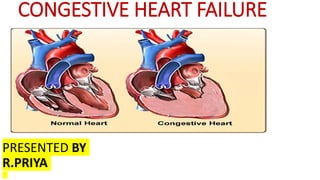
Congestive Heart Failure: Causes, Symptoms & Treatment
- 1. CONGESTIVE HEART FAILURE PRESENTED BY R.PRIYA
- 2. INTRODUCTION The burden of Heart Failure in India appears high, and estimates of prevalence range from 1.3 million to 4.6 million, with an annual incidence of 491 600–1.8 million. Heart failure is a common, costly, and potentially fatal condition, and it is the leading cause of both hospitalization and readmission amongst older adults. In 2015, it affected about 40 million people globally.Overall around 2% of adults have heart failure and in those over the age of 65, this increases to 6–10%. Rates are predicted to increase. The risk of death is about 35% the first year after diagnosis, while by the second year the risk of death is less than 10% for those who remain alive. This degree of risk of death is similar to some cancers.In the United Kingdom, the disease is the reason for 5% of emergency hospital admissions. Heart failure has been known since ancient times, with the Ebers papyruscommenting on it around 1550 BCE.
- 3. DEFINITION OF CCF • Heart failure (HF), also known as congestive heart failure (CHF), (congestive) cardiac failure (CCF), and decompensation cordis, is when the heart is unable to pump sufficiently to maintain blood flow to meet the body tissues needs for metabolism.
- 4. TYPES OF CCF •Left-sided heart failure. Left-sided heart failure is the most common type of heart failure. ... •Right-sided heart failure. The right heart ventricle is responsible for pumping blood to lungs to collect oxygen. ... •Both sided heart failure/Biventricular heart failure • CLASSIFIED BY PUMPING ABILITY OF THE HEART •Diastolic heart failure. ... •Systolic heart failure. • CLASSIFIED BY COURSE OF DISEASE • Acute heart failure • Chronic heart failure
- 5. LEFT SIDE HEART FAILURE Left-sided heart failure: The left ventricle of the heart no longer pumps enough blood around the body. As a result, blood builds up in the pulmonary veins (the blood vessels that carry blood away from the lungs). This causes shortness of breath, trouble breathing or coughing – especially during physical activity. Left-sided heart failure is the most common type. Left-sided heart failure is usually caused by coronary artery disease (CAD), a heart attack or long-term high blood pressure.
- 6. RIGHT SIDE HEART FAILURE Right-sided heart failure: Here the right ventricle of the heart is too weak to pump enough blood to the lungs. This causes blood to build up in the veins (the blood vessels that carry blood from the organs and tissue back to the heart). The increased pressure inside the veins can push fluid out of the veins into surrounding tissue. This leads to a build-up of fluid in the legs, or less commonly in the genital area, organs or the abdomen (belly). Right-sided heart failure generally develops as a result of advanced left-sided heart failure, and is then treated in the same way. It is sometimes caused by high blood pressure in the lungs, an embolism in the lungs (pulmonary embolism), or certain lung diseases such as COPD.
- 7. BOTH SIDED HEART FAILURE Biventricular heart failure: In biventricular heart failure, both sides of the heart are affected. This can cause the same symptoms as both left-sided and right-sided heart failure, such as shortness of breath and a build-up of fluid.
- 8. CLASSIFIED BY PUMPING ABILITY SYSTOLIC HEART FAILURE AND DIASTOLIC HEART FAILURE Heart failure with reduced pumping ability: The heart muscle has become weaker, and no longer pumps enough blood around the body when it contracts (squeezes). As a result, the organs in the body don’t get enough oxygen. The medical term for this is “heart failure with reduced ejection fraction.” (SYSTOLIC HEART FAILURE) Heart failure with preserved pumping ability: Although the heart muscle is still strong, it can no longer relax and widen enough after it has squeezed blood out, so it doesn’t fill up with blood properly. Despite pumping strongly enough, not enough blood is pumped out into the body as a result, especially during physically strenuous activities. Doctors call this “heart failure with preserved ejection fraction.”(DIASTOLIC HEART FAILURE)
- 9. CLASSIFIED BY COURSE OF DISEASE ACUTE HEART FAILURE Heart failure can develop suddenly, for instance after a heart attack or due to certain heart rhythm problems. This is known as acute heart failure. CHRONIC HEART FAILURE But it usually develops gradually over time as a result of a different medical problem, such as permanently high blood pressure. This is known as chronic heart failure.
- 10. CAUSES AND RISK FACTOR •High blood pressure. heart works harder than it has to if blood pressure is high. •Coronary artery disease. ... •Heart attack. ... •Diabetes. ... •Some diabetes medications. ... •Certain medications. ... •Sleep apnea. ... •Congenital heart defects.
- 11. •Age. Growing older increases risk of damaged and narrowed arteries and a weakened or thickened heart muscle. •Sex. Men are generally at greater risk of heart disease. ... •Family history. ... •Smoking. ... •Poor diet. ... •High blood pressure. ... •High blood cholesterol levels. ... •Diabetes. CAUSES AND RISK FACTOR
- 15. SIGNS AND SYMTOMS LEFT SIDED HEART FAILURE SIGNS AND SYMPTOMS •Awakening at night with shortness of breath •Shortness of breath during exercise or when lying flat •Chronic coughing or wheezing •Difficulty concentrating •Fatigue •Fluid retention causing swelling, or edema, in the ankles, legs and/or feet •Lack of appetite and nausea •Rapid or irregular heartbeat •Sudden weight gain As these symptoms occur, they cause the heart to try to pump harder, which causes further damage such as: •Enlarged heart •Rapid heart rate •High blood pressure •Less blood flowing to the arms and legs
- 16. SIGNS AND SYMPTOMS • RIGHT SIDE HEART FAILURE SYMPTOMS • feet, legs, and ankles will likely to swell because blood is backing up in veins.This symptom is called edema. •If it backs up into stomach or liver, may notice that abdomen is distended, too. • might find that have to go to the bathroom more, especially at night.This is caused by fluid buildup, too. As heart failure gets worse, may also see some of these symptoms: •It’s hard to breathe. •neck veins are swollen. •pulse is fast or feels “off.” •chest hurts. •gaining weight from excess fluid. •don’t feel like eating. •skin is cold and sweaty. •very tired. •confused and forget things. •Other types of heart failure have same symptoms
- 17. DIAGNOSTIC EVALUTION OF HEART FAILURE • Blood tests. doctor may take a blood sample to look for signs of diseases that can affect the heart. He or she may also check for a chemical called N-terminal pro-B-type natriuretic peptide (NT-proBNP) if diagnosis isn't certain after other tests. • Chest X-ray. X-ray images help doctor see the condition of lungs and heart. doctor can also use an X-ray to diagnose conditions other than heart failure that may explain signs and symptoms. • Electrocardiogram (ECG). This test records the electrical activity of heart through electrodes attached to skin. It helps doctor diagnose heart rhythm problems and damage to heart. • Echocardiogram. An echocardiogram uses sound waves to produce a video image of heart. This test can help doctors see the size and shape of heart along with any abnormalities. An echocardiogram measures ejection fraction, an important measurement of how well heart is pumping, and which is used to help classify heart failure and guide treatment. • Stress test. Stress tests measure the health of heart by how it responds to exertion. may be asked to walk on a treadmill while attached to an ECG machine, or may receive a drug intravenously that stimulates heart similar to exercise. • Sometimes the stress test can be done while wearing a mask that measures the ability of heart and lungs to take in oxygen and breathe out carbon dioxide. If doctor also wants to see images of heart while 're exercising, he or she may use imaging techniques to visualize heart during the test. • Cardiac computerized tomography (CT) scan. In a cardiac CT scan, lie on a table inside a doughnut-shaped machine. An X- ray tube inside the machine rotates around body and collects images of heart and chest. • Magnetic resonance imaging (MRI). In a cardiac MRI, lie on a table inside a long tubelike machine that produces a magnetic field, which aligns atomic particles in some of cells. Radio waves are broadcast toward these aligned particles, producing signals that create images of heart. • Coronary angiogram. In this test, a thin, flexible tube (catheter) is inserted into a blood vessel at groin or in arm and guided through the aorta into coronary arteries. A dye injected through the catheter makes the arteries supplying heart visible on an X- ray, helping doctors spot blockages. • Myocardial biopsy. In this test, doctor inserts a small, flexible biopsy cord into a vein in neck or groin, and small pieces of the heart muscle are taken. This test may be performed to diagnose certain types of heart muscle diseases that cause heart failure.
- 18. DIAGNOSTIC EVALUTION Cardiac catheterization • How the procedure is done: • A very small tube (catheter) is inserted into a blood vessel in upper thigh or arm. • The tip of the tube is positioned either in the heart, or where the arteries supplying the heart originate. • A special fluid (called a contrast medium or dye) is injected. This fluid is visible by X- ray. • The pictures that are obtained are called angiograms. • This procedure may involve some discomfort from placement of the catheter. may be required to rest in a certain position after the procedure. • What cardiac catheterization shows: • Blockages in the coronary arteries are visible on the X-rays. • The parts of heart that are fed by the blocked or narrowed arteries may be weakened or damaged from lack of blood.
- 19. TREATMENT FOR HEART FAILURE • Vasodilators expand blood vessels, ease blood flow, and reduce blood pressure. • Diuretics correct fluid retention. • Aldosterone inhibitors help with fluid retention and improve chances of living longer. • ACE inhibitors or ARB drugs improve heart function and life expectancy. • Digitalis glycosides strengthen the heart’s contractions. • Anticoagulants or antiplatelets such as aspirin help prevent blood clots. • Beta-blockers improve heart function and chances of living longer. • Tranquilizers reduce anxiety.
- 20. TREATMENT CON Beta blockers (Carvedilol,metoprolol,bisoprilol) These medicines lower heart rate and blood pressure, and protect heart from certain substances that can damage heart. Beta blockers are often started at a very low dose and then are increased until a dose is reached that works best. Common side effects of beta blockers: •Dizziness •Feeling tired •Worsening of usual symptoms (this might improve over time without changing medicines) Stopping beta blockers suddenly can cause symptoms to get worse. Don't stop taking medicine without talking to doctor or nurse. Call doctor if feel faint, pass out, have increased shortness of breath or wheezing, or have other symptoms that bother . ACE inhibitors(lisinopril,captopril) Angiotensin converting enzyme (ACE) inhibitors reduce the amount of heart-damaging hormones body produces. They also dilate blood vessels and lower blood pressure to lessen the workload of heart. Common side effects of ACE inhibitors: •Dizziness •Changes in kidney function •Dry cough that often improves with time •Increased potassium levels will have regular blood tests to check kidney function and potassium levels while taking this medicine. Get medical help right away if have swelling of mouth, lips, or tongue. This could be an allergic reaction that
- 21. TREATMENT CON Angiotensin receptor blockers (losartan) • Angiotensin receptor blockers are similar to ACE inhibitors, but they don't cause the cough that some people have when taking ACE inhibitors. • Common side effects of angiotensin receptor blockers: • Dizziness • Changes in kidney function • Increased potassium levels • will have regular blood tests to check kidney function and potassium levels while taking this medicine. • Get medical help right away if have swelling of mouth, lips, or tongue. This could be an allergic reaction that can be life- threatening. Combination medicines (Entresto, or sacubitril/valsartan) • Entresto is a medicine that combines the angiotensin receptor blocker (ARB) valsartan with a substance known as sacubitril that causes the heart to squeeze harder and can help body eliminate excess fluid. The effect of this combination can be more powerful than either drug alone. Entresto is usually started after a person has been able to tolerate target doses of either an angiotension converting enzyme inhibitor (ACEI) or an angiotensin receptor blocker (ARB), so this is not usually the first medicine used to treat heart failure. It is currently only used if other medicines have not improved the heart’s ability to pump effectively. If are taking an ACEI (such as lisinopril or enalapril) will need to stop that medication for 36 hours before starting Entresto. This is very important; not doing so could result in a serious reaction. • Common side effects: • Dizziness • Changes in kidney function • Increased potassium levels • Get medical help right away if have swelling of mouth, lips, or tongue. This could be an allergic reaction that can be life- threatening. • Call doctor if have rapid weight loss soon after starting Entresto
- 22. TREATMENT CON Aldosterone antagonist( spironolactone,eplerenone) These medicines prevent body from producing too much of the hormone aldosterone that can damage heart. Common side effects of aldosterone antagonists: •Changes in kidney function •Increased potassium levels •Swelling or tenderness in the breasts (in both men and women) will have regular blood tests to check kidney function and potassium levels while taking this medicine. Digoxin (Lanoxin) This medicine slows heart rate and might improve the pumping ability of heart. 'll get a blood test to make sure the dose 're taking is right for . Common side effects of digoxin: •Nausea •Poor appetite •Digestive problems Call doctor if are nauseated, or notice a yellow tinge or "halos" in vision. Hydralazine and nitrates (Apesoline, Nitrobid, I mdur,Isordil) Hydralazine and nitrates are often used together to treat heart failure. They dilate blood vessels so it's easier for heart to receive and pump blood. Common side effects of hydralazine and nitrates: •Dizziness •Headache
- 23. TREATMENT CON Diuretics: furosemide (Lasix), bumetanide (Bumex), torsemide (Demadex), metolazone (Zaroxolyn) These medicines are called water pills because they remove excess fluid from the body to help breathe easier and feel better. If take a diuretic once a day, take it in the morning. If take it twice a day, try to take the second dose no later than 4 p.m. to lessen the urge of going to the bathroom during the night. If take metolazone plus another diuretic, take metolazone first, about 30 minutes before the other diuretic. Diuretics (especially metolazone) can cause to lose potassium, so doctor might prescribe a potassium supplement. Not everyone taking diuretic medicine needs extra potassium, so ask doctor if have any questions. If diuretic dose is changed, will need lab tests to monitor kidney function. Common side effects of diuretics: •Increased urination •Dizziness •Dehydration •Changes in kidney function •Ringing or buzzing in the ears •Skin rash or hives •Itching •Increased blood sugar levels
- 24. SURGICAL MANAGEMENT OF CCF Coronary Artery Bypass Graft (CABG) Surgery Coronary artery bypass graft (CABG) surgery involves the use of a blood vessel graft to bypass one or more blocked coronary arteries. The bypass restores normal blood flow to the heart muscle. The graft goes around the clogged artery/arteries and forms new pathways for oxygen- rich blood to flow to the heart muscle. The blood vessel grafts usually come from own arteries and veins in the chest, leg or arm. The bypass grafts are put in place by sewing one section of the artery or vein around a tiny opening just below the blockage in the diseased coronary artery and attaching the other end to a tiny opening made in the aorta. This redirects the blood flow around the blockage. If an internal thoracic (mammary) artery is used, one end is connected to the coronary artery while the other stays attached to the aorta. During the surgery, surgeon will place temporary pacing wires and a chest tube before sternum is closed with special wires. chest incision will be closed with internal stitches or traditional external stitches. The chest tube is needed to drain fluid. The pacing wires are placed in case have an abnormal heart rhythm after surgery. This is common, and if it happens, the wires are attached to a temporary pacemaker until heart rhythm returns to normal. The surgery generally lasts 3 to 5 hours, depending on the number of arteries that are being bypassed.
- 25. SURGICAL MANAGEMENT OF CCF Valve Surgery As heart failure gets worse, changes in the left ventricle (lower chamber of the heart) papillary muscles to stretch out of shape. The papillary muscles support mitral valve to keep blood flowing in only one direction. When the papillary muscles get weak, support the mitral valve leaflets, and the valve starts to leak .Mitral valve reshaping the leaflets and supporting the mitral valve with a ring. Mitral valve repair surgery helps to •Preserve the natural anatomy of the heart •Improve the heart’s ability to pump properly •Decrease heart failure symptoms •Improve survival Heart failure can be caused by aortic valve stenosis (stiffness) or regurgitation (leaky valve cannot open fully, or if blood leaks backward into the left ventricle, the heart strongly to meet the body’s needs for oxygen-rich blood and heart failure can occur.
- 26. SURGICAL MANAGEMENT OF CCF Implantable left ventricular assist device (LVAD) A left ventricular assist device (VAD -- also called ventricular assist system of mechanical circulatory support device (MCSD). It is a mechanical pump in patients who have heart failure to help the heart’s weakened left ventricle pumping chamber of the heart) pump blood throughout the body. The VAD devices can be used as “bridge to transplant” or destination Clinic is one of the few institutions worldwide that has access to all clinically mechanical ventricular assist systems, including the Heartmate II®, HVAD, devices, allowing us to choose the device that will best suit an individual needs. Cleveland Clinic also participates in clinical trails so we are able to technology developed for our patients The pump unit is placed in the chest. by the surgeon into the apex of the heart where it receives blood. A tube blood from the device to the aorta (the large artery that takes blood from the rest of the body. It works by pumping blood by continuous flow from the left aorta..
- 27. SURGICAL MANAGEMENT OF CCF Heart transplant The surgery Once are in the operating suite, the actual heart transplant procedure can take anywhere from longer. Each person's case is different. The donor heart A surgeon from the heart transplant center goes to harvest the donor heart. The surgeon will donor heart is in good condition before beginning surgery. The donor heart is removed by pulmonary artery in the mid-section. The atria are removed from the veins leading into the The transplant When the donor heart arrives in the operating room, surgeon will remove most of heart and will be placed in proper position and attached to major blood vessels. Recovery How quick a patient recovers after heart transplant depends on many factors: age, general to the transplant. Most patients are up and about within a few days after surgery and home in days.
- 28. SURGICAL MANAGEMENT OF CCF Aneurysm Repair Surgery How do prepare for the procedure? Before the procedure, pre-procedure tests may be performed to ensure that it is safe to perform the surgery. may need to discontinue certain medications before the procedure. health care team will provide specific instructions to help prepare for the procedure. What happens during the procedure? The surgeon will perform the repair under general anesthesia. After have been given the general anesthesia, the surgeon will make a long incision in the skin to open the chest or abdomen (depending upon the area in which the aneurysm occurs). The normal segments of the aorta above and below the bulging section is clamped and the aneurysmal segment is opened. Tubes constructed of artificial material, such as polyester, are positioned inside the artery in the region of the aneurysm and fastened in place with sutures or stitches to essentially become a new aorta. This procedure replaces and repairs the area of the diseased aorta. How long does the procedure last? The procedure itself generally takes three to four hours, but the preparation and recovery time add several hours. The surgery may require a minimum hospital stay of five to 10 days. Some patients may require a stay at a rehabilitation facility to regain their independence. Full recovery may take from four to six weeks. What happens after the procedure? surgeon will give specific instructions need to follow after the surgery until incision heals adequately. Restrictions may include: •No driving until approved by physician (usually within one to two weeks after the procedure, when are no longer taking pain medication) •No baths until the incisions heal; showers and sponge baths around the incision are permitted •Avoid lifting more than 10 pounds for approximately four to six weeks after the procedure
- 29. PREVENTION OF CCF Stop smoking • Smoking is the most preventable risk factor for cardiovascular disease and stroke. Smokers (including cigarette, pipe, and cigar smokers) have more than twice the risk of a heart attack than nonsmokers. Smoking is also the biggest risk factor for sudden cardiac death. Even one to two cigarettes a day greatly increases the risk of heart attack, stroke, and other cardio-vascular conditions. Nonsmokers who are exposed to constant smoke also have an increased risk. • Goal: • Eliminate the use of all tobacco products. Stay away from others’ smoke. Lower high blood pressure Blood pressure is a measurement of the pressure or force inside the arteries with each heartbeat. High blood pressure increases the workload of the heart and kidneys, increasing the risk of heart attack, heart failure, stroke, and kidney disease. High blood pressure is the biggest risk factor for stroke. •Goals • Ideal blood pressure is less than 120/80. For patients with diabetes and established cardiovascular disease, blood pressure should be less than 130/85. • Control blood pressure through diet (low-salt diet), exercise, weight management, and if needed, medications. • Also limit alcohol, as it can increase blood pressure.
- 30. PREVENTION OF CCF Lower total cholesterol, LDL (bad) cholesterol, and triglyceride levels Excessive lipids (fatty substances including cholesterol and triglycerides), especially in the cholesterol, cause the build-up of fatty deposits within arteries, reducing or blocking the flow oxygen to heart. There’s a sharp increase in the risk for cardiovascular disease when total 240 mg/dl and above. •Goals: • Total cholesterol less than 200 mg/dl. • LDL cholesterol should be less than 70 mg/dl for those with heart or blood vessel disease. • LDL should be less than 100 mg/dl for those who have a high risk of cardiovascular disease, such as diabetes or those who have multiple heart disease risk factors. • For all others, LDL cholesterol should be less than 130 mg/dl. • Triglycerides less than 150 mg/dl. For most patients, it is recommended to have cholesterol level checked as early as age 20. profile includes an evaluation of fasting total cholesterol, HDL, LDL, and triglyceride levels. can tell how often to have cholesterol tested. Raise HDL (good) cholesterol HDL cholesterol takes the LDL (bad) cholesterol away from the arteries and back to the liver passed out of the body. High levels of HDL seem to protect against cardiovascular disease. Low HDL: less than 40 mg/dl •Goal: • Greater than 55 mg/dl for women, greater than 45 mg/dl for men; the higher the HDL level, the better.
- 31. PREVENTION OF CCF Control diabetes • Diabetes occurs when the body is unable to produce insulin or use the insulin it has. This sugar levels. People with diabetes (especially women) have a higher risk of cardiovascular diabetes increases other risk factors, such as high cholesterol, LDL, and triglycerides; lower pressure. Keeping diabetes under control is essential in reducing risk. • Goal: • Hemoglobin A1c test less than 6.5 if have diabetes. • Hemoglobin A1c less than 5.7 if do not have diabetes. • Follow up with doctor on a regular basis. Maintain a healthy body weight • The more weigh, the harder heart has to work to give body nutrients. Research has shown contributes to the onset of diabetes and cardiovascular disease. Excess weight also raises blood triglycerides, and blood pressure, lowers HDL cholesterol, and increases the risk of diabetes. Exercise The heart is like any other muscle -- it needs a workout to stay strong and healthy. Exercising helps improve how well the heart pumps blood through body. Activity and exercise also help reduce so many other risk factors: can lower blood pressure, lower high cholesterol, reduce stress, achieve and maintain a healthy body weight, help self quit smoking, and improve blood sugar levels. •Goal: • Moderate exercise 30 minutes a day, on most days. More vigorous activities are associated with more benefits. Exercise should be aerobic, involving the large muscle groups. Aerobic activities include brisk walking, cycling, swimming, jumping rope, and jogging. • If walking is exercise of choice, use the pedometer goal of 10,000 steps a day.
- 32. PREVENTION OF CCF Follow a heart-healthy diet The old saying " are what eat," may be truer than ever - especially when it comes to cardiovascular are related to diet: high blood pressure, high blood cholesterol, diabetes, and obesity. •Goal: • Eat foods low in sodium, saturated fat, cholesterol, trans fat (partially hydrogenated fats), and • Omega-3 fatty acids are good fats and come from tuna, salmon, flaxseed, almonds, and • Mono-unsaturated fats also are preferred and are found in olive, canola and peanut oils. • Also eat plant-based foods such as fruit and vegetables, nuts, and whole grains. Contributing Risk Factors Individual response to stress: Although stress is not considered a traditional risk factor, some researchers have noted a relationship disease risk and stress in a person’s life, their health behaviors, and socioeconomic status. Stress may factors. Learn to manage stress by practicing relaxation techniques, learning how to manage time, setting realistic some new relaxation techniques such as guided imagery, massage, Tai Chi, meditation, or yoga. Drinking too much alcohol: Drinking too much alcohol can lead to increased blood pressure, heart failure, and stroke. It is also linked irregular heartbeats, obesity, and cancer. Research has shown that those who drink one drink per day (4 beer, or 1-1/2 oz. of 80-proof spirits) may have less risk. However, the American Heart Association does non-drinkers start using alcohol or that drinkers increase the amount they drink. If have a family history of cardiovascular disease or high cholesterol, it is even more important to decrease Get cholesterol levels tested every year. Know numbers, including blood pressure, BMI, waist A1c. Make sure follow up with health care provider every year for a checkup.