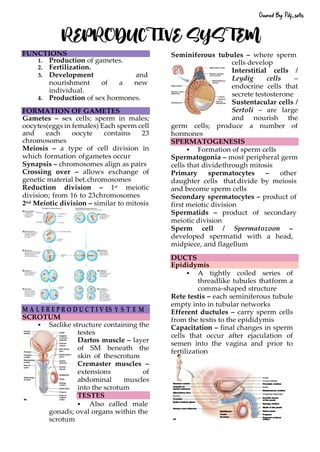
Male Reproductive System Functions
- 1. FUNCTIONS 1. Production of gametes. 2. Fertilization. 3. Development and nourishment of a new individual. 4. Production of sex hormones. FORMATION OF GAMETES Gametes – sex cells; sperm in males; oocytes(eggs in females) Each sperm cell and each oocyte contains 23 chromosomes Meiosis – a type of cell division in which formation ofgametes occur Synapsis – chromosomes align as pairs Crossing over – allows exchange of genetic material bet.chromosomes Reduction division – 1st meiotic division; from 16 to 23chromosomes 2nd Meiotic division – similar to mitosis M A L E R E P R O D U C T I V ES Y S T E M SCROTUM ▪ Saclike structure containing the testes Dartos muscle – layer of SM beneath the skin of thescrotum Cremaster muscles – extensions of abdominal muscles into the scrotum TESTES ▪ Also called male gonads; oval organs within the scrotum Seminiferous tubules – where sperm cells develop Interstitial cells / Leydig cells – endocrine cells that secrete testosterone Sustentacular cells / Sertoli – are large and nourish the germ cells; produce a number of hormones SPERMATOGENESIS ▪ Formation of sperm cells Spermatogonia – most peripheral germ cells that dividethrough mitosis Primary spermatocytes – other daughter cells that divide by meiosis and become sperm cells Secondary spermatocytes – product of first meiotic division Spermatids – product of secondary meiotic division Sperm cell / Spermatozoon – developed spermatid with a head, midpiece, and flagellum DUCTS Epididymis ▪ A tightly coiled series of threadlike tubules thatform a comma-shaped structure Rete testis – each seminiferous tubule empty into in tubular networks Efferent ductules – carry sperm cells from the testis to the epididymis Capacitation – final changes in sperm cells that occur after ejaculation of semen into the vagina and prior to fertilization REPRODUCTIVE SYSTEM Owned By: Pdf_sells
- 2. Ductus Deferens / Vas deferens ▪ Emerges from the epididymis and ascends along the posterior side of the testis Spermatic cord – consists of the ductus deferens, testicular artery and veins, lymphatic vessels, and testicular nerve Ampulla of the ductus deferens – ductus deferens increases in diameter Seminal Vesicle Ejaculatory Duct DuctSeminal vesicle – sac-shaped gland Ejaculatory duct – formed by the ducts from the seminal vesicle and the ampulla of the ductus deferens Urethra Prostatic urethra – passes through the prostate gland Membranous urethra – passes through the floor of thepelvis; surrounded by the external urinary sphincter Spongy urethra – extends the length of the penis andopens at its end PENIS ▪ Male organs of copulation ▪ Functions in transfer of sperm cells from the male to the female Erection – process of the engorgement of the erectile tissue with blood that causes the penis to enlarge and become firm Corpora cavernosa – two columns of erectile tissue that form the dorsal portion Corpus spongiosum – third, small erectile column thatoccupies the ventral portion of the penis Glans penis – a formed cap External urethra orifice – spongy urethra that opens to the exterior Prepuce / foreskin – lose fold of skin that covers the glans penis GLANDS Seminal Vesicles – next to ductus deferens help form ejaculatory duct Prostate gland – consists of glandular _ muscular tissue & empties into the urethra Bulbourethral glands / Cowper glands – a pair of small, mucus-secreting glands that empty into the urethra SECRETIONS Semen – mixture of sperm cells + gland secretions; provides a transport medium and nutrients that protect and activate sperm - 60% of fluid is from seminal vesicles - 30% of fluid is from prostate gland - 5% of fluid is from bulbourethral gland - 5% of fluid is from testes Prostate fluid – contains nutrients and proteolyticenzymes; neutralizes the pH Owned By: Pdf_sells
- 3. of the vagina Bulbourethral + urethral mucuous glands – produce mucus that neutralizes the acidic pH of the urethra PATH OF SPERM 1. Sperm develop in seminiferous tubules (testes) 2. Epididymis (mature) 3. Ductus deferens 4. Receive secretions from seminal vesicles, prostate gland, and bulbourethral gland 5. Urethra where semen (sperm) exit body PHYSIOLOGY OF MALE REPRODUCTION Regulation of Sex Hormone Secretion Gonadotropin-releasing hormone (GnRH) – produced in hypothalamus; stimulates release of LH and FSH from the anterior pituitary Luteinizing hormone (LH) – stimulates interstitial cells to produce testosterone Follicle-stimulating hormone (FSH) – binds to sustentacular cells and stimulates spermatogenesis and secretion of inhibin Testosterone – has a negative-feedback effect on GnRH, LH, and FSH Inhibin – has a negative-feedback effect on FSHsecretion PRODUCTION OF SPERM CELLS 1. Germ cells 2. Spermatogonia 3. Primary spermatocytes 4. Secondary spermatocytes 5. Spermatids 6. Sperm cells SPERM CELL’S STRUCTURE • Head: contain a nucleus and DNA • Midpiece: contain mitochondria • Tail: flagellum for movement Puberty in Males ▪ Before puberty; small amounts of testosterone inhibit GnRH release. ▪ During puberty; testosterone does not completely suppress GnRH release, resulting in increased prod. of FSH, LH, and testosterone. Puberty – sequence of events by which a child is transformed into a young adult Effects of Testosterone ▪ Enlargement of the genitals; necessary for spermatogenesis Owned By: Pdf_sells
- 4. ▪ Responsible for the development of secondary sexual characteristics (hair distribution and growth, skin texture, fat distribution, skeletal muscle growth, changes in the larynx) Male Sexual Behavior and the Male Sex Act Testosterone – required for normal for sex drive Emission – movement of sperm cells, mucus, prostatic secretions, and seminal vesicle secretions into the prostatic, membranous, spongy urethra Orgasm / climax – result of pleasurable, intensesensation Resolution – penis becomes flaccid; an overall feeling ofsatisfaction exists Erection – first major component of the male sex act Erectile dysfunction (ED) – impotence; failure toachieve erections Infertility in Males ▪ Common cause is a low sperm cell count Artificial insemination – concentrating the sperm cellsand inserting them into the female’s reproductive tract F E M A L E R E P R O D U C T I V E S Y S T E M Broad ligament – spreads out on both sides of the uterusand attaches to the ovaries and uterine tubes; Produce female oocytes • (sex cells) • Produce female sex hormones • Receive sperm from males • Develop and nourish embryos OVARIES Suspensory ligament – extends from each ovary to thelateral body wall Ovarian ligament – attaches the ovary to the superiormargin of the uterus Mesovarium – folds of peritoneum OOGENESIS AND FERTILIZATION Oogonia – the cells form which oocytes develop Primary oocyte – oogonia that has stopped I prophase I Ovulation – release of an oocyte from an ovary Secondary oocyte – released when the first meioticdivision is complete Fertilization – when a sperm cell penetrates thecytoplasm of a secondary oocyte Zygote – 23 chromosomes from the sperm + 23 chromosomes from the female gamete Follicle Development Primordial follicle – primary oocyte surrounded by granulosa cells (single layer of flat cells) Primary follicles – oocyte enlarges and the single layer of granulosa cells become enlarged and cuboidal Zona pellucida – a layer of clear material that is deposited around the primary oocyte Secondary follicle – fluid-filled vesicles appear and a theca form around the follicle Fluid filled spaces – vesicles Theca – a capsule that forms around the follicle Antrum – a single, fluid-filled chamber Graafian follicle – mature follicle Cumulus cells – mass of granulosa cells Corpus luteum – remaining cells of the ruptured follicleare transformed into a glandular structure Human chorionic gonadotropin hormone (hCG) – the corpus luteum Owned By: Pdf_sells
- 5. enlarges in response to this hormone UTERINE TUBES ▪ Fallopian tube or oviduct ▪ Receive the secondary oocyte Fimbriae – long, thin processes that surrounds each the opening of each uterine tube ➢ Cilia on fimbriae – sweep the oocyte into theuterine tube Ampulla – where fertilization usually occurs Implantation – process wherein the fertilized oocyte embeds itself in the uterine wall UTERUS Fundus – superior to the entrance of the uterine tubes Body – main part of the uterus Cervix – inferiorly, narrower part Uterine cavity & cervical canal – spaces formed by theuterus Perimetrium – outer layer; serous layer of the uterusformed from visceral peritoneum Myometrium – middle layer; muscular layer hat accounts for the bulk of the uterine wall Endometrium – innermost layer; consists of simple columnar epithelial cells with an underlying CT layer Spiral glands – simple tubular glands formed by foldsof endometrium Prolapsed uterus – occurs when the uterus extendsinferiorly into the vagina VAGINA ▪ Female organs of copulation ▪ Allows menstrual flow and childbirth Muscular layer – smooth muscle + elastic fibers Mucous membrane – moist stratified squamous epithelium that forms a protective surface Hymen – thin mucous membrane EXTERNAL GENITALIA Vulva – pudendum; external female genitalia Vestibule – the space into which the vagina and urethra open Labia minora – thing, longitudinal skin folds Clitoris – small, erectile structure; well supplied with sensory receptors, made up of erectile tissue Greater vestibular glands – produce a lubricating fluid that helps maintain the moistness of the vestibule Labia majora – prominent, rounded folds of skin Mons pubis – an elevation of tissue over the pubic symphysis Pudendal cleft – space bet. the labia majora Clinical perineum – region bet. the vagina and the anus Episiotomy – an incision made I the clinical perineum to avoid tearing during childbirth MAMMARY GLANDS ▪ Organs of milk production ▪ Located in the breasts ▪ Modified sweat glands Owned By: Pdf_sells
- 6. Areola – a circular, pigmented area that surrounds the nipple Gynecomastia – occurs when the breasts of a male become permanently enlarged; results from hormonal imbalance and the abuse of anabolic steroids Glandular lobes – covered by adipose tissue; gives the breast its form Lactiferous duct – opens independently to the surface of the nipple Myoepithelial cells – surround the alveoli and contract to expel milk from the alveoli OVULATION • when a mature follicle rupture forcing oocyte into peritoneal (pelvic) cavity • due to LH (anterior pit. gland) PHYSIOLOGY OF FEMALE REPRODUCTION Puberty in Females Menarche – first episode of the menstrual bleeding Menstrual cycle – series of changes that occur in sexually mature, non- pregnant females, and that culminate in menses Menses – a period of mild hemorrhage; part of the endometrium is sloughed and expelled from the uterus; day 1 – 4: menstrual fluid is produced by degeneration of the endometrium Proliferative phase – day 5 – ovulation: epithelial cells multiply and form glands Secretory phase – day of ovulation – 28: endometrium becomes thicker, endometrial glands secete Blastocyst – a collection of cells produced by the zygote Ectopic pregnancy – implantation occurs anywhere other than in the uterine cavity STAGES OF MENSTRUAL CYCLE Days 1-5 Menses (shedding of endometrium) o menstrual bleeding (menses) o estrogen and progesterone levels are low o follicle begins to mature Days 6-13 Proliferative (between end of menses and ovulation) - endometrium rebuilds - estrogen levels begin to increase - progesterone levels remain low - follicle matures Day 14 Ovulation - oocyte is released due to LH - estrogen levels high - progesterone levels are increasing - cervical mucus thins Days 15-28 Secretory (between Owned By: Pdf_sells
- 7. ovulation and next menses) - endometrium is preparing for implantation - estrogen levels decrease (low) - progesterone levels high - cervical mucus thickens MENOPAUSE ▪ Cessation of menstrual cycles (Female) Climacteric – the whole time period from the onset of irregular cycles to their complete cessation FEMALE SEXUAL BEHAVIOR AND THE FEMALE SEX ACT Orgasm / climax – triggered by tactile stimulation of the female’s genitalia during intercourse or psychological stimuation Resolution – the overall sense of satisfaction and relaxation after the sex act Owned By: Pdf_sells