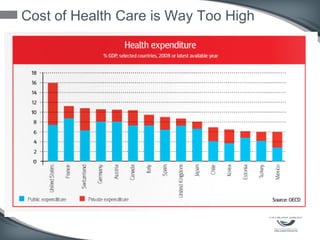
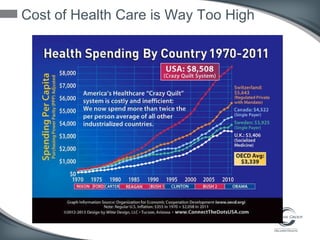
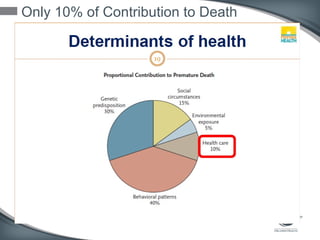
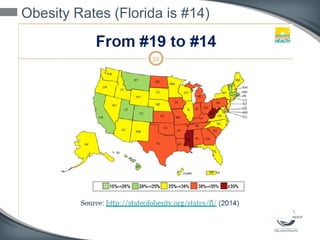
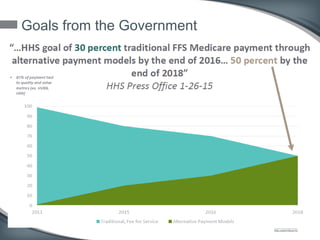
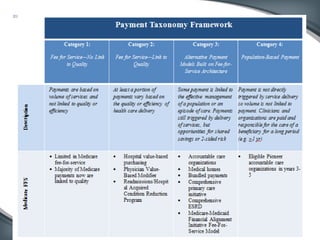
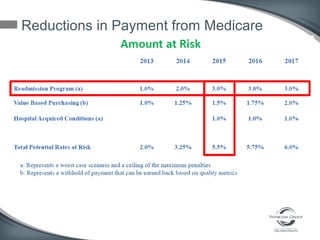
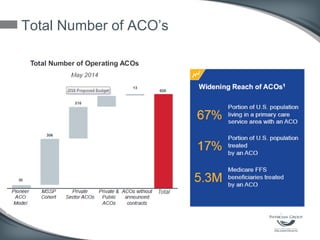
This document discusses the U.S. healthcare system's transition from fee-for-service payment to value-based payment methods. It notes that healthcare costs are too high and the government's goals include reducing Medicare, Medicaid spending by $400 billion over 10 years through mechanisms like accountable care organizations (ACOs) and reduced provider payments. ACOs are groups of doctors and hospitals that coordinate care for Medicare patients while aiming to lower costs through shared savings arrangements. One example, Collaborative Care of Florida, saved $3 million in its first year in 2013 through an ACO program.