More Related Content
Similar to Pneumothorax (20)
More from Hiba Ashibany (20)
Pneumothorax
- 1. Copyright © 2006 by Mosby, Inc.Slide 1
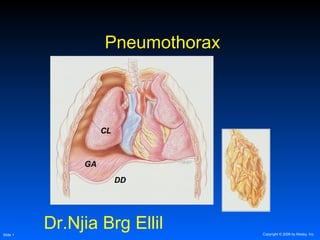
PneumothoraxPneumothorax
GA
DD
CL
Dr.Njia Brg Ellil
- 2. Copyright © 2006 by Mosby, Inc.Slide 2
Anatomic Alterations of the LungsAnatomic Alterations of the Lungs
Lung collapseLung collapse
AtelectasisAtelectasis
Chest wall expansionChest wall expansion
Compression of the great veins andCompression of the great veins and
decreased cardiac venous returndecreased cardiac venous return
- 3. Copyright © 2006 by Mosby, Inc.Slide 3
Etiology—3 WaysEtiology—3 Ways
From the lungs through a perforation of theFrom the lungs through a perforation of the
visceral pleuravisceral pleura
From the surrounding atmosphere through aFrom the surrounding atmosphere through a
perforation of the chest wall and parietalperforation of the chest wall and parietal
pleura or, rarely, through an esophagealpleura or, rarely, through an esophageal
fistula or a perforated abdominal viscusfistula or a perforated abdominal viscus
From gas-forming microorganisms in anFrom gas-forming microorganisms in an
empyema in the pleural space (rare)empyema in the pleural space (rare)
- 4. Copyright © 2006 by Mosby, Inc.Slide 4
Pneumothorax ClassificationsPneumothorax Classifications
General TermsGeneral Terms
Closed pneumothoraxClosed pneumothorax
Open pneumothoraxOpen pneumothorax
Tension pneumothoraxTension pneumothorax
- 5. Copyright © 2006 by Mosby, Inc.Slide 5
Pneumothorax ClassificationsPneumothorax Classifications
Based on OriginBased on Origin
Traumatic pneumothoraxTraumatic pneumothorax
Spontaneous pneumothoraxSpontaneous pneumothorax
Iatrogenic pneumothoraxIatrogenic pneumothorax
- 8. Copyright © 2006 by Mosby, Inc.Slide 8
Spontaneous PneumothoraxSpontaneous Pneumothorax
- 9. Copyright © 2006 by Mosby, Inc.Slide 9
Iatrogenic PneumothoraxIatrogenic Pneumothorax
- 10. Copyright © 2006 by Mosby, Inc.Slide 10
Overview of the CardiopulmonaryOverview of the Cardiopulmonary
Clinical Manifestations AssociatedClinical Manifestations Associated
with PNEUMOTHORAXwith PNEUMOTHORAX
The following clinical manifestations result fromThe following clinical manifestations result from
the pathophysiologic mechanisms caused (orthe pathophysiologic mechanisms caused (or
activated) byactivated) by AtelectasisAtelectasis
- 12. Copyright © 2006 by Mosby, Inc.Slide 12
Clinical Data Obtained at theClinical Data Obtained at the
Patient’s BedsidePatient’s Bedside
Vital signsVital signs
Increased respiratory rateIncreased respiratory rate
Stimulation of peripheral chemoreceptorsStimulation of peripheral chemoreceptors
Other possible mechanismsOther possible mechanisms
• Decreased lung complianceDecreased lung compliance
• Activation of the deflation receptorsActivation of the deflation receptors
• Activation of the irritant receptorsActivation of the irritant receptors
• Stimulation of the J receptorsStimulation of the J receptors
• Pain/anxietyPain/anxiety
Increased heart rate, cardiac output, blood pressureIncreased heart rate, cardiac output, blood pressure
- 14. Copyright © 2006 by Mosby, Inc.Slide 14
Clinical Data Obtained at theClinical Data Obtained at the
Patient’s BedsidePatient’s Bedside
CyanosisCyanosis
Chest assessment findingsChest assessment findings
Hyperresonant percussion note over theHyperresonant percussion note over the
pneumothoraxpneumothorax
Diminished breath sounds over the pneumothoraxDiminished breath sounds over the pneumothorax
Tracheal shiftTracheal shift
Displaced heart soundsDisplaced heart sounds
Increased thoracic volume on the affected sideIncreased thoracic volume on the affected side
• Particularly in tension pneumothoraxParticularly in tension pneumothorax
- 18. Copyright © 2006 by Mosby, Inc.Slide 18
Clinical Data Obtained fromClinical Data Obtained from
Laboratory Tests and SpecialLaboratory Tests and Special
ProceduresProcedures
- 19. Copyright © 2006 by Mosby, Inc.Slide 19
Pulmonary Function Study:Pulmonary Function Study:
Lung Volume and Capacity FindingsLung Volume and Capacity Findings
VT RV FRC TLC
N or ↓ ↓ ↓ ↓
VC IC ERV RV/TLC%
↓ ↓
↓ N
VT RV FRC TLC
N or ↓ ↓ ↓ ↓
VC IC ERV RV/TLC%
↓ ↓
↓ N
- 20. Copyright © 2006 by Mosby, Inc.Slide 20
Arterial Blood GasesArterial Blood Gases
Small PneumothoraxSmall Pneumothorax
Acute alveolar hyperventilation withAcute alveolar hyperventilation with
hypoxemiahypoxemia
pH PaCO2 HCO3
-
PaO2
↑ ↓ ↓ (Slightly) ↓
- 21. Copyright © 2006 by Mosby, Inc.Slide 21
Time and Progression of Disease
100
50
30
80
0
PaCO
2
10
20
40
Alveolar Hyperventilation
60
70
90 Point at which PaO2
declines enough to
stimulate peripheral
oxygen receptors
Point at which PaO2
declines enough to
stimulate peripheral
oxygen receptors
PaO2
Disease OnsetPaO2orPaCO2
- 22. Copyright © 2006 by Mosby, Inc.Slide 22
Arterial Blood GasesArterial Blood Gases
Large PneumothoraxLarge Pneumothorax
Acute ventilatory failure with hypoxemiaAcute ventilatory failure with hypoxemia
pH PaCO2 HCO3
-
PaO2
↓ ↑ ↑ (Slightly) ↓
- 23. Copyright © 2006 by Mosby, Inc.Slide 23
Time and Progression of Disease
100
50
30
80
0
PaO
2
10
20
40
Alveolar Hyperventilation
60
70
90
Point at which PaO2
declines enough to
stimulate peripheral
oxygen receptors
Point at which PaO2
declines enough to
stimulate peripheral
oxygen receptors
PaCO 2
Acute Ventilatory FailureDisease Onset
Point at which disease
becomes severe and patient
begins to become fatigued
Point at which disease
becomes severe and patient
begins to become fatigued
Pa02orPaC02
- 24. Copyright © 2006 by Mosby, Inc.Slide 24
Radiologic FindingsRadiologic Findings
Chest radiographChest radiograph
Increased translucencyIncreased translucency
Mediastinal shift to unaffected sideMediastinal shift to unaffected side
in tension pneumothoraxin tension pneumothorax
Depressed diaphragmDepressed diaphragm
Lung collapseLung collapse
AtelectasisAtelectasis
- 27. Copyright © 2006 by Mosby, Inc.Slide 27
General Management ofGeneral Management of
PneumothoraxPneumothorax
>20%—gas should be evacuated>20%—gas should be evacuated
Negative pressure—5 to 12 cm HNegative pressure—5 to 12 cm H22OO
Should not exceed negative 12 cm HShould not exceed negative 12 cm H22OO
- 28. Copyright © 2006 by Mosby, Inc.Slide 28
General Management ofGeneral Management of
PneumothoraxPneumothorax
Respiratory care treatment protocolsRespiratory care treatment protocols
Oxygen therapy protocolOxygen therapy protocol
Hyperinflation therapy protocolHyperinflation therapy protocol
Mechanical ventilation protocolMechanical ventilation protocol
- 29. Copyright © 2006 by Mosby, Inc.Slide 29
General Management ofGeneral Management of
PneumothoraxPneumothorax
PLEURODESISPLEURODESIS
Chemical or medication injected into theChemical or medication injected into the
chest cavitychest cavity
TalcTalc
TetracyclineTetracycline
Bleomycin sulfateBleomycin sulfate
Produces inflammatory reaction betweenProduces inflammatory reaction between
lungs and inner chest cavitylungs and inner chest cavity
Causes lung to stick to chest cavityCauses lung to stick to chest cavity
- 30. Copyright © 2006 by Mosby, Inc.Slide 30
Conditions requiring chestConditions requiring chest
drainagedrainage
Air between the pleuraeAir between the pleurae
is ais a pneumothoraxpneumothorax
- 31. Copyright © 2006 by Mosby, Inc.Slide 31
Conditions requiring chestConditions requiring chest
drainagedrainage
Blood in the pleuralBlood in the pleural
space is aspace is a hemothoraxhemothorax
- 32. Copyright © 2006 by Mosby, Inc.Slide 32
Conditions requiring chest drainageConditions requiring chest drainage
Transudate or exudateTransudate or exudate
in the pleural space is ain the pleural space is a
pleural effusionpleural effusion
- 33. Copyright © 2006 by Mosby, Inc.Slide 33
Conditions requiring chest drainage:Conditions requiring chest drainage:
pneumothoraxpneumothorax
PneumothoraxPneumothorax
Occurs when there is an opening on the surface ofOccurs when there is an opening on the surface of
the lung or in the airways, in the chest wall — orthe lung or in the airways, in the chest wall — or
bothboth
The opening allows air to enter the pleural spaceThe opening allows air to enter the pleural space
between the pleurae, creating an actual spacebetween the pleurae, creating an actual space
- 34. Copyright © 2006 by Mosby, Inc.Slide 34
Conditions requiring chest drainage:Conditions requiring chest drainage:
open pneumothoraxopen pneumothorax
Open pneumothoraxOpen pneumothorax
Opening in the chestOpening in the chest
wall (with or withoutwall (with or without
lung puncture)lung puncture)
Allows atmospheric airAllows atmospheric air
to enter the pleuralto enter the pleural
spacespace
Penetrating trauma:Penetrating trauma:
stab, gunshot,stab, gunshot,
impalementimpalement
SurgerySurgery
- 35. Copyright © 2006 by Mosby, Inc.Slide 35
Conditions requiring chest drainage: closedConditions requiring chest drainage: closed
pneumothoraxpneumothorax
Closed pneumothoraxClosed pneumothorax
Chest wall is intactChest wall is intact
Rupture of the lungRupture of the lung
and visceral pleura (orand visceral pleura (or
airway) allows air intoairway) allows air into
the pleural spacethe pleural space
- 36. Copyright © 2006 by Mosby, Inc.Slide 36
Conditions requiring chest drainage: openConditions requiring chest drainage: open
pneumothoraxpneumothorax
AnAn open pneumothoraxopen pneumothorax is also called a “suckingis also called a “sucking
chest wound”chest wound”
With the pressure changes in the chest thatWith the pressure changes in the chest that
normally occur with breathing, air moves in andnormally occur with breathing, air moves in and
out of the chest through the opening in the chestout of the chest through the opening in the chest
wallwall
Looks bad and sounds worse, but the openingLooks bad and sounds worse, but the opening
acts as a vent so pressure from trapped airacts as a vent so pressure from trapped air
cannot build up in the chestcannot build up in the chest
- 37. Copyright © 2006 by Mosby, Inc.Slide 37
Conditions requiring chest drainage: closedConditions requiring chest drainage: closed
pneumothoraxpneumothorax
In aIn a closedclosed
pneumothoraxpneumothorax, a, a
patient who is breathingpatient who is breathing
spontaneously canspontaneously can
have an equilibration ofhave an equilibration of
pressures across thepressures across the
collapsed lungcollapsed lung
The patient will haveThe patient will have
symptoms, but this issymptoms, but this is
not life-threateningnot life-threatening
- 38. Copyright © 2006 by Mosby, Inc.Slide 38
Conditions requiring chest drainage:Conditions requiring chest drainage:
tension pneumothoraxtension pneumothorax
AA tension pneumothoraxtension pneumothorax can killcan kill
Chest wall is intactChest wall is intact
Air enters the pleural space from the lung orAir enters the pleural space from the lung or
airway, and it has no way to leaveairway, and it has no way to leave
There is no vent to the atmosphere as there is inThere is no vent to the atmosphere as there is in
an open pneumothoraxan open pneumothorax
Most dangerous when patient is receivingMost dangerous when patient is receiving
positive pressure ventilation in which air ispositive pressure ventilation in which air is
forced into the chest under pressureforced into the chest under pressure
- 39. Copyright © 2006 by Mosby, Inc.Slide 39
Conditions requiring chest drainage:Conditions requiring chest drainage:
tension pneumothoraxtension pneumothorax
Tension pneumothoraxTension pneumothorax
occurs when aoccurs when a closedclosed
pneumothoraxpneumothorax createscreates
positive pressure in thepositive pressure in the
pleural space thatpleural space that
continues to buildcontinues to build
That pressure is thenThat pressure is then
transmitted to thetransmitted to the
mediastinum (heart andmediastinum (heart and
great vessels)great vessels)
- 40. Copyright © 2006 by Mosby, Inc.Slide 40
Conditions requiring chest drainage:Conditions requiring chest drainage:
mediastinal shiftmediastinal shift
Mediastinal shift
Mediastinal shiftMediastinal shift occursoccurs
when the pressure getswhen the pressure gets
so high that it pushes theso high that it pushes the
heart and great vesselsheart and great vessels
into the unaffected sideinto the unaffected side
of the chestof the chest
These structures areThese structures are
compressed fromcompressed from
external pressure andexternal pressure and
cannot expand to acceptcannot expand to accept
blood flowblood flow
- 41. Copyright © 2006 by Mosby, Inc.Slide 41
Conditions requiring chest drainage:Conditions requiring chest drainage:
mediastinal shiftmediastinal shift
Mediastinal shiftMediastinal shift can quickly lead tocan quickly lead to
cardiovascular collapsecardiovascular collapse
The vena cava and the right side of the heartThe vena cava and the right side of the heart
cannot accept venous returncannot accept venous return
With no venous return, there is no cardiac outputWith no venous return, there is no cardiac output
No cardiac output = not able to sustain lifeNo cardiac output = not able to sustain life
- 42. Copyright © 2006 by Mosby, Inc.Slide 42
Conditions requiring chest drainage:Conditions requiring chest drainage:
tension pneumothoraxtension pneumothorax
When the pressure isWhen the pressure is
external, CPR will notexternal, CPR will not
help – the heart will stillhelp – the heart will still
not accept venous returnnot accept venous return
Immediate, live-savingImmediate, live-saving
treatment is placing atreatment is placing a
needle toneedle to
relieve pressurerelieve pressure
followed byfollowed by
chest tubechest tube
- 43. Copyright © 2006 by Mosby, Inc.Slide 43
Conditions requiring chest drainage:Conditions requiring chest drainage:
hemothoraxhemothorax
HemothoraxHemothorax occurs after thoracic surgery andoccurs after thoracic surgery and
many traumatic injuriesmany traumatic injuries
As with pneumothorax, the negative pressureAs with pneumothorax, the negative pressure
between the pleurae is disrupted, and the lung willbetween the pleurae is disrupted, and the lung will
collapse to some degree, depending on thecollapse to some degree, depending on the
amount of bloodamount of blood
The risk of mediastinal shift is insignificant, as theThe risk of mediastinal shift is insignificant, as the
amount of blood needed to cause the shift wouldamount of blood needed to cause the shift would
result in a life-threatening intravascular lossresult in a life-threatening intravascular loss
- 44. Copyright © 2006 by Mosby, Inc.Slide 44
Remove fluid & airRemove fluid & air
ThoracostomyThoracostomy creates an opening in the chest wallcreates an opening in the chest wall
through which a chest tube (also called thoracicthrough which a chest tube (also called thoracic
catheter) is placed, which allows air and fluid tocatheter) is placed, which allows air and fluid to
flow out of the chestflow out of the chest
- 45. Copyright © 2006 by Mosby, Inc.Slide 45
Remove fluid and airRemove fluid and air
- 46. Copyright © 2006 by Mosby, Inc.Slide 46
Remove fluid & airRemove fluid & air
Choose site
Explore with finger
Place tube with clamp
Suture tube to chest
- 47. Copyright © 2006 by Mosby, Inc.Slide 47
Remove fluid & air through chest tubeRemove fluid & air through chest tube
- 48. Copyright © 2006 by Mosby, Inc.Slide 48
Remove fluid and air after thoracicRemove fluid and air after thoracic
surgerysurgery
At the end of theAt the end of the
procedure, theprocedure, the
surgeon makes asurgeon makes a
stab wound in thestab wound in the
chest wall throughchest wall through
which the chestwhich the chest
tube is placed intotube is placed into
the pleural spacethe pleural space
- 49. Copyright © 2006 by Mosby, Inc.Slide 49
Prevent air & fluid from returning toPrevent air & fluid from returning to
the pleural spacethe pleural space
Chest tube is attached to aChest tube is attached to a drainage devicedrainage device
Allows air and fluid to leave the chestAllows air and fluid to leave the chest
Contains a one-way valve to prevent air & fluidContains a one-way valve to prevent air & fluid
returning to the chestreturning to the chest
Designed so that the device is below the level of theDesigned so that the device is below the level of the
chest tube for gravity drainagechest tube for gravity drainage
- 50. Copyright © 2006 by Mosby, Inc.Slide 50
Prevent air & fluid from returning toPrevent air & fluid from returning to
the pleural spacethe pleural space
How does a chest drainage system work?How does a chest drainage system work?
It’s all aboutIt’s all about
bottles andbottles and
strawsstraws
- 51. Copyright © 2006 by Mosby, Inc.Slide 51
Prevent air & fluid from returning toPrevent air & fluid from returning to
the pleural spacethe pleural space
Tube from patient
Tube open to
atmosphere
vents air
Most basic conceptMost basic concept
Straw attached toStraw attached to
chest tube from patientchest tube from patient
is placed under 2cm ofis placed under 2cm of
fluid (water seal)fluid (water seal)
Just like a straw in aJust like a straw in a
drink, air can pushdrink, air can push
through the straw, butthrough the straw, but
air can’t be drawn backair can’t be drawn back
up the strawup the straw
- 52. Copyright © 2006 by Mosby, Inc.Slide 52
Prevent air & fluid from returning toPrevent air & fluid from returning to
the pleural spacethe pleural space
This system works if only air is leaving the chestThis system works if only air is leaving the chest
If fluid is draining, it will add to the fluid in theIf fluid is draining, it will add to the fluid in the
water seal, and increase the depthwater seal, and increase the depth
As the depth increases, it becomes harder forAs the depth increases, it becomes harder for
the air to push through a higher level of water,the air to push through a higher level of water,
and could result in air staying in the chestand could result in air staying in the chest
- 53. Copyright © 2006 by Mosby, Inc.Slide 53
Prevent air & fluid from returning toPrevent air & fluid from returning to
the pleural spacethe pleural space
Tube open to
atmosphere
vents air Tube from patient
Fluid
drainage
2cm
fluid
For drainage, a secondFor drainage, a second
bottle was addedbottle was added
TheThe first bottlefirst bottle collectscollects
thethe drainagedrainage
TheThe second bottlesecond bottle isis
thethe water sealwater seal
With an extra bottle forWith an extra bottle for
drainage, the waterdrainage, the water
seal will then remain atseal will then remain at
2cm2cm
- 54. Copyright © 2006 by Mosby, Inc.Slide 54
Prevent air & fluid from returning toPrevent air & fluid from returning to
the pleural spacethe pleural space
The two-bottle system is the key for chestThe two-bottle system is the key for chest
drainagedrainage
A place for drainage to collectA place for drainage to collect
A one-way valve that prevents air or fluid fromA one-way valve that prevents air or fluid from
returning to the chestreturning to the chest
- 55. Copyright © 2006 by Mosby, Inc.Slide 55
Restore negative pressure in the pleuralRestore negative pressure in the pleural
spacespace
Many years ago, it was believed that suction wasMany years ago, it was believed that suction was
always required to pull air and fluid out of thealways required to pull air and fluid out of the
pleural space and pull the lung up against thepleural space and pull the lung up against the
parietal pleuraparietal pleura
However, recent research has shown that suctionHowever, recent research has shown that suction
may actually prolong air leaks from the lung bymay actually prolong air leaks from the lung by
pulling air through the opening that wouldpulling air through the opening that would
otherwise close on its ownotherwise close on its own
IfIf suctionsuction is required, ais required, a third bottlethird bottle is addedis added
- 56. Copyright © 2006 by Mosby, Inc.Slide 56
Restore negative pressure in theRestore negative pressure in the
pleural spacepleural space
Tube to
vacuum
source
Tube open to
atmosphere
vents air
Tube from patient
Fluid
drainage
Straw under
20 cmH2O
- 57. Copyright © 2006 by Mosby, Inc.Slide 57
Restore negative pressure in the pleuralRestore negative pressure in the pleural
spacespace
The straw submerged in the suction control bottleThe straw submerged in the suction control bottle
(typically to 20cmH(typically to 20cmH22O) limits the amount ofO) limits the amount of
negative pressure that can be applied to thenegative pressure that can be applied to the
pleural space – in this case -20cmHpleural space – in this case -20cmH22OO
The submerged straw is open at the topThe submerged straw is open at the top
As the vacuum source is increased, once bubblingAs the vacuum source is increased, once bubbling
begins in this bottle, it means atmosphericbegins in this bottle, it means atmospheric
pressure is being drawn in to limit the suction levelpressure is being drawn in to limit the suction level
- 58. Copyright © 2006 by Mosby, Inc.Slide 58
Restore negative pressure in theRestore negative pressure in the
pleural spacepleural space
TheThe depth of the waterdepth of the water
in the suction bottlein the suction bottle
determines the amountdetermines the amount
of negative pressureof negative pressure
that can be transmittedthat can be transmitted
to the chest,to the chest, NOT theNOT the
reading on thereading on the
vacuum regulatorvacuum regulator
- 59. Copyright © 2006 by Mosby, Inc.Slide 59
Restore negative pressure in the pleuralRestore negative pressure in the pleural
spacespace
There is no research to support this number ofThere is no research to support this number of
-20cmH-20cmH22O, just conventionO, just convention
Higher negative pressure can increase the flowHigher negative pressure can increase the flow
rate out of the chest, but it can also damagerate out of the chest, but it can also damage
tissuetissue
- 60. Copyright © 2006 by Mosby, Inc.Slide 60
How a chest drainage systemHow a chest drainage system
worksworks
Expiratory positive pressureExpiratory positive pressure from the patientfrom the patient
helps push air and fluid out of the chest (cough,helps push air and fluid out of the chest (cough,
Valsalva)Valsalva)
GravityGravity helps fluid drainage as long as the chesthelps fluid drainage as long as the chest
drainage system is below the level of the chestdrainage system is below the level of the chest
SuctionSuction can improve the speed at which air andcan improve the speed at which air and
fluid are pulled from the chestfluid are pulled from the chest
- 61. Copyright © 2006 by Mosby, Inc.Slide 61
From bottles to a boxFrom bottles to a box
The bottle system worked, but it was bulky at theThe bottle system worked, but it was bulky at the
bedside and with 16 pieces and 17 connections,bedside and with 16 pieces and 17 connections,
it was difficult to set up correctly whileit was difficult to set up correctly while
maintaining sterility of all of the partsmaintaining sterility of all of the parts
In 1967, a one-piece, disposable plastic box wasIn 1967, a one-piece, disposable plastic box was
introducedintroduced
The box did everything the bottles did – andThe box did everything the bottles did – and
moremore
- 62. Copyright © 2006 by Mosby, Inc.Slide 62
At the bedsideAt the bedside
Keep drain below the chestKeep drain below the chest
for gravity drainagefor gravity drainage
This will cause aThis will cause a pressurepressure
gradientgradient with relativelywith relatively
higher pressure in the chesthigher pressure in the chest
Fluid, like air, moves fromFluid, like air, moves from
an area of higher pressurean area of higher pressure
to an area of lower pressureto an area of lower pressure
Same principle as raising anSame principle as raising an
IV bottle to increase flowIV bottle to increase flow
raterate
- 63. Copyright © 2006 by Mosby, Inc.Slide 63
Monitoring intrathoracic pressureMonitoring intrathoracic pressure
The water seal chamber and suction controlThe water seal chamber and suction control
chamber provide intrathoracic pressure monitoringchamber provide intrathoracic pressure monitoring
Gravity drainage without suctionGravity drainage without suction: Level of water in: Level of water in
thethe water seal chamber = intrathoracic pressurewater seal chamber = intrathoracic pressure
(chamber is calibrated manometer)(chamber is calibrated manometer)
Slow, gradual rise in water level over time means moreSlow, gradual rise in water level over time means more
negative pressure in pleural space and signals healingnegative pressure in pleural space and signals healing
Goal is to return to -8cmHGoal is to return to -8cmH2200
With suctionWith suction: Level of water in: Level of water in suction control +suction control +
level of water inlevel of water in water sealwater seal chamberchamber ==
intrathoracic pressureintrathoracic pressure
- 64. Copyright © 2006 by Mosby, Inc.Slide 64
Monitoring air leakMonitoring air leak
Water seal is a window intoWater seal is a window into
the pleural spacethe pleural space
Not only for pressureNot only for pressure
If air is leaving the chest,If air is leaving the chest,
bubbling will be seen herebubbling will be seen here
Air leak meter (1-5) provides aAir leak meter (1-5) provides a
way to “measure” the leak andway to “measure” the leak and
monitor over time – gettingmonitor over time – getting
better or worse?better or worse?
- 65. Copyright © 2006 by Mosby, Inc.Slide 65
Setting up the drainSetting up the drain
Follow the manufacturer’s instructions for addingFollow the manufacturer’s instructions for adding
water to the 2cm level in the water seal chamber,water to the 2cm level in the water seal chamber,
and to the 20cm level in the suction controland to the 20cm level in the suction control
chamber (unless a different level is ordered)chamber (unless a different level is ordered)
Connect 6' patient tube to thoracic catheterConnect 6' patient tube to thoracic catheter
Connect the drain to vacuum, and slowly increaseConnect the drain to vacuum, and slowly increase
vacuum untilvacuum until gentle bubblinggentle bubbling appears in theappears in the
suction control chambersuction control chamber
- 66. Copyright © 2006 by Mosby, Inc.Slide 66
Setting up suctionSetting up suction
You don’t need to boil spaghetti!You don’t need to boil spaghetti!
Vigorous bubbling isVigorous bubbling is loudloud andand
disturbing to most patientsdisturbing to most patients
Will also causeWill also cause rapid evaporationrapid evaporation in thein the
chamber, which willchamber, which will lower suction levellower suction level
Too much bubbling isToo much bubbling is not needed clinicallynot needed clinically inin
98% of patients – more is not better98% of patients – more is not better
If too much, turn down vacuum source untilIf too much, turn down vacuum source until
bubbles go away, then slowly increase until theybubbles go away, then slowly increase until they
reappear, then stopreappear, then stop
- 67. Copyright © 2006 by Mosby, Inc.Slide 67
Disposable chest drainsDisposable chest drains
Collection chamberCollection chamber
Fluids drain directly into chamber, calibrated in mL fluid,Fluids drain directly into chamber, calibrated in mL fluid,
write-on surface to note level and timewrite-on surface to note level and time
Water sealWater seal
One way valve, U-tube design, can monitor air leaks &One way valve, U-tube design, can monitor air leaks &
changes in intrathoracic pressurechanges in intrathoracic pressure
Suction control chamberSuction control chamber
U-tube, narrow arm is the atmospheric vent, large arm isU-tube, narrow arm is the atmospheric vent, large arm is
the fluid reservoir, system is regulated, easy to controlthe fluid reservoir, system is regulated, easy to control
negative pressurenegative pressure