Thyroid hormone
The thyroid hormones, triiodothyronine (T3) and its prohormone, thyroxine (T4), are tyrosine-based hormones produced by the thyroid gland that are primarily responsible for regulation of metabolism. Iodine is necessary for the production of T3 and T4. A deficiency of iodine leads to decreased production of T3 and T4, enlarges the thyroid tissue and will cause the disease known as simple goitre. The major form of thyroid hormone in the blood is thyroxine (T4), which has a longer half-life than T3.The ratio of T4 to T3 released into the blood is roughly 20 to 1. T4 is converted to the active T3 (three to four times more potent than T4) within cells by deiodinases (5'-iodinase). These are further processed by decarboxylation and deiodination to produce iodothyronamine (T1a) and thyronamine (T0a). All three isoforms of the deiodinases are selenium-containing enzymes, thus dietary selenium is essential for T3 production.
Recommended
More Related Content
What's hot
What's hot (20)
Viewers also liked
Viewers also liked (20)
Similar to Thyroid hormone
Similar to Thyroid hormone (20)
More from Atai Rabby
More from Atai Rabby (20)
Recently uploaded
Recently uploaded (20)
Thyroid hormone
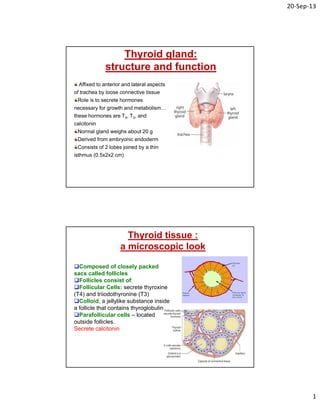
- 1. 20‐Sep‐13 1 Thyroid gland: structure and function Affixed to anterior and lateral aspects of trachea by loose connective tissue Role is to secrete hormones necessary for growth and metabolism… these hormones are T4, T3, and calcitonin Normal gland weighs about 20 g Derived from embryonic endoderm Consists of 2 lobes joined by a thin isthmus (0.5x2x2 cm) Thyroid tissue : a microscopic look Composed of closely packed sacs called follicles Follicles consist of: Follicular Cells: secrete thyroxine (T4) and triiodothyronine (T3) Colloid, a jellylike substance inside a follicle that contains thyroglobulin Parafollicular cells – located outside follicles. Secrete calcitonin
- 2. 20‐Sep‐13 2 Thyroid hormones are stored extracellularly in the colloid inside the follicle in the form of ioidinated thyroglobulin Follicular cells and Colloid: inter-relationship Glycoprotein (10% carbohydrate) MW 66 KDa 2 identical subunits of 33 KDa 132 tyrosines 25 to 30 iodinated Thyroglobulin T3 and T4 are attached to thyroglobulin (after they are iodinated) inside the follicles Storage function The hormones are only released after thyroglobulin is endocytosed and hydrolysed Hydrolysis accomplished by lysosomal proteases inside the follicular cells Important in coupling reaction Thyroglobulin
- 3. 20‐Sep‐13 3 All are amino acid derivatives (tyrosine), but are hydrophobic molecules Can freely cross the cell membrane Transported in circulation bound to specific protein carriers Bind to intracellular receptors on target tissues Synthesis accomplished via iodination of tyrosine residues on thyroglobulin in iodide cycle All aspects of hormone synthesis are regulated by extra thyroid mechansims (TRH-TSH) Thyroid hormones Maintain metabolic homeostasis by regulating: Intermediary metabolism Body weight Oxygen requirements Body temperature Positive control of growth, reproduction and differentiation The ratio of T4 to T3 released into the blood is roughly 20 to 1. Thyroid hormones
- 4. 20‐Sep‐13 4 Thyroid hormones: tyrosine derivatives (T3 and T4) Thyroid hormones
- 5. 20‐Sep‐13 5 T3 has approximately 10 times potency of T4 Most circulating T3 (about 80%) is produced by monodeiodination of T4 in peripheral tissues Conversion occurs in kidney and liver Remaining 20% is directly secreted by thyroid Primary iodothyronine secreted by thyroid gland is T4 However, the affinity of the nuclear receptor for this hormone is less than T3 The other monodeiodinated product from T4 is “reverse” T3 Nearly all produced extrathyroidally Only about one third of T4 is converted to this More rapid metabolic clearance Little or no biological activity Both T3 and rT3 can be further deiodinated T3 T4 rT3 Needed for synthesis of thyroid hormones Sources: oIodized salt oIodated bread oDairy products Daily requirement: 75 micrograms which is in about 10g of iodized salt Most iodide is absorbed and mainly confined to the extracellular fluid Iodide ingested in organic/inorganic forms Removal of iodide from ECF is done by the thyroid gland and the kidneys Largest pool of iodide located in the thyroid Iodide How are the hormones synthesized???
- 7. 20‐Sep‐13 7 The Na+/I- symporter transports two sodium ions across the basement membrane of the follicular cells along with an iodine ion. This is a secondary active transporter that utilises the concentration gradient of Na+ to move I- against its concentration gradient. I- is moved across the apical membrane into the colloid of the follicle. Thyroperoxidase (TPO) oxidises two I- to form I2. Iodide is non-reactive, and only the more reactive iodine is required for the next step. The thyroperoxidase iodinates the tyrosyl residues of the thyroglobulin within the colloid. The thyroglobulin was synthesised in the ER of the follicular cell and secreted into the colloid. Thyroid-stimulating hormone (TSH) released from the pituitary gland binds the TSH receptor ( a Gs protein-coupled receptor) on the basolateral membrane of the cell and stimulates the endocytosis of the colloid. The endocytosed vesicles fuse with the lysosomes of the follicular cell. The lysosomal enzymes cleave the T4 from the iodinated thyroglobulin. These vesicles are then exocytosed, releasing the thyroid hormones. 5’-Deiodinase convert Thyroxin to Triiodothyronin mainly in the peripheral tissues (80%). Thyroid Hormone Synthesis The steps in this process are as follows: Thyroid Hormone Synthesis
- 8. 20‐Sep‐13 8 Thyroid Hormone Synthesis: Organification and coupling Iodination (Organification) Coupling H2O2 H2O2 Thyroid gland contains about 8000 μg iodide ~90% is in an organic form At least 2 weeks reserve is stored Form in which stored is the modified thyroglobulin In response to TSH, colloid droplets form at apical surface by endocytosis of luminal colloid Colloid droplets contain thyroglobulin with T3 and T4 attached and with MIT and DIT attached Can be stored in this form. Thyroid Hormone: Storage
- 9. 20‐Sep‐13 9 Thyroid Hormone Transportation Thyroid hormones are not very soluble in water (but are lipid- soluble). In circulation, bound to: oThyroid hormone-binding globulin (TBG) o 70% of T3 & T4 oTransthyretin o 10% of T4 and very little of T3 oAlbumin o 25% of T3 and 15% of T4 Less than 1% of thyroid hormone is found free in the circulation. Only free and albumin-bound thyroid hormone is biologically available to tissues. Regulation of Thyroid hormone production Regulation by Iodide: The rate of iodine uptake and incorporation into thyroglobulin is influenced by the amount of iodide available: - low iodide levels increase iodine transport into follicular cells - high iodide levels decrease iodine transport into follicular cells Thus, there is negative feedback regulation of iodide transport by iodide.
- 10. 20‐Sep‐13 10 Endocrine regulation of Thyroid hormone secretion Wolff–Chaikoff effect The Wolff–Chaikoff effect is a reduction in thyroid hormone levels caused by ingestion of a large amount of iodine. It is generally seen only in patients with either autoimmune thyroid disease (eg. Graves disease) or with patients with severe hyperthyroidism It is an autoregulatory phenomenon that inhibits organification (oxidation of iodide) in the thyroid gland, the formation of thyroid hormones inside the thyroid follicle, and the release of thyroid hormones into the bloodstream. The Wolff–Chaikoff effect can be used as a treatment principle against hyperthyroidism (especially thyroid storm) by infusion of a large amount of iodine to suppress the thyroid gland.
- 11. 20‐Sep‐13 11 Thyroid Stimulating Hormone (TSH) • Thyroid-stimulating hormone (TSH) is produced by thyrotroph cells of the anterior pituitary. • TSH is a glycoprotein hormone composed of two subunits: - alpha subunit (common to LH, FSH, TSH) - TSH beta subunit, which gives specificity of receptor binding and biological activity LH FSH TSH LH FSH TSH TSH mode of action
- 12. 20‐Sep‐13 12 Other Factors Regulating Thyroid Hormone Levels Diet: a high carbohydrate diet increases T3 levels, resulting in increased metabolic rate (diet-induced thermogenesis). Low carbohydrate diets decrease T3 levels, resulting in decreased metabolic rate. Cold Stress: increases T3 levels in other animals, but not in humans. Any condition that increases body energy requirements (e.g., pregnancy, prolonged cold) stimulates hypothalamus TRH TSH (Pit)
- 13. 20‐Sep‐13 13 Actions of Thyroid Hormones Thyroid hormones are essential for normal growth of tissues, including the nervous system. Lack of thyroid hormone during development results in short stature and mental deficits (cretinism). Thyroid hormone stimulates basal metabolic rate. Required for GH and prolactin production and secretion Required for GH action Increases intestinal glucose reabsorption (glucose transporter) Increases mitochondrial oxidative phosphorylation (ATP production) One Major Target Gene of T3: The Na+/K+ ATPase Pump Pumps sodium and potassium across cell membranes to maintain resting membrane potential Activity of the Na+/K+ pump uses up energy, in the form of ATP About 1/3 of all ATP in the body is used by the Na+/K+ ATPase T3 increases the synthesis of Na+/K+ pumps, markedly increasing ATP consumption. T3 also acts on mitochondria to increase ATP synthesis The resulting increased metabolic rate increases thermogenesis (heat production).
- 14. 20‐Sep‐13 14 Mode of Action of Thyroid Hormone Mono carboxylate transporter (MCT8) The transport of T3 into target cells occurs by thyroid hormone transporters and subsequent binding of thyroid receptor/retinoic acid (RXR) dimmers, which stimulate transcription of target genes. Thyroxine preferentially binds αVβ3 integrins to stimulate MAPK signaling pathways; T4 and rT3 stimulate actin polymerization. Triiodothyronine has also been shown to affect several mitochondrial functions and NO production via PI3K activation. All of these functions rely on deiodinase (D) activities (denoted as D1–D3). Thyroid hormone action and metabolism in the cells.
- 15. 20‐Sep‐13 15 Thyroid Hormone Deficiency: Hypothyroidism Early onset: delayed/incomplete physical and mental development Later onset (youth): Impaired physical growth Adult onset (myxedema) : gradual changes occur. Tiredness, lethargy, decreased metabolic rate, slowing of mental function and motor activity, cold intolerance, weight gain, goiter, hair loss, dry skin. Eventually may result in coma. Causes: (insufficient iodine, lack of thyroid gland, lack of hormone receptors, lack of TH binding globulin….)
- 16. 20‐Sep‐13 16 How is Hypothyroidism Related to Goiter? During iodine deficiency, thyroid hormone production decreases. This results in increased TSH release (less negative feedback). TSH acts on thyroid, increasing blood flow, and stimulating follicular cells and increasing colloid production. Thyroid Hormone Excess: Hyperthyroidism Emotional symptoms (nervousness, irritability), fatigue, heat intolerance, elevated metabolic rate, weight loss, goiter, muscle wasting, apparent bulging of eyes, may develop congestive heart failure. Also due to many causes (excessive TSH release, autoimmune disorders,…)
