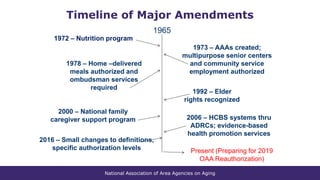
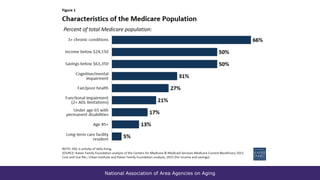
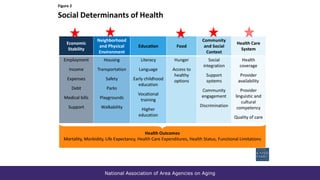
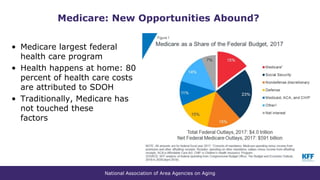
The document summarizes a presentation given at the 2018 NADO Annual Training Conference on current issues in aging. The presentation covered topics like the aging network and federal funding, the Older Americans Act reauthorization process, building connections to health care through programs like Medicare and Medicaid, and advocacy strategies. It provided data on trends in aging services and the needs of older adults, discussed the 2019 federal budget deal's impact on aging programs, and looked ahead to potential policy discussions in the coming years.























![National Association of Area Agencies on Aging
Older Americans Act BIG INCREASES!
• + $35 million for Title III B Supportive Services
• + $40 million for III C 1 Congregate Nutrition
• + $19 million for III C 2 Home-Delivered Meals
• + $5 million for III D Preventative Health
• + $30 million for III E National Family Caregiver Support
Program
• + $4 million for Title VI Native American
• +$1 million for Title VII Ombudsman
[HUD Section 202 +$105 million, Service Coords +$90 mil]
What Happened in FY 2018? (March)](https://image.slidesharecdn.com/currentissuesinaging-181026030354/85/Current-Issues-in-Aging-Campell-38-320.jpg)