INTUSSUSCEPTION.pptx
•Download as PPTX, PDF•
2 likes•183 views
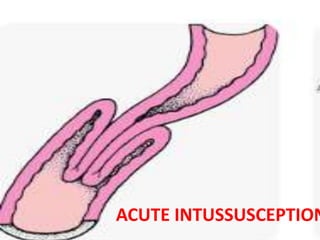
ACUTE INTUSSUCEPTION
Report
Share
Report
Share
Recommended
More Related Content
What's hot
What's hot (20)
Infantile hypertrophic pyloric stenosis by pp mubashir

Infantile hypertrophic pyloric stenosis by pp mubashir
Presentation1, radiological imaging of hypertrophic pyloric stenosis.

Presentation1, radiological imaging of hypertrophic pyloric stenosis.
Similar to INTUSSUSCEPTION.pptx
Similar to INTUSSUSCEPTION.pptx (20)
Per abdomen examination - Clinical Methods - Abdomen

Per abdomen examination - Clinical Methods - Abdomen
More from DR.P.S SUDHAKAR
More from DR.P.S SUDHAKAR (20)
Recently uploaded
Independent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for Real Meet
WHATSAPP On Here: 9352988975
Today call girl service available 24X7*▬█⓿▀█▀ 𝐈𝐍𝐃𝐄𝐏𝐄𝐍𝐃𝐄𝐍𝐓 CALL 𝐆𝐈𝐑𝐋 𝐕𝐈𝐏 𝐄𝐒𝐂𝐎𝐑𝐓 SERVICE ✅
⭐➡️HOT & SEXY MODELS // COLLEGE GIRLS
AVAILABLE FOR COMPLETE ENJOYMENT WITH HIGH PROFILE INDIAN MODEL AVAILABLE HOTEL & HOME
★ SAFE AND SECURE HIGH CLASS SERVICE AFFORDABLE RATE
★ 100% SATISFACTION,UNLIMITED ENJOYMENT.
★ All Meetings are confidential and no information is provided to any one at any cost.
★ EXCLUSIVE PROFILes Are Safe and Consensual with Most Limits Respected
★ Service Available In: - HOME & HOTEL 24x7 :: 3 * 5 *7 *Star Hotel Service .In Call & Out call SeRvIcEs :
★ A-Level (5 star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)Receive advanced sexual techniques in different mode make their life more pleasurable #G05.
★ Spending time in hotel rooms
★ BJ (Blowjob Without a Condom)
★ Completion (Oral to completion)
★ Covered (Covered blowjob Without condom
100% SAFE AND SECURE 24 HOURS SERVICE AVAILABLE HOME AND HOTEL SERVICESIndependent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for R...

Independent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for R...Ahmedabad Call Girls
🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludhiana Call Girls Service 🍑👄 Call Girls In Ludhiana Book Now :- 98157-77685
Our agency presents a selection of young, charming call girls available for bookings at Oyo Hotels. Experience high-class escort services at pocket-friendly rates, with our female escorts exuding both beauty and a delightful personality, ready to meet your desires. Whether it's Housewives, College girls, Russian girls, Muslim girls, or any other preference, we offer a diverse range of options to cater to your tastes.
We provide both in-call and out-call services for your convenience. Our in-call location in Delhi ensures cleanliness, hygiene, and 100% safety, while our out-call services offer doorstep delivery for added ease.
We value your time and money, hence we kindly request pic collectors, time-passers, and bargain hunters to refrain from contacting us. l Ludhiana, Majestic Grand Hotel, Ramada by Wyndham Ludhiana City Centre, Park Plaza Ludhiana, Windsor Fountain, G.T Road Ludhiana escort all Ludhiana service Russian available model female girls in Ludhiana VIP Lo price personal Ludhiana off class call girls payment high profile model and female escort 70% Off On Your First Booking Ludhiana Call Girls Service Cash Payment
Welcome to DILPREET Ludhiana Call Girl Service, the Trusted call girl agency around. We Offer 70% Discount On Your First Booking For Ludhiana Call Girls Service Cash Payment is available.🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludh...

🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludh...dilpreetentertainmen
❤️Ludhiana Call Girls ☎️98157-77685☎️ Call Girl service in Ludhiana☎️Ludhiana Call Girls Service ☎️ Call Girls In Ludhiana Ludhiana City Centre, Park Plaza Ludhiana, Windsor Fountain, G.T Road Ludhiana escort all Ludhiana service Russian available model female girls in Ludhiana VIP Lo price personal Ludhiana off class call girls payment high profile model and female escort 70% Off On Your First Booking Ludhiana Call Girls Service Cash Payment
Welcome to DILPREET Ludhiana Call Girl Service, the Trusted call girl agency around. We Offer 70% Discount On Your First Booking For Ludhiana Call Girls Service Cash Payment is available.❤️Ludhiana Call Girls ☎️98157-77685☎️ Call Girl service in Ludhiana☎️Ludhiana...

❤️Ludhiana Call Girls ☎️98157-77685☎️ Call Girl service in Ludhiana☎️Ludhiana...dilpreetentertainmen
(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The Service Of A Mumbai Call Girl At Any Time
WHATSAPP On Here:9920725232
Today call girl service available 24X7*▬█⓿▀█▀ 𝐈𝐍𝐃𝐄𝐏𝐄𝐍𝐃𝐄𝐍𝐓 CALL 𝐆𝐈𝐑𝐋 𝐕𝐈𝐏 𝐄𝐒𝐂𝐎𝐑𝐓 SERVICE ✅
⭐➡️HOT & SEXY MODELS // COLLEGE GIRLS
AVAILABLE FOR COMPLETE ENJOYMENT WITH HIGH PROFILE INDIAN MODEL AVAILABLE HOTEL & HOME
★ SAFE AND SECURE HIGH CLASS SERVICE AFFORDABLE RATE
★ 100% SATISFACTION,UNLIMITED ENJOYMENT.
★ >> 03-05-2024 (GRV)
★ All Meetings are confidential and no information is provided to any one at any cost.
★ EXCLUSIVE PROFILes Are Safe and Consensual with Most Limits Respected
★ Service Available In: - HOME & HOTEL 24x7 :: 3 * 5 *7 *Star Hotel Service .In Call & Out call SeRvIcEs :
★ A-Level (5 star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)Receive advanced sexual techniques in different mode make their life more pleasurable.
★ Spending time in hotel rooms
★ BJ (Blowjob Without a Condom)
★ Completion (Oral to completion)
★ Covered (Covered blowjob Without condom
100% SAFE AND SECURE 24 HOURS SERVICE AVAILABLE HOME AND HOTEL SERVICES(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The S...

(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The S...Ahmedabad Call Girls
Punjab Call Girls Contact Number +919053,900,678 Punjab Call Girls
(๏ 人 ๏) Punjab Call Girls provide you with erotic massage therapy
Punjab Call Girls are well-trained in courtship and seduction. They can offer you true love and companionship. They can also. They can help you forget your problems and frustrations. They are also experts in playing several roles.
( • )( • )ԅ(≖⌣≖ԅ) Call Girls Punjab is also available for special occasions. They can take you to business meetings or business tours. They can also take you to public functions or any special occasion. These ladies are ready to serve their clients with care and respect. They have a wide range of experience and can also offer customized services. College Call Girls Punjab These websites can help you find escorts in your area. You can also find reviews about them and get recommendations. Their expertise allows them to reach the sensational areas of a man's body and release feelings more intensely with touches and adult words.
You can full your all deserts with Punjab Call Girls
Punjab Call Girls you can find the best escort girls to meet your sexual desires. There are many options, from cute college girls to sexy models. However, you should be careful when choosing an escort service because some will not offer quality services.
Independent Call Girls Punjab will offer companionship services in addition to their sexual services. They can also accompany you to dinner or other social events. In addition, some escorts will perform intimate massages to increase your sensual pleasure another option is to hire a hot Russian escort. These girls are not only beautiful but also very talented in sex. In addition to orgasm, they can offer various erotic positions.
These sexy babes are a perfect choice for a sexy night in town. They know all the sexy positions and will make you moan in delight. They can also play with your dick in the deep throat position and lick it like ice cream. There are plenty of Call girls in Punjab who are available for one-night stands. Just make sure that you use a trusted site and read reviews before booking. You can find a wide variety of gorgeous call girls in our city on the internet. These websites offer a safe and convenient way to meet a woman and enjoy her company for a night of fun. These sites typically offer a photo of the girl and her number. You can contact her through the phone or sexing to arrange a rendezvous.
★OUR BEST SERVICES: - FOR BOOKING A-Level (5 star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)
★ Spending time in my rooms
★ BJ (Blowjob Without a Condom)
★ COF (Come On Face)
★ Completion
★ (Oral to completion) bjnonCovered
★ Special Massage
★ O-Level (Oral sex)
★ Blow Job;
★ Oral sex with a noncondom)
★ COB (Come On Body)Punjab Call Girls Contact Number +919053,900,678 Punjab Call Girls

Punjab Call Girls Contact Number +919053,900,678 Punjab Call Girls@Chandigarh #call #Girls 9053900678 @Call #Girls in @Punjab 9053900678
Recently uploaded (20)
Gorgeous Call Girls In Pune {9xx000xx09} ❤️VVIP ANKITA Call Girl in Pune Maha...

Gorgeous Call Girls In Pune {9xx000xx09} ❤️VVIP ANKITA Call Girl in Pune Maha...
Independent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for R...

Independent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for R...
Kottayam Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Kottayam Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Sexy Call Girl Nagercoil Arshi 💚9058824046💚 Nagercoil Escort Service

Sexy Call Girl Nagercoil Arshi 💚9058824046💚 Nagercoil Escort Service
Indore Call Girl Service 📞9235973566📞Just Call Inaaya📲 Call Girls In Indore N...

Indore Call Girl Service 📞9235973566📞Just Call Inaaya📲 Call Girls In Indore N...
Dehradun Call Girls 8854095900 Call Girl in Dehradun Uttrakhand

Dehradun Call Girls 8854095900 Call Girl in Dehradun Uttrakhand
Sexy Call Girl Villupuram Arshi 💚9058824046💚 Villupuram Escort Service

Sexy Call Girl Villupuram Arshi 💚9058824046💚 Villupuram Escort Service
Escorts Service Ahmedabad🌹6367187148 🌹 No Need For Advance Payments

Escorts Service Ahmedabad🌹6367187148 🌹 No Need For Advance Payments
Best Lahore Escorts 😮💨03250114445 || VIP escorts in Lahore

Best Lahore Escorts 😮💨03250114445 || VIP escorts in Lahore
Escorts Lahore || 🔞 03274100048 || Escort service in Lahore

Escorts Lahore || 🔞 03274100048 || Escort service in Lahore
🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludh...

🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludh...
❤️Ludhiana Call Girls ☎️98157-77685☎️ Call Girl service in Ludhiana☎️Ludhiana...

❤️Ludhiana Call Girls ☎️98157-77685☎️ Call Girl service in Ludhiana☎️Ludhiana...
Ludhiana Call Girls Service Just Call 6367187148 Top Class Call Girl Service ...

Ludhiana Call Girls Service Just Call 6367187148 Top Class Call Girl Service ...
💚Chandigarh Call Girls Service 💯Jiya 📲🔝8868886958🔝Call Girls In Chandigarh No...

💚Chandigarh Call Girls Service 💯Jiya 📲🔝8868886958🔝Call Girls In Chandigarh No...
Call Girl in Indore 8827247818 {Low Price}👉 Meghna Indore Call Girls * DXZ...

Call Girl in Indore 8827247818 {Low Price}👉 Meghna Indore Call Girls * DXZ...
(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The S...

(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The S...
Sexy Call Girl Tiruvannamalai Arshi 💚9058824046💚 Tiruvannamalai Escort Service

Sexy Call Girl Tiruvannamalai Arshi 💚9058824046💚 Tiruvannamalai Escort Service
Rishikesh Call Girls Service 6398383382 Real Russian Girls Looking Models

Rishikesh Call Girls Service 6398383382 Real Russian Girls Looking Models
Call Girls In Indore 📞9235973566📞Just Call Inaaya📲 Call Girls Service In Indo...

Call Girls In Indore 📞9235973566📞Just Call Inaaya📲 Call Girls Service In Indo...
Punjab Call Girls Contact Number +919053,900,678 Punjab Call Girls

Punjab Call Girls Contact Number +919053,900,678 Punjab Call Girls
INTUSSUSCEPTION.pptx
- 2. When one portion of the gut invaginates into the immediately adjacent loop, the condition is called intussusception.
- 3. • Usually proximal loop is invaginated into the distal bowel. But rarely the distal loop may invaginate into the proximal loop and this condition is called retrograde intussusception (e.g. jejunogastric intussusception following gastrojejunostomy).
- 4. COMPOUND OR DOUBLE INTUSSUSCEPTION. Sometimes the mass of intussusception may again invaginate into the distal bowel and this condition is called compound or double intussusception.
- 5. MULTIPLE INTUSSUSCEPTIONS. Intussusception is usually single but very occasionally one may find more than one intussusception at different levels. This is called multiple intussusceptions.
- 6. Intussusception is usually acute, but rarely chronic intussusception may persist for months or years. Intussusception may recur and this is called recurrent intussusception.
- 7. AETIOLOGY • Broadly speaking there are two varieties of intussusception — • I. Where there is definite cause of intussusception — Secondary intussusception and • 2. Where there is no definite cause for intussusception — Primary or idiopathic intussusception.
- 8. 1. SECONDARY INTUSSUSCETION • Polyp, papilliferous carcinoma, lymphoma, hamartoma, submucous lipoma, stump of appendix, an inverted Meckel’s diverticulum etc. may cause intussusception. • This type of intussusception, which is caused by some pathology, is known as secondary intussusception. • This type of intussusception may occur at any age. • Secondary intussusception usually occurs in the ileum. • Sometimes intussusception may occur in the early postoperative period due to inco-ordinale peristalsis in the small intestine.
- 9. 2. PRIMARY OR IDIOPATHIC INTUSSUSCEPTION • The majority of the intussusceptions belong to this group. • This type of intussusception usually occurs in children between 6 to 9 months of age.
- 10. PATHOLOGY • An intussusception is composed of three parts • (i) the entering or inner tube, • (ii) the returning or the middle tube and • (iii) the sheath or the outer tube.
- 11. PATHOLOGY • The entering or inner tube and the returning tube are together called intussusceptum. • The ensheathing tube or outer tube is called intussuscipiens. • The starting point ofthe intussusception is called the apex. • It is the junction of the entering and returning tubes. • It is the fixed point of intussusception and intussusception progresses at the cost of the ensheathing tube or the outer tube. • The site where the retuning layer and the ensheathing layer meet is called the neck and this point varies as the intussusception progresses.
- 12. PATHOLOGY Intussusception is a type of intestinal obstruction which often accompanies strangulation
- 13. • As the intussusception progresses, the mesentery of the entering and returning tubes is dragged alongwith the gut through the neck of the intussusception. • Gradually the mass of the intussusception by the pull of the mesentery becomes sausage-shaped with concavity towards the umbilicus (approximately the point of attachment of the mesentery). the mesentery becomes compressed between the entering and returning tubes. • In the beginning the mesentery become constricted and severe venous engorgement and oedema of the wall of the intussusceptum oedematous intussusceptum may cause total intestinal obstruction.
- 14. SAUSAGE-SHAPED WITH CONCAVITY TOWARDS THE UMBILICUS
- 15. PATHOLOGY • If the mesentery is quite long intussusception can even present through the rectum at the anal canal pull on the mesentery becomes sufficient enough to occlude the arteries. • This causes onset of gangrene • Gangrene is dependent upon the tightness of the invagination and it often occurs in ileocolic intussusception ileocaecal valve exerts pressure on the mesentery. • The returning layer near the apex is the first site to gangrene. • Gangrene may cause perforation and ultimately peritonitis. • The ensheathing tube is hardly affected.
- 16. • In rare instances gross adhesion may develop at the neck between intussusceptum and intussuscipiens, develops in such case, the whole mass of intussusceptum becomes necrosed and sloughs out. • This brings cure.
- 17. CLINICAL FEATURES Healthy male children between 6 and 9 months of age are mostly affected.
- 18. CLINICAL FEATURES • Onset is usually sudden. The child screams with abdominal pain, which is colicky in nature. • Alongwith the pain the child draws up his legs. During the attack the child may vomit. • But remember that vomiting is a late feature and usually does not appear before 24 hours of the onset of the disease.
- 19. CLINICAL FEATURES • Such attacks are also accompained by facial pallor. • The attacks usually last for a few minutes and recur every 15 minutes. • In between the attacks the child lies motionless and looks very drawn. • Patient may pass a few normal motions before current jelly stool is passed.
- 20. CLINICAL FEATURES • In long continued and untreated cases pain becomes continuous. After 2 or 3 days, the abdomen gradually starts distending. • Vomiting becomes copious. • Absolute intestinal obstruction occurs and death is the ultimate result from intestinal obstruction alone or peritonitis following gangrene and perforation
- 21. PHYSICAL SIGNS • The abdomen becomes voluntarily contracted during paroxysms of pain. • In early cases distension is not noticed. • Distension only appears after 2 or 3 days of the commencement of the disease. • If the abdomen is carefully palpated between the attacks one may feel a lump under the right or left costal margin.
- 22. PHYSICAL SIGNS • This lump is a sausage-shaped lump with concavity towards the umbilicus. • Right iliac fossa is peculiarly empty on palpation. called Signe-de-Dance. • This is due to the fact that the If terminal part of ileum and caecum do not remain m right iliac fossa, but arc involved in intussusception and arc tclcscopcd through the ascending colon, transverse colon and descending colon according to the various stages.
- 23. PHYSICAL SIGNS • RECTAL EXAMINATION should always be performed One may feel the intussusceptum if it has reached the rectum. • It will feel very much like cervix uteri in the vagina. • In majority of cases the apex of the intussusception cannot be felt per rectum but the finger will be smeared by blood-stained mucus. • This will give a definite clue to the diagnosis.
- 24. PHYSICAL SIGNS • In very occasional cases intussusception may actually protrude through the anus when the patient possesses an unusually long mesentery. • In this case it looks like a prolapse.
- 25. SPECIAL INVESTIGATIONS • X-ray of the abdomen shows absence of caecal gas shadow and increased gas shadows in the small intestine. • Barium Enema Radiography is very diagnostic when the intussusception has passed distally through ileocaecal valve. • When the intussusception has reached at least the ascending colon the barium will stop intussusceptum and there it will show a ‘pincer- shaped ’ or ‘colied-spring ’ deformity or ‘pitch fork.
- 26. • Barium enema has got a therapeutic value, in the sense that the pressure of the barium enema may cause spontaneous reduction of the intussusception.
- 27. ‘pincer-shaped ’ or ‘colied-spring ’ deformity
- 28. TREATMENT PREOPERATIVE MANAGEMENT • Intra- venous fluid administration should be started immediately and appropriate fluid resuscitation should be begun. • Decompression of the small intestine through nasogastric suction is similarly important. • Prophylactic antibiotics should be given if symptoms have been present for more than 24 hours.
- 29. HYDROSTATIC REDUCTION When infants present with less than 24 hours of symptoms. hydrostatic reduction is a successful treatment in 60 to 70% of patients Barium enema can be used for hydrostatic reduction of intussusception. OPERATIVE TREATMENT RESECTION
- 30. THANKYOU