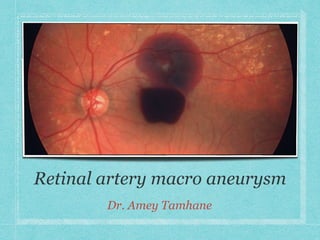
Retinal Artery Macroaneurysm.pptx
- 2. INTRODUCTION RAMs are defined as fusiform or saccular dilatations of the retinal arteries, usually emanating from the first three branches of the arteriolar tree. They are commonly associated with macular exudation and haemorrhage, which may result in decreased visual acuity. Female preponderance (ratio of 3:1), typically after 60 years of age, and with a medical history of systemic hypertension and/or arteriosclerotic vascular disease. 10 % of patients have bilateral disease and 20 % have multiple macro-aneurysms. The term “simple RAM” refers to isolated vascular ectasia, while “complex RAM” is used when the ectasia is accompanied by haemorrhage.
- 3. CLINICAL PRESENTATION Often, RAM is noted on clinical examination but the patient is asymptomatic. The involved artery may be narrowed proximally and distally to the macroaneurysm. Severe vision loss can occur from leakage of the aneurysm with resultant haemorrhage into the vitreous cavity, subhyaloid space and/or intraretinally or subretinally. Many times, “hourglass haemorrhages” defined as the simultaneous presence of preretinal and subretinal haemorrhage, can be seen. Serous fluid can also collect intraretinally, producing diffuse or focal cystoid macular oedema with or without the accumulation of lipid exudates.
- 4. DIFFERENTIAL DIAGNOSIS Exudative ARMD Branch Retinal Vein Occlusion Capillary Hemangioma Cavernous Hemangioma Diabetic Macular Oedema Subretinal neovascular membranes Radiation Retinopathy Leber Miliary Aneurysms
- 5. VASCULAR SIGNS & SITES OF OCCURRENCE Macroaneurysms more commonly affect the right eye than the left. The supero temporal artery is most commonly involved. However, macroaneurysms also have been reported in cilioretinal arteries, on the optic nerve head, and associated with congenital retinal macrovessels. Usually, leakage of protein-rich serum occurs, leading to circinate exudation and macular oedema. Serous retinal detachment can occur. Bleeding is a common complication of aneurysm formation and can occur beneath the retina, the retinal pigment epithelium (RPE), or the internal limiting membrane (ILM), or into the vitreous. Pulsatile flow occasionally is observed but does not necessarily indicate a higher risk of haemorrhage.
- 6. PATHOGENESIS The pathogenesis of RAM is thought to be secondary to several mechanisms causing blood vessel wall weakness and subsequent aneurysmal dilatation. Systemic arteriosclerosis Fibrosis of vessel wall Decreased Elasticity Systemic Hypertension Macroaneurysm. Histopathologically, RAMs are found to have arterial dilatation with variable degrees of artery wall hyalinization and surrounding retinal exudate or haemorrhages. Microvascular abnormalities (eg. widening of the periarterial capillary free zone, capillary dilation, nonperfusion, intra-arterial collaterals) have been identified. Lipid-laden macrophages, hemosiderin, and fibroglial reaction are also observed. Histopathology of a ruptured RAM with preretinal, intraretinal and subretinal hemorrhage.
- 7. IMAGING OF RAM A complete assessment of RAM requires a combination of clinical examination and imaging studies, such as B-scan ultrasonography, fundus fluorescein angiography (FFA), indocyanine green angiography (ICGA), and optical coherence tomography (OCT). B scan If extensive vitreous haemorrhage obscures the view of the fundus, ultrasound B scan can be used to exclude conditions such as retinal tears, detachments, and breakthrough haemorrhage from polypoidal choroidal vascuolopathies. FFA The typical RAM fills up uniformly in the early phase, revealing a fusiform dilation of the arteriole with late leakage. The presence of a thrombus may result in filling defects. Areas of blocked fluorescence due to the overlying blood may also be present. With the aid of dynamic FFA, pulsatility of the macroaneurysm may be observed in 10% of cases. ICGA If significant haemorrhage renders FFA inconclusive, ICGA may be a useful alternative, allowing deeper penetration through the areas of haemorrhage.
- 8. FFA VS. ICGA. In the presence of excessive blood with significant blocked hyperfluorescence, ICGA may be superior to FFA. RAM is completely obscured by blood on FFA (2A) but can be seen clearly on ICGA (2B).
- 9. IMAGING OF RAM OCT SD-OCT enables visualization of the lesion as well as associated complications. The macroaneurysm will appear as a round or oval hyperreflective lesion in the inner retinal layers. In addition, it may demarcate the extent of lipid deposition and accumulation of intraretinal and/or subretinal fluid. Diagnostic challenges Despite several imaging options at our disposal, diagnosing RAM may prove challenging when extensive haemorrhage is present. In such cases, examining the fellow eye closely may help guide the physician. Important diagnostic clues for RAM include absence of drusen and the presence of significant hypertensive retinopathy in the fellow eye in the setting of an asymmetric vascular lesion with lipid or blood concentrated around the bifurcation of an arteriole in the affected eye. Horizontal SD-OCT section scan showing sub- internal limiting membrane (ILM) haemorrhage in the scan passing through upper part of haemorrhage and boat-shaped subhyaloid haemorrhage in lower part.
- 10. TREATMENT The majority of RAMs can be observed, and many will spontaneously involute. In a natural-history study, Cathleen McCabe and colleagues described a series of 41 patients with macular haemorrhages secondary to RAMs managed solely with observation. The patients average visual acuity at baseline was 20/200 or worse. After an average follow-up of 15.7 months, 37 % of eyes achieved a final visual acuity of 20/40 or better, 29 % achieved 20/50 to 20/100, and 34 % were 20/200 or worse. While good visual acuity outcomes can be achieved with observation alone, poorer visual acuity was associated with macular pigmentary changes after resorption of blood. McCabe CM, Flynn HW Jr, McLean WC et al. Nonsurgical management of macular hemorrhage secondary to retinal artery macroaneurysm. Arch Ophthalmol 2000;118:780-785.
- 15. LASER TREATMENT Intervention may be required in cases of exudative or hemorrhagic RAMs, or recurrent/persistent cystoid macular oedema. Laser photocoagulation, first described by J. Donald M. Gass in 1976, was shown to reduce leakage in approximately 16 to 27 percent of RAMs. Laser of the artery and surrounding area may decrease flow and intraluminal pressure, thereby reducing the macroaneurysm. However, this therapy can be associated with the risk of vascular occlusion, early increase in exudates from selective reabsorption of fluid, arteriovenous shunts, macular pucker and scotomas.
- 16. LASER PHOTOCOAGULATION The most frequently cited indication for laser photocoagulation of a macroaneurysm is persistence or progression of macular exudation. The current recommendation for photocoagulation of macroaneurysms is the use of the argon green or yellow dye laser for direct photocoagulation of the lesion. Low power settings are preferred, sufficient to create a light to moderate burn intensity, using a large spot size (500µm) and long-duration (0.5s) pulses directly on the lesion, to avoid rupture of the RAM It has been reported that only 16% to 27% of RAMs are successfully thrombosed after treatment with laser photocoagulation. Meyer JC et al. Graefes Arch Clin Exp Ophthalmol. 2015;253(4):537-541.
- 17. LASER HYAIOLODOTOMY In the setting of dense subhyaloid haemorrhage, YAG-laser hyaloidotomy has been performed to release the sequestered blood into the vitreous cavity. Release of blood may reduce the risk of macular scarring and epiretinal fibrosis. This approach remains controversial due to the possible complications of macular hole, retinal detachment, or vitreous haemorrhage requiring vitrectomy. Ulbig MW et al. Arch Ophthalmol. 1998;116(11):1465-1469.
- 18. ANTI VEGF Anti-vascular endothelial growth factor therapy has emerged as a useful treatment modality for RAMs. VEGF inhibition is thought to decrease vascular permeability, block angiogenesis to reduce further bleeding and exudation, and decrease the binding of pro- thrombotic VEGF receptor. A recent report demonstrated improvement of vision from 20/60 to 20/30 in a patient with a RAM and macular exudation after a series of six injections; however, ultimately focal laser photocoagulation was needed due to recurrence of CME with stabilization of vision at 20/30 at 19 months of follow-up. Leung EH, Reddy AK, Vedula AS, Flynn HW Jr. Serial bevacizumab injections and laser photocoagulation for macular edema associated with a retinal artery macroaneurysm. Clin Ophthalmol 2015;9:601-609.
- 19. SURGICAL EVACUATION In rare settings in which vitreous haemorrhage is present and the etiology of bleeding is unclear, vitrectomy may be indicated. However, removal of dense subretinal haemorrhage is very controversial and has the potential to cause many serious complications. In one study from Mark Humayun and co-workers described nine eyes with submacular haemorrhage secondary to ruptured RAMs, treated with submacular surgery with tissue plasminogen activator-assisted thrombolysis, showed that 89 percent of eyes achieved a corrected visual acuity of 20/60 or better. These options are currently used less often with thin submacular haemorrhages, given the positive response with anti-VEGF agents.
- 20. PROGNOSIS The visual prognosis is excellent for many patients with macroaneurysm. The natural history of these lesions suggests that most close spontaneously, with restoration of near-normal vision. In some patients, the Valsalva maneuver may be associated with an increased risk of haemorrhage. However, although reducing the risk of the Valsalva maneuver in patients with active, pulsatile retinal macroaneurysms may be beneficial, this has not been proven to reduce the incidence of haemorrhage in these patients.
- 21. COMPLICATIONS Clinical complications of retinal macroaneurysms include vitreous haemorrhage, retinal detachment, macular holes, and choroidal neovascular membrane formation. Vision loss from macular oedema due to chronic exudation is well documented in many patients, and laser treatment may be appropriate. Vision loss resulting from retinal macroaneurysms usually results from scarring in the macula due to either chronic oedema or haemorrhage. Several studies suggests that patients with preretinal haemorrhage or vitreous haemorrhage due to retinal macroaneurysms have a good visual prognosis. In contrast, the visual prognosis is poor in patients with submacular haemorrhage.
- 22. TAKE HOME MESSAGE RAMs are rare clinical findings occurring most often in older, hypertensive women. While anti-VEGF therapy can be a useful treatment option to improve vision and decrease macular oedema, more complex RAMs may require laser photocoagulation and / or surgical intervention.