Abdominal tb
•Download as PPTX, PDF•
2 likes•346 views
ALL YOU KNOW ABOUT ABDOMINAL KOCH'S
Report
Share
Report
Share
Recommended
More Related Content
What's hot
What's hot (20)
3. Sexually transmitted diseases (st ds) Dr. Mahadi Hassan

3. Sexually transmitted diseases (st ds) Dr. Mahadi Hassan
Similar to Abdominal tb
Similar to Abdominal tb (20)
GASTROINTESTINAL TUBERCULOSIS ABDOMINAL TUBERCULOSIS

GASTROINTESTINAL TUBERCULOSIS ABDOMINAL TUBERCULOSIS
More from anwaradil4
More from anwaradil4 (13)
Recently uploaded
Independent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for Real Meet
WHATSAPP On Here: 9352988975
Today call girl service available 24X7*▬█⓿▀█▀ 𝐈𝐍𝐃𝐄𝐏𝐄𝐍𝐃𝐄𝐍𝐓 CALL 𝐆𝐈𝐑𝐋 𝐕𝐈𝐏 𝐄𝐒𝐂𝐎𝐑𝐓 SERVICE ✅
⭐➡️HOT & SEXY MODELS // COLLEGE GIRLS
AVAILABLE FOR COMPLETE ENJOYMENT WITH HIGH PROFILE INDIAN MODEL AVAILABLE HOTEL & HOME
★ SAFE AND SECURE HIGH CLASS SERVICE AFFORDABLE RATE
★ 100% SATISFACTION,UNLIMITED ENJOYMENT.
★ All Meetings are confidential and no information is provided to any one at any cost.
★ EXCLUSIVE PROFILes Are Safe and Consensual with Most Limits Respected
★ Service Available In: - HOME & HOTEL 24x7 :: 3 * 5 *7 *Star Hotel Service .In Call & Out call SeRvIcEs :
★ A-Level (5 star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)Receive advanced sexual techniques in different mode make their life more pleasurable #G05.
★ Spending time in hotel rooms
★ BJ (Blowjob Without a Condom)
★ Completion (Oral to completion)
★ Covered (Covered blowjob Without condom
100% SAFE AND SECURE 24 HOURS SERVICE AVAILABLE HOME AND HOTEL SERVICESIndependent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for R...

Independent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for R...Ahmedabad Call Girls
(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The Service Of A Mumbai Call Girl At Any Time
WHATSAPP On Here:9920725232
Today call girl service available 24X7*▬█⓿▀█▀ 𝐈𝐍𝐃𝐄𝐏𝐄𝐍𝐃𝐄𝐍𝐓 CALL 𝐆𝐈𝐑𝐋 𝐕𝐈𝐏 𝐄𝐒𝐂𝐎𝐑𝐓 SERVICE ✅
⭐➡️HOT & SEXY MODELS // COLLEGE GIRLS
AVAILABLE FOR COMPLETE ENJOYMENT WITH HIGH PROFILE INDIAN MODEL AVAILABLE HOTEL & HOME
★ SAFE AND SECURE HIGH CLASS SERVICE AFFORDABLE RATE
★ 100% SATISFACTION,UNLIMITED ENJOYMENT.
★ >> 03-05-2024 (GRV)
★ All Meetings are confidential and no information is provided to any one at any cost.
★ EXCLUSIVE PROFILes Are Safe and Consensual with Most Limits Respected
★ Service Available In: - HOME & HOTEL 24x7 :: 3 * 5 *7 *Star Hotel Service .In Call & Out call SeRvIcEs :
★ A-Level (5 star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)Receive advanced sexual techniques in different mode make their life more pleasurable.
★ Spending time in hotel rooms
★ BJ (Blowjob Without a Condom)
★ Completion (Oral to completion)
★ Covered (Covered blowjob Without condom
100% SAFE AND SECURE 24 HOURS SERVICE AVAILABLE HOME AND HOTEL SERVICES(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The S...

(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The S...Ahmedabad Call Girls
Recently uploaded (20)
💚 Punjabi Call Girls In Chandigarh 💯Lucky 🔝8868886958🔝Call Girl In Chandigarh

💚 Punjabi Call Girls In Chandigarh 💯Lucky 🔝8868886958🔝Call Girl In Chandigarh
VIP Call Girls Noida Jhanvi 9711199171 Best VIP Call Girls Near Me

VIP Call Girls Noida Jhanvi 9711199171 Best VIP Call Girls Near Me
VIP Call Girls Noida Sia 9711199171 High Class Call Girl Near Me

VIP Call Girls Noida Sia 9711199171 High Class Call Girl Near Me
ooty Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

ooty Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Call Girl Gorakhpur * 8250192130 Service starts from just ₹9999 ✅

Call Girl Gorakhpur * 8250192130 Service starts from just ₹9999 ✅
Jaipur Call Girls 9257276172 Call Girl in Jaipur Rajasthan

Jaipur Call Girls 9257276172 Call Girl in Jaipur Rajasthan
bhopal Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

bhopal Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Mangalore Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Mangalore Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
raisen Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

raisen Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Sambalpur Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Sambalpur Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Call Girl in Bangalore 9632137771 {LowPrice} ❤️ (Navya) Bangalore Call Girls ...

Call Girl in Bangalore 9632137771 {LowPrice} ❤️ (Navya) Bangalore Call Girls ...
Russian Call Girls in Noida Pallavi 9711199171 High Class Call Girl Near Me

Russian Call Girls in Noida Pallavi 9711199171 High Class Call Girl Near Me
Independent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for R...

Independent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for R...
palanpur Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

palanpur Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The S...

(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The S...
Russian Call Girls Kota * 8250192130 Service starts from just ₹9999 ✅

Russian Call Girls Kota * 8250192130 Service starts from just ₹9999 ✅
Vip Call Girls Makarba 👙 6367187148 👙 Genuine WhatsApp Number for Real Meet

Vip Call Girls Makarba 👙 6367187148 👙 Genuine WhatsApp Number for Real Meet
Call Girls Service Anantapur 📲 6297143586 Book Now VIP Call Girls in Anantapur

Call Girls Service Anantapur 📲 6297143586 Book Now VIP Call Girls in Anantapur
neemuch Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

neemuch Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Call Girls in Udaipur Girija Udaipur Call Girl ✔ VQRWTO ❤️ 100% offer with...

Call Girls in Udaipur Girija Udaipur Call Girl ✔ VQRWTO ❤️ 100% offer with...
Abdominal tb
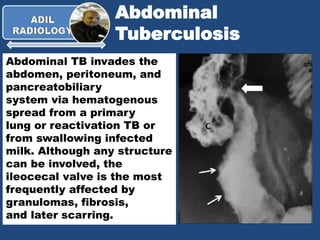
- 1. Abdominal Tuberculosis Abdominal TB invades the abdomen, peritoneum, and pancreatobiliary system via hematogenous spread from a primary lung or reactivation TB or from swallowing infected milk. Although any structure can be involved, the ileocecal valve is the most frequently affected by granulomas, fibrosis, and later scarring.
- 2. Abdominal Tuberculosis TB peritonitis may develop causing ascites and omental and peritoneal thickening. TB peritonitis is divided into three forms: wet, fibrotic, and dry. Wet peritonitis is characterized by a large amount of viscous ascetic fluid (90 % of cases). Fibrotic peritonitis is characterized by large omental masses and intestinal adhesions, causing the omentum to form a hard mass on palpation. Dry or plastic peritonitis is characterized by fibrous peritoneal reaction, dens adhesions, and caseous nodules.
- 3. Abdominal Tuberculosis Thickened peritoneum may be seen as a tiny nodules or a thick nodular line surrounding the viscera beneath the abdominal walls, with marked enhancement after contrast injection.
- 4. Abdominal Tuberculosis Irregular or focal omental thickening (omental cake sign ).
- 5. Abdominal Tuberculosis TB ascitic fluid with septations is seen in 30–100 % of cases. The fluid typically has attenuation between 25 and 45 HU, which may reflect its exudative nature.
- 6. Abdominal Tuberculosis Retroperitoneal (e.g., para-aortic) node enlargement.
- 7. Abdominal Tuberculosis Intestinal adhesions are identified on CT as intestinal loops sticking to the abdominal wall.
- 8. Abdominal Tuberculosis In Bauhin ’s ileocecal valve syndrome , the CT show hypertrophic ileocecal valve with dilated small bowel loops proximally. The absence of abnormal contrast enhancement, pathologic intestinal manifestations, and ileocecal mass are supportive signs that assist in establishing the diagnosis. Definite diagnosis requires colonic biopsy that typically shows hypertrophic muscularis layer with absence of inflammatory or malignant changes.