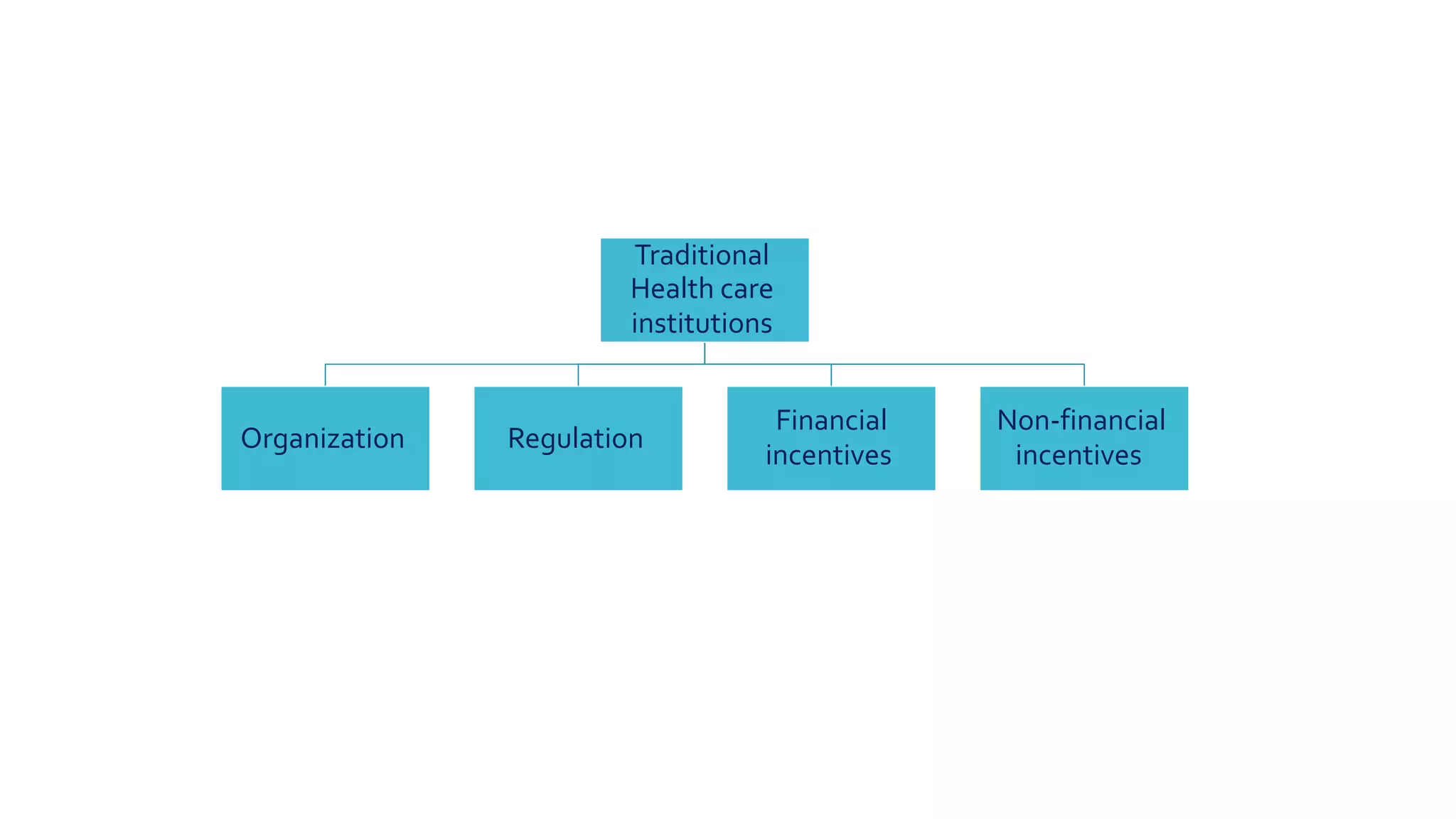
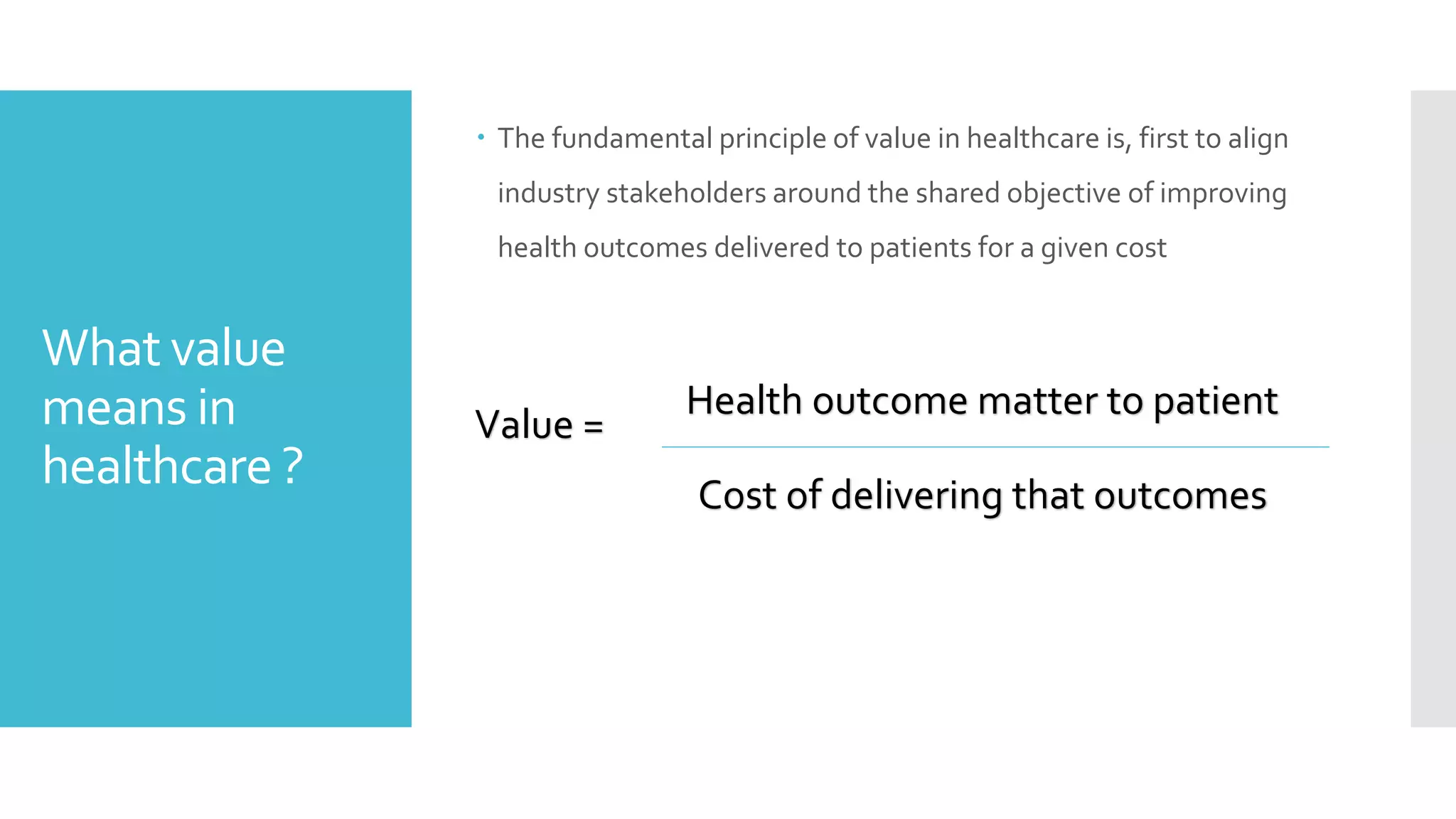
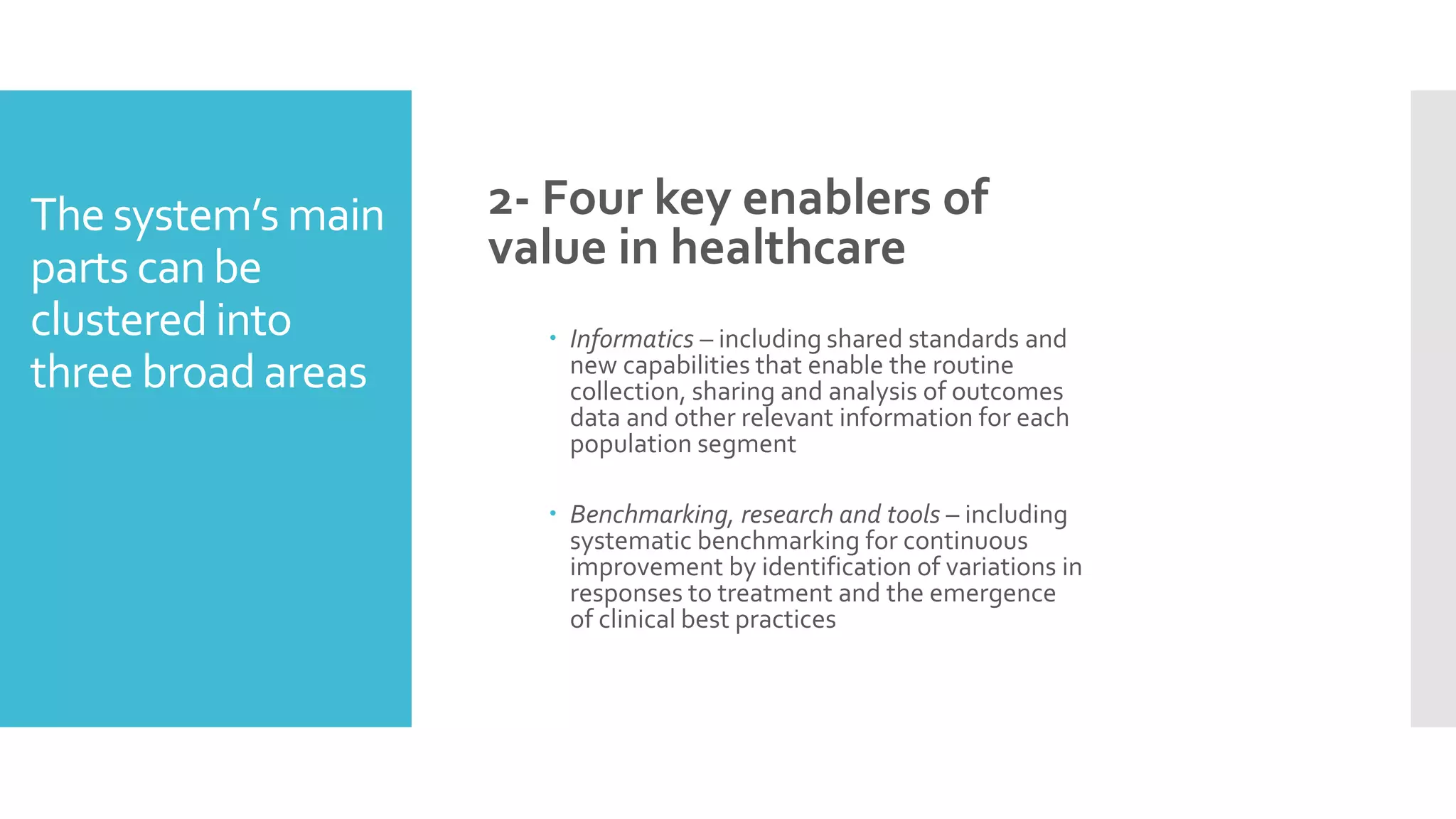
Value in healthcare aims to improve patient outcomes while lowering costs. It rewards providers for quality rather than quantity of care. While some progress has been made through examples like integrated systems in India and Germany that lower costs through better processes, value-based care has not been widely adopted due to barriers like entrenched financial incentives that prioritize volume over value. Fully realizing value-based care requires health informatics to track outcomes, benchmarking to share best practices, alternative payment models, and delivery innovations to better coordinate care.