Anticholinergic system and drugs
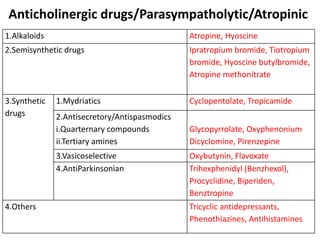
- 1. Anticholinergic drugs/Parasympatholytic/Atropinic 1.Alkaloids Atropine, Hyoscine 2.Semisynthetic drugs Ipratropium bromide, Tiotropium bromide, Hyoscine butylbromide, Atropine methonitrate 3.Synthetic drugs 1.Mydriatics Cyclopentolate, Tropicamide 2.Antisecretory/Antispasmodics i.Quarternary compounds ii.Tertiary amines Glycopyrrolate, Oxyphenonium Dicyclomine, Pirenzepine 3.Vasicoselective Oxybutynin, Flavoxate 4.AntiParkinsonian Trihexphenidyl (Benzhexol), Procyclidine, Biperiden, Benztropine 4.Others Tricyclic antidepressants, Phenothiazines, Antihistamines
- 3. Atropine Pharmacological actions/Mechanism of action Atropine is a highly selective competitive blocker of muscarinic receptor. It blocks all subtypes of muscarinic receptors. Heart Causes tachycardia by blocking M2receptor on SA node Temperature Increases Blood pressure No marked effect, vasodilation at high doses Smooth muscles Tone & contractility of smooth muscles are reduced Eye Mydriasis (Dilation of pupils), cyclopegia (paralysis of accommodation)
- 4. Indication • Analgesic spasmolytic in the treatment of gastro-intestinal spasms and biliary or hepatic colic • Antispasmodic in asthma • Cough medicine (with codeine mixture) • Treatment of tremor and rigidity in Parkinson's disease • Mydriatic and during ophthalmic surgery • Pre-anesthetic (to inhibit salivation and respiratory secretions and to prevent the risk of vagal inhibition of the heart) • Treatment of bradycardia and cardiac arrest in intensive care medicine • Antidote to nerve agent poisoning (organophosphates poisoning) Contraindication • Patients with chronic respiratory disease because of it it acts on parasympathetic nervous system in which inhibit salivary and mucus secretion. • It also contraindicated to patients with glaucoma, thyrotoxicosis, pyloric stenosis (narrowing of opening of stomach), UTI obstruction and hypersensitivity reactions.
- 5. Side Effects Allergic reaction Dysphagia Restlessness Constipation Arrhythmias Confusion Excitement Headache Dizziness Blurred vision Respiratory depression Photosensitivity reaction Dose: • For bradycardia- 500mcg IV push, may repeat every 3 to 5 minutes up to a total dose of 3 mg (maximum 0.04 mg/kg) • For dilation of pupil- 1 drop of a 1% solution BID for 1 to 2 day, 0.5% solution for children. • For pre-anaesthesia- 300 to 600 mcg S/c or I/M injection, usually 30 to 60 minutes before anaesthesia.
- 6. Anticholinergic drugs Action Dose Dicyclomine Smooth muscle relaxant, antispasmodic 20mg oral Oxybutynin/ Flavoxate Smooth muscle relaxant, antispasmodic specific to urinary bladder & salivary glands Oxybutynin 5mg BD/TDS oral Flavoxate 200mg TDS oral Drotaverine Antispasmodic, muscle relaxant 40-80mg TDS oral
- 7. Anticholinergic drugs Uses Dose Hyoscine butylbromide Esophageal or GI spasms 20-40mg oral also given i.v./i.m./s.c. Atropine methonitrate Abdominal colic, hyperacidity 2.5-10mg oral Ipratopium bromide Asthma, COPD 40-80 mcg inhalational
- 8. Mydriatics Dilation Potency Atropine 30-40 mins Potent Homatropine 45-60 mins Less potent Cyclopentolate 30-60 mins Potent & rapidly acting Tropicamide 20-40 mins Quickest & briefest
- 10. • Parkinson's disease (PD) is a neurodegenerative disorder that affects predominately dopamine- producing neurons in a specific area of the brain called substantia nigra. Symptoms of Parkinsons’s disease includes tremor, slowness of movements, limb rigidity, etc. • Anti-Parkinsonian drugs: • Trihexphenidyl (Benzhexol) 2-10mg/day • Procyclidine • Biperiden Levodopa + Carbidopa (dopa decarboxylase inhibitor)
- 11. Uses of anticholinergic drugs: • Antisecretory i. Pre-anaesthetic medicine ii. Peptic ulcer iii. Pulmonary embolism • Antispasmodic (Intestinal colic, renal colic, abdominal cramps, dysmenorrhoea, urinary frequency & urgency) • Bronchial asthma, COPD • Mydriatic & cyclopegic (diagnostic & therapeutic) • Bradycardia & partial heart block • Parkinsonism • Motion sickness • Lie dectector (Hyoscine) • Poisoning • Organophosphorus, carbamate & mushroom poisoning
- 12. Adverse Effects: ANTI-CHOLINERGIC TOXIDROMES • Symptoms: Agitated Delirium Signs Of Peripheral Muscarinic Blockade: Blurred Vision, Coma, Decreased Bowel Sounds, Delirium, Dry Skin, Fever, Flushing, Hallucinations, Ileus, Memory Loss, Mydriasis (Dilated Pupils), Myoclonus, Psychosis, Seizures, & Urinary Retention • Substances: The four "anti"s: Antihistamines, Antipsychotics, Antidepressants & Antiparkinsonian • Atropine, Benztropine, Datura, and Scopolamine. “Blind as a bat, mad as a hatter, red as a beet, hot as Hares, dry as a bone, the bowel and bladder lose their tone, and the heart runs alone.”- Atropine Poisoning Complications: Hypertension, Hyperthermia, Tachycardia
- 14. Resuscitation • ABCDE Risk Assessment • Agent(s), Dose(s), Time since ingestion • Clinical features and progress • Patient factors and co-morbidities Investigations • Screening: ECG • Specific: Drug levels, Electrolytes, renal function, ABG Supportive Care •Quiet, Well lit Room •Intravenous Fluids •Catheterization •Diazepam for agitation Decontamination •Activated Charcoal ANTI-CHOLINERGIC TOXIDROME MANAGEMENT Antidotes •Physostigmine 1-3mg i.v.
