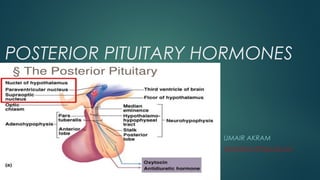
Posterior Pituitary
- 2. INTRODUCTION The pituitary gland, or hypophysis, is an endocrine gland about the size of a pea and weighing 0.5 grams (0.018 oz) in humans. It is a protrusion off the bottom of the hypothalamus at the base of the brain. The hypophysis rests upon the hypophysial fossa of the sphenoid bone in the center of the middle cranial fossa and is surrounded by a small bony cavity (sella turcica) covered by a dural fold (diaphragma sellae). The posterior pituitary (or neurohypophysis) is a lobe of the gland that is functionally connected to the hypothalamus by the median eminence via a small tube called the pituitary stalk (also called the infundibular stalk or the infundibulum). The posterior lobe develops as an extension of the hypothalamus. The Posterior pituitary hormones are synthesized by cell bodies in the hypothalamus. The magnocellular neurosecretory cells of the supraoptic and paraventricular nuclei located in the hypothalamus that project axons down the infundibulum to terminals in the posterior pituitary. This simple arrangement differs sharply from that of the adjacent anterior pituitary, which does not develop from the hypothalamus.
- 3. SECRETION The posterior pituitary stores and secretes (but does not synthesize) the following important endocrine hormones: •Antidiuretic hormone (ADH, also known as vasopressin and arginine vasopressin AVP), the majority of which is released from the supraoptic nucleus in the hypothalamus. •Oxytocin, most of which is released from the paraventricular nucleus in the hypothalamus. Oxytocin is one of the few hormones to create a positive feedback loop. For example, uterine contractions stimulate the release of oxytocin from the posterior pituitary, which, in turn, increases uterine contractions. This positive feedback loop continues throughout labour. •Both hormones are polypeptide, each having 9 amino acids. •Transported from site of synthesis to posterior pituitary via 'Hypothalmo- Hypophysial Tract' with carrier protein called neurophysin. •
- 4. ANTIDIURETIC HORMONE(ADH) ADH or Arginine vasopressin(AVP) is produced mainly in supraoptic nucleiof hypothalamus. ADH works by activating 2 second messenger systems 1-cAMP 2-IP3/Calcium Its two primary functions are to retain water in the body and to constrict blood vessels Vasopressin is a peptide hormone that increases water permeability of the kidney's collecting duct and distal convoluted tubule by inducing translocation of aquaporin-CD water channels in the plasma membrane of collecting duct cells. It also increases peripheral vascular resistance, which in turn increases arterial bloo pressure. It plays a key role in homeostasis, by the regulation of water, glucose, and salts in the blood. It has a very short half-life between 16–24 minutes.
- 5. ACTION OF ADH Vasopressin has three main effects: 1.Increasing the water permeability of distal convoluted tubule and collecting duct cells in the kidney, thus allowing water reabsorption and excretion of more concentrated urine, i.e., antidiuresis. This occurs through increased transcription and insertion of water channels (Aquaporin-2) into the apical membrane of distal convoluted tubule and collecting duct epithelial cells. Aquaporins allow water to move down their osmotic gradient and out of the nephron, increasing the amount of water re-absorbed from the filtrate (forming urine) back into the bloodstream. This effect is mediated by V2 receptors. Vasopressin also increases the concentration of calcium in the collecting duct cells, by episodic release from intracellular stores. Vasopressin, acting through cAMP, also increases transcription of the aquaporin-2 gene, thus increasing the total number of aquaporin-2 molecules in collecting duct cells. 2.Increasing permeability of the inner medullary portion of the collecting duct to urea by regulating the cell surface expression of urea transporters, which facilitates its reabsorption into the medullary interstitium as it travels down the concentration gradient created by removing water from the connecting tubule, cortical collecting duct, and outer medullary collecting duct. 3.Acute increase of sodium absorption across the ascending loop of henle. This adds to the countercurrent multiplication which aids in proper water reabsorption later in the distal tubule and collecting duct.
- 6. REGULATION • Ethanol (alcohol) reduces the calcium- dependent secretion of AVP by blocking voltage-gated calcium channels in neurohypophyseal nerve terminals in rats. • Angiotensin II stimulates AVP secretion, in keeping with its general pressor and pro- volumic effects on the body. • Atrial natriuretic peptide inhibits AVP secretion, in part by inhibiting Angiotensin II-induced stimulation of AVP secretion. • Cortisol inhibits secretion of antidiuretic hormone.
- 7. DISORDERS Decreased AVP release (neurogenic — i.e. due to alcohol intoxication or tumour) or decreased renal sensitivity to AVP (nephrogenic, i.e. by mutation of V2 receptor or AQP) leads to diabetes insipidus, a condition featuring hypernatremia (increased blood sodium concentration), polyuria (excess urine production), and polydipsia (thirst). Syndrome of inappropriate antidiuretic hormone secretion (SIADH) is characterized by excessive release of antidiuretic hormone from the posterior pituitary gland or another source. The increase in blood volume (hypervolemia) often results in true hyponatremia in which the plasma sodium levels are lowered and total body fluid is increased. Although the sodium level is low, SIADH is brought about by an excess of water rather than a deficit of sodium.
- 8. OXYTOCIN Produced mainly in paraventricular nucleus of hypothalamus. is a peptide hormone and neuropeptide. It plays a role in social bonding, sexual reproduction in both sexes, and during and after childbirth. Oxytocin is released into the bloodstream as a hormone in response to stretching of the cervixand uterus during labor and with stimulation of the nipples from breastfeeding. Oxytocin is also used as a medication to facilitate childbirth Half life of 2-3 minutes.
- 9. ACTION OF OXYTOCIN • Milk ejection reflex/Letdown reflex: In lactating (breastfeeding) mothers, oxytocin acts at the mammary glands, causing milk to be 'let down' into subareolar sinuses, from where it can be excreted via the nipple.In males it inceases ejaculation. • Uterine contraction: Important for cervical dilation before birth, oxytocin causes contractions during the second and third stages of labor.[47] Oxytocin release during breastfeedingcauses mild but often painful contractions during the first few weeks of lactation. • Cardiac effects: Oxytocin and oxytocin receptors are also found in the heart in some rodents, and the hormone may play a role in the embryonal development of the heart by promoting cardiomyocyte differentiation. • Oxytocin, under certain circumstances, indirectly inhibits release of adrenocorticotropic hormone and cortisol and, in those situations, may be considered an antagonist of vasopressin. • Crossing the placenta, maternal oxytocin reaches the fetal brain and induces a switch in the action of neurotransmitter GABA from excitatory to inhibitory on fetal cortical neurons. This silences the fetal brain for the period of delivery and reduces its vulnerability to hypoxic damage.[ • Plays important role in emotional bonding between humans.