CT angiography.pptx
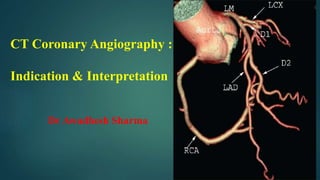
- 1. CT Coronary Angiography : Indication & Interpretation Dr Awadhesh Sharma
- 2. Indications of CTA in current scenario
- 5. Stable chest pain 1. No Known CAD: Appropriate as the first line test in stable typical or atypical chest pain, or other symptoms which are thought to represent a possible anginal equivalent (e.g. dyspnoea on exertion, jaw pain). After a nonconclusive functional test, in order to obtain more precision regarding diagnosis and prognosis, if such information will influence subsequent patient management. May be appropriate in some asymptomatic high-risk individuals, such as those with a higher likelihood of non-calcified plaque. Rarely appropriate in very low-risk symptomatic patients – those under age 40 with non- cardiac symptoms – or those with low- to intermediate-risk asymptomatic patients.
- 6. Indications.. 2. Known CAD: It is appropriate to perform CTA as a first line test for evaluating patients with known CAD who present with stable typical or atypical chest pain, or other symptoms which are thought to represent a possible anginal equivalent (e.g. dyspnea on exertion, jaw pain). 3. Functional imaging: It may be appropriate to perform CT derived FFR and CT myocardial perfusion Imaging to evaluate the functional significance of intermediate stenoses on CTA (30-70% diameter stenosis). Add FFRCT and stress-CTP to CTA to increase specificity, positive predictive value, and diagnostic accuracy. CTP can be a valuable alternative when CT-FFR is technically difficult.
- 7. Indications.. 4. Stable Coronary Artery Disease: CCTA Post-Revascularization In intra-coronary stent ≥ 3.0 mm, implementing measures to improve stent imaging accuracy, such as heart-rate control, iterative, sharp kernel, and mono-energetic reconstruction. CCTA is appropriate to evaluate patients with prior CABG, particularly for graft patency, and to visualize grafts and other structures prior to cardiac surgery re-do. Protocols to optimize stent imaging should be developed and followed. It may also be appropriate to perform coronary CTA in symptomatic patients with stents <3.0 mm, especially those known to have thin stent struts (<100 mm) in proximal, non-bifurcation locations.
- 8. Indications.. 5. Stable Coronary Artery Disease: CCTA in Other Conditions Asymptomatic high risk subjects: may be appropriate in selected asymptomatic high risk individuals, especially in those who have a higher likelihood of having a large amount of non-calcified plaque. Asymptomatic low or intermediate risk : rarely appropriate. Coronary artery bypass grafts : It is appropriate to perform CTA for evaluation of patients with prior CABG, particularly if graft patency is the primary objective.
- 9. Other Indications: CTA is appropriate for coronary artery evaluation before non-coronary cardiac surgery as an equivalent alternative to invasive angiography in patients with low- to-intermediate probability of CAD and younger patients with primarily non- degenerative valvular conditions. CTA is appropriate to exclude coronary artery disease in patients with suspected non-ischemic cardiomyopathy. Late enhancement CT imaging may be appropriate to pinpoint infiltrative heart disease or scar in some patients who have non-ischemic or ischemic cardiomyopathy who cannot undergo cardiac MRI.
- 10. CTA is appropriate for the evaluation of coronary anomalies. Limited delay image CTA (60 seconds-to-90 seconds) is appropriate alternative to TEE to exclude LA/LAA thrombus, as well as in patients where TEE-associated risks outweigh the benefits. Late enhancement CT imaging may be appropriate to evaluate myocardial viability in some patients who cannot undergo cardiac MRI if it has the potential to impact diagnosis and treatment.
- 11. Coronary anomalies (A) Three-dimensional multi-detector row computed tomography reconstruction of a right-sided single coronary artery with a pre- pulmonary course of the left main stem in a 42-year-old man. The left main coronary artery (black arrows) is originating from the proximal part of the right coronary artery (black arrowheads; left panel) than following a pre-pulmonary course to the anterior interventricular groove, where the left main coronary artery splits in the left anterior descending coronary angiography (LAD), an intermediate branch (RIM), and the circumflex coronary artery (RCX, right panel). Ao, ascending aorta; PA, pulmonary artery. (B) Transaxial multi-detector row computed tomography image of a right-sided single coronary artery with an interarterial path of the left main stem in a 64-year-old man. The left main coronary artery (white arrowheads) originates from the proximal part of the right coronary artery (black arrow) than following an interarterial path between the ascending aorta and the pulmonary trunk. The white arrows indicate the mid part of the circumflex coronary artery. Ao, ascending aorta; LA, left atrium; LV, left ventricle.
- 12. Implementation In Clinical Practice
- 13. 1. Medical versus Invasive Treatment A central aim of evaluation for CAD is to identify patients who need appropriate revascularization to improve prognosis or symptoms not responding to medical therapy, as well as those that can be managed with medical therapy alone. Stenosis severity still remains the primary arbiter of therapeutic decisions, but more and more data now suggest that anatomy coupled with a physiologic correlate is a better or even possibly, a necessary way for optimal decision-making.
- 14. 2. Role of CTA for guiding further non-invasive evaluation: CTA facilitates decision making by dividing patients into multiple informative categories. Those with a negative CTA or demonstration of non-obstructive CAD would generally exclude flow limiting CAD with high certainty and avoid downstream testing. CTA seems to allow for more appropriate use of statins and anti-platelet therapies better than when using non CTA methods for CAD diagnosis. CTA and FFRCT may allow for even more uniform down-stream interventions and narrow the differences between revascularization rates between men and women unlike what happens after usual stress testing imaging.
- 15. How to Interpret CTA
- 17. Anterior projection: Left Main or left coronary artery (LCA) Left anterior descending (LAD) diagonal branches (D1, D2) septal branches Circumflex (Cx) Marginal branches (M1,M2) Right coronary artery Acute marginal branch (AM) AV node branch Posterior descending artery (PDA)
- 19. RAO projection:
- 25. CAD-RADS: Cad-Rads is the Coronary Artery Disease-Reporting and Data System. It was published in 2016 by the Society of Cardiovascular Computed Tomography (SCCT), the American College of Radiology (ACR) and the North American Society for Cardiovascular Imaging (NASCI) and it has been endorsed by the American College of Cardiology (ACC) . Cad-Rads is developed to standardize reporting of coronary CTA, to improve communication and to guide therapy.
- 28. Post CABG ..
- 29. Vulnerable plaque… Vulnerable plaque features include: Low-attenuation plaque Positive remodeling Spotty calcification Napkin-ring sign If two or more of these features are present modifier “V” should be added to the CAD-RADS category.
- 30. Plaque Characteristics.. There are three plaque types on coronary CTA: Calcified- Atherosclerotic plaque in which the entire plaque appears as calcium density (>130 HU on non-enhanced CT). Partially calcified- Atherosclerotic lesion with 2 components of which one is calcification. Non-calcified- Plaque with no calcium content
- 31. Low-attenuation plaque- Lesions associated with plaque rupture frequently have a large lipid rich core. Lipid on CT appears as low attenuation. Plaques with <30 HU on CTA were found to be present significantly more often in patients with acute coronary syndrome
- 32. Positive remodelling- is defined as a compensatory outward enlargement of the vessel wall at the site of the atherosclerotic lesion with preservation of the coronary lumen. Higher lipid content and abundance of macrophages. Can present with an acute coronary syndrome without any prior cardiac history.
- 33. Spotty calcification- usually defined as calcifications < 3 mm . Small (< 1 mm), intermediate (1-3 mm) and large (> 3 mm) calcifications. Small spotty calcifications on CTA are associated with high-risk plaques.
- 34. Napkin-ring sign- high-risk plaque feature on CTA. It is defined as a central low-attenuation area adjacent to the coronary lumen and a higher “ring- like” attenuation tissue surrounding this central area.. On histology the area of low-attenuation corresponds to the large necrotic core, while the “ring- like” outer area correlates with fibrous plaque tissue. The Napkin-ring sign is strongly associated with major adverse cardiovascular events.
- 35. Fig. 2 (A1) Presence of positive remodeling (yellow arrows) and low attenuation plaques (LAP, red arrow) are the most important determinants of plaque vulnerability. (A2) Stable plaques lack both these features. (A3) Major adverse cardiac events by the presence of 1 or both features in a follow up of -- - patients for 2 years, and 300 patients for up to 10 years. (A4) Patients with HRP had 45 and 10 folds higher likelihood of adverse outcomes, respectively.
- 36. Presence of significant stenosis over and above HRP features (A5) and interval progression in plaque magnitude (A6) increased the likelihood of adverse events further. Greater number of adverse plaque characteristics were associated with greater of adverse outcomes (A7) and the HRP characteristics were associated with abnormal fractional flow reserve regardless of luminal stenosis (A8).
- 37. Imaging of coronary atherosclerotic plaque by multidetector row computed tomography. The contrast- enhanced multi-detector row computed tomography data set shows a noncalcified plaque in the proximal right coronary artery with substantial positive remodelling and only a mild associated reduction of the coronary lumen.
- 38. Case 1-
- 40. (a) Sixty-one year old man with vague chest pain, not typical for angina with normal treadmill. 3D- VR images clearly shows segment of significant stenosis in large diagonal branch. (b) The segment of stenosis, which was missed on initial reading of axial images as it is difficult to visualise well, until 3D-VR images were reviewed. (c) Segment of stenosis also clearly visible on a reconstructed 3D-MIP reconstructed to simulate LAO cranial angio view. (d) Lesion seen on corresponding angiogram view. Segment of stenosis was subsequently treated by PCI. Note the stenosis appears more severe on the 3D images, due to parameters used to create the images
- 41. (a) 58 year old man.16 MSCT scan. In this CPR image, a short segment of significant stenosis in the distal RCA, is clearly visible and there is associated non calcified plaque seen surrounding the contrast filled lumen (arrow). (b) The fibrous plaque in the lumen of the RCA is also well visualised on the axial image surrounding the contrast filled narrowed lumen (arrow). (c) At coronary angiography, the segment of stenosis is seen and corresponds to the CTCA findings
- 42. (a) 53 year old man with CTCA showing soft and calcified plaque in left main extending to bifurcation and proximal LAD. Could be easily misread as associated with significant stenosis by inexperienced reader. (b) Conventional angiography recommended because of segment of significant stenosis in mid LAD (not shown here). Coronary angiogram shows slight narrowing and tapering of lumen of distal left main segment but no significant segment of stenosis is identified (arrow). (c) Cross sectional image at orthogonal plane of contrast filled normal lumen of left main proximal to lesion in Fig. a (arrow). (d) Cross sectional image of lumen of distal left main at level of lesion in Fig. a showing soft and calcified plaques (arrowhead) and contrast filled lumen (arrow) with narrowing of less than 20% of its diameter.
- 43. A potential pitfall in the assessment of coronary artery stenosis is to mistake a motion artefact for a noncalcified plaque. This might particularly occur in coronary CTA datasets of reduced image quality. One should always check a second reconstruction time-point for the presence of any noncalcified plaque. If the plaque is seen only on one of the reconstruction time points, a motion artefact has to be expected mimicking the finding. Curved-planar reformations of the right coronary artery (RCA) at two different reconstruction time-points: At 75% of the R-R interval a noncalcified plaque in the distal RCA is suspected. Reviewing this area at 45% of the R-R interval shows no evidence of plaque, proving the “lesion” in diastole to be a motion artefact Motion Artifact
- 44. summary In general, CTA has the advantage of visualizing the stenosis and the atheromatous plaque as opposed to making an educated guess about its presence, as with physiologic testing. CTA has excellent sensitivity for identifying flow limiting disease and has very high negative predictive value, making it the strongest test to rule out flow limiting CAD, especially in patients with low to intermediate risk.
- 45. This Photo by Unknown Author is licensed under CC BY-SA
Editor's Notes
- Central Illustration Role of CTA in chronic CAD. Also please see Table 1.
- CT angiography for detection of high-risk plaques. (A1) Presence of positive remodeling (yellow arrows) and low attenuation plaques (LAP, red arrow) are the most important determinants of plaque vulnerability. (A2) Stable plaques lack both these features. Major adverse cardiac events by the presence of 1 or both features in a follow up of --- patients for 2 years (A3), and 300 patients for up to 10 years. (A4) Patients with HRP had 45 and 10 folds higher likelihood of adverse outcomes, respectively. Presence of significant stenosis over and above HRP features (A5) and interval progression in plaque magnitude (A6) increased the likelihood of adverse events further. Greater number of adverse plaque characteristics were associated with greater of adverse outcomes (A7) and the HRP characteristics were associated with abnormal fractional flow reserve regardless of luminal stenosis (A8). (B) Potential indicators of inflammation by CTA as a complementary feature for identification of plaque vulnerability. It can be detected either by simultaneous PET imaging with F-18 FDG (that targets macrophage infiltration) (A1 & A2), or by fat attenuation index of perivascular fat (that represents lower prevalence of adipocytes consequent to greater cytokines in neointima) (A3 & A4). Modified from Motoyama et al. JACC 2007, Motoyama et al. JACC 2009, Lee et al. JACC 2019 Ahmadi et al. JACC-Imaging 2018, Rogers et al. JACC-Imaging 2010, Antoniades et al. Lancet 2018.
- CT angiography for detection of high-risk plaques. (A1) Presence of positive remodeling (yellow arrows) and low attenuation plaques (LAP, red arrow) are the most important determinants of plaque vulnerability. (A2) Stable plaques lack both these features. Major adverse cardiac events by the presence of 1 or both features in a follow up of --- patients for 2 years (A3), and 300 patients for up to 10 years. (A4) Patients with HRP had 45 and 10 folds higher likelihood of adverse outcomes, respectively. Presence of significant stenosis over and above HRP features (A5) and interval progression in plaque magnitude (A6) increased the likelihood of adverse events further. Greater number of adverse plaque characteristics were associated with greater of adverse outcomes (A7) and the HRP characteristics were associated with abnormal fractional flow reserve regardless of luminal stenosis (A8). (B) Potential indicators of inflammation by CTA as a complementary feature for identification of plaque vulnerability. It can be detected either by simultaneous PET imaging with F-18 FDG (that targets macrophage infiltration) (A1 & A2), or by fat attenuation index of perivascular fat (that represents lower prevalence of adipocytes consequent to greater cytokines in neointima) (A3 & A4). Modified from Motoyama et al. JACC 2007, Motoyama et al. JACC 2009, Lee et al. JACC 2019 Ahmadi et al. JACC-Imaging 2018, Rogers et al. JACC-Imaging 2010, Antoniades et al. Lancet 2018.
- On average, the CT attenuation within ‘fibrous’ plaques is higher than within ‘lipid-rich’ plaques (mean attenuation values of 91–116 vs. 47–71 HU)
- One should always compare ‘‘lumen to lumen’’, the contrast filled lumen with the lesion to the normal lumen proximal or distal to the lesion, rather than compare ‘‘wall to wall’’ as this will lead to overestimation of the stenosis, especially if there is positive remodelling
