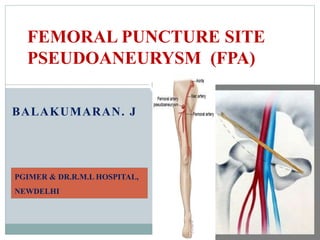
Femoral site psudeoaneurysm
- 1. BALAKUMARAN. J FEMORAL PUNCTURE SITE PSEUDOANEURYSM (FPA) PGIMER & DR.R.M.L HOSPITAL, NEWDELHI
- 2. Introduction A pseudoaneurysm refers to a defect in an arterial wall, which allows communication of arterial blood with the adjacent extra-luminal space. Blood extravasates out of the artery, which is contained by surrounding soft tissue forming the cavity or sac. There is often a narrow tract from the arterial wall to the pseudoaneurysm sac, termed the ‘neck’. A pseudoaneurysm is distinct from a ‘true’ aneurysm, which results from dilation of all layers of the arterial wall.
- 3. INTRODUCTION Groin complications related to the femoral arterial access site used for various invasive cardiovascular procedures represent a significant problem. Among these, femoral artery pseudoaneurysm (FPA) is one of the most troublesome. The FPA occurs in 0.1% to 0.2% of diagnostic angiograms and 3.5% to 5.5% after interventional procedures. The incidence of the FPA has increased recently with the more frequent use of high doses of antiplatelet and anticoagulant therapy and the use of larger-sized cannulas for various interventional procedures.
- 4. Femoral pseudoaneurysm is the second most common complication after bleeding. The most common site of pseudoaneurysm occurrence is the common femoral artery. The incidence is 10 times greater after angioplasty than after diagnostic procedures owing to the circumference of the catheters use. Angiology Volume 56, Number 5, 2005
- 5. Factors Associated With the Formation of FPA Antiplatelet agents (often aspirin and clopidogrel) and Anticoagulation Large sheath size, 8F Age 65 years, Female. Obesity Poor postprocedural compression Simultaneous artery and vein catheterization Hypertension, diabetes mellitus. Peripheral arterial disease Complex interventions Multiple punctures Low or high puncture sites, inadvertent catheterisation of the superficial femoral artery or profunda femoris artery. Increased number of cases performed in a day in same room. (avg. 17 cases in single room per day)
- 7. COMPLICATIONS 1. RUPUTURE The most catastrophic complication of FPA is rupture. Although the exact rate is unknown, the risk of spontaneous rupture is related to -size > 3 cm. -presence of symptoms. -large hematoma. -continued growth of the sac. 2. INFECTION Although most postcatheterization FPAs are sterile, infection of it significantly increases the risk of rupture as well as septic emboli. 3. Pseudoaneurysms which persist may enlarge and lead to complications related to compression of the adjacent femoral vein, nerve, and overlying skin. This can lead to leg swelling, deep vein thrombosis, compressive neuropathy and skin necrosis. Circulation. 2007;115:2666-2674
- 8. How to diagnose FPA ? H/o of catheterization Gradually expanding pulsatile mass Painful, tender. Extensive skin discoloration or ecchymosis Thrill or bruit.
- 9. Prediction of FPA after Percutaneous Procedures The presence of a palpable groin mass is predictive. A platelet count of less than 200 x 109/L is strongly associated. Radiology: Volume 240: Aug-2006 100 %
- 10. DIAGNOSIS Color Doppler flow mapping has been the mainstay in diagnosing FPA. Criteria used to diagnose a pseudoaneurysm include: Swirling color flow seen in a mass separate from the affected artery. Color flow within a tract leading from the artery to the mass consistent with pseudoaneurysm neck. Typical “to and fro” Doppler waveform in the pseudoaneurysm neck. Clin Med Res. 2003 July; 1(3): 243–247
- 11. Doppler USG The sensitivity of doppler ultrasound to identify a FPA is 94% with a specificity of 97%. Number, size, and depth of the chambers of the FPA, the depth, width, and length of the tract that connects the artery to the FPA should be identified. Feeding artery should be made clear.
- 12. TREATMENT A proportion of femoral pseudoaneurysms will resolve spontaneously without any form of intervention. An accepted approach is to monitor small (less than 3cm), stable, asymptomatic pseudoaneurysms, as the majority of them will thrombose within 4 weeks. In one large series of small (<3cm) pseudoaneurysms, reported a rate of spontaneous thrombosis of ~90% at 60 days . Spontaneous thrombosis of the pseudoaneurysm may be less likely in patients who are fully anticoagulated.
- 13. TREATMENT OPTIONS 1. ULTRASOUND GUIDED COMPRESSION REPAIR 2. THROMBIN INJECTION 3. FIBRIN INJECTION 4. COLLAGEN 5. ENDOVASCULAR TECHNIQUES 6. OPEN SURGICAL REPAIR.
- 14. 1. ULTRASOUND GUIDED COMPRESSION REPAIR The treatment is ultrasound probe compression of the neck of the pseudoaneurysm. The "neck" of the pseudoaneurysm is the narrow path of blood flow between the artery, through the arterial wall, and into the pseudoaneurysm cavity. The artery, neck, and pseudoaneurysm are seen on ultrasound. Ultrasonographic guided compression repair is a safe, cost-effective first approach to treatment for many femoral artery pseudoaneurysms and does not affect possible surgical intervention if the ultrasonographic guided compression repair attempt fails. .
- 15. CONTRAINDICATIONS FOR UGCR Inaccessible site. Limb ischemia. Infection. Large hematomas with overlying skin ischemia. Compartment syndrome
- 16. UGCR- PROCEDURE Iv line in place Oral diazepam or analgesics. Discontinue heparin 2hrs before and 4 hrs after compression. Baseline ankle brachial index and look of peripheral pulses also as to confirm after the procedure. The pseudoaneurysm and the underlying artery were localized, the communicating tract was centered on the color-flow image. Direct vertical pressure was manually applied with the ultrasound probe just sufficient to impede arterial flow into the pseudoaneurysm. Journal of Vascular Surgery, 425-433, October 1995
- 17. UGCR - PROCEDURE Start compressing the neck with transducer and after 30 minutes, pressure was temporarily released every 20 minutes to check whether the lesion was cured; release for every 1 min for distal perfusion. Sometimes if necessity for femoral artery compression decrease the compression interval to 10 min, UGCR was stopped as soon as this was the case. Approximately every 15 minutes, a change of operators was undertaken, without releasing the pressure or altering the position of the transducer. The procedure was also terminated when success could not be obtained within 120 minutes. Flow was then reassessed, and, if the pseudoaneurysm was still present, repeat compression was undertaken, with the same time increments, until successful pseudoaneurysm thrombosis was achieved. Circulation. 1994;90:1861-1865
- 18. The artery and vein were also restudied after compression to exclude subsequent thrombosis. All successfully treated patients were confined to bed for 24 to 48 hours with a compression dressing over the affected site. The arteries were reexamined with doppler at 24 hours after the initial UGCC to assure closure. If clinically warranted, additional scans were ordered.
- 19. PRINCIPLE OF COMPRESSION REPAIR Transducer- start –compress-30min-then visusalise every 20 min intervals-release for 1 min-again compress-max. compress for 120 minutes. Repeat after 24 hrs Success-bed rest for 24 hrs If not-other methods.
- 20. Factors Affecting Success by UGCR Ability to compress Anticoagulation status Pseudoaneurysm size Age of the pseudoaneurysm (epithelialization of the tract and more fibrous capsule) Neck width, length of communicating tract.
- 21. UGCR Less successful if the patient is obese and if the neck of the pseudoaneurysm is wider. Finally, it is also much less successful if the patient is taking aspirin, warfarin or another anticoagulant, since these would prevent clotting of blood within the pseudoaneurysm. Advantages are that this is the least invasive method of stopping arterial blood flow into a pseudoaneurysm.
- 22. UGCR Ultrasound-guided compression is now increasingly used as a therapeutic tool, to avoid the need for surgery. Patients will require effective analgesia or sedation, or both, in order to tolerate the procedure. Success rates of 63% to 88% have been reported. Care must be taken to avoid compromising flow within the underlying femoral artery.
- 23. 2. Ultrasound guided thrombin injection Another minimally-invasive technique used today is ultrasound-guided thrombin injection. Thrombin (factor IIa in the coagulation cascade) is a clotting factor that converts fibrinogen into fibrin, which then polymerizes to form a blood clot. Under ultrasound guidance, thrombin can be injected directly into a pseudoaneurysm, causing it to clot. Advantages are that the technique is relatively easy to perform, is successful, and is minimally invasive. One contraindication to this procedure is if there is an arteriovenous fistula (communication between an artery and vein), in addition to the pseudoaneurysm. This occurs with about 10% of pseudoaneurysms. If this is present, thrombin injected into the pseudoaneurysm could then enter the venous circulation and possibly lead to distant thrombosis
- 24. Thrombin injection An average dose of 1100 U of thrombin was used. Time to coagulation ranged from 10 to 60 seconds. A new study shows the average dose of 192 U thrombin will act on FPA.. Bovine Thrombin comes in strengths of 5000 or 20,000 units, in a powder form with 0.9% sodium chloride as diluent. It is reconstituted at a concentration of 1000 U/mL and then diluted to a concentration of 100 U/mL with sterile saline. With sonographic guidance, a 22 gauge needle is introduced into the pseudoaneurysm.
- 25. Dose of thrombin The needle tip is visualized and positioned at a site distant from the neck of the pseudoaneurysm. Increments of 0.5-1.0 mL (50-100 U) of thrombin were slowly injected at a rate of approximately 1 mL/10 sec. A period of 5-10 sec is allowed to elapse before additional thrombin is injected. Results are monitored continuously with color-flow Doppler sonography. Injection is stopped when no further flow is identified in the pseudoaneurysm. When possible, the neck of the pseudoaneurysm must be occluded manually or with the sonographic probe during the injection procedure.
- 26. Adv. and disadv. of thrombin The success rate of thrombin injection reported in the literature has been consistently high, at an average of 97%, even with patients treated with therapeutic levels of anticoagulants. Treatment can usually be completed within several minutes. Topical bovine thrombin has been used extensively for hemostasis for more than 20 years. Recent descriptions of antibody responses show high titers against endogenous coagulation factors, with resulting bleeding complications. Prior exposure to bovine thrombin is considered a contraindication to treatment of pseudoaneurysms with thrombin.
- 27. Disadv. of thrombin injection The first attempts to close a FPA with ultrasound-guided thrombin injections were not without complications. Distal migration of the thrombin have been described may be these complications due to the nature of the injected thrombin . Because thrombin is used in liquid form, it can easily diffuse from the cavity through the neck of the FPA toward the lumen of the artery. It is also possible that if the thrombin is injected in a too diluted concentration, it does not remain in the cavity of the FPA long enough to form a clot. Furthermore, it has been described that patients receiving thrombin are at risk for hypersensitivty reaction.
- 28. 3. Percutaneous injection of fibrin This technique involves percutaneous injection of the adhesive components using ultrasound and screening control following successful occlusion of the aneurysm neck by angioplasty balloon. The fibrin adhesive mimics the final stage of coagulation cascade. Thrombin is used to convert fibrinogen to fibrin, and the fibrin is then crosslinked in the presence of calcium to create a mechanically stable network filling the aneurysm. The technique has several advantages-the balloon virtually eliminates the chance of distal embolization. The tissue adhesive does not rely on the patient's own clotting factors. Therefore it is more likely to work in anticoagulated patients . Br J Radiol. 1998;71:1255–1259
- 29. 4. FEMORAL COLLAGEN INJECTION. When collagen comes in contact with blood, platelets aggregate on the collagen and release coagulation factors that, together with plasma factors, result in the formation of a fibrin matrix. Initially, the collagen was applied guided by selective angiography using the contralateral access site with a 4F sheath. After puncture of the contralateral femoral artery, the 4F catheter is introduced through the sheath and positioned across the iliac bifurcation in the affected proximal common femoral artery over a guide wire. The injection of the contrast medium allows one to locate the FPA exactly and correctly, together with its tract and connections.
- 30. Procedure of collagen injection After applying routine local anesthesia with 1% lignocaine, the pseudoaneurysm cavity is then directly punctured, leading to high-pressure backflow of blood ensuring correct access to the pseudoaneurysm. The initial application of the collagen plugs required a larger 11F sheath. After puncture of the pseudoaneurysm, a guidewire was introduced through the needle to the pseudoaneurysm. The needle is then removed, leaving the guidewire in place. A sheath-dilatator is passed over the guidewire into the pseudoaneurysm cavity, and the guidewire and the dilatator are removed, leaving only the sheath through which collagen plug could be inserted. The application of the collagen paste allows use of a thinner needle. The pseudoaneurysm cavity is directly punctured percutaneously using a 9F needle. Then the collagen paste is applied directly through this 9F needle into the center of the FPA. This produces a very rapid filling and thrombosis of the pseudoaneurysm. After 1 to 2 min, a repeat angiogram is performed through the 4F sheath of the opposite access, to confirm aneurysm occlusion .
- 31. Procedure
- 32. Success of collagen injection This results in a final success rate of 98.2%. Injection of collagen is easily accepted by the patients, and during the procedure there was no need for systemic analgesic medication . Not bothered whether or not the patient is receiving anticoagulant therapy as it would not appear to impair the results.
- 33. Inj. of collagen Complete obliteration was usually achieved within some 10 s, which is comparable to thrombin closure. The advantages of collagen lie in its physical-chemical properties. The fact that it consists of long paste fibers allows the collagen to remain within the FPA cavity, which putatively reduces the risk of migration through the neck of the FPA.
- 34. 5. Open surgical repair INDICATIONS Rapid expansion of the FPA. There may not be time to wait for noninvasive treatments. Concomitant distal ischemia or neurological deficit due to local pressure from the FPA, or distal embolization. Mycotic infection of FPA. Failure of percutaneous intervention. Compromised soft tissue viability.
- 35. Open surgical repair (OSR) ‘Gold standard’ treatment for iatrogenic femoral pseudoaneurysms, as the arterial defect is repaired definitively. Principle steps of OSR involve obtaining proximal and distal control of the affected artery, evacuating the aneurysm sac and repairing the defect in the arterial wall (either by primary or patch closure). Complications of OSR include blood loss and infection. Other major adverse events such as myocardial infarction or death are recognised. Recovery time and inpatient stay may be prolonged following OSR.
- 36. 6. Other Options Placement of covered stents. Percutaneous coil placement to occlude the FPA. In some cases the coil was placed in the neck, while in other patients the coil was placed inside the pseudoaneurysm in order to achieve closure and local thrombosis.
- 37. CONCLUSION In conclusion, as vascular interventional procedures are on a rise, there are more possibilities for occurrence of Iatrogenic Pseudoaneurysms. Initially Ultrasound Guided Compression Repair was the preferred treatment as it was non invasive. But due to its failure in 25% of patients on studies conducted, increased pain experienced by the patient, long procedure time and recent development of other minimally invasive treatments which are more effective, UGCR is less preferred nowadays. Percutaneous injection of thrombin, fibrin, collagen can be completed in several minutes, has the advantage of avoiding surgical intervention or the pain associated with ultrasound- guided compression, and can be performed effectively in patients who have received anticoagulation.
- 38. PREVENTION Vascular complications are less common when the fluoroscopy is used for localization of the femoral head to puncture the femoral artery in the correct location and with the first attempt. Always need effective compression after sheath removal. Monitor before the patient is discharged. If in doubt kindly review with doppler and needs follow up. Attention to puncture under fluoroscopic guidance is strongly recommended.
- 39. THANK YOU