Cardiomyopathy om verma
- 2. Cardiomyopathy PRESENTED BY MR. OM VERMA ASSISTANT PROFESSOR MEDICAL SURGICAL NURSING RELIANCE INSTITUTE OF NURSING
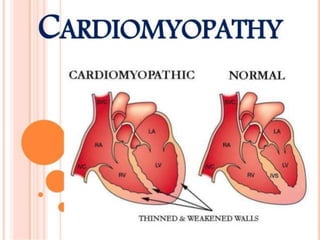
- 3. DEFINITION u Cardiomyopathy is a type of heart disease in which the heart muscle is abnormal enlarge thickened and stiffened as a result the heart muscle ability to pump blood is usually impaired . u JOYCE M BLACK
- 4. Cardiomyopathy is a wakening of heart muscle or a change in heart muscle structure ,it is often associated with inadequate heart pumping or other function heart problem . BRUNNER AND SIDDHARTH
- 5. Cardiomyopathy is a define as structural and functional abnormality of the heart muscle
- 6. disease of the heart muscle in which the heart loses its ability to pump blood effectively the heart muscle becomes enlarged or abnormally thick or rigid. In rare cases, the muscle tissue in the heart is replaced with scar tissue. As cardiomyopathy progresses the heart becomes weaker and less able to pump blood through the body to heart failure, arrhythmias, systemic and pulmonary edema and, more rarely, endocarditis Cardiomyopathy
- 7. A primary disorder of the heart muscle that causes abnormal myocardial performance and is not the result of disease or dysfunction of other cardiac structures … myocardial infarction, systemic hypertension, valvular stenosis or regurgitation” According to lippin cott
- 8. 12/98 medslides.com 8 Incidence and Prognosis 3-10 cases per 100,000 20,000 new cases per year in the U.S.A. death from progressive pump failure 1-year 25% 2-year 35-40% 5-year 40-80% stabilization observed in 20-50% of patient complete recovery is rare
- 9. THE 3 MAIN TYPES OF CARDIOMYOPATHY ARE: 1. Dilated cardiomyopathy 2. Hypertrophic cardiomyopathy 3. Restrictive cardiomyopathy
- 11. DILATED CARDIOMYOPATHY u most common form of cardiomyopathy u generally occurs in adults aged 20 to 60 years u more common in men the heart muscle begins to dilate or stretch and become thinner Ventricular chamber size over time, the heart becomes weaker heart failure symptoms of heart failure: fatigue, edema, and SOB can also lead to heart valve problems (regurgitation), arrhythmias, and blood clots in the heart (poor blood flow), emboli formation a common reason for needing a heart transplant.
- 12. It refers to overall enlargement of the heart chamber especially the ventricles and increase atrial chamber size and weakness of heart muscle and poor pumping . According to lippin cott
- 13. Dilated cardiomyopathy (DCM) is when the heart's ability to pump blood is lessened because its main pumping chamber, the left ventricle, is enlarged and weakened. In some cases, this prevents the heart from filling with blood . According to lewis
- 15. Types and Causes: u Ischemic cardiomyopathy - caused by CAD & MI , w/c leave scars in the heart muscle Ischemic cardiomyopathy (IC) is a condition when your heart muscle is weakened as a result of a heart attack or coronary artery disease. In coronary artery disease, the arteries that supply blood to your heart muscle become narrowed. u Idiopathic cardiomyopathy - the cause is unknown. u Hypertensive cardiomyopathy - seen in people who have high BP for a long time, particuarly when it has gone untreated for years.
- 16. u Infectious cardiomyopathy - HIV, viral myocarditis u Alcoholic cardiomyopathy - usually begins about 10 years after sustained, heavy alcohol consumption. u Toxic cardiomyopathy – due to cocaine, amphetamines, and some chemotherapy drugs (doxorubicin, daunorubicin) u Peripartum cardiomyopathy: This type appears in women during the last trimester of pregnancy or after childbirth. u Radiotherapy (cobalt) u diabetes and thyroid disease
- 17. HYPERTROPHIC CARDIOMYOPATHY Is an overgrowth of heart muscle that can impair blood flow both in to and out of the heart and thickened inter ventricular septum and left ventricular hypertrophy According to Brunner & Suddarth's
- 18. Hypertrophic cardiomyopathy (HCM) is a condition in which a portion of the heart becomes thickened without an obvious cause. This results in the heart being less able to pump blood effectively. Symptoms vary from none to feeling tired, leg swelling, and shortness of breath. According lippin cott
- 19. Hypertrophic Cardiomyopathy occurs when the heart muscle thickens abnormally (left ventricle) 1.) obstructive type - the septum thickens and bulges into the left ventricle blocks the flow of blood into the aorta the ventricle must work much harder to pump blood past the blockage and out to the body - symptoms can include chest pain, dizziness, shortness of breath, or fainting. - can also affect the mitral valve, causing blood to leak backward through the valve. 2.) non-obstructive type - the entire ventricle may become thicker (symmetric ventricular hypertrophy) or it may happen only at the bottom of the heart (apical hypertrophy). The right ventricle also may be affected.
- 21. Pathophysiology: Left ventricular hypertrophy (thick ventricular wall) ventricular chamber size hold less blood CO pressure in the ventricles and lungs changes in the cardiac muscles interfere with the heart's electrical signals, leading to arrhythmias sudden cardiac arrest Causes: u inherited because of a gene mutation u develop over time because of high blood pressure or aging u often, the cause is unknown. Hypertrophic Cardiomyopathy
- 23. RESTRICTIVE CARDIOMYOPATHYu u The ventricles become stiff and rigid due to replacement of the normal heart muscle with abnormal tissue, such as scar tissue. u As a result, the ventricles cannot relax normally and expand to fill with blood, which causes the atria to become enlarged. u Eventually, blood flow in the heart is reduced, and complications such as heart failure or arrhythmias occur. Causes: u radiation treatments, infections, or scarring after surgery u Hemochromatosis - a condition in which too much iron is deposited into tissues, including heart tissue u Amyloidosis, a disease in which abnormal proteins are deposited into heart tissue u Sarcoidosis, a disease in which inflammation produces tiny lumps of cells in various organs in the body, including the heart
- 24. Restrictive cardiomyopathy (RCM) is a form of cardiomyopathy in which the walls of the heart are rigid (but not thickened). Thus the heart is restricted from stretching and filling with blood properly. According to lippin cott
- 25. RESTRICTIVE CARDIOMYOPATHY Is the common type of Cardiomyopathy I n this condition the heart muscle is too stiff . According to luckmans
- 26. ARRHYTHMOGENIC RIGHT VENTRICLE HYPERTROPHY Fibrous scar And adipose tissue covering the right ventricle .
- 27. u Arrhythmogenic right ventricular dysplasia (ARVD) is a rare type of cardiomyopathy. It occurs if the muscle tissue in the right ventricle dies and is replaced with scar tissue. This disrupts the heart's electrical signals and causes arrhythmias. Symptoms include palpitations and fainting after physical activity.
- 28. ETIOLOGY Chronic excessive alcohol consumption INFECTION= viral endocarditis and myocardaties Adenovirus Parvovirus Human immune deficiency virus Parasites protozoa
- 29. u THIAMINE DEFICIENCY u Thiamine (vitamin B1) serves as an important cofactor ( help) in body metabolism and energy production. a lack of thiamine affects several organ systems, in particular the cardiovascular and nervous system.
- 30. ZINC DEFICIECY u Zinc is a vital element in maintaining the normal structure and physiology of cells. ... to have protective effects in coronary artery disease and Cardiomyopathy.
- 31. COLLEGEN VASCUL DISEASE increase connective tissue growth AUTO IMMUNE DISEASE GLYCOGEN STORAGE DISEASE
- 32. u Glycogen storage disease type II, also called Pompe disease, is an autosomal recessive metabolic disorder which damages muscle and nerve cells throughout the body. It is caused by an accumulation of glycogen in the lysosome due to deficiency of the lysosomal acid alpha- glucosidase enzyme. It is the only glycogen storage disease with a defect in lysosomal metabolism, Con……………………………………………………..plto
- 33. The build-up of glycogen causes progressive muscle weakness (myopathy) throughout the body and affects various body tissues, particularly in the heart, skeletal muscles, liver and the nervous system.
- 34. AMYLOIDOSIS Cardiac Amyloidosis ("stiff heart syndrome") occurs when amyloid deposits take the place of normal heart muscle. It is the most typical type of restrictive cardiomyopathy. Cardiac Amyloidosis may affect the way electrical signals move through the heart (conduction system). This can lead to abnormal heartbeats (arrhythmias) and faulty heart signals (heart block).
- 35. STRESS is a condition in which intense emotional or physical stresscan cause rapid and severe heart muscle weakness (cardiomyopathy).
- 36. Other drugs Exposure to heavy metals such as lead, arsenic, cobalt, or mercury Cocaine Cobalt Emetine ( amebic dysentery) Anthracyclines ( antibiotics )
- 37. Major Risk Factors uHaving a family history of cardiomyopathy, heart failure, or sudden cardiac death uHaving a disease or condition that can lead to cardiomyopathy, such as: u Coronary artery disease u A previous heart attack u Myocarditis uDiseases that can damage the heart (for example, hemochromatosis, sarcoidosis, or amyloidosis) uLong-term alcoholism uLong-term high blood pressure uDiabetes and other metabolic diseases
- 38. PATHOPHYSIOLOGY Due to etiological factors Impaired cardiac output Decrease stroke volume ( amount of b/d ejected per beat by the lift ventricle in to arota )
- 39. u Stimulate the sympathetic nervous system renin angiotension and aldosterone response Result increase systemic valular resistance Na increase and fluid retention
- 40. Increase workload of heart Then lead to Cardiomyopathy
- 41. Signs and Symptoms u some have no symptoms in the early stages of the disease u as cardiomyopathy progresses and the heart weakens, signs and symptoms of heart failure usually appear. These signs and symptoms include: uTiredness uWeakness uShortness of breath after exercise or even at rest uSwelling of the abdomen, legs, ankles, and feet uOther signs and symptoms: dizziness, lightheadedness, fainting during exercise, abnormal heart rhythms, murmurs
- 42. common symptoms are: Chest pain or pressure (more likely with exercise) Cough Fatigue, weakness, faintness Irregular or rapid pulse Loss of appetite Shortness of breath with activity or after lying down (or being asleep) for a while Swelling of feet and ankles
- 43. 12/98 medslides.com 43 History and Physical Examination Symptoms of heart failure pulmonary congestion (left HF) dyspnea (rest, exertional, nocturnal), orthpnea systemic congestion (right HF) edema, nausea, abdominal pain, nocturia low cardiac output fatigue and weakness hypotension, tachycardia, tachypnea, JVD
- 44. 12/98 medslides.com 44 Cardiac Imaging Chest radiogram Electrocardiogram 24-hour ambulatory ECG (Holter) lightheadedness, palpitation, syncope Two-dimensional echocardiogram Radionuclide ventriculography Cardiac catheterization age >40, ischemic history, high risk profile, abnormal ECG
- 45. Interventions The main goals of treating cardiomyopathy are to: u Manage any conditions that cause or contribute to the cardiomyopathy u Control symptoms so that the person can live as normally as possible u Stop the disease from getting worse u Reduce complications and the chance of sudden cardiac death Medications: u Diuretics, which remove excess fluid and sodium from the body. u Angiotensin-converting enzyme (ACE) inhibitors, which lower blood pressure and reduce stress on the heart. u Beta-blockers, which slow the heart rate by reducing the speed of the heart's contractions. These medicines also lower BP u Calcium channel blockers, which slow a rapid heartbeat by reducing the force and rate of heart contractions, decrease BP
- 46. Medications u Digoxin - increases the force of heart contractions and slows the heartbeat. u Anticoagulants, which prevent blood clots from forming. Anticoagulants are often used in the treatment of dilated cardiomyopathy. u Antiarrhythmia medicines, which keep the heart beating in a normal rhythm. u Antibiotics, which are used before dental or surgical procedures. Antibiotics help to prevent endocarditis, an infection of the heart walls, valves, and vessels. u Corticosteroids, which reduce inflammation.
- 47. Surgery u Septal myectomy - also called septal myomectomy - is open-heart surgery for hypertrophic obstructive cardiomyopathy - generally used in younger patients and when medicines aren't working well. u Procedure: 1. a surgeon removes part of the thickened septum that is bulging into the left ventricle this widens the pathway in the ventricle that leads to the aortic valve and improves blood flow through the heart and out to the body 2. If necessary, the mitral valve can be repaired or replaced at the same time. This surgery is often successful, and the person can return to a normal life with no symptoms.
- 48. Surgery (cont.) u Surgically implanted devices. - Surgeons can place several different types of devices in the heart to help it beat more effectively. 1. A left ventricular assist device (LVAD) - helps the heart pump blood to the body - LVAD can be used as a long-term therapy or as a short-term treatment for people who are waiting for a heart transplant. 2. An implantable cardioverter defibrillator (ICD) - is used in people who are at risk of life-threatening arrhythmia or sudden cardiac death. - This small device is implanted in the chest and connected to the heart with wires. If the ICD senses a dangerous change in heart rhythm, it will send an electric shock to the heart to restore a normal heartbeat. u Heart Transplant
- 51. Lifestyle Changes uThe doctor may recommend lifestyle changes to manage a condition that is causing the cardiomyopathy. These changes may help reduce symptoms. Lifestyle changes may include: uQuitting smoking uLosing excess weight uEating a low-salt diet uGetting moderate exercise, such as walking, and avoiding strenuous exercise uAvoiding the use of alcohol and illegal drugs uGetting enough sleep and rest uReducing stress uTreating underlying conditions, such as diabetes and high blood pressure
- 52. Heart Transplant u an operation in which the diseased heart in a person is replaced with a healthy heart from a deceased donor. u 90% of heart transplants are performed on patients with end-stage heart failure ---.
- 53. u Patients who might not be candidates for heart transplant surgery, because the procedure is less likely to be successful. u Advanced age - most transplant surgery isn't performed on patients older than 70 years. u Poor blood circulation throughout the body, including the brain. u Diseases of the kidney, lungs, or liver that can't be reversed. u History of cancer or malignant tumors. u Inability or unwillingness to follow lifelong medical instructions after a transplant. u Pulmonary arterial hypertension (high blood pressure in the lungs) that can't be reversed. u Active infection throughout the body. Heart Transplant (cont.)
- 54. u Organs are matched for blood type and size of donor and recipient. u The Donor Heart Guidelines on how a donor heart is selected : the donor meet the legal requirement for brain death consent forms are signed younger than 65 years of age have little or no history of heart disease or trauma to the chest not exposed to hepatitis or HIV donor heart must be transplanted w/in 4 hrs. after removal from the donor Heart Transplant (cont.)
- 56. u A bypass machine is hooked up to the arteries and veins of the heart. The machine pumps blood through the patient's lungs and body while the diseased heart is removed and the donor heart is sewn into place. u Preventing Rejection Immunosuppressants used: cyclosporine, tacrolimus, MMF (mycophenolate mofetil), and steroids such as prednisone. uWatching for Signs of Rejection u Shortness of breath u Fever u Fatigue u Weight gain u Reduced amounts of urine u Preventing Infection Heart Transplant (cont.)
- 57. What Are the Risks of a Heart Transplant? u Failure of the donor heart u Primary Graft Dysfunction u Rejection of the Donor Heart u Cardiac Allograft Vasculopathy - the walls of the new heart's coronary arteries become thick, hard, and lose their elasticity. - can cause heart attack, heart failure, dangerous arrhythmias, and sudden cardiac arrest u Complications from medicines - risk of infection, diabetes, osteoporosis , high blood pressure, kidney damage, and cancer u Infection u Cancer – lymphoma and skin cancer (due to suppression of the immune system)
- 58. COMPLICATION Heart failure. Heart failure means your heart can't pump enough blood to meet your body's needs. The thickened, stiffened or weakened heart muscle due to cardiomyopathy can become unable to pump or can stop blood from flowing out of the heart
- 59. Valve problems. Because people with Cardiomyopathy have an enlarged heart, the heart valves may not close properly, leading to a backward flow of blood. Cardiac arrest and sudden death.
