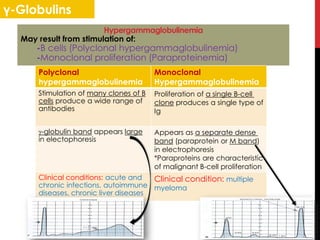
Plasma contains over 300 proteins that serve important functions like transport, maintaining oncotic pressure, defense, and clotting. The major classes of plasma proteins include albumin, globulins, fibrinogen, and immunoglobulins. Diseases can affect plasma protein levels and cause hypo- or hyperproteinemia, changing the electrophoretic pattern seen on protein tests.