This document discusses preventive prosthodontics at the primary, secondary, and tertiary levels. At the primary level, prevention includes oral hygiene, fluoride application, diet counseling, and protective devices like mouthguards. The secondary level focuses on early detection and treatment of issues like occlusal interferences, bruxism, and sleep apnea. Tertiary prevention aims to limit disability through complex treatments, rehabilitation with prosthetics, and carefully timed extractions to prevent ridge resorption.















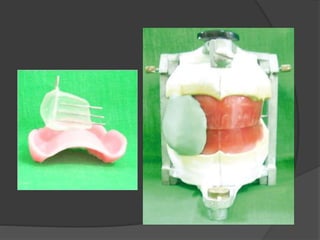
























![Overdentures
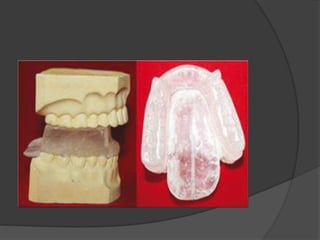
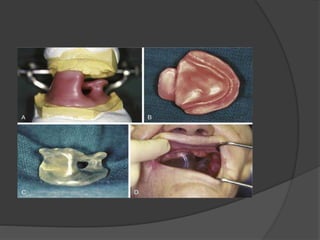
Some authors advised to retain the stumps beneath the
artificial teeth, and stated that these roots maintain the
alveolar bone health and height for longer duration.
This can be achieved by fabricating an overdenture.[36]
This can be advantageous in terms of conserving the
natural teeth, reducing the rate of residual ridge
resorption, proprioceptive feedback by existing
periodontal ligaments and thus controlling the occlusive
forces and preventing the rapid residual ridge
resorption.](https://image.slidesharecdn.com/preventiveprosthodontics-170620004102/85/Preventive-prosthodontics-45-320.jpg)