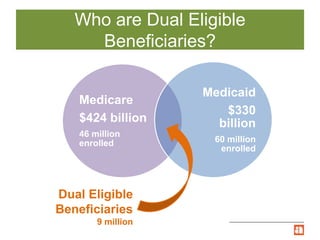
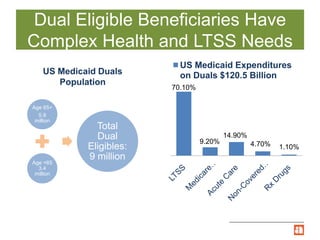
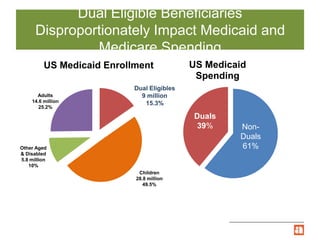
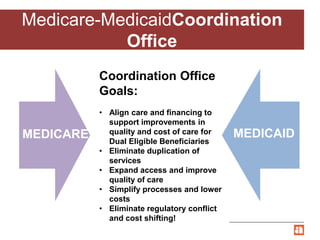
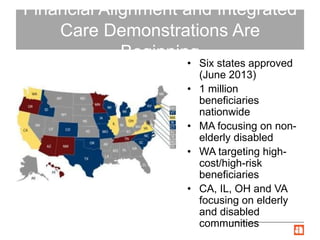
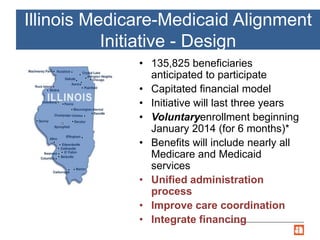
The document summarizes Illinois' Medicare-Medicaid Alignment Initiative to integrate care and financing for dual eligible beneficiaries (9 million Americans enrolled in both Medicare and Medicaid). It aims to improve quality of care while lowering costs by 1-5% annually through care coordination and capitated managed care plans. Key aspects include voluntary enrollment of 135,825 beneficiaries in capitated financial models, unified processes, and testing through the Center for Medicare and Medicaid Innovation's financial alignment demonstrations in six states.