clubfoot ppt.pptx
- 1. NASIR AHMAD (M.Sc. NURSING 2nd YEAR SPECIALITY: CHILD HEALTH NURSING
- 2. CONGENITAL TALIPES EQUINOVARUS (CTEV) commonly known as Clubfoot is one of the most common congenital musculoskeletal deformity among newborns. Although it is called congenital, it is not an embryonic malformation but is developmental deformation occurring during 2nd trimester.
- 3. CTEV or Club foot describes a range of foot abnormalities usually present at birth (congenital) in which the baby’s foot is twisted out of shape or position. In clubfoot the tissues connecting the muscles to the bone (tendons) are shorter than usual. Clubfoot is a fairly common birth defect and is usually an isolated problem for an otherwise healthy newborn.
- 4. Incidence of CTEV is 1 per 1000, making it the fifth most common congenital malformation after cardiovascular anomalies (9 per 1000) hypospadiasis (3.4 per 1000) urinary tract malformations (2.4 per 1000) & Down’s Syndrome (1.5 per 1000). Greater incidence is found in male babies as compared to the female babies.
- 5. GENDER- males are twice as likely as females to be born with club foot. GENETICS- if a parent who was born with club foot, they have a higher chance of having a child with the same condition. The risk is higher if both parents have the condition.
- 6. The clubfoot is mainly idiopathic, the genetic factors are believed to play a major role and some specific gene changes have been associated with it, but this is not yet well understood. It appears to be passed down through families. It is not caused by the fetus’ position in the uterus. Sometimes it may be linked to other skeletal abnormalities, such as spina bifida cystic, or a developmental hip condition known as hip dysplasia or developmental dysplasia of the hip (DHH). It may be due to a disruption in a neuromuscular pathway, possibly in the brain, the spinal cord, a nerve or a muscle.
- 7. Environmental factors may play a role. Research has found a link between the incidence of club foot and maternal age, as well as whether the mother smokes cigarettes and if she has diabetes. A link has also been noted between chance of clubfoot and early amniocentesis that is before 13 weeks of gestation during pregnancy. Oligohydramnios Amniotic Band Syndrome and congenital constriction rings. Increased occurrences in those children with neuromuscular disorders, such as cerebral palsy and spina bifida.
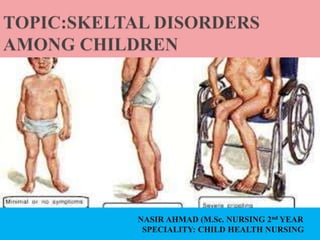
- 8. The top of the foot is usually twisted downward and inward, increasing the arch and turning the heel inward. The foot may be turned so severely that it actually looks as if it’s upside down. The affected leg or foot may be slightly shorter. The calf muscles in the affected leg are usually underdeveloped. Despite its look, clubfoot itself does not cause any discomfort or pain. But the difficulty in walking. In fact the Achilles tendon is too short.
- 9. IDIOPATHIC CLUBFOOT: Also known as talipes equinovirus, idiopathic club foot is the most common type of clubfoot and is present at birth. This congenital anomaly is seen in one out of every 1000 babies, with half of the cases of clubfoot involving only one foot. There is currently no known cause of idiopathic clubfoot, but baby boys are twice as likely to have clubfoot compared to baby girls. Neurogenic Clubfoot Neurogenic clubfoot is caused by an underlying neurologic condition. For instance, a child born with spina bifida A clubfoot may also develop later in childhood due to cerebral palsy or a spinal cord compression.
- 10. Syndromic Clubfoot Syndromic clubfoot is found along with a number of other clinical conditions, which relate to an underlying syndrome. Examples of syndromes where a clubfoot can occur include arthrogryposis, constriction band syndrome (streeter’s dysplasia), tibial hemimelia & diastrophic dwarfism.
- 11. Clubfoot consists of bone deformity and soft tissue contracture. It has several tissue abnormalities, including muscle and cartilage anomalies, bone primary germ plasm defects, and vascular abnormalities such as hypoplasia/absence of the anterior tibial artery. Retracting fibrosis (or myofibrosis) may occur secondary to increased fibrous tissue in muscles and ligaments, results into shortening of the Achilles tendon which in turn results the deformity of the foot.
- 12. Most commonly, a doctor recognizes clubfoot soon after birth just from looking at the shape and positioning of the newborn's foot. Occasionally, the doctor may request X-rays to fully understand how severe the clubfoot is, but usually X- rays are not necessary. It's possible to clearly see most cases of clubfoot before birth during a routine ultrasound exam in 20th of pregnancy. While nothing can be done before birth to solve the problem, knowing about the condition may give you time to learn more about clubfoot and get in touch with appropriate health experts, such as a paediatric orthopaedic surgeon and a genetic counsellor.
- 13. Because your newborn's bones, joints and tendons are very flexible, treatment for clubfoot usually begins in the first week or two after birth. The goal of treatment is to improve the way your child's foot looks and works before he or she learns to walk, in hopes of preventing long-term disabilities. Treatment options include: Stretching and casting (Ponseti method) Surgery
- 14. This is the most common treatment for clubfoot. The doctor will: Move your baby's foot into a correct position and then place it in a cast to hold it there Reposition and recast your baby's foot once a week for several months Perform a minor surgical procedure to lengthen the Achilles tendon (percutaneous Achilles tenotomy) toward the end of this process After the shape of your baby's foot is realigned, you'll need to maintain it with one or more of the following: Doing stretching exercises with your baby Putting your child in special shoes and braces Making sure your child wears the shoes and braces as long as needed — usually full time for three months, and then at night and during naps for up to three years For this method to be successful, you'll need to apply the braces according to your doctor's directions so that the foot doesn't return to its original position. The main reason this procedure sometimes doesn't work is because the braces are not used as directed.
- 16. If your baby's clubfoot is severe or doesn't respond to nonsurgical treatments, more-invasive surgery may be needed. An orthopaedic surgeon can lengthen or reposition tendons and ligaments to help ease the foot into a better position. After surgery, your child will be in a cast for up to two months, and then need to wear a brace for a year or so to prevent the clubfoot from coming back. Even with treatment, clubfoot may not be totally correctable. But in most cases, babies who are treated early grow up to wear ordinary shoes and lead full, active lives.
- 17. Nursing Assessment History:- Seek a detailed family history of clubfoot or neuromuscular disorders, and perform a general examination to identify any other abnormalities. Physical exam. Examine the feet with the child prone, with the plantar aspect of the feet visualized, and supine to evaluate internal rotation and varus; if the child can stand, determine whether the foot is plantigrade, whether the heel is bearing weight, and whether it is in varus, valgus, or neutral.
- 18. Nursing Diagnosis Based on the assessment data, the major nursing diagnoses are: Disturbed body image related to permanent alteration in structure and/or function. Deficient knowledge related to the condition, prognosis, treatment, self-care, and discharge needs. Risk for peripheral neurovascular dysfunction related to mechanical compression (cast or brace). Risk for impaired skin integrity related to cast application, traction or surgery. Risk for impaired parenting related to maladaptive coping strategies secondary to diagnosis of talipes deformity.
- 19. The major nursing care planning goals for patients with congenital talipes equinovarus (clubfoot) are: Parents verbalize acceptance of self in the situation Family discuss about situation and changes that would have occurred. Parents develop realistic goals/plans for the future. Parents explain disease state, recognizes the need for medications and understands treatments. Parents demonstrate how to incorporate new health regimen into lifestyle. Parents exhibit ability to deal with health situation and remain in control of life. Parents demonstrate an understanding of plan to heal tissue and prevent injury. Parents describe measures to protect and heal the tissue, including wound care.
- 20. Protect skin integrity. Monitor site of impaired tissue integrity at least once daily for color changes, redness, swelling, warmth, pain, or other signs of infection; monitor patient’s skin care practices, noting type of soap or other cleansing agents used, temperature of water, and frequency of skin cleansing; and provide gloves or clip the nails if necessary to avoid damaging the skin with scratches. Promote acceptance of body image. Acknowledge and accept an expression of feelings of frustration, dependency, anger, grief, and hostility; support verbalization of positive or negative feelings about the actual or perceived loss; and be realistic and positive during treatments, in health teaching, and in setting goals within limitations. Provide health education. Include the parents in creating the teaching plan, beginning with establishing objectives and goals for learning at the beginning of the session; provide clear, thorough, and understandable explanations and demonstrations; and render positive, constructive reinforcement of learning.
- 21. Goals are met as evidenced by: Parents verbalized acceptance of self in situation Family discussed about situation and changes that would have occurred. Parents developed realistic goals/plans for the future. Parents explained disease state, recognizes need for medications, and understands treatments. Parents demonstrated how to incorporate new health regimen into lifestyle. Parents exhibited ability to deal with health situation and remain in control of life. Parents demonstrated an understanding of plan to heal tissue and prevent injury. Parents described measures to protect and heal the tissue, including wound care.
- 22. Because doctors don't know what causes clubfoot, you can't completely prevent it. However, if you're pregnant, you can do things to limit your baby's risk of birth defects, such as: Not smoking or spending time in smoky environments Not drinking alcohol Avoiding drugs not approved by your doctor
- 23. Kruse LM, Buchan JG, Gurnett CA, Dobbs MB. Polygenic threshold model with sex dimorphism in adolescent idiopathic scoliosis: the Carter effect. J Bone Joint Surg Am. 2012 Aug 15;94(16):1485-91. [PubMed] Honein MA, Paulozzi LJ, Moore CA. Family history, maternal smoking, and clubfoot: an indication of a gene-environment interaction. Am J Epidemiol. 2000 Oct 01;152(7):658-65. [PubMed] Parker SE, Mai CT, Strickland MJ, Olney RS, Rickard R, Marengo L, Wang Y, Hashmi SS, Meyer RE., National Birth Defects Prevention Network. Multistate study of the epidemiology of clubfoot. Birth Defects Res A Clin Mol Teratol. 2009 Nov;85(11):897-904. [PubMed] Halmesmäki E, Raivio K, Ylikorkala O. A possible association between maternal drinking and fetal clubfoot. N Engl J Med. 1985 Mar 21;312(12):790. [PubMed] Barker SL, Macnicol MF. Seasonal distribution of idiopathic congenital talipes equinovarus in Scotland. J Pediatr Orthop B. 2002 Apr;11(2):129- 33. [PubMed] Mandlecha P, Kanojia RK, Champawat VS, Kumar A. Evaluation of modified Ponseti technique in treatment of complex clubfeet. J Clin Orthop Trauma. 2019 May-Jun;10(3):599-608. [PMC free article] [PubMed]