Cervical ca screening ..
•
0 likes•95 views
Cervical Cancer Screening Recommendations
Report
Share
Report
Share
Download to read offline
Recommended
UOG Journal Club: Single deepest vertical pocket or amniotic fluid index as e...

UOG Journal Club: Single deepest vertical pocket or amniotic fluid index as e...International Society of Ultrasound in Obstetrics and Gynecology (ISUOG)
UOG Journal Club: Screening for trisomies 21, 18 and 13 by cell-free DNA anal...

UOG Journal Club: Screening for trisomies 21, 18 and 13 by cell-free DNA anal...International Society of Ultrasound in Obstetrics and Gynecology (ISUOG)
UOG Journal Club: September 2016

UOG Journal Club: September 2016International Society of Ultrasound in Obstetrics and Gynecology (ISUOG)
UOG Journal Club: Ability of a preterm surveillance clinic to triage risk of ...

UOG Journal Club: Ability of a preterm surveillance clinic to triage risk of ...International Society of Ultrasound in Obstetrics and Gynecology (ISUOG)
UOG Journal Club: Genomic microarray in fetuses with increased nuchal translu...

UOG Journal Club: Genomic microarray in fetuses with increased nuchal translu...International Society of Ultrasound in Obstetrics and Gynecology (ISUOG)
UOG Journal Club: Prevention of pre-eclampsia by low-molecular-weight heparin...

UOG Journal Club: Prevention of pre-eclampsia by low-molecular-weight heparin...International Society of Ultrasound in Obstetrics and Gynecology (ISUOG)
More Related Content
What's hot
UOG Journal Club: Single deepest vertical pocket or amniotic fluid index as e...

UOG Journal Club: Single deepest vertical pocket or amniotic fluid index as e...International Society of Ultrasound in Obstetrics and Gynecology (ISUOG)
UOG Journal Club: Screening for trisomies 21, 18 and 13 by cell-free DNA anal...

UOG Journal Club: Screening for trisomies 21, 18 and 13 by cell-free DNA anal...International Society of Ultrasound in Obstetrics and Gynecology (ISUOG)
UOG Journal Club: September 2016

UOG Journal Club: September 2016International Society of Ultrasound in Obstetrics and Gynecology (ISUOG)
UOG Journal Club: Ability of a preterm surveillance clinic to triage risk of ...

UOG Journal Club: Ability of a preterm surveillance clinic to triage risk of ...International Society of Ultrasound in Obstetrics and Gynecology (ISUOG)
UOG Journal Club: Genomic microarray in fetuses with increased nuchal translu...

UOG Journal Club: Genomic microarray in fetuses with increased nuchal translu...International Society of Ultrasound in Obstetrics and Gynecology (ISUOG)
UOG Journal Club: Prevention of pre-eclampsia by low-molecular-weight heparin...

UOG Journal Club: Prevention of pre-eclampsia by low-molecular-weight heparin...International Society of Ultrasound in Obstetrics and Gynecology (ISUOG)
What's hot (20)
UOG Journal Club: Single deepest vertical pocket or amniotic fluid index as e...

UOG Journal Club: Single deepest vertical pocket or amniotic fluid index as e...
UOG Journal Club: Screening for trisomies 21, 18 and 13 by cell-free DNA anal...

UOG Journal Club: Screening for trisomies 21, 18 and 13 by cell-free DNA anal...
Dept. of Health cervical cancer fogsi_ screening test npcdcs_dept. of genera...

Dept. of Health cervical cancer fogsi_ screening test npcdcs_dept. of genera...
The 10 recommendations of society for maternal fetal medicine" AN Testing

The 10 recommendations of society for maternal fetal medicine" AN Testing
Cervical length for preterm birth prevention Aboubakr ELNASHAR

Cervical length for preterm birth prevention Aboubakr ELNASHAR
The limits to the number of EMBRYO TO TRANSFER. Prof Aboubakr Elnashar

The limits to the number of EMBRYO TO TRANSFER. Prof Aboubakr Elnashar
UOG Journal Club: Ability of a preterm surveillance clinic to triage risk of ...

UOG Journal Club: Ability of a preterm surveillance clinic to triage risk of ...
UOG Journal Club: Genomic microarray in fetuses with increased nuchal translu...

UOG Journal Club: Genomic microarray in fetuses with increased nuchal translu...
UOG Journal Club: Prevention of pre-eclampsia by low-molecular-weight heparin...

UOG Journal Club: Prevention of pre-eclampsia by low-molecular-weight heparin...
Similar to Cervical ca screening ..
Similar to Cervical ca screening .. (20)
screening programme in breast and colorectal carcinoma

screening programme in breast and colorectal carcinoma
Servikal Displazi -Pap Smear - Serviks Kanseri - www.jinekolojivegebelik.com

Servikal Displazi -Pap Smear - Serviks Kanseri - www.jinekolojivegebelik.com
Cervical cancer screening guidelines 2013 on 7th sept

Cervical cancer screening guidelines 2013 on 7th sept
РREMALIGNANT AND MALIGNANT DISORDERS OF THE CERVIX.pdf

РREMALIGNANT AND MALIGNANT DISORDERS OF THE CERVIX.pdf
More from med_students0
More from med_students0 (20)
Recently uploaded
Escort Service Call Girls In Sarita Vihar,, 99530°56974 Delhi NCR

Escort Service Call Girls In Sarita Vihar,, 99530°56974 Delhi NCR9953056974 Low Rate Call Girls In Saket, Delhi NCR
Russian Call Girls in Delhi Tanvi ➡️ 9711199012 💋📞 Independent Escort Service...

Russian Call Girls in Delhi Tanvi ➡️ 9711199012 💋📞 Independent Escort Service...Call Girls In Delhi Whatsup 9873940964 Enjoy Unlimited Pleasure
Recently uploaded (20)
Russian Call Girls in Chennai Pallavi 9907093804 Independent Call Girls Servi...

Russian Call Girls in Chennai Pallavi 9907093804 Independent Call Girls Servi...
Call Girls Service Chennai Jiya 7001305949 Independent Escort Service Chennai

Call Girls Service Chennai Jiya 7001305949 Independent Escort Service Chennai
Russian Call Girl Brookfield - 7001305949 Escorts Service 50% Off with Cash O...

Russian Call Girl Brookfield - 7001305949 Escorts Service 50% Off with Cash O...
Escort Service Call Girls In Sarita Vihar,, 99530°56974 Delhi NCR

Escort Service Call Girls In Sarita Vihar,, 99530°56974 Delhi NCR
Low Rate Call Girls Pune Esha 9907093804 Short 1500 Night 6000 Best call girl...

Low Rate Call Girls Pune Esha 9907093804 Short 1500 Night 6000 Best call girl...
Artifacts in Nuclear Medicine with Identifying and resolving artifacts.

Artifacts in Nuclear Medicine with Identifying and resolving artifacts.
Call Girls Service Noida Maya 9711199012 Independent Escort Service Noida

Call Girls Service Noida Maya 9711199012 Independent Escort Service Noida
Russian Call Girls Chennai Madhuri 9907093804 Independent Call Girls Service ...

Russian Call Girls Chennai Madhuri 9907093804 Independent Call Girls Service ...
Call Girls Service Bellary Road Just Call 7001305949 Enjoy College Girls Service

Call Girls Service Bellary Road Just Call 7001305949 Enjoy College Girls Service
Hi,Fi Call Girl In Mysore Road - 7001305949 | 24x7 Service Available Near Me

Hi,Fi Call Girl In Mysore Road - 7001305949 | 24x7 Service Available Near Me
Vip Call Girls Anna Salai Chennai 👉 8250192130 ❣️💯 Top Class Girls Available

Vip Call Girls Anna Salai Chennai 👉 8250192130 ❣️💯 Top Class Girls Available
Call Girls Service in Bommanahalli - 7001305949 with real photos and phone nu...

Call Girls Service in Bommanahalli - 7001305949 with real photos and phone nu...
VIP Mumbai Call Girls Hiranandani Gardens Just Call 9920874524 with A/C Room ...

VIP Mumbai Call Girls Hiranandani Gardens Just Call 9920874524 with A/C Room ...
Ahmedabad Call Girls CG Road 🔝9907093804 Short 1500 💋 Night 6000

Ahmedabad Call Girls CG Road 🔝9907093804 Short 1500 💋 Night 6000
CALL ON ➥9907093804 🔝 Call Girls Baramati ( Pune) Girls Service

CALL ON ➥9907093804 🔝 Call Girls Baramati ( Pune) Girls Service
Russian Call Girls in Delhi Tanvi ➡️ 9711199012 💋📞 Independent Escort Service...

Russian Call Girls in Delhi Tanvi ➡️ 9711199012 💋📞 Independent Escort Service...
Call Girls Yelahanka Just Call 7001305949 Top Class Call Girl Service Available

Call Girls Yelahanka Just Call 7001305949 Top Class Call Girl Service Available
Russian Call Girls in Pune Tanvi 9907093804 Short 1500 Night 6000 Best call g...

Russian Call Girls in Pune Tanvi 9907093804 Short 1500 Night 6000 Best call g...
Russian Call Girls in Bangalore Manisha 7001305949 Independent Escort Service...

Russian Call Girls in Bangalore Manisha 7001305949 Independent Escort Service...
Sonagachi Call Girls Services 9907093804 @24x7 High Class Babes Here Call Now

Sonagachi Call Girls Services 9907093804 @24x7 High Class Babes Here Call Now
Cervical ca screening ..
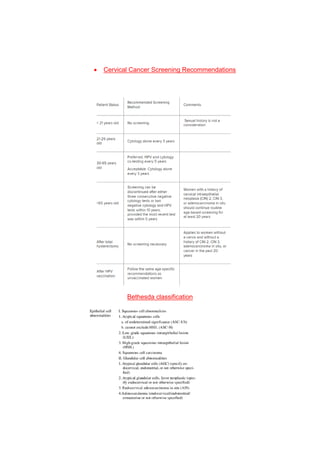
- 1. Cervical Cancer Screening Recommendations Bethesda classification
- 2. For a women less than 25 years of age, a Pap result of “atypical squamous cells of undetermined significance,” is preferably followed by another pap smear in 1 year
- 3. In women over 30 years of age, the preferred routine screening regimen is co- testing (cytology + HPV testing) every 5 years in a woman with negative HPV, the risk of significant cytologic abnormality is low and should be followed by routine screening (cotesting in 5 years). women aged 21 to 24 years of age with ASC-US or LSIL should have repeat cytology in 1 year. If that repeat cytology is negative, ASC-US or LSIL, the clinician should repeat cytology in another 12 months. If the repeat cytology shows high-grade atypical squamous cells (ASC-H), atypical glandular cells (AGC), or high-grade squamous intraepithelial lesions (HSIL), the clinician should proceed to colposcopy at that time. Once there are two consecutive negative cytologies, normal screening can be resumed. If the repeat cytology (on the third Pap) is ASC-US or greater, it is recommended to proceed to colposcopy.
- 4. According to the current ASCCP guidelines, any result of ASC-H should be followed by colposcopy. This should happen regardless of HPV result in a woman more than 25 years of age due to the possibility of significant cytologic abnormality. Types 16 and 18 are particularly correlated with cervical cancer and should prompt more frequent monitoring. Women more than 30 years of age with normal cytology and the presence of high-risk sub-types of HPV should have repeat cotesting (cytology and HPV testing) at 1 year. If the high-risk sub-type
- 5. is still present at that time or the cytology is ASC-US or greater, clinicians should proceed with colposcopy. All subcategories of AGC should proceed with colposcopy with endocervical sampling and endometrial sampling in women who are 35 years of age or older, OR at risk for endometrial neoplasia Although HPV status is useful in the management of abnormal cervical pathology, it is not predictive of endometrial cancer and AGC should prompt endometrial biopsy even in the absence of HPV infection
- 6. The preferred action in this step is to proceed to colposcopy without endocervical sampling during this pregnancy. Deferring until 6 weeks postpartum is an option, but not the preferred recommendation, due to the risk of significant cytologic abnormality. ================================
- 7. :SUMMERY 1-Age 21-24 with ASC-US or LSIL Repeat cytology in 1 year if the result : Negative , ASC-US or LSIL Repeat cytology in 1 year- AGC, HSIL, ASC-H colposcopy 2-Age >30 with TZ absent or insufficient + HPV negative routine testing every 5 years-screening regimen is co testing every 1-coPositive+ HPVTZ absent or insufficientAge >30 with-3 years -corepeatPositivecytology and + HPVnormalwith30 yearsAge >-4 .testing at 1 year regardless of HPVcolposcopyshould be followed byH-ASCny result ofA-5 result. colposcopyPositiveHPV+LSIL-6 - LSIL + No HPV Test colposcopy if theyearat 1testing-repeat conegativeHPV+LSIL30 yearsAge >- yearat 3testing-repeat coresult negative 7- Age >35 years with AGC with colposcopy with endocervical sampling. 8-Women with HSIL colposcopy with endocervical assessment Prepared by dr.anas alsaab
