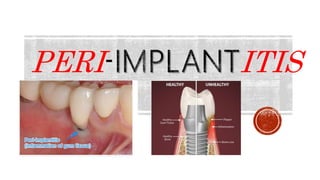
Peri implantitis
- 1. PERI ITIS
- 2. Swedish orthopedic surgeon and research professor. PER INGVAR BRANEMARK
- 3. IMPLANTS ARE USED AS REPLACEMENT FOR NATURAL ROOT Dental implants?????? Why Maintenance of alveolar bone……
- 11. PERI-IMPLANT MUCOSITIS Inflammatory changes are confined to soft tissues surrounding an implant
- 12. Similar to gingivitis- BACTERIAL PLAQUE
- 13. Similar to gingivitis Symptoms of inflammation Bleeding on probing Difference in morphology of periimplant mucosa and gingiva around tooth and lack of light transmission through metal may mask visible signs of inflammation Suppuration and slight increase in PPD may be present
- 15. mobility
- 17. Bacterial infection Biomechanical factors-excess forces Co-factors- smoking, compromised host, traumatic surgery….
- 18. Class I : slight horizontal bone loss with minimal peri-implant defect Class 2: moderate horizontal bone loss with isolated vertical defect Class 3: moderate to advanced horizontal bone loss with broad circular bony defect Class 4: advanced horizontal bone loss with broad circumferential vertical defect as well as loss of oral and vestibular bony wall
- 19. CLINCIAL ASSESSMENT: inflammation signs, BOP, suppuration, mobility, peri- implant radiography PERI-IMPLANT PROBING: USE ONLY BLUNT ,STRAIGHT PLASTIC PERIODONTAL PROBE Probing depth of more than 4mm suggestive of peri-implant disease
- 21. MOMBELLI suggested 5 considerations in periimplantitis therapy 1. Removal of bacterial biofilm 2.Decontamination and conditioning of implant surface 3.Correction via reduction or elimination of site that cannot be maintained by oral hygiene measures 4.Establishment of effective plaque control regime 5.Re-osseointegration
- 22. Treatment of periimplantitis Initial therapeutic phase Surgical phase
- 23. INITIAL THERAPEUTIC PHASE Occlusal therapy-prosthesis analysis and occlusal evaluation Anti-infective therapy-remove plaque with plastic instruments ,irrigate pockets with 0.12% chlorhexidine Systemic antibiotics: doxycycline, metronidazole, or combination of amox and metronidazole Implant surface preparation: in periimplantitis implant surface is contaminated with bacteria and its byproducts.thus wound healing is compromised. Air powder abrasive Apply tetracycline HCL Lasers –CO2
- 24. Periimplant resective therapy-Flap is raised and bone recontouring is done. And sutured by apically positioning the flap. Done in peri-implant lesions with horizontal bone loss or moderate vertical bone defects. Periimplant regenerative therapy- guided bone regeneration in moderate to deep vertical defects . Surgical therapy includes removal of granulation tissue after flap elevation, implant surface preparation and use of bone grafts and barrier membranes. Re-osseointegration: treatment goal – denovo bone formation at the portion of implant that has lost its osseointegration in the inflammatory process.
- 25. CIST Cumulative Interceptive Supportive Therapy Protocol for monitoring healthy implants and interception of peri-implant diseases.
- 26. CIST PROTOCOL A (mechanical debridement) PPD < 4mm , oral hygiene improved by scaler, rubber cup and paste. CIST PROTOCOL A+ B ( antiseptic therapy) PPD 4-5mm chlorhexidine is used with step A CIST PROTOCOL A+B+C (antibiotic therapy) PPD > or = to 6mm ,tetracycline fibers for 10 days and systemic antibiotic for 10 days along with step A+B CIST PROTOCOL A+B+C+D(regeneration and resective therapy) Considerable amount of bone loss and pocket depth are present surgical therapy along with step A+B+C.
- 28. GOAL OF CIST: to intercept peri-implant tissue destruction as early as possible.
- 29. PLAQUE CONTROL INTERDENTAL CLEANING AIDS PERIODIC RECALL