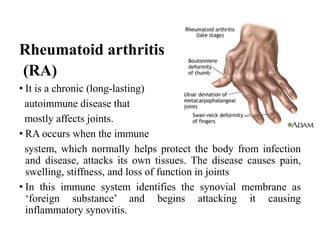
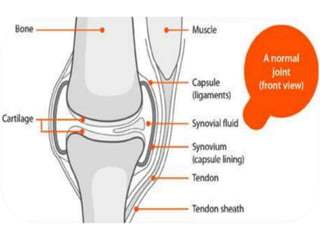
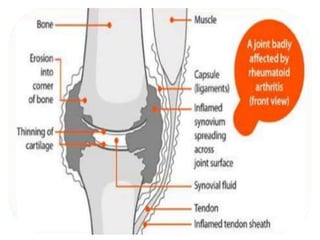
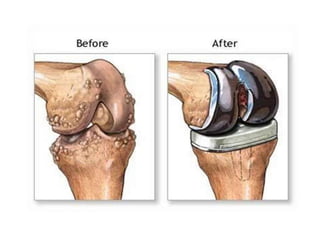
This document provides an overview of arthritis, detailing its types, symptoms, risk factors, and treatment options. It explains the differences between common forms of arthritis, such as osteoarthritis and rheumatoid arthritis, and outlines management strategies including medication, physical therapy, and possible surgical interventions. Additionally, the document highlights that while there is no cure, various treatments can help manage symptoms effectively.