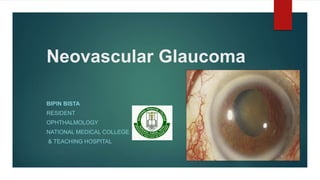
Neovascular glaucoma
- 1. Neovascular Glaucoma BIPIN BISTA RESIDENT OPHTHALMOLOGY NATIONAL MEDICAL COLLEGE & TEACHING HOSPITAL
- 2. Terminology Coats (1906) described new vessel formation on the iris in eyes with CRVO. This neovascularisation is known as rubeosis iridis. RI is associated with a severe form of glaucoma Called as : Congestive G, Thrombotic G, Vascular G, Haemorrhagic G Weiss and colleague proposed : Neovascular Glaucoma or Rubeotic Glaucoma
- 3. Factors predisposing to Rubeosis Iridis Retinal Ischemic Disease : DR, CRVO, CRAO, BRVO, BRAO, RD, Hemorrhagic retinal disorders,Coat’s exudative retinopathy, Eales disease, ROP, sickle cell retinopathy,Retinoschisis Irradiation Tumours Inflammatory disorders :VKH,SO,Endophthalmitis Surgical :Carotid endarterectomy,cataract extraction,pars plana vitrectomy, Nd:Yag capsulotomy Extraocular Vascular Disorders : carotid-cavernous fistula, ICA occlusion
- 4. Theories of Neovascularisation Retinal Hypoxia Angiogenesis Factors : ocular tissues have angiogenic activity related to a key angiogenic peptide, Vascular Endothelial Growth Factor (VEGF). o VEGF : primary source is from Mϋller cells. Has 4 isoforms (VEGF121 , VEGF165 ,VEGF189 , VEGF206 ). It is a potent angiogenic stimulator, promoting proliferation, migration, proteolytic activity, and capillary tube formation. Vasoinhibitory Factors : Possible source from vitreous and lens.
- 5. Clinicopathological Course Prerubeosis Stage Preglaucoma stage : Rubeosis iridis Open angle glaucoma Stage Angle closure glaucoma Stage
- 6. Prerubeosis Stage : DM Risk is RI in Dm is greatly increased when arteriolar or capillary nonperfusion is present or after vitrectomy or lensectomy. Fluorescence angiography : peripapillary leakage Important to pay close attention to the papillary margin of iris, neovascularisation is first seen here.
- 7. Prerubeosis Stage : CRVO Develops hypotony Fluorescein angiography reveals abnormal, leaking vessels in virtually all eyes with extensive retinal capillary closure after CRVO. Aqueous protein and cells concentration shows severity : Laser flare cell meter RAPD Most diagnostic finding : ERG ERG finding : B-wave implicit time delay and a reduced B-wave A-wave amplitude ratio. Blood flow velocity : Color Doppler Imaging.
- 9. Preglaucoma Stage :Rubeosis Iridis Characterised by normal IOP, unless pre-existing COAG presents Slitlamp : dilated tufts of preexiting capillaries and fine, randomly oriented vessels on the surface of the iris near the pupillary margin Leakage of fluorescein : New vessels Peripupillary iris : first sight to be seen with Neovascularisation. Gonioscopy : angle neovacularisation, single vascular trunks crossing the ciliary body band and scleral spur and arborizing on the TM.
- 11. Preglaucoma Stage :Rubeosis Iridis HISTOPATHOLOGICAL FEATURES : begins intrastromally and then reaches on the surface of the iris. New vessels in the angle run circumferentially in the TM, with branches coursing into the Schlemm canal and occasionally into collector channels These new vessels have fenestrated walls are arranged in irregular patterns. Ultrastructure of iris neovascularisation : Interendothelial cell junctions, attenuated intraendothelial cytoplasm and pericyte formation.
- 12. Open Angle Glaucoma Stage Doesn’t invariably follow the development of rubeosis iridis. May resolve spontaneously in DR, with incidence of 13 to 41% CRVO has higher incidence, typically occurs 8 to 15 weeks after the vascular occlusive event. It has been called as 90 day glaucoma. RI is more florid in this stage. In Gonioscopy , AC angle is still open, but neovascularisation may be intense.
- 13. Open Angle Glaucoma Stage Histopathological features : Hallmark is fibrovascular membrane that covers the AC angle and anterior surface of the iris and may even extend to the posterior iris. Glaucoma occurs d/t obstruction of the TM by the fibrovascular membrane, with variable contribution from the inflammation and haemorrhage. Spaced between the trabecular beams were lined by a single layer of vascular endothelium and were filled with RBCs.
- 14. Angle Closure Glaucoma Stage Stroma of the iris has become flattened , with a smooth,glistening appearance . Ectropion uveae is frequently present. Iris is dilated and pulled anteriorly from the lens. Contracture leads to formation of peripheral anterior synechia.
- 15. Open Angle Glaucoma Stage Histological feature : alterations of the angle from the contracture of tissue overlying these structures. Tissue contraction : superficial layer of myofibroblasts (i.e, fibroblastic cells with smooth muscle differentiation)
- 16. Management Panretinal Photocoagulation • Ablation of the peripheral retina with laser (argon) is the first line therapy. • Significant to reduce or eliminate anterior segment neovascularisation. • Mechanism : Uncertain , related to decreasing the retinal oxygen demand • Reduce the stimulus for release of an angiogenesis factor or may reduce the hypoxia in the anterior ocular segment • Indicated in all cases of RI • Photocoagulation should be performed in prerubeosis stage.
- 17. Management Panretinal Cryotherapy • When cloudy media preclude Panretinal coagulation
- 18. Management Anti-VEGF Agents : Bevacizumab (1.25mg) in the vitreous cavity and (1.0-1.25 mg) in the anterior chamber Seems to show significant regression of a concomitant reduction in IOP. Important to proceed with PRP as soon as practical to help prevent recurrent neovascularisations
- 19. Glaucoma surgical procedures Cyclodestructive surgery : transscleral Nd:YAG cyclophotocoagulation and diode laser cyclophotocoagulation Filtering surgery : Rare successful, Glaucoma Drainage device surgery : Encouraging results with adjuvant bevacizumab. Endoscopic cyclophotocoagulation Silicone oil injection IV injection of crystalline triamcinolone acetonide.
- 20. Reference: 1.Glaucoma – Shield Textbook of Glaucoma 6th edition 2.Curbside Consultation in Glaucoma : Steven J. Gedde 3.Myron yanoff and jay s duker4th edition THANK YOU
