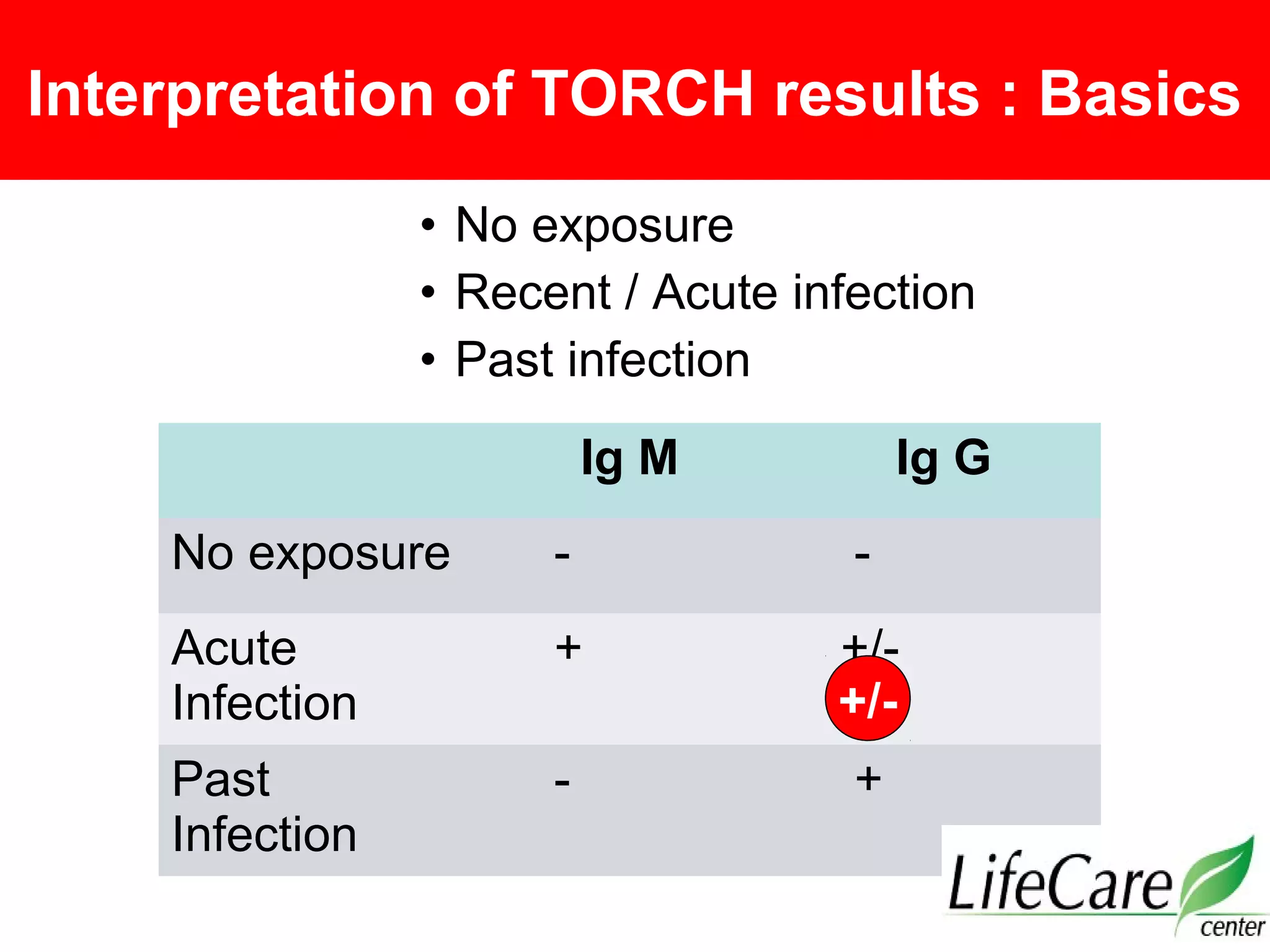
1. The document provides guidance on interpreting abnormal TORCH test results and managing infections during pregnancy through various case studies.
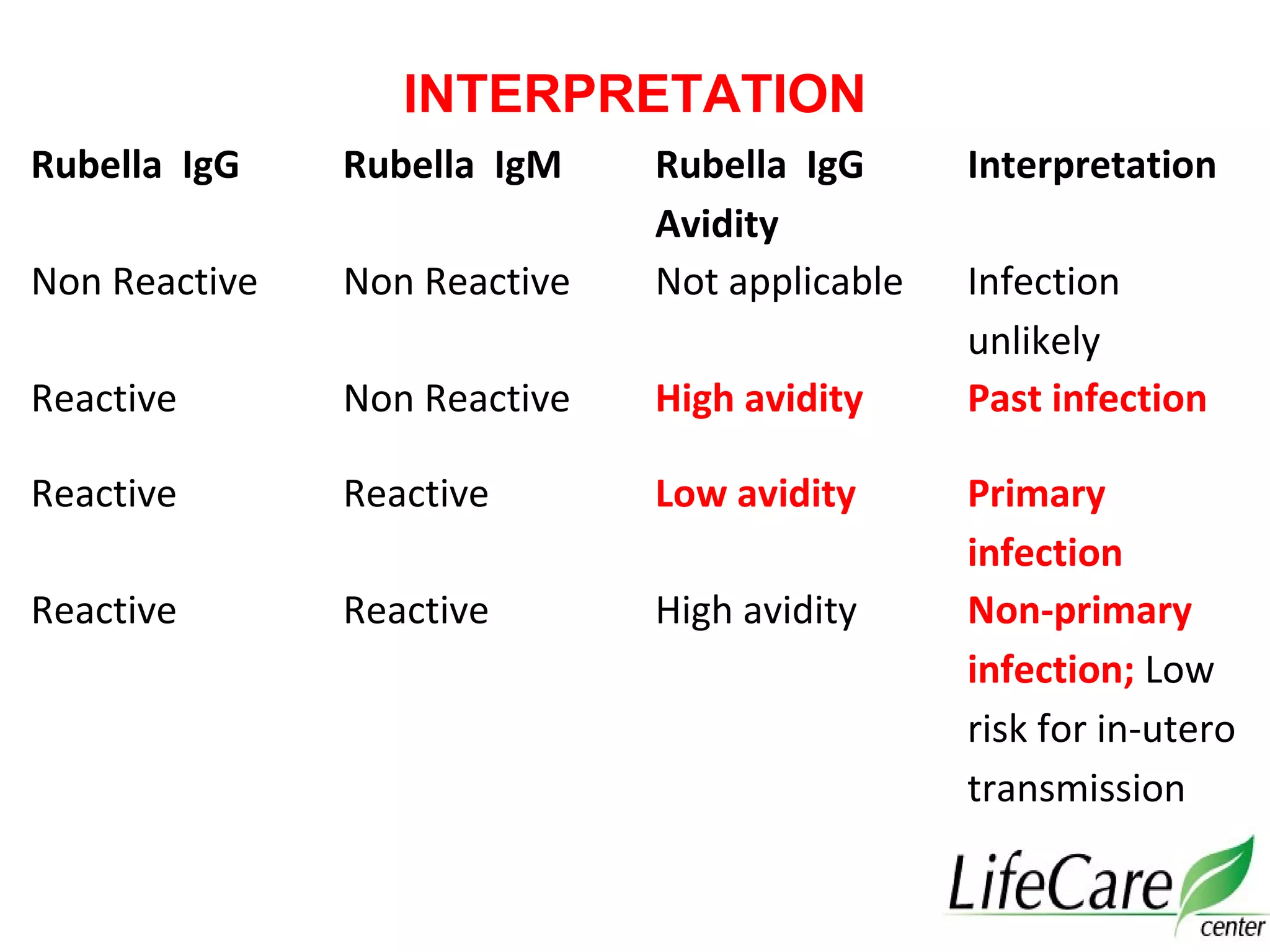
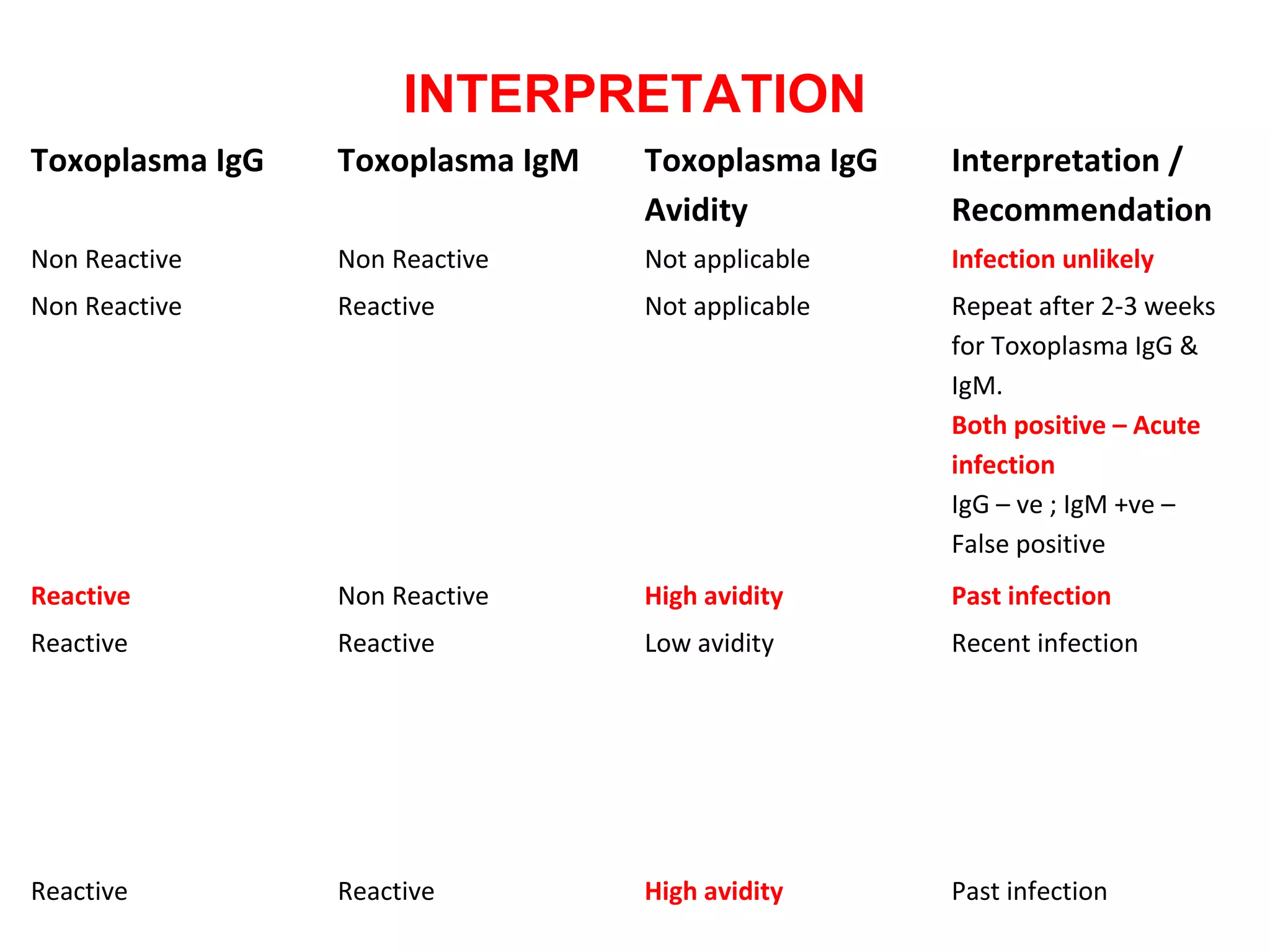
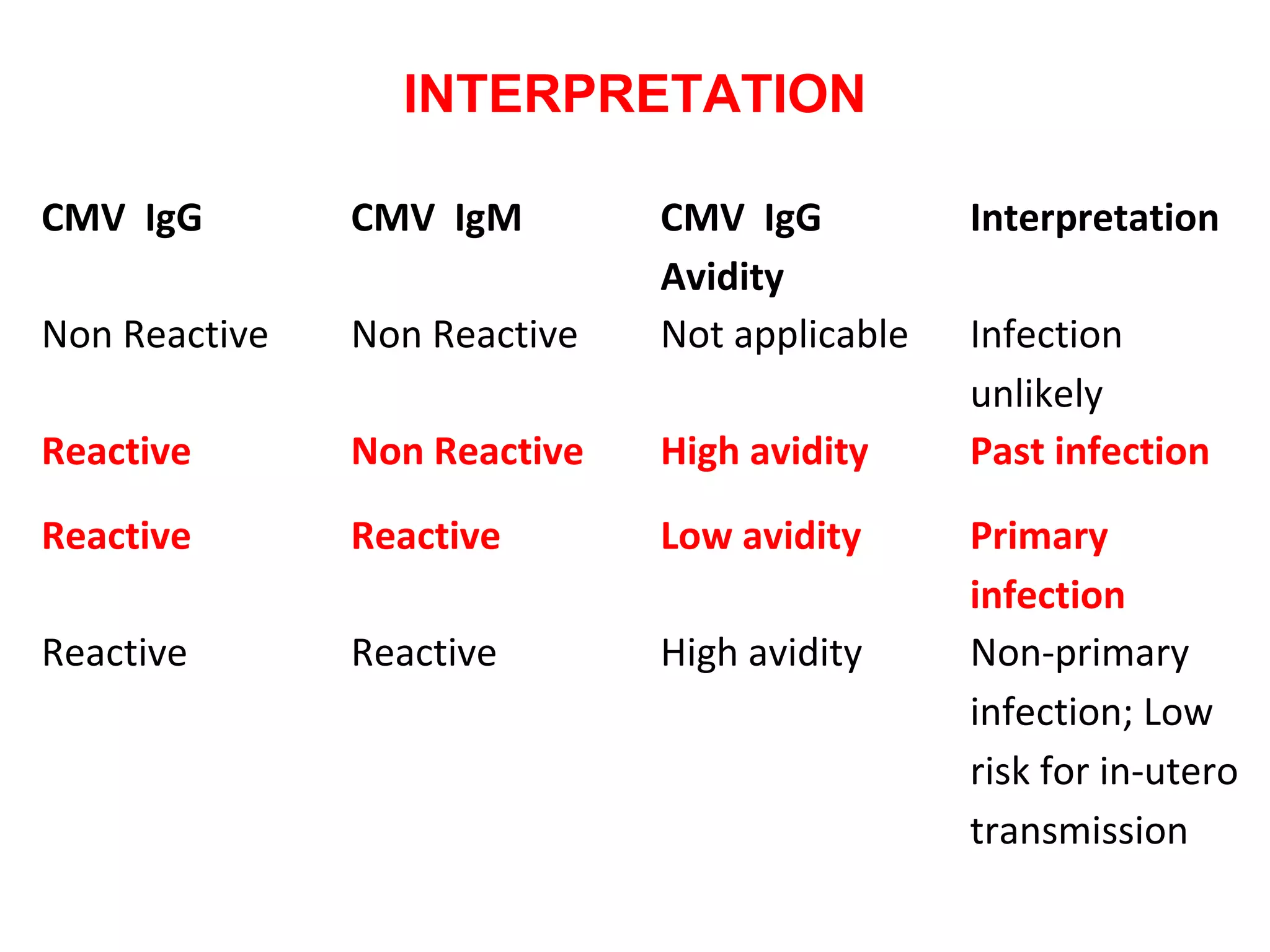
2. It emphasizes the importance of distinguishing between primary and non-primary infections using IgG avidity and IgM/IgG levels to guide treatment and counseling.
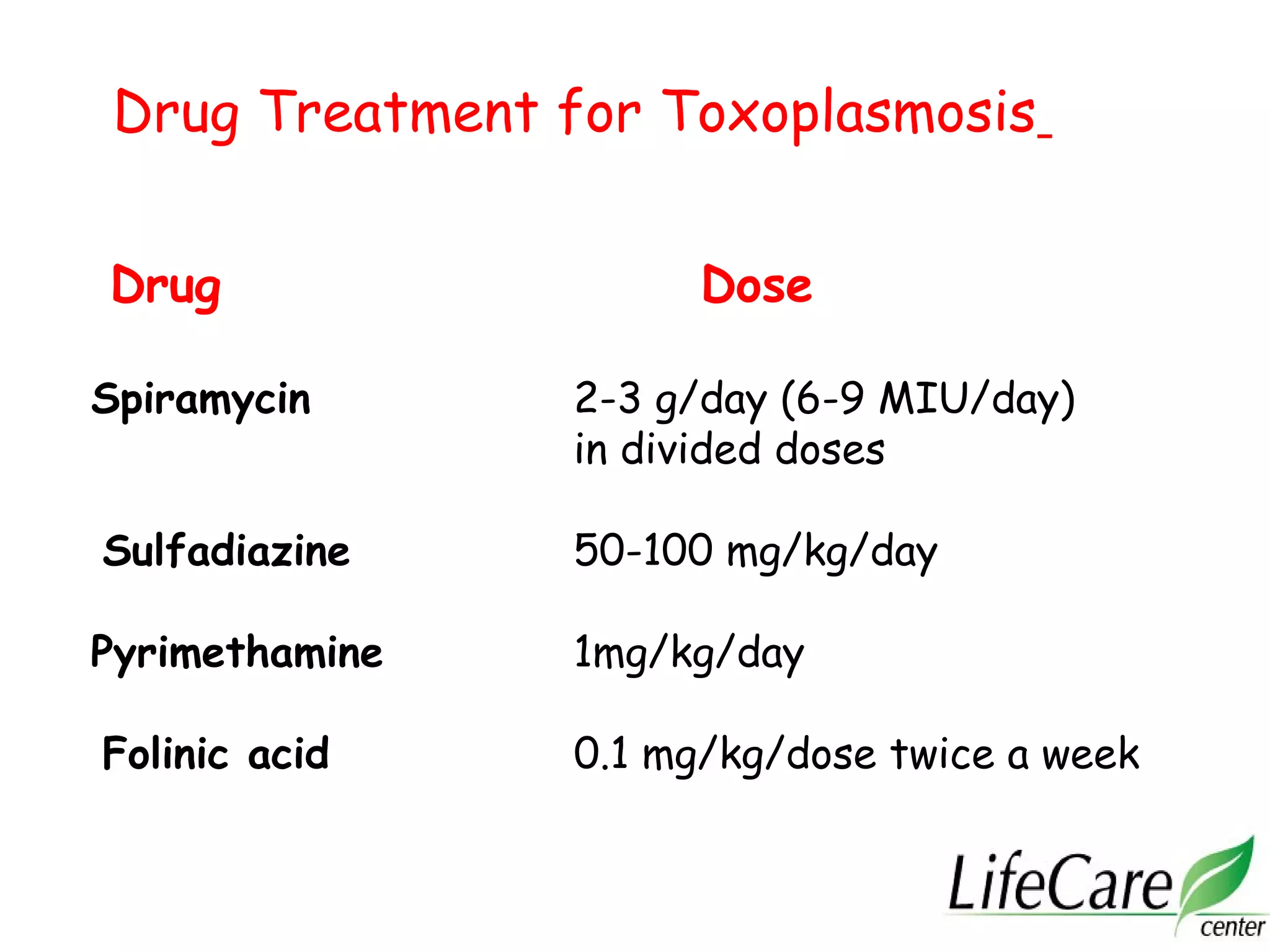
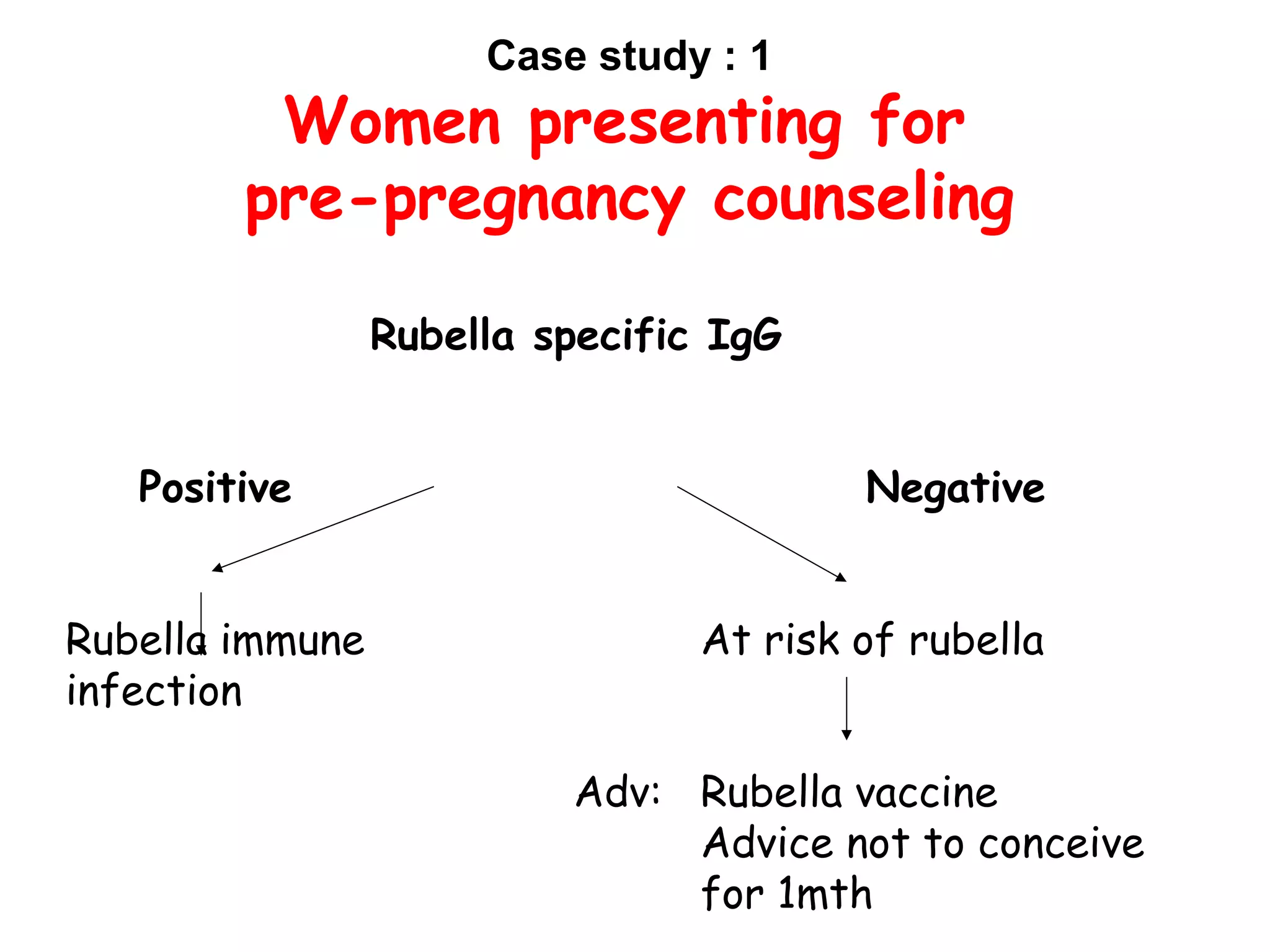
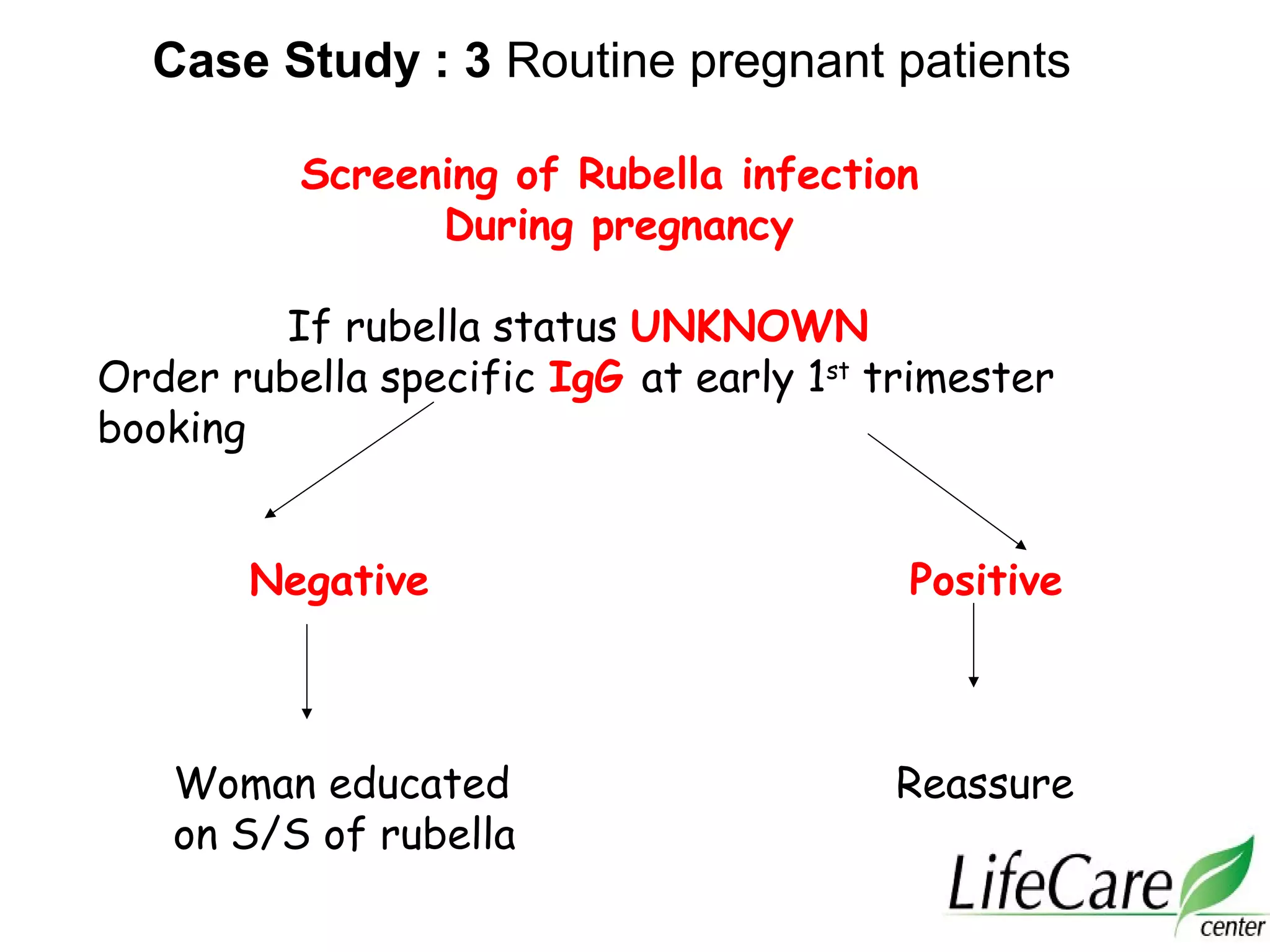
3. For toxoplasmosis, rubella, CMV, and herpes infections, treatment and management strategies depend on the gestational age and whether the infection is primary or non-primary. Termination may be advised for early primary infections while recurrent infections pose lower risk.