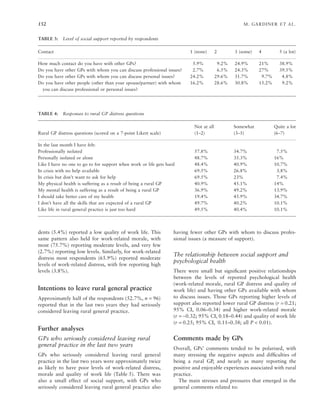
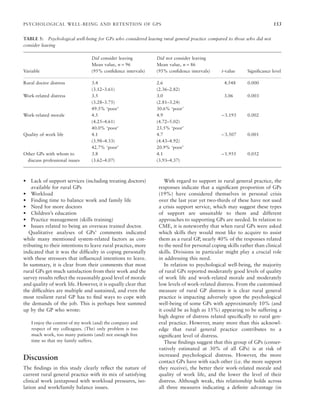
This study examined the psychological well-being and retention of rural general practitioners (GPs) in South Australia. A survey of 187 rural GPs found that those seriously considering leaving rural practice reported higher work-related distress, lower work-related morale, and lower quality of work life than those not considering leaving. GPs considering leaving also reported having fewer colleagues with whom to discuss professional issues. The results indicate that psychological interventions targeting stress reduction and coping mechanisms, such as cognitive behavioral training and increased interaction with colleagues, may help increase retention of rural GPs by improving their psychological well-being.