Pp antianemic drugs
- 1. ANTIANEMIC DRUGS - 04/17/19 1patki
- 2. At the end of the session , student should be able to • Identify types of anemia. • Describe manifestations of megaloblastic anemia. • describe physiological functions of Vitamin B 12. • Identify clinical conditions where Vitamin B12 is uses , and mentions Folate trap • Enumerate the indications of Folic acid. 04/17/19 2patki
- 3. Anemia is a condition in which blood will have too few red blood cells 04/17/19 3patki
- 4. TYPES OF ANEMIAS Classified based on the size of red blood cells i.e. mean corpuscular volume (MCV) Microcytic: smaller than normal (under 80 fl) Normocytic:normal size (80-100 fl) Macrocytic: larger than normal (over 100 fl) femtoliters 04/17/19 4patki
- 5. MICROCYTIC ANEMIA Iron deficiency anemia: most common Paler & smaller than usual Normocytic anemia Overall Hb levels decreased red blood cell size (MCV) remains normal Causes: Acute blood loss, chronic disease, Aplastic anemia (bone marrow failure), Hemolytic anemia 04/17/19 5patki
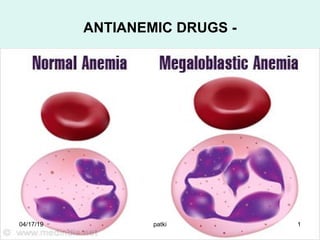
- 6. MACROCYTIC ANEMIA Megaloblastic anemia: deficiency of either Vitamin B12 or folic acid or both Folate deficiency: No neurological symptoms B12 deficiency : neurological symptoms present Pernicious anemia : autoimmune condition leading to poor absorption of vitamin B12 Alcoholism 04/17/19 6patki
- 7. Vitamine B12 (cyanocobalamine) Source Animals/plants do not synthesize, Microbes synthesize Animal source: liver, kidneys, sea fish, egg yolk, meat, cheese Vegetable source: Legumes Colonic microflora synthesize insufficient Streptomyces griseus: commercial source Daily requirement 1-3 μg; pregnancy & lactation: 3-5 μg. 04/17/19 7patki
- 8. Dietary and storage folate 04/17/19 8patki
- 9. Utilization of B12 Parietal cells Intrinsic factor B12 + Intrinsic factor Absorption (ileum) Total body storage: 4 mg Surgery and antibodies Liver (stored) Intrinsic factor Transcob alamine 04/17/19 9patki
- 10. INDICATIONS OF B12 Pernicious anemia Malabsorption Gastric mucosal damage Schilling test: diminished absorption of radioactively labelled vitamin B12. This is corrected with intrinsic factor + radioactive B12 04/17/19 10patki
- 11. Manifestations of B12 Symptoms of megaloblastic anemia Hematologic – macrocytic anemia Neurological – peripheral neuritis, poor memory etc. Psychiatric illness Neuropathies 04/17/19 11patki
- 12. Therapeutic use of B12 Due to lack of intrinsic factor Orally B-12 can not be given B-12 should be given parenterally (im/sc) Not given iv due to anaphylaxis Treatment is life long 04/17/19 12patki
- 13. TREATMENT REGIMEN 1-10 days = 30-100 μg Weekly = 100 μg Monthly = 100 μg 04/17/19 13patki
- 14. 04/17/19 14patki
- 15. FOLIC ACID (B-9) Dietary source: liver, green leafy vegetables, egg, meat, milk Absorbed from upper intestine. Folic acid DHFA CH3THFA Liver traps large amount of Ch3THFA and releases into the bile and again absorbed by enterohepatic circulation. 04/17/19 15patki
- 16. Folate Deficiency Malabsorption Chronic alcoholism Pregnancy and lactation Drug induced deficiency: Phenytoin, phenobarbitone, primidone, oral contraceptives etc. 04/17/19 16patki
- 17. Manifestations Epithelial damage, glossitis, enteritis, diarrhea, steatorrhoea, weight loss, sterility etc. Dietary source: Liver, green leafy vegetables, egg, meat, milk etc Daily requirement: 400 μg 04/17/19 17patki
- 18. Therapeutic Uses Megaloblastic anemia Prophylaxis: pregnancy, lactation, antiepileptic therapy, malabsoption etc. Folinic acid (leucovorin/citrovorum factor/5-formyl-THFA) readily converted to folic acid derivatives. Dihydrofolate reductase is not required. 04/17/19 18patki
- 19. ERYTHROPOIETIN Essential for normal erythropoiesis Produced by peritubular cells of the kidney during anemia and hypoxia 04/17/19 19patki
- 20. USES OF ERYTHROPOIETIN Anemia in chronic renal failure(sc/iv) Cancer chemotherapy induced anemia AIDS induced anemia Prophylaxis – anemia in premature infants Anemia – inflammatory conditions (Rheumatoid) Adverse effects: flu-like symptoms, mild hypertension, encephalopathy, occasionally convulsions, risk of thrombosis due to hematocrit rises. 04/17/19 20patki
- 21. ADVERSE EFFECTS OF ERYTHROPOIETIN Increased clot formation Hypertensive episodes Flu like symptoms lasting 2-4 hr 04/17/19 21patki
- 22. Granulocyte colony-stimulating factor (G- CSF) Stimulates neutrophil progenitors. intravenously or subcutaneously. 04/17/19 22patki
- 23. Granulocyte-macrophage colony-stimulating factor (GM-CSF) Stimulates many types of progenitor cell. intravenously, subcutaneously. Side effects: fever, rashes, bone pain, hypotension, git symptoms, arterial oxygen desaturation. 04/17/19 23patki
- 24. 04/17/19 24patki
- 25. 04/17/19 25patki
- 26. Which of the following defects is associated with megaloblastic anemia? – Defective RNA synthesis – Defective immunoglobulin synthesis – Defective globin synthesis – Defective DNA synthesis – Defective hemopoitic pathway. 04/17/19 26patki
- 27. What is a leading cause of anemia in a patient who is alcoholic? – Folate deficiency – Iron deficiency – Vitamin B 12 deficiency – Uridine triphosphate deficiency 04/17/19 27patki
- 28. – Most common disorder in clinical practice. – Charectarized by a decrease in the O2 carrying capacity of the blood due to reduced concentration of Hb or RBCS Iron deficiency anemia Pink of your health
- 29. IRON DEF ANAEMIA CHARACTERISED BY- • MICROCYTOSIS (presence of small erythrocytes). • HYPO CHROMIA ( poorly filled with haemoglobin). • POIKILOCYTOSIS (bizzare shaped cells). • ANISOCYTIOSIS (different shapes). •
- 30. DISTRIBUTION OF IRON IN THE BODY – Iron(Fe) is the essential body constituent . – Total body iron in an adult – 2.5 – 5 g (average 3.5g). – It is more in men - (50mg/kg) Than in women (38mg/kg) – It is distributed as follows : •Hemoglobin (Hb) – 66% •Iron stores ferritin and Haemosiderin – 25% •Myoglobin ( in muscles) – 3% •Parenchymal iron (in enzymes etc) – 6%
- 31. Loss of 100ml of blood (containing 15g Hb) means loss of 50mg elemental iron. To raise Hb level of blood by 1g/dl about 200mg of iron is needed. Daily requirement of iron Adult male – 0.5 – 1 mg (13mg/kg) Adult female – 1 – 2 mg (21mg/kg) (Menstruating) Infants – 60mg/kg Children – 25 mg/kg Pregnancy – 3.5 mg (80mg/kg) (Last 2 trimesters)
- 32. DIETARY SOURCES OF IRON Rich → liver, egg yolk, oyster, drybeans, dry fruits, wheat germ, yeast. Medium → meat, chicken, fish, spinach, banana, apple. Poor → milk and its products, root vegetables.
- 33. Iron absorption Average daily diet contains- 10-20mg of iron. Absorption occurs all over the intestine, but more in the upper part. There are two major forms of dietary iron. Heme iron, found primarily in red meats, is the most easily absorbed form. Majority of dietary iron is in ferric form. It is reduced to ferrous form before absorption. Absorption occurs through 2 separate iron transporters in the intestinal mucosal cells. •Divalent metal transporter – 1 (DMT 1) •Ferroportin
- 34. FACTORS FACILITATING FE ABSORPTION – Acid: By favouring dissolution and reduction of ferric form. – Reducing substances – Ascorbic acid. – Meat – By increasing Hcl secretionand providing heme iron. FACTORS IMPEDING FE ABS – Alkalies – (Antacids) Renders iron insoluble, oppose its reduction. – Phosphates (rich in egg yolk) – Phytates (maize, wheat) by complexing iron – Tetracyclines – Prescence of other foods in stomach.
- 35. MUCOSAL BLOCK • It is a mechanism to prevent entry of excess iron in the body • Iron reaching inside mucosal cell is eigther transported to plasma or oxidised to ferric form and complexed with apoferritin to form ferritin. • The ferritin stored on the mucosal cells is lost when they are shed (life span 2-4 days). • This is called ferritin curtain. • Thus the amount of iron entering into the body is governed by the iron status of the body and the erythropoietic activity.
- 36. Transport, utilization, storage and excretion. • Free iron is highly toxic. • It is converted to ferric form and complexed with a glycoprotein - transferrin (TF). • Iron is transported in to erythropoietic and other cells by attachment of transferrin to transferrin receptors (TFRS) which is engulfed by endocytosis. • Iron dissociates from complex and is utilised for Hb synsthesis while TF and TFR return to cell surface to carry fresh loads.
- 37. Cont… • Iron is stored in reticulo endothelial cells in liver, spleen bone morrow, also in hepatocytes & myocytes as ferritin and haemosiderin. • Daily excretion – 0.5mg daily (adult male) mainly as exfoliated G.I mucosal cells some RBC’s and in bile, desquamated skin. • In menstruating women – monthly menstrual loss may be averaged to 0.5-1 mg/day. • Excess iron is required during pregnancy for expansion of RBC mass, transfer to foetus and loss during delivery totaling about 700mg .
- 39. PREPARATIONS AND DOSAGE Oral iron This is the preferred route of iron administration. – Because • Dissociable Ferrous salts are inexpensive. •Have high iron content •Better absorbed than ferric salts. Some oral iron preparations •Ferrous sulphate – cheapest •Ferrous gluconate •Ferrous fumarate. •Colloidal ferric hydroxide •Ferric hydroxy poly maltose
- 40. • Sustained release preperations – not rational. • Most of iron absorbed in upper intestine – but these preperations release iron lower down. • Liquid formulations – may stain teeth. – Hence should be put back on tongue. DOSE A total of 200mg of elemental iron given daily in 3 divided doses – produce maximal haematopoietic response. Absorption of iron is much better when it is taken on empty stomach – side effects are also more on empty stomach. Prophylactic dose – 30 mg iron daily.
- 41. INDICATIONS OF IRON THERAPY PROPHYLATIC pregnancy ,menstruation ,blood donors . • THERAPEUTIC - to treat existing iron deficiency. • Nutritional deficiency. • Anaemia of infancy and pregnancy. • Anaemia due to acute or chronic blood loss. menorrhagia ,peptic ulcer, hookworm infestation.
- 42. ADVERSE EFFECTS OF ORAL IRON – Adverse effects are related to elemental iron content. 1. Epigastric pain 2. Heart burn 3. Nausea & vomiting 4. Staining of teeth 5. Metallic taste 6. Bloating, colic 7. Constipation
- 43. PARENTERAL IRON INDICATIONS 1. Oral iron is not tolerated - bowel upset is more. 2. Failure to absorb iron – mal absorption, Inflammatory bowel disease. 3. Non compliance to oral iron. 4. In prescence of severe deficiency with chronic bleeding. • Parenteral iron therapy needs calculation of the total iron requirement of the pt. • Iron requirement (mg) = 4.4 X body wt (kg) X Hb deficit (g/dl)
- 44. PARENTERAL IRON THERAPY PREPARATIONS: • IRON DEXTRAN for IMIV use {imferon} contra indicated in early pregnancy. • IRON SORBITOL CITRIC ACID COMPLEX{JECTOFER} for IM injection (urine turns black –iron sulfide formation).
- 45. • IRON CARBOHYDRATE COMPLEX {UNIFERON} - iron ,dextran sorbitol citric acid . - Given IM , each ml contains 50 mg of elemental iron. • Injection made by Z technique. • Test dose of 25 mg is given followed by 100 mg . • IV infusion is given at the rate of 10 drops per minute.
- 46. IV Route • Iron dextran • Ferrous –sucrose • Sodium ferric gluconate After a test dose with 0.5ml, 2ml to be given over 10min. Alternatively dose diluted in 500ml glucose/saline –to be infused over 6-8hrs. • Should be stopped if pt complains of giddiness, paraesthesias and tightness in the chest.
- 47. ADVERSE EFFECTS OF PARENTERAL IRON LOCAL – pain at injection site pigmentation of skin, sterile abscess. SYSTEMIC – fever, head ache, joint pains, flushing, palpitation, chest pain, dyspnoea, lymphnode enlargement.
- 48. USES IRON DEFICIENCY ANEMIA Most imp indication for medicinal iron. CAUSES: 1.Nutritional deficiency 2.Chronic bleeding from G.I tract (common cause) (ulcers, hook worm infestation) 3.Repeated attacks of malaria. 4.Chr. inflammatary diseases.
- 49. 04/17/19 patki 49 BE HAPPY BE INTELLIGENT One tab of Fersolate per day
Editor's Notes
- rheumatois
