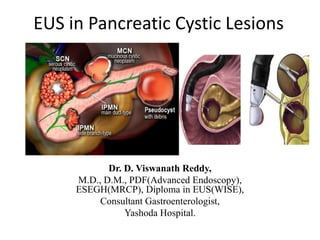
EUS in Pancreatic cystic lesions.pptx
- 1. EUS in Pancreatic Cystic Lesions Dr. D. Viswanath Reddy, M.D., D.M., PDF(Advanced Endoscopy), ESEGH(MRCP), Diploma in EUS(WISE), Consultant Gastroenterologist, Yashoda Hospital.
- 2. Synopsis • PCLs – Magnitude, Types • Challenge: Benign or Malignant!, Surgery? • Radiology • EUS-Diagnosis of PCLs • Newer tools • EUS in Therapy of PCLs • Case snippets
- 3. PCLs • 2–45% of general population(24% Autopsy) • Reported prevalence 2.1–2.6% for CT & 13.5–45% for MRI/MRCP. • Age, Asians, Pancreatitis, Family history.... • Incidental, Asym., benign malignant. • Earlier 40% resection was of benign, still ~15-20% • Early detection paramount for early treatment.
- 6. • 45 year old ethanol consumer presented with acute abdominal pain 4 weeks back with SIRS recovered and now has persistent pain.
- 7. Pseudocyst • 20%-49% • 5th decade • 7:3 Body/tail > Head/uncinate • Well-defined • Peripancreatic fluid collection of homogenously low attenuation
- 9. Case: 50 year old female, nonalcoholic, nonsmoker with pain abdomen, jaundice or weight loss. Lap. Chole. done considering Biliary Pancreatitis. Collection considered as Pseudocyst. • Well-defined, unilocular/ • Macrolacunae • Mural Nodule/mass
- 10. Mucinous Cystadenoma • 11-18% • 5th decade • 1:9 M:F • Body/tail > head/uncinate • Well-defined, unilocular/ • Macrolacunae • Peripheral rim of calcification • CEA >192; String Sign; Cytology • High malignant potential
- 11. Serous cystadenoma • 13-23% • 6th decade • 4:6 M:F • Head/uncinate = body/tail • Well-defined • Small cysts separated by delicate septa • Central stellate scar with sunburst pattern of calcification • CEA<5; Amylase-low • Low malignancy potential
- 13. MD-IPMN • 21-33% • 7th decade • 6:4 M:F • Head/uncinate > body/tail • Distended pancreatic duct • Polypoid intraductal lesion • Patulous ampulla with mucin extrusion • CEA>192; String Sign • High malignancy potential 60 year old male presented with pain abdomen s/o Acute pancreatitis.
- 14. BD-IPMN
- 15. SPEN • 2% • 3rd decade • 1:9 M:F • Body/tail > head/uncinate • Well-defined • Heterogeneous-appearing mass with solid and cystic areas • High malignancy potential
- 16. Cystic PNET • 4-7% • 6th decade • 5:5 M:F • Body/tail > Head/uncinate • Well-defined • Heterogeneous-appearing mass • with solid and cystic areas • Hypervascular cyst rim
- 18. EUS- Mural Nodule vs Mucus Plug • Mucus – hypoechoic & smooth, hyperechoic rim • Nodules - iso- or hyperechoic without hyperechoic rim or smooth edge • Rotating patient & try move lesion with FNA needle can help to differentiate mucus vs nodule. • CH-EUS enhancement in nodule, not if mucus. • The sensitivity and specificity of EUS (75% and 83%) were superior to CT (24% and 100%) for nodules, and surpasses diagnostic yield of MRI
- 19. Current Diagnostic Approach • History • Initially- Non-invasive imaging-CT/MRI • EUS – Fluid analysis- Biomarkers, cytology. – Biopsy – Molecular analysis
- 20. Radiology • Combining MDCT and MRI, the accuracy of predicting malignancy of a PCL increased from 61% (CT) to 81% • Accuracy for identifying the specific type of PCN is between 40% - 95% for MRI/MRCP and between 40% and 81% for CT • MRI/MRCP is preferable – Better to evaluate septa, nodules, – Main duct, branch duct involvement, communication with MPD and – Cyst contents/debris; 79%-82% accurate in identifying mucinous cysts. • 18-FDG PET/CT had sensitivity of 57–94%, specificity of 65– 97% and accuracy of 94% in benign vs malignant cysts. European evidence-based guidelines on pancreatic cystic neoplasms; Gut. 2018 May; 67(5): 789–804. 10.1136/gutjnl-2018- 316027 Kadiyala V, Lee LS. Endosonography 24in the diagnosis and management of pancreatic cysts. World J Gastrointest Endosc 2015; 7(3): 213-223 [PMID: 25789091 DOI: 10.4253/wjge.v7.i3.213]
- 21. EUS scores over Radiology • EUS is recommended as an adjunct to other imaging modalities (GRADE 2C) • EUS with or without cyst fluid aspirate analysis more sensitive (76%) than CT or MRI (48% and 34%) differentiating neoplastic vs non- neoplastic cysts. Khashab MA et al. Should we do EUS/FNA on patients with pancreatic cysts? The incremental diagnostic yield of EUS over CT/MRI for prediction of cystic neoplasms. Pancreas. 2013;42:717- 721.
- 22. Glucose level(<50mg%) in PCF is better than CEA(94 vs 85%) for preoperative diagnosis of mucinous cysts. McCarty T.R., Garg R., Rustagi T. Pancreatic cyst fluid glucose in differentiating mucinous from nonmucinous pancreatic cysts: A systematic review and meta-analysis. Gastrointest. Endosc. 2021
- 23. EUS-FNA • EUS-FNA should only be performed if change in management expected(GRADE 2C). • No - if diagnosis is established by imaging, or where clear indication for surgery (GRADE 2C). • Relative contraindications-distance of >10 mm • EUS-FNA for PCN is safe procedure with relatively low risk (3.4%) of complications.
- 24. Antibiotic before FNA of PCL? • One retrospective study of 253 patients found antibiotic prophylaxis had no effect on risk of infection (7% vs 9.3%), although conclusive evidence is lacking. • Current practice is single shot antibiotic treatment prior to EUS-FNA of a cystic lesion.
- 25. Newer tools • Contrast EUS – Mural Nodules, – Assess vascularity in cyst & septa – Sonazoid>Sonovue -EUS-FNA of pancreatic cysts sensitivity 54% for mucinous versus non-mucinous cysts, - 44% - 78% when more passes from solid component. - 84.2% sensitivity when CH-EUS-FNA from fluid analysis & mural nodules.
- 26. Other tools • Moray Forceps – cyst tissue acquisition yield 90% – 83.7–88.6% sensitivity and 81.8–94.7% specificity for mucinous PCN – adverse events was 8.6–9.9% • Confocal Laser endocytoscopy(nCLE) • Molecular analysis(NGS): 4mutations: – KRAS, GNAS, VHL and one other (PIK3CA, TP53, SMAD4, PTEN, CDKN2A) • Artificial Intelligence – Imaging – EUS – Fluid analysis
- 29. EUS guided Therapy for PCLs • ?Alternative to surgery in poor / reluctant surgical candidates and low-risk in cases where malignant potential is uncertain. • Ethanol lavage • Paclitaxel stabilizes microtubule polymer to inhibit its disassembly & induce apoptosis. • RFA • Cryotherapy • Benign with no malignant features, 2-4 cm, uni/oligolocular, and no connection with MPD. • Post procedure pain, Pancreatitis, intracyst bleed, infection, Peritonitis. • EUS-guided therapies for IPMNs should not be performed outside trials.
- 31. Current Guidelines on PCLs
- 33. Summary • Increasing prevalence of PCLs recently. • Accurate diagnosis & risk stratifying paramount. • Multimodal diagnosis, EUS complementary. • EUS scores higher with FNA, Biopsy. • Fluid biomarkers and Molecular testing key • Newer tools promising. • F/U- No-surveillance, Surveillance or Surgery. • Therapeutic role of EUS in PCLs needs evidence.
- 34. Thank You