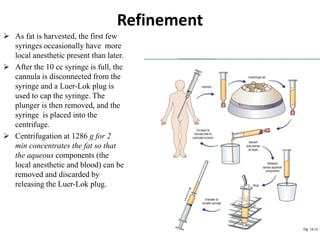
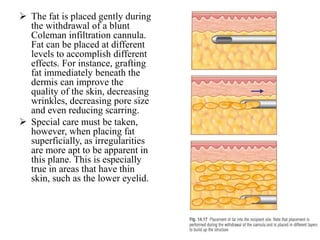
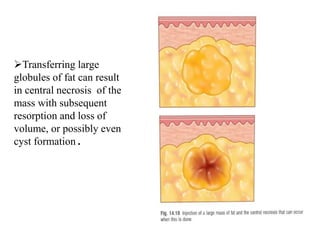
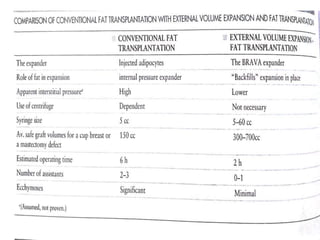
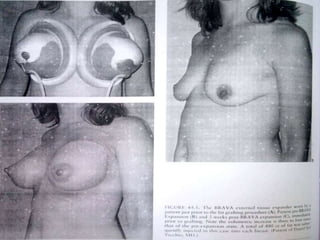
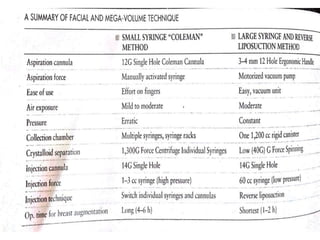
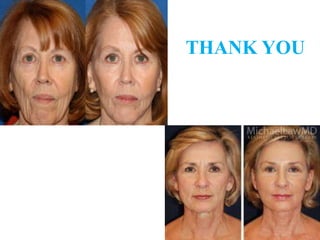
This document discusses structural fat grafting techniques. It provides an overview of the history and concepts behind fat grafting, outlines the surgical technique including gentle fat harvesting, refinement through centrifugation, and placement in small aliquots. Key areas it can be used for restoration of volume in the face, hands and body are mentioned. Proper patient selection and post-operative care including dressings and massage are also summarized.