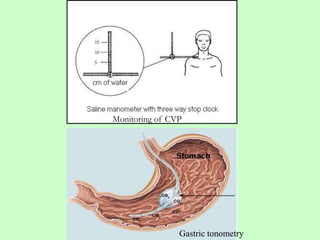
This document discusses the monitoring of critically ill patients. It explains that critically ill patients are difficult to diagnose and manage in general wards due to incomplete histories, inconclusive exams, and disappearing signs near death. Intensive care units are better equipped with monitoring technologies and expert staff to continuously monitor patients. The document outlines various physiological parameters to monitor in critically ill patients, including cardiovascular, respiratory, renal, central nervous, coagulation systems, and hematological factors. Continuous monitoring in ICUs allows for assessment of patients' physiological reserves and the effectiveness of treatments.