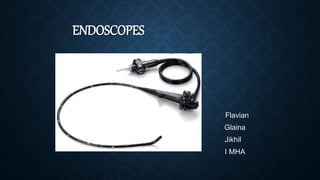
Endoscopes
- 2. INTRODUCTION During an endoscopy, the doctor inserts a tool called an endoscope into a person’s body. Most endoscopes are thin tubes with a powerful light and tiny camera at the end. The endoscope’s length and flexibility depend on the part of the body the doctor needs to see. For example, a straight endoscope helps a doctor look at joints. Meanwhile, a flexible one helps a doctor view the inside of the colon.
- 3. ENDOSCOPY Endoscopy is a procedure that allows a doctor to view the inside of a person’s body. Doctors use it to diagnose diseases in the following parts of the body: Esophagus Stomach Colon Ears Nose Throat Heart Urinary tract Joints Abdomen
- 4. FUNCTIONS Endoscopes were first developed to look at parts of the body that couldn’t be seen any other way. 1. To prevent and screen for cancer 2. To find cancer early 3. Looking for causes of symptoms 4. Looking at problems found on imaging tests 5. Destroying or removing cancer cell.
- 5. TYPES OF ENDOSCOPES Name of procedure Name of tool Area or organ viewed How endoscope reaches target area Anoscopy Anoscope Anus and/or rectum Inserted through the anus Arthroscopy Arthroscope Joints Inserted through a small incision over the joint Bronchoscopy Bronchoscope Trachea, or windpipe, and the lungs Inserted through the mouth Colonoscopy Colonoscope Entire length of the colon and large intestine Inserted through the anus Colposcopy Colposcope Vagina and cervix Placed at the vagina’s opening after a tool called a speculum dilates the vagina. It is not inserted in the body.
- 6. Bronchoscope
- 9. Cystoscopy Cystoscope Inside of the bladder Inserted through the urethra Esophagoscopy Esophagoscope Esophagus Inserted through the mouth Gastroscopy Gastroscope Stomach and duodenum, which is the beginning of the small intestine Inserted through the mouth Laparoscopy Laparoscope Stomach, liver, or other abdominal organs, including female reproductive organs, including the uterus, ovaries, and fallopian tubes Inserted through a small, surgical opening in the abdomen Laryngoscopy Laryngoscope Larynx, or voice box Inserted through the mouth
- 10. Neuroendoscopy Neuroendoscope Areas of the brain Inserted through a small incision in the skull Proctoscopy Proctoscope Rectum and sigmoid colon, which is the bottom part of the colon Inserted through the anus Sigmoidoscopy Sigmoidoscope Sigmoid colon Inserted through the anus Thoracoscopy Thoracoscope Pleura, which are the 2 membranes covering the lungs and lining the chest cavity, and structures covering the heart Inserted through a small surgical opening in chest
- 11. OTHER TOOLS USED DURING AN ENDOSCOPY Typically, an endoscope has a channel through which the doctor can insert tools. These tools collect tissue or provide treatment. Types of tools include: 1.Flexible forceps: These tong-like tools take a tissue sample. 2.Biopsy forceps: These remove a tissue sample or a suspicious growth. 3.Cytology brushes: These take cell samples. 4.Suture removal forceps: These remove stitches inside the body
- 14. ENDOSCOPE CONSIST OF: An endoscope consists of the following: • A lighting system (to illuminate inner cavities); • An image transmission system (to send an image outside of the body by means of an objective lens which focuses it on aligned image guide fibers or a CCD) • Channels for air (to inflate the body cavity and for suction to remove fluids) and water (to wash the objective lens and to introduce biopsy forceps) • A bending mechanism to deflect the endoscope tip. • An Endoscopy monitor to display the examinations, surgical procedures.
- 17. SAFETY CONCERNS RELATED TO THE EQUIPMENT • Bite guard for the endoscopes • For the patient safety • The concerned endoscopes are Sterilized before insertion • Reprocessing
- 18. Reprocessing To ensure flexible endoscopes are safe for patient use, all staff involved in reprocessing this equipment must understand and consistently follow a number of steps which have been distilled down to seven essential steps. Ensuring adherence to these steps requires a complete and effective reprocessing program. These recommendations apply to all settings where endoscopic procedures are performed and where endoscopes are reprocessed.
- 19. Pre-Cleaning a. Pre-Clean flexible endoscopes and reusable accessories by following the device manufacturer’s instructions for use (IFU). Perform pre-cleaning immediately following completion of the endoscope procedure to help prevent the formation of biofilm. Leak-Testing a. For endoscopes that require leak testing, perform the leak test using manufacturer’s IFU after each use and prior to manual cleaning. Leak testing detects damage to the external surfaces and internal channels of the endoscope that can lead to inadequate disinfection and further damage of the endoscope. Manual Cleaning a. Perform meticulous manual cleaning including brushing and flushing channels and ports consistent with the manufacturer’s IFU before performing high-level disinfection (HLD) or sterilization. Perform manual cleaning within the timeframe specified in the manufacturer’s IFU. Manual cleaning is the most critical step in the disinfection process since residual organic material can reduce the effectiveness of HLD and sterilization.
- 20. Visual Inspection a. After manual cleaning, visually inspect the endoscope and its accessories. Visual inspection provides additional assurance that the endoscope and its accessories are clean and free of defects. Complex devices such as flexible endoscopes may require the use of lighted magnification or additional methods to assist with the inspection process. Disinfection or Sterilization a. Following cleaning and visual inspection perform HLD or sterilization in accordance with the manufacturer’s IFU. Carefully review and adhere to the endoscope manufacturer’s reprocessing instructions and to the IFU for chemicals or sterilants and any equipment (e.g., automated endoscope reprocessors) used for reprocessing to help ensure that effective disinfection occurs.
- 21. Storage a. After reprocessing is complete, store endoscopes and accessories in a manner that prevents recontamination, protects the equipment from damage, and promotes drying. Store processed flexible endoscopes in a cabinet that is either: i. of sufficient height, width, and depth to allow flexible endoscopes to hang vertically without coiling and without touching the bottom of the cabinet OR ii. designed and intended by the manufacturer for horizontal storage of flexible endoscopes. Documentation a. Maintain documentation of adherence to these essential steps each time an endoscope is reprocessed. Documentation is essential for quality assurance purposes and for patient tracing in the event a look back is necessary.
- 22. NEED OF THE EQUIPMENT TO THE SPECIFIC DEPARTMENT IN HOSPITAL Surgical gastroenterology Respiratory Medicine Gastroenterology Surgical Orthopedics
- 23. COST COMPARISON AND COMPANIES OUR HOSPITAL PURCHASES FROM • Olympus (40 lakh) • Stryker (35 lakh) • Karl Storz (35 lakh) • Smith & Nephew – Ortho (35-55 lakh)
- 24. ENDOSCOPE EQUIPMENT MAINTENANCE Proper Handling of Endoscope • Avoid touching the eyepiece lens or the objective lens to prevent contamination. Even the smallest dust or dirt or fingerprint may cause an undesirable image. Light Source and Monitor Maintenance • Light Source and Monitor Maintenance • Check the image quality on the display to ensure the camera is 100% dust or dirt free. The image or display should be clear, with no blurring, distortion or discoloration. • Perform a white balance test to ensure the clearest display.
- 25. SAFETY AND PRECAUTION • Calibration of the equipment • Leakage test • Bite guard is used to prevent any gag reflex by the patients to make sure there is no damage to the equipment. • Sterilizer- machine is put on the sterilizer for 60 minutes.
