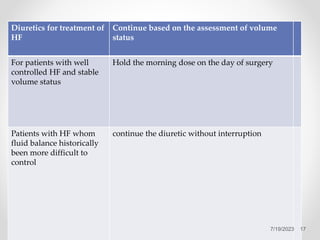
This document discusses guidelines for preoperative medication management. It provides guidance on cardiovascular, gastrointestinal, pulmonary, endocrine, diabetic, anticoagulant, psychiatric and other medications. The key principles are to continue most chronic medications to avoid complications from withdrawal, taper long-term steroids, hold certain medications like insulin on the day of surgery, and check coagulation status if anticoagulants are held preoperatively. The goal is to minimize perioperative risks while continuing necessary treatments.











































![Use of bridging
preoperatively
We generally reserve bridging for individuals
considered at very high or high risk of
thromboembolism , EXAMPLES
• recent [within the prior three months] stroke,
• mechanical heart valve,
• CHA2DS2-VASc score of 7 or 8
• if they require interruption of warfarin
45
7/19/2023](https://image.slidesharecdn.com/preoperativemedicationmanagementseminar-230719135103-4f3a8400/85/Preoperative-medication-management-seminar-pptx-45-320.jpg)
![Cont…
• In these cases, the bridging agent (e.g.,
therapeutic-dose subcutaneous low molecular
weight [LMW] heparin) is started three days
before surgery
46
7/19/2023](https://image.slidesharecdn.com/preoperativemedicationmanagementseminar-230719135103-4f3a8400/85/Preoperative-medication-management-seminar-pptx-46-320.jpg)









