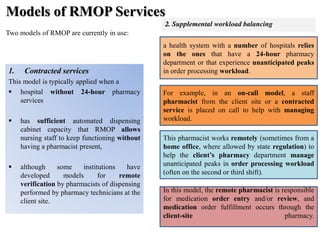
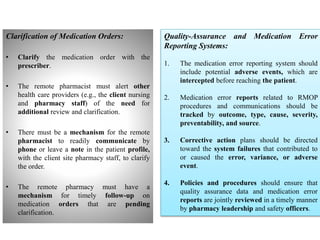
The document outlines guidelines for remote medication order processing (RMOP), emphasizing the need for health-system policies that ensure quality assurance, safety, and access to drug information while maintaining privacy and compliance with regulations. It describes various RMOP models, the essential roles of pharmacists, and the importance of training, communication, and problem resolution within remote and client sites. The conclusion advocates for 24-hour pharmacist accessibility and offers a framework for safely implementing RMOP in health systems.