Valvular disorders
- 1. Nursing management of patients with cardiovascular disorders • Prepared By • Dr. Zuhair Rushdi Mustafa • Lecturer at University of Duhok/ College of Nursing
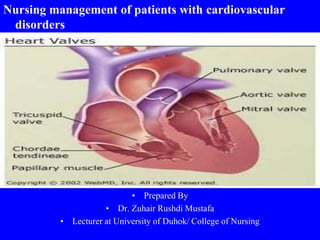
- 2. VALVULAR DISORDERS The valves of the heart control the flow of blood through the heart into the pulmonary artery and aorta by opening and closing through heart contraction and relaxing through the cardiac cycle. The valves of the heart (aortic , tricuspid, and mitral) in the closed position.
- 4. Tricuspid valve separates the right atrium from the right ventricle, and the mitral valve separates the left atrium from the left ventricle. pulmonic valve Aortic valve
- 5. Disorders of the mitral valve fall into the following categories: 1. mitral valve prolapse (ie, stretching of the valve leaflet into the atrium during systole) 2. Mitral stenosis. 3. Mitral regurgitation These valvular disorders may require surgical repair or replacement of the valve to correct the problem, depending on severity of symptoms.
- 6. Mitral Valve Prolapse _is a deformity that usually produces no symptoms. _Rarely, it progresses and can result in sudden death. _This condition occurs more frequently in women than in men. The cause is usually an inherited connective tissue
- 7. Pathophysiology _In mitral valve prolapse, a portion of one or both mitral valve leaflets balloons back into the atrium during systole. _Blood then regurgitates from the left ventricle back into the left atrium.
- 8. Clinical Manifestations _Most people never have symptoms. _A few have symptoms of: 1. Fatigue 2. shortness of breath 3. Dizziness 4. Syncope 5. Palpitations 6. chest pain 7. anxiety.
- 9. Assessment and Diagnostic Findings 1. a murmur of mitral regurgitation may be heard. 2. A few patients experience signs and symptoms of heart failure. 3. Echocardiography may be used to diagnose and monitor the progression of mitral valve prolapse.
- 10. Medical Management Medical management is directed at controlling symptoms. 1. Most patients do not require any medications. 2. If dysrhythmias occur, the patient is advised to eliminate caffeine and alcohol from the diet and to stop smoking. 3. antiarrhythmic medications may be prescribed (Verapamil, Amiodaron, Adenosine).
- 11. 4. Chest pain that does not respond to nitrates may respond to calcium channel blockers (Diltiazem, amlodepine) or beta-blockers (Propranolol, Atenolol). 5. In advanced stages of disease, Surgical intervention consists of mitral valvuloplasty (ie, surgical repair of the valve) or valve replacement may be necessary. valve replacement
- 12. Nursing Management 1. The nurse educates the patient about the diagnosis and the possibility that the condition is hereditary. Parents and siblings may be advised to have echocardiograms. 2. Patients may be at risk for infectious endocarditis The nurse teaches the patient how to minimize this risk by: a. practicing good oral hygiene b. obtaining routine dental care c. Avoid using toothpicks or other sharp objects in the oral cavity.
- 13. 3. To minimize symptoms, the nurse teaches the patient to avoid caffeine and alcohol. 4. The nurse also give advices regarding diet, activity, sleep, and other lifestyle factors that may correlate with symptoms.
- 14. Mitral Stenosis Mitral stenosis is an obstruction of blood flowing from the left atrium into the left ventricle. • _It is most often caused by rheumatic endocarditis, which progressively thickens the mitral valve leaflets. • The leaflets often fuse together. Eventually, the mitral valve orifice narrows and progressively obstructs blood flow into the ventricle.
- 15. Mitral Stenosis: Pathophysiology Source Undetermined
- 16. • Clinical Manifestations 1. Dyspnea on exertion as a result of pulmonary venous hypertension. 2. fatigue. 3. The enlarged left atrium may create pressure on the left bronchial tree, resulting in a dry cough or wheezing. 4. Patients may expectorate blood (ie, hemoptysis) or experience palpitations, orthopnea, paroxysmal nocturnal dyspnea (PND), and repeated respiratory infections.
- 17. Assessment and Diagnostic Findings 1. The pulse is weak and often irregular. 2. diastolic murmur is heard at the apex. 3. As a result of the increased blood volume and pressure, the atrium dilates, hypertrophies, and becomes electrically unstable, and patients experience atrial dysrhythmias. 4. Echocardiography is used to diagnose mitral stenosis. 5. Electrocardiography (ECG) and cardiac catheterization may be used to help determine the severity of the mitral stenosis.
- 18. Echocardiography: Short Axis Normal Mitral Stenosis Source Undetermined Source Undetermined
- 19. Medical Management 1. Anticoagulants to decrease the risk for developing atrial thrombus. 2. Treatment of anemia. 3. Patients are advised to avoid tiring activities and competitive sports, both of which increase the heart rate. 4. Surgical intervention consists of: 1. Open surgical commissurotomy to open or rupture the fused commissures of the mitral valve. 2. Mitral valve replacement may be performed. 3. Balloon mitral commissurotomy
- 21. Mitral Regurgitation _Mitral regurgitation involves blood flowing back from the left ventricle into the left atrium during systole. The leaflets cannot close completely because the leaflets have thickened and fibrosed.
- 22. Causes of Mitral Regurgitation : • mitral valve prolapse • ischemia of the left ventricle • rheumatic heart disease . • infective endocarditis, • annular calcification • cardiomyopathy • ischemic heart disease
- 23. Clinical Manifestations Chronic mitral regurgitation is often asymptomatic, but acute mitral regurgitation (eg, that resulting from a myocardial infarction) usually manifests as severe congestive heart failure. 1. Dyspnea 2. Fatigue 3. weakness are the most common symptoms. 4. Palpitations 5. shortness of breath on exertion 6. cough.
- 24. Assessment and Diagnostic Findings 1. A systolic murmur is heard. 2. Echocardiography is used to diagnose and monitor the progression of mitral regurgitation. 4. C-XR: LA and LV enlargement XR: LA and LV enlargement
- 25. Medical Management 1. Management is the same as that for heart failure 2. Reduction (arterial dilation) by treatment with angiotensin-converting enzyme (ACE) inhibitors (Vasodilators) , such as captopril (Capoten), enalapril (Vasotec), lisinopril (Prinivil, Zestril), ramipril (Altace), or hydralazine (Apresoline). 3. Angiotensin receptor blockers (ARBs), such as losartan (Cozar) or valsartan (Diovan). 4. beta-blockers, such as carvedilol (Coreg). 5. Digoxin For Arterial Fibrilation 6. Antibiotic Prophylaxis against Infective
- 26. 7. Once symptoms of heart failure develop, the patient needs to restrict his or her activity level to minimize symptoms. 8. Surgical intervention consists of mitral valvuloplasty (ie, surgical repair of the valve) or valve replacement. Prosthetic valve in place at the completion of the procedure
- 29. Nursing Management: Valvular Heart Disorders The nurse teaches the patients about: 1. the diagnosis, the progressive nature of valvular heart disease, and the treatment plan. 2. medication schedule and teaches about the name, dosage, actions, adverse effects, and any interactions of the prescribed medications for heart failure, dysrhythmias, angina pectoris, or other symptoms. 3. Rest and relaxation.
- 30. 4. Instruct the patient to check weigh daily and report gains of 1 kg in 1 day or 2.5 Kg in 1 week to the health care provider 5. The nurse measures the patient’s vital sings and compares results with previous data, and notes any changes. 6. The nurse auscultate heart and lung sounds and palpate peripheral pulses. 7. The nurse also take care of patients treated with valvuloplasty or surgical valve replacement.