This study analyzed over 21,000 office-based cataract surgeries performed between 2011-2014 to evaluate safety and effectiveness outcomes. Key findings include:
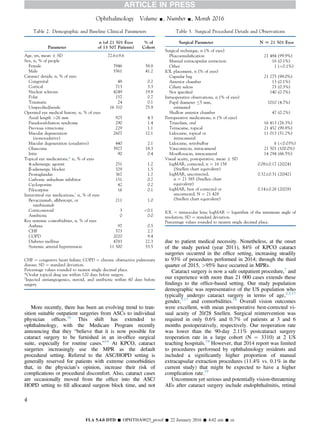
1) Post-operative visual acuity was excellent, with a mean of 20/28.
2) Intraoperative complications like capsule tears and vitreous loss occurred in 0.55% and 0.34% of cases respectively.
3) Postoperative adverse events like iritis and corneal edema each affected around 1-2% of cases. No cases of endophthalmitis were reported.
Second surgeries were required in 0.70% of cases within 6 months. The study found office-based cataract