Report
Share
Recommended
The primary onset of this study is to determine the short and longer term effects of dual task training gait on walking performance when dual tasking in people with Parkinson’s disease.. The aim of the study is to analyze the efficacy of dual task training to improve functional gait performance in idiopathic Parkinson’s disease subjects. Design and setting: A randomized controlled study design was used to examine the differences in conventional therapeutic exercises and conventional therapeutic exercises with specific external cueing strategies given between two groups. Subjects: A sample of 10 subjects with idiopathic Parkinson’s disease was screened using Timed up and go test (TUG Test) and those who scored 24% less was taken for the study .the subjects were of both genders aged between 50-75 years of age with medically stable patients. They were divided into two groups of control and experimental group.the study was done in Masterskill College of nursing and health. Outcome Measurement: Functional gait performance will be measured using the timed up and Go (TUG) test with added motor and cognitive tasks, participants will be asked to walk as quickly as they safely can under all conditions and will be permitted to use their usual gait aid. Results: Data Analysis of the subjects after dual task training led to a greater improvement in functional walking capacity and step length. The average percentage of improvement in timed up and go test is 53%. Conclusion: According to this study Dual task training had improved step length and functional walking capacity in idiopathic Parkinson’s disease.
Efficacy of Dual Task Training to Improve Functional Gait Performance in Idio...

Efficacy of Dual Task Training to Improve Functional Gait Performance in Idio...International Journal of Science and Research (IJSR)
Recommended
The primary onset of this study is to determine the short and longer term effects of dual task training gait on walking performance when dual tasking in people with Parkinson’s disease.. The aim of the study is to analyze the efficacy of dual task training to improve functional gait performance in idiopathic Parkinson’s disease subjects. Design and setting: A randomized controlled study design was used to examine the differences in conventional therapeutic exercises and conventional therapeutic exercises with specific external cueing strategies given between two groups. Subjects: A sample of 10 subjects with idiopathic Parkinson’s disease was screened using Timed up and go test (TUG Test) and those who scored 24% less was taken for the study .the subjects were of both genders aged between 50-75 years of age with medically stable patients. They were divided into two groups of control and experimental group.the study was done in Masterskill College of nursing and health. Outcome Measurement: Functional gait performance will be measured using the timed up and Go (TUG) test with added motor and cognitive tasks, participants will be asked to walk as quickly as they safely can under all conditions and will be permitted to use their usual gait aid. Results: Data Analysis of the subjects after dual task training led to a greater improvement in functional walking capacity and step length. The average percentage of improvement in timed up and go test is 53%. Conclusion: According to this study Dual task training had improved step length and functional walking capacity in idiopathic Parkinson’s disease.
Efficacy of Dual Task Training to Improve Functional Gait Performance in Idio...

Efficacy of Dual Task Training to Improve Functional Gait Performance in Idio...International Journal of Science and Research (IJSR)
More Related Content
What's hot
What's hot (14)
Article from the National Psychologist about Scott Miller's speech at Evoluti...

Article from the National Psychologist about Scott Miller's speech at Evoluti...
Fricchione psychosomatic medicine in mental health

Fricchione psychosomatic medicine in mental health
Information interventions for injury recovery: a review

Information interventions for injury recovery: a review
How to Improve Quality of Services by Integrating Common Factors into Treatme...

How to Improve Quality of Services by Integrating Common Factors into Treatme...
Neurodevelopmental Treatment and Cerebral Palsy- Research

Neurodevelopmental Treatment and Cerebral Palsy- Research
Scientific paper presentation-EFFECTIVENESS OF DEEP BREATHING EXERCISE TO RED...

Scientific paper presentation-EFFECTIVENESS OF DEEP BREATHING EXERCISE TO RED...
Does publication bias inflate the apparent efficacy of psychological treatmen...

Does publication bias inflate the apparent efficacy of psychological treatmen...
Viewers also liked
Viewers also liked (6)
Similar to AliRushmer-Honors
On March 31st 2014 - following the inaugural World Bipolar Day - Dr. Erin Michalak, Associate Professor of Psychiatry, hosted a live webinar to explore findings from CREST.BD's current Delphi Self-Management study. During the webinar Dr. Michalak discussed the study's participatory methods, shared some of the demographic data and research findings from Phase 1 of the study, as well as discussed the team's experiences with using Delphi Consensus methods. We've recently launched Round 2 of our Delphi study to our 150 survey panel members. In this 30 minute webinar you'll learn more about the findings of this unique international study, how the findings will be used to improve wellness in bipolar disorder, and how to get involved in CREST.BD's community-engaged research.
Don't forget to check out the Storify from our World Bipolar Day #bipolarchat on March 30th 2014! http://sfy.co/tSZULiving Successfully with Bipolar Disorder - Webinar with Dr. Erin Michalak

Living Successfully with Bipolar Disorder - Webinar with Dr. Erin MichalakCollaborative RESearch Team to study Bipolar Disorder, UBC
Similar to AliRushmer-Honors (20)
Can you provide tips or strategies for managing insomnia while seeking treatm...

Can you provide tips or strategies for managing insomnia while seeking treatm...
Original ArticleDesign and implementation of a randomized.docx

Original ArticleDesign and implementation of a randomized.docx
1. the effectiveness of emotional freedom techniques (eft) as a treatment for...

1. the effectiveness of emotional freedom techniques (eft) as a treatment for...
Saúde baseada em evidencias: Clube de revista - Encontro 01

Saúde baseada em evidencias: Clube de revista - Encontro 01
Living Successfully with Bipolar Disorder - Webinar with Dr. Erin Michalak

Living Successfully with Bipolar Disorder - Webinar with Dr. Erin Michalak
Terapia cognitiva-comportamental para pessoas com dor musculo-esquelética

Terapia cognitiva-comportamental para pessoas com dor musculo-esquelética
AliRushmer-Honors
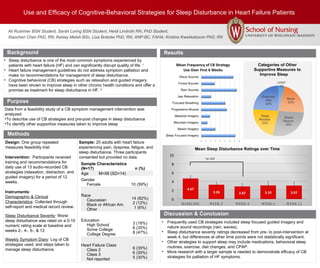
- 1. Use and Efficacy of Cognitive-Behavioral Strategies for Sleep Disturbance in Heart Failure Patients Ali Rushmer BSN Student, Sarah Loring BSN Student, Heidi Lindroth RN, PhD Student, Xiaochen Chen PhD, RN, Kelsey Melah BSc, Lisa Bratzke PhD, RN, ANP-BC, FAHA, Kristine Kwekkeboom PhD, RN Background Methods Sample: 20 adults with heart failure experiencing pain, dyspnea, fatigue, and sleep disturbance. Three participants consented but provided no data. Results Discussion & Conclusion • Frequently used CB strategies included sleep focused guided imagery and nature sound recordings (rain, waves). • Sleep disturbance severity ratings decreased from pre- to post-intervention at week 4; but differences at other time points were not statistically significant. • Other strategies to support sleep may include medications, behavioral sleep routines, exercise, diet changes, and CPAP. • More research with a larger sample is needed to demonstrate efficacy of CB strategies for palliation of HF symptoms. Purpose • Sleep disturbance is one of the most common symptoms experienced by patients with heart failure (HF) and can significantly disrupt quality of life. 1 • Heart failure management guidelines do not address symptom palliation and make no recommendations for management of sleep disturbance. • Cognitive behavioral (CB) strategies such as relaxation and guided imagery have been shown to improve sleep in other chronic health conditions and offer a promise as treatment for sleep disturbance in HF. 2 Data from a feasibility study of a CB symptom management intervention was analyzed: •To describe use of CB strategies and pre-post changes in sleep disturbance •To identify other supportive measures taken to improve sleep Sample Characteristics (N=17) n (%) Age M=58 (SD=14) Gender Female 10 (59%) Race Caucasian Black or African Am. Other 14 (82%) 2 (12%) 1 (6%) Education High School Some College College Degree 3 (18%) 6 (35%) 8 (47%) Heart Failure Class Class 2 Class 3 Not reported 6 (35%) 6 (35%) 5 (30%) *p=.032 Design: One group repeated measures feasibility trial. Intervention: Participants received training and recommendations for daily use of 13 audio-recorded CB strategies (relaxation, distraction, and guided imagery) for a period of 12 weeks. Instruments: Demographic & Clinical Characteristics: Collected through self-report and medical record review. Sleep Disturbance Severity: Worst sleep disturbance was rated on a 0-10 numeric rating scale at baseline and weeks 2-, 4-, 6-, & 12. Weekly Symptom Diary: Log of CB strategies used, and steps taken to manage sleep disturbance.