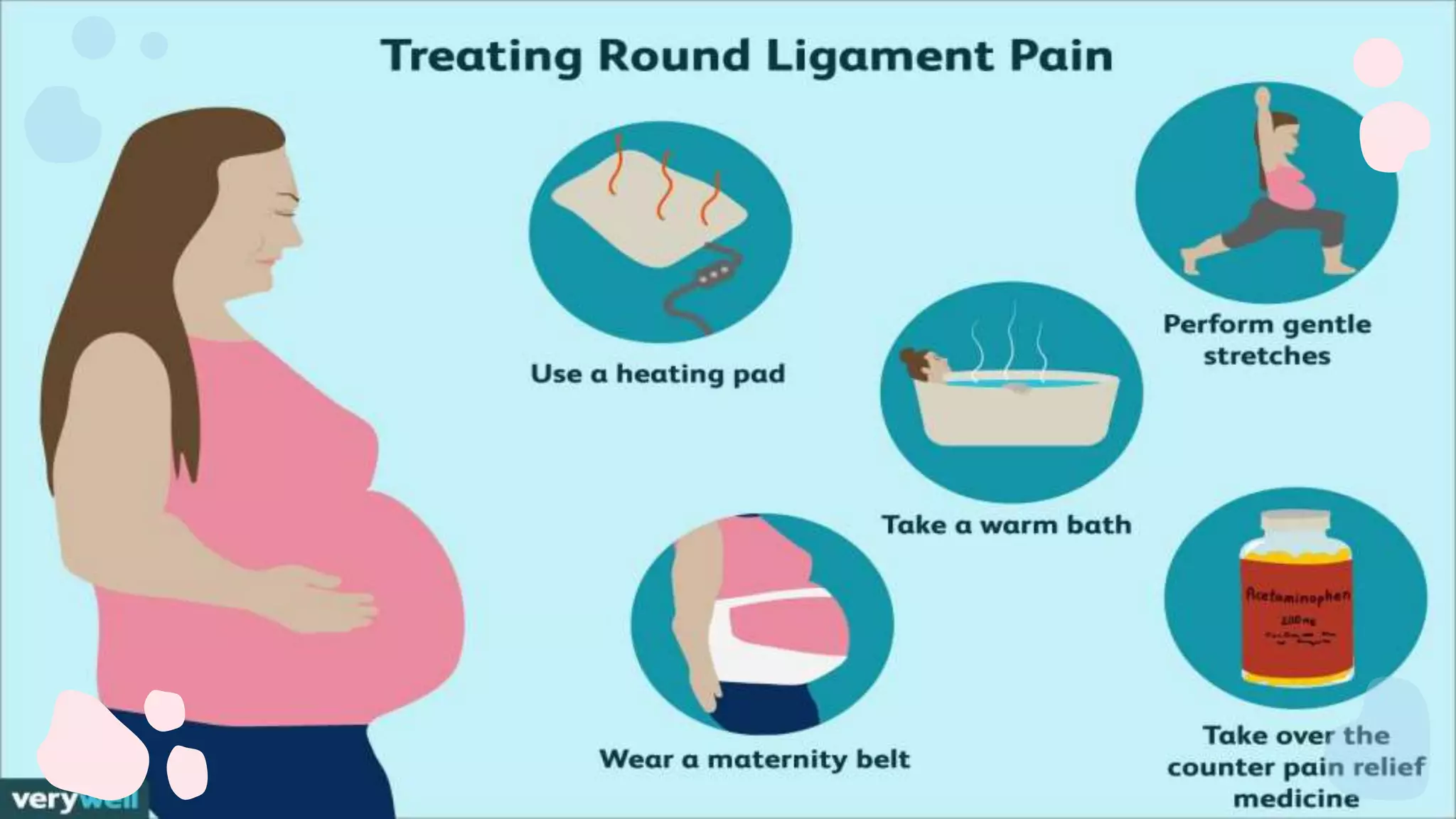
This document provides an outline for a presentation on minor discomforts during pregnancy. It is divided into three sections focusing on the first, second, and third trimesters. For each trimester, the most common minor discomforts are listed along with their causes and nursing care recommendations. The objectives of the presentation are also stated. Some of the minor discomforts discussed include nausea and vomiting, urinary frequency, breast tenderness, constipation, heartburn, and shortness of breath. For each issue, specific causes related to hormonal and physical changes in pregnancy are described, as well as non-pharmacological nursing interventions.