian Cancer Society.
Siegel R, Desantis C, Jemal A. Cancer statistics, 2014. CA Cancer J Clin. 2014 Mar-Apr 64(2):104-17.
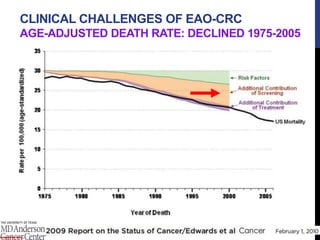
Edwards BK, Ward E, Kohler BA, et al. Annual report to the nation on the status of cancer, 1975-2006, featuring colorectal cancer trends and impact of interventions (risk factors, screening, and treatment) to reduce future
rates. Cancer. 2010 Feb 1;116(3):544-73.
Cheng L, Eng C, Neiman LX, Kapadia AS, Du XL. Trends in colorectal cancer incidence by anatomic site and disease stage in the United States from 1976-2005. Am J Clin Oncol. 2011 Dec;34(6):573-80
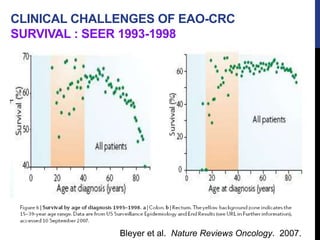
Surveillance Epidemiology and End Results. Fast Stats, http:// seer.cancer.gov/faststats. Accessed November 15, 2014.
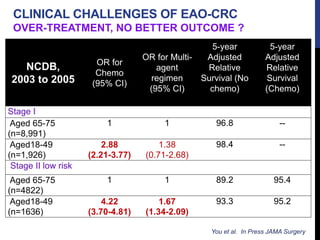
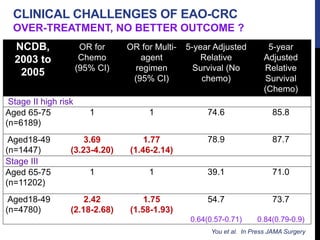
Bailey CE, Hu CY, You YN, et al. Increasing Disparities in the Age-Related Incidences of Colon and Rectal Cancers in the United States, 1975-2010. JAMA Surg. 2014 Nov 5:1-6.
Siegel RL, Jemal A, Ward EM. Increase in incidence of colorectal cancer among young men and women in the United States. Cancer Epidemiol Biomarkers Prev. 2009 Jun;18(6):1695-8.
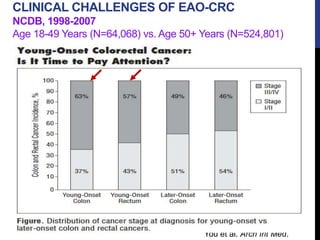
You YN, Xing Y, Feig BW, Chang GJ, Cormier JN. Young-onset colorectal cancer: is it time to pay attention? Arch Intern Med. 2012 Feb 13;172(3):287-9.
Pignone M, Rich M, Teutsch SM, et al. Screening for colorectal cancer in adults at average risk: a summary of the evidence for the US Preventive Services Task Force. Ann Intern Med. 2002 Jul 16;137(2):132-41.
Whitlock EP, Lin JS, Liles E, Beil TL, Fu R. Screening for colorectal cancer: a targeted, updated systematic review for the U.S. Preventive Services Task Force. Ann Intern Med. 2008 Nov 4;149(9):638-58.
Myers EA, Feingold DL, Forde KA, et al. Colorectal cancer in patients under 50 years of age: A retrospective analysis of two institutions' experience. World J Gastroenterol. 2013 Sep 14;19(34):5651-7.
Kirzin S, Marisa L, Guimbaud R, et al. Sporadic early-onset colorectal cancer is a specific sub-type of cancer: a morphological, molecular and genetics study. PLoS One. 2014 Aug 1;9(8):e103159.
Chang DT, Pai RK, Rybicki LA, et al. Clinicopathologic and molecular features of sporadic early-onset colorectal adenocarcinoma: an adenocarcinoma with frequent signet ring cell differentiation, rectal and sigmoid
involvement, and adverse morphologic features. Mod Pathol 2012 Aug;25(8):1128–1139
Yantiss RK, Goodarzi M, Zhou XK, et al. Clinical, pathologic, and molecular features of early-onset colorectal carcinoma. Am J Surg Pathol 2009 Apr;33(4):572–582
Fante R, Benatti P, di Gregorio C, et al. Colorectal carcinoma in different age groups: a population-based investigation. Am J Gastroenterol. 1997;92:1505–1509.
Minardi AJ, Sittig KM, Zibari GB, McDonald JC. Colorectal cancer in the young patient. Am Surg. 1998;64:849–853.
Domergue J, Ismail M, Astre C, et al. Colorectal carcinoma in patients younger than 40 years of age. Montpellier Cancer Institute experience with 78 patients. Cancer. 1988;61:835–840.
Palmer ML, Herrera L, Petrelli NJ. Colorectal adenocarcinoma in patients less than 40 years of age. Dis Colon Rectum. 1991;34:343–346.
Chiang JM, Chen MC, Changchien CR, et al. Favorable influence of age on tumor characteristics of sporadic colorectal adenocarcinoma: patients 30 years of age or younger may be a distinct patient group. Dis Colon Rectum.
2003 Jul;46(7):904-10.
Parramore JB, Wei JP, Yeh KA (1998) Colorectal cancer in patients under forty: presentation and outcome. Am Surg 64: 563–567 discussion 567–568
Liang JT, Huang KC, Cheng AL, Jeng YM, Wu MS, et al. (2003) Clinicopathological and molecular biological features of colorectal cancer in patients less than 40 years of age. Br J Surg 90: 205–214
Berg M, Danielsen SA, Ahlquist T, Merok MA, Agesen TH, et al. (2010) DNA sequence profiles of the colorectal cancer critical gene set KRAS-BRAF-PIK3CA-PTEN-TP53 related to age at disease onset. PLoS One. 2010 Nov
12;5(11):e13978.
Alsop K, Mead L, Smith LD, Royce SG, Tesoriero AA, et al. (2006) Low somatic K-ras mutation frequency in colorectal cancer diagnosed under the age of 45 years. Eur J Cancer 42: 1357–1361
Fearon ER, Vogelstein B. A genetic model for colorectal tumorigenesis. Cell. 1990;61:759–67.
Reich DE, Lander ES. On the allelic spectrum of human disease. Trends Genet. 2001;17:502–10.
Wang WY, Barratt BJ, Clayton DG, Todd JA. Genome-wide association studies: theoretical and practical concerns. Nat Rev Genet. 2005;6:109–118.
Bodmer W1, Bonilla C. Common and rare variants in multifactorial susceptibility to common diseases. Nat Genet. 2008 Jun;40(6):695-701. doi: 10.1038/ng.f.136.
Frayling I, Beck NE, Ilyas M, Dove-Edwin I, Goodman P, Beck JA, et al. The APC variants I1307K and E1317Q are associated with colorectal tumors, but not always with a family history. Proc Natl Acad Sci USA. 1998 Sep
1;95(18):10722–7.
Fearnhead N, Wilding JL, Winney B, Tonks S, Bartlett S, Bicknell DC, et al. Multiple rare variants in different genes account for multifactorial inherited susceptibility to colorectal adenomas. Proc Natl Acad Sci USA. 2004 Nov
9;101(45):15992–7.
Comino-Mendez I, Gracia-Aznarez FJ, Schiavi F, Landa I, Leandro-Garcia LJ, Leton R, et al. Exome sequencing identifies MAX mutations as a cause of hereditary pheochromocytoma. Nat Genet 2011 Jun 19;43(7):663–7.
Jones S, Hruban RH, Kamiyama M, Borges M, Zhang X, Parsons DW, et al. Exomic sequencing identifies PALB2 as a pancreatic cancer susceptibility gene. 2009 Science Apr 10;324(5924):217
Palles C, Cazier JB, Howarth KM, Domingo E, Jones AM, Broderick P, et al. Germline mutations affecting the proofreading domains of POLE and POLD1 predispose to colorectal adenomas and carcinomas. Nat Genet. 2013
Feb;45(2):136-44.
Smith CG, Naven M, Harris R, Colley J, West H, Li N, et al. Exome resequencing identifies potential tumor-suppressor genes that predispose to colorectal cancer. Hum Mutat. 2013 Jul;34(7):1026-34.
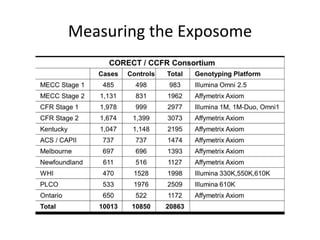
Newcomb PA, Baron J, Cotterchio M, Gallinger S, Grove J, Haile R, et al. Colon Cancer Family Registry: an international resource for studies of the genetic epidemiology of colon cancer. Cancer Epidemiol Biomarkers Prev. 2007
Nov;16(11):2331-43.](https://image.slidesharecdn.com/earlyageonsetcolorectalcancer2015-150511170431-lva1-app6891/85/Early-age-onset_colorectal_cancer_2015-160-320.jpg)